Intro & Scope - Defining Darkness
- Defines visual loss magnitude & impact. Preventable blindness is a key public health issue.
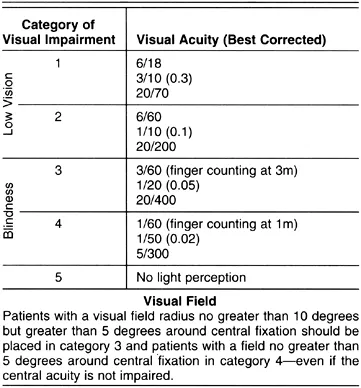
- WHO Blindness: Best Corrected Visual Acuity (BCVA) <3/60 or visual field <10° in better eye.
- WHO Categories (better eye): Severe VI (BCVA <6/60-3/60), Moderate VI (BCVA <6/18-6/60).
- India (NPCB) Blindness: <6/60 (or <1/60 / Counting Fingers at 1m) or field ≤20° in better eye.
⭐ India's blindness prevalence (≥50 yrs) is 0.36% (NBVIS 2015-19).
Major Causes - Preventable Villains
| Cause | Key Impact / At-Risk Group | Core Prevention / Community Strategy |
|---|---|---|
| Cataract | Leading cause; age-related opacity | Mass screening, high-volume quality cataract surgery (SICS, Phaco) |
| Refractive Errors | School children, adults; blurred vision | School eye health programs, vision screening, affordable spectacles |
| Vitamin A Deficiency | Children < 5 yrs; Xerophthalmia (XN, X1B) | Vit A prophylaxis (1 lakh IU <1yr, 2 lakh IU 1-6yr q 6mo), dietary diversification |
| Trachoma | Endemic areas; Chlamydia trachomatis; Cicatricial disease (TT) | WHO SAFE strategy (Surgery for TT, Antibiotics, Facial cleanliness, Environmental change) |
| Glaucoma | "Silent thief"; ↑IOP, optic neuropathy | Opportunistic screening, awareness, early diagnosis, lifelong management |
| Diabetic Retinopathy | Long-standing diabetes; neovascularization | Regular dilated fundus exam (annual), strict glycemic & BP control, laser photocoagulation |
⭐ Cataract is the leading cause of blindness and visual impairment in India, accounting for over 60% of cases. Most of this is surgically curable.
National Efforts - India's Vision Quest
-
National Programme for Control of Blindness & Visual Impairment (NPCBVI):
- Launched 1976. Current goal: reduce blindness prevalence to 0.3% by 2025.
- Key Target: Cataract Surgery Rate (CSR) of 600/lakh population/year (or 6000/million).
- Key components:
- Free cataract operations.
- School eye screening (refractive errors).
- Management of other causes (Diabetic Retinopathy, Glaucoma, Corneal Blindness).
- Eye banking & donation.
- Information, Education, Communication (IEC); Human Resource Development (HRD) & Infrastructure strengthening.
-
Vision 2020: The Right to Sight - India:
- Global WHO-IAPB initiative adopted by India to eliminate avoidable blindness.
- Pillars: Disease control (cataract, RE, childhood blindness, DR, glaucoma), HRD, infrastructure development, advocacy.
⭐ The National Programme for Control of Blindness (NPCB) was launched by India in 1976.
Screening & Action - Detect & Deflect
- Goal: Early detection & timely intervention to prevent blindness.
- Key Actions:
- Active (camps) & passive (opportunistic) case finding.
- Robust referral system (Primary → Tertiary care).
- Community health education on eye care.
Screening Priorities:
| Area | Target Group | Conditions Screened | Critical Action Thresholds (Examples) |
|---|---|---|---|
| School Eye Health | School children | Refractive errors, Vit. A deficiency, squint, amblyopia | VA < 6/9, any Bitot's spot |
| Diabetic Retinopathy | Known diabetics | Diabetic Retinopathy (DR), CSME | Any DR (referral), Mod. NPDR for ophthalmologist review |
| Childhood Blindness | Infants, <5 yrs | Congenital cataract, ROP (preterm <34wks, <1700g) | Leukocoria, absent red reflex, ROP Zone I or Stage 3 |
| Glaucoma (opportunistic) | Adults >40 yrs | Glaucoma | IOP >21 mmHg, CDR >0.5, suspicious optic disc |
Community Referral Flowchart:
⭐ ASHA's Role (NPCBVI): Creating awareness, identifying common eye problems (cataract, refractive errors), mobilizing community for screening camps, facilitating referrals, and ensuring treatment compliance (e.g., post-cataract surgery).
High‑Yield Points - ⚡ Biggest Takeaways
- Cataract: Leading cause of preventable blindness in India.
- Refractive Errors: Second most common cause of avoidable visual impairment.
- Vitamin A Deficiency: Major cause of childhood blindness; Bitot's spots are a key sign.
- Trachoma: Control via SAFE strategy (Surgery, Antibiotics, Facial cleanliness, Environmental improvement).
- Glaucoma: Early detection is vital to prevent irreversible blindness.
- Diabetic Retinopathy: Preventable with good glycemic control and regular screening.
- NPCBVI Target: Reduce blindness prevalence in India to 0.3% by 2025.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

