Photoreceptors & Transduction - Light's First Spark

- Rods: ~120 million; scotopic (night) vision; rhodopsin; slow response; high sensitivity; achromatic.
- Cones: ~6 million; photopic (day) vision; photopsins (color); fovea; fast response; lower sensitivity.
Phototransduction:
- Dark State (Depolarization):
- High cGMP → Na⁺/Ca²⁺ channels OPEN (dark current).
- Cell depolarized (~-40mV).
- Continuous glutamate release.
- Light State (Hyperpolarization):
- Light → 11-cis retinal to all-trans retinal (in rhodopsin/photopsin).
- Activates Transducin (G-protein).
- Transducin activates Phosphodiesterase (PDE).
- PDE ↓cGMP → Na⁺/Ca²⁺ channels CLOSE.
- Cell hyperpolarizes (~-70mV).
- ↓Glutamate release.
⭐ In the dark, photoreceptors are depolarized and continuously release glutamate. Light causes hyperpolarization and reduces glutamate release.
Retinal Processing - Retina's Router Room
- Signals from photoreceptors processed by retinal interneurons. 📌 People Buy Hats And Gloves (Photoreceptor → Bipolar → Horizontal/Amacrine → Ganglion).
- Bipolar Cells (BCs): First-order neurons.
- ON-center (depolarize to light in center) & OFF-center (hyperpolarize to light in center).
- Horizontal Cells (HCs): Mediate lateral inhibition; shape receptive field surrounds.
- Amacrine Cells (ACs): Diverse; modulate BC-GC synapse (e.g., motion, direction).
- Ganglion Cells (GCs): Output to brain; axons form optic nerve.
- Types: M (magnocellular: motion), P (parvocellular: detail, color).
- Center-surround receptive fields enhance contrast.
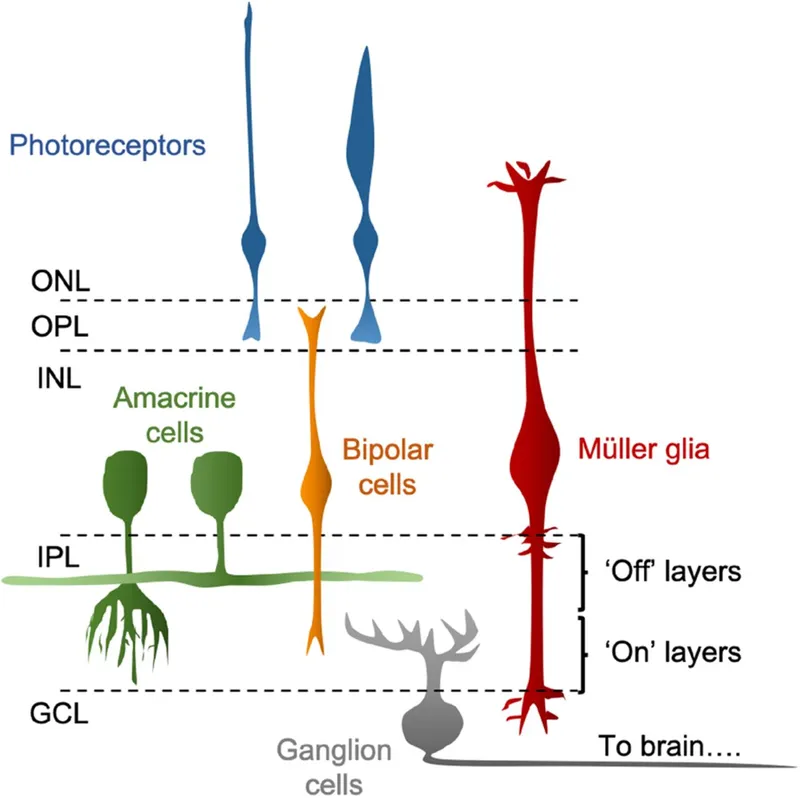
⭐ Center-surround receptive fields of bipolar and ganglion cells are crucial for edge detection and contrast enhancement.
Visual Pathway & Cortex - Brain's Big Screen
Signal flow from eye to brain:
- Optic Chiasm: Nasal retinal fibers decussate; temporal fibers remain ipsilateral.
⭐ A lesion at the optic chiasm typically causes bitemporal hemianopia.
- LGN (Lateral Geniculate Nucleus): Thalamic relay. 📌 "LGN = Light Goes Next".
- Magnocellular layers (1,2): Motion, spatial analysis ("Where" pathway).
- Parvocellular layers (3-6): Color, fine detail ("What" pathway).
- Optic Radiations (Geniculocalcarine Tract):
- Meyer's Loop (Temporal lobe): Info from inferior retina (superior visual field). Lesion → Superior quadrantanopia ("Pie in the sky").
- Baum's Loop (Parietal lobe): Info from superior retina (inferior visual field). Lesion → Inferior quadrantanopia ("Pie on the floor").
- Primary Visual Cortex (V1): Brodmann area 17; occipital lobe (calcarine sulcus). Retinotopic map; macula has large cortical representation.
Reflexes & Adaptation - Eye's Auto-Focus
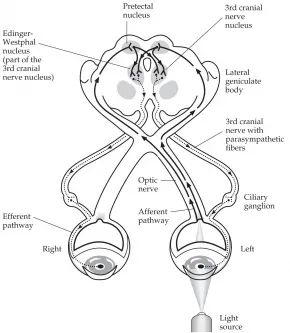
- Pupillary Light Reflex (PLR): Regulates light entry.
- Pathway: CN II → Pretectal Nucleus → Edinger-Westphal Nucleus → CN III → Sphincter Pupillae (miosis).
- Direct (same eye) & Consensual (opposite eye).
⭐ Relative Afferent Pupillary Defect (RAPD) or Marcus Gunn pupil indicates a lesion in the afferent pathway (optic nerve or severe retinal disease) anterior to the optic chiasm.
- Near Reflex Triad: For focusing on near objects. 📌 Mnemonic: CAM
- Convergence: Eyes adduct (medial recti, CN III).
- Accommodation: Lens thickens (ciliary muscle, CN III).
- Miosis: Pupil constricts (sphincter pupillae, CN III).
- Adaptation: Adjusts to varying light levels.
- Light Adaptation: Fast; pupil constricts, ↓ retinal sensitivity.
- Dark Adaptation: Slow (~30-40 mins); pupil dilates, rhodopsin regenerates, ↑ retinal sensitivity (rods primarily).
High‑Yield Points - ⚡ Biggest Takeaways
- Visual pathway: Retina → Optic Nerve → Chiasm (nasal decussation) → Tract → LGN → Radiations → Visual Cortex (Area 17).
- LGN: 6 layers; P-cells (form, color), M-cells (motion, depth).
- Visual cortex: V1 (striate); V4 (color), V5/MT (motion). Dorsal stream ("where"), Ventral stream ("what").
- Pupillary light reflex: Afferent CN II, Efferent CN III.
- Optic chiasm lesion: Bitemporal hemianopia. Post-chiasmal: Contralateral homonymous hemianopia.
- Meyer's loop lesion: Contralateral superior quadrantanopia ("pie in the sky").
- Retinotopic organization maintained throughout primary visual pathway.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

