Ocular Pharmacokinetics & Routes - Eye Drug Journey
- Key Barriers: Cornea (Lipophilic-Hydrophilic-Lipophilic layers), Blood-Aqueous Barrier (BAB), Blood-Retinal Barrier (BRB).
- Topical Route: Commonest. Bioavailability ~5%. Governed by $pH = pKa + log([A-]/[HA])$. Systemic absorption via nasolacrimal duct.
- Periocular Routes: Subconjunctival, Sub-Tenon's. Bypasses cornea, achieving higher local drug levels.
- Intraocular Routes: Intravitreal, Intracameral. Offer 100% bioavailability; direct to target.
- Systemic Route: Limited by BAB/BRB, especially for posterior segment delivery.
⭐ Topical drug absorption: Un-ionized, lipid-soluble forms penetrate the cornea more effectively.
oka
Autonomic Agents - Pupil & Pressure Puppeteers
- Cholinergics (Miotics): Miosis, ciliary spasm, ↑outflow.
- Direct: Pilocarpine (glaucoma), Carbachol.
- Pilocarpine: 📌 Pilo-pin pupil.
- Indirect: Physostigmine, Echothiophate.
- Action: Miosis, accommodation, ↑trabecular outflow.
⭐ Pilocarpine 2% helps differentiate 3rd nerve palsy from pharmacological mydriasis.
- Direct: Pilocarpine (glaucoma), Carbachol.
- Anticholinergics (Mydriatics/Cycloplegics): Mydriasis, cycloplegia (for refraction).
- Atropine (long), Tropicamide (short).
- Uses: Refraction (esp. children), uveitis (pain relief, prevent synechiae).
- ⚠️ Risk: Angle-closure glaucoma.
- Adrenergics:
- α1 Agonist: Phenylephrine (mydriasis only, no cycloplegia).
- α2 Agonists: Brimonidine, Apraclonidine (↓aqueous, ↑uveoscleral outflow).
- β-Blockers: Timolol, Betaxolol (β1 selective) (↓aqueous production).
- SEs: Bradycardia, bronchospasm.
 oka
oka
Glaucoma Guardians - IOP Busters
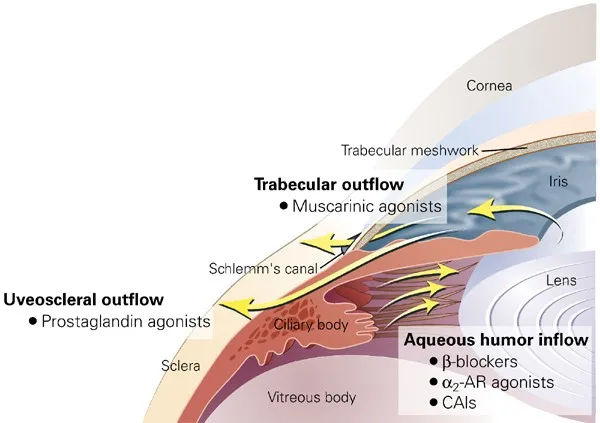
Primary goal: Lower Intraocular Pressure (IOP). Medications target aqueous humor (AH) dynamics by decreasing production or increasing outflow.
- Prostaglandin Analogs (PGAs): E.g., Latanoprost. ↑ Uveoscleral outflow. SE: iris pigmentation, lash growth. 📌 "Prosts" for outflow.
- Beta-blockers: E.g., Timolol. ↓ AH production (ciliary body). Caution: systemic effects.
- Alpha-2 Agonists: E.g., Brimonidine. Dual: ↓ AH production & ↑ uveoscleral outflow.
- Carbonic Anhydrase Inhibitors (CAIs): E.g., Dorzolamide (topical), Acetazolamide (systemic). ↓ AH production (inhibits $HCO_3^-$ formation).
- Miotics (Cholinergics): E.g., Pilocarpine. ↑ Trabecular outflow (ciliary muscle contraction).
⭐ Latanoprost is often first-line for open-angle glaucoma due to potent IOP reduction and once-daily dosing.
Anti-Inflammatory & Anti-Infective Arsenal - Soothers & Slayers
- Corticosteroids (Steroids):
- Mechanism: Inhibit $PLA_2$ → ↓$PGs$, $LTs$.
- Potent: Dexamethasone, Prednisolone. Soft: Fluorometholone (FML), Loteprednol (less IOP↑).
- Uses: Uveitis, post-op, severe allergy.
- SE: ↑IOP, PSC, infection risk.
- NSAIDs (Non-Steroidal Anti-Inflammatory Drugs):
- Mechanism: Inhibit $COX$ → ↓$PGs$.
- Examples: Ketorolac, Nepafenac, Diclofenac.
- Uses: Post-op pain/CME, allergy.
- Anti-Infectives:
- Antibacterial:
- Fluoroquinolones (Moxifloxacin): Broad spectrum. 📌 "Floxacins Flock Everywhere" (penetration).
- Aminoglycosides (Tobramycin): Gram -ve.
- Macrolides (Azithromycin): Chlamydia.
- Antifungal: Natamycin (filamentous), Amphotericin B/Voriconazole (Candida/Aspergillus).
- Antiviral: Acyclovir (HSV), Ganciclovir (CMV).
- Antiprotozoal: PHMB, Brolene (Acanthamoeba).
- Antibacterial:
⭐ Steroid-induced glaucoma: common with Dexamethasone; less with FML, Loteprednol etabonate (soft steroids).
Miscellaneous Meds - Special Ops Agents
- Anesthetics: Topical (Proparacaine); Injectable (Lignocaine).
- Diagnostic Dyes:
- Fluorescein: Stains corneal defects; Seidel's. (📌 FADES)
⭐ IV Fluorescein for Fundus Angiography (FFA) visualizes retinal circulation.
- Rose Bengal/Lissamine Green: Stains devitalized cells (dry eye).
- Anti-VEGF: Ranibizumab, Bevacizumab, Aflibercept (neovascularization).
- Lubricants: Artificial tears (CMC, HPMC) for dry eye.
High‑Yield Points - ⚡ Biggest Takeaways
- Autonomic drugs: pilocarpine (miotic), atropine (mydriatic/cycloplegic), timolol (↓IOP).
- Prostaglandin analogs (e.g., latanoprost): first-line for glaucoma, ↑ uveoscleral outflow.
- Topical steroids: potent anti-inflammatory; risk ↑IOP, cataracts.
- Antivirals (e.g., acyclovir) treat herpes simplex keratitis.
- Anti-VEGF agents (e.g., ranibizumab) for wet AMD, diabetic macular edema.
- Fluorescein dye stains corneal abrasions; used in applanation tonometry.
- Benzalkonium chloride (BAK), a common preservative, can cause ocular surface toxicity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

