General Ocular Pathology - Inflammatory Insights
-
Cardinal Signs: Rubor, tumor, calor, dolor, functio laesa.
-
Types:
- Acute: PMNs, exudative (e.g., bacterial keratitis).
- Chronic: Lymphocytes, macrophages, proliferative (e.g., chronic uveitis).
- Granulomatous: Epithelioid cells, giant cells (e.g., sarcoid uveitis, TB).
- Key cells: Langhans giant cells.
-
Mediators: Prostaglandins (PGs), leukotrienes, histamine, cytokines (TNF-α, ILs).
- PGs: Miosis, pain, ↑ vascular permeability.
-
Cellular Players:
- Neutrophils: Acute bacterial.
- Lymphocytes/Plasma cells: Chronic, viral.
- Eosinophils: Allergy, parasites.
- Macrophages: Phagocytosis, chronic.
-
Sequelae: Synechiae, cataract, glaucoma, phthisis bulbi.
⭐ Sympathetic ophthalmia is a bilateral granulomatous panuveitis following penetrating ocular trauma to one eye.
Corneal & Lens Pathologies - Clarity Compromised
- Corneal Clouding:
- Keratitis (Inflammation):
- Bacterial: Hypopyon, contact lens wear.
- Viral: HSV (dendritic ulcer), HZO (pseudodendritic).
- Fungal: Satellite lesions, feathery edges.
- Acanthamoeba: Ring infiltrate, severe pain.
- Dystrophies (Inherited, bilateral):
- Fuchs: Endothelial decompensation, guttata.
- Lattice: Amyloid deposits.
- Granular: Hyaline deposits.
- Macular: Mucopolysaccharide. 📌 AR, most severe.
- Keratoconus: Conical protrusion, Fleischer ring, Munson's sign.
- Keratitis (Inflammation):
- Lens Opacification (Cataract):
- Types: Senile (Nuclear sclerosis, Cortical spokes, PSC), Congenital (e.g., Rubella), Traumatic (Rosette), Metabolic (Galactosemia - oil droplet).
- Ectopia Lentis: Displaced lens (e.g., Marfan - superotemporal, Homocystinuria - inferonasal).
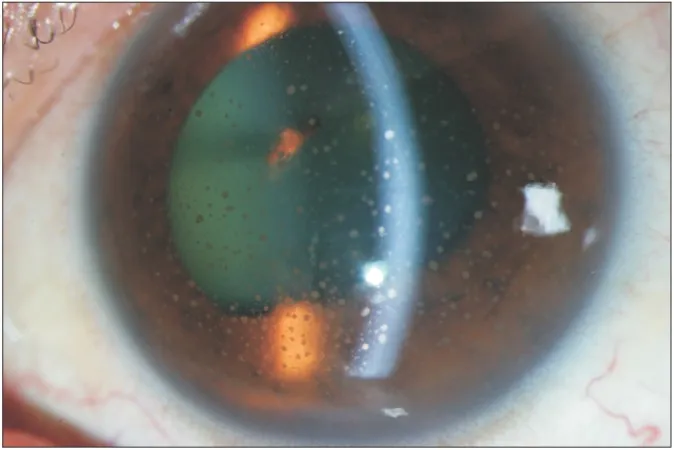
⭐ Posterior Subcapsular Cataract (PSC) is common with chronic steroid use and causes early, significant glare.
Retinal & Uveal Pathologies - Vision Vanquishers
- Retinal Vascular Diseases:
- Diabetic Retinopathy (DR):
- NPDR: Microaneurysms, hemorrhages, exudates, Cotton Wool Spots (CWS).
- PDR: Neovascularization (NVD/NVE), vitreous hemorrhage, tractional RD.
- Hypertensive Retinopathy: Arteriolar narrowing, AV nipping, CWS, flame hemorrhages, macular star, papilledema (Grade IV).
- Retinal Vein Occlusion (RVO):
- CRVO: "Blood & thunder" fundus, sudden painless vision loss.
- BRVO: Sectoral hemorrhages.
- Retinal Artery Occlusion (RAO):
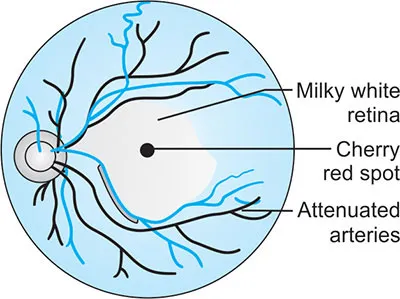
- CRAO: Sudden, profound, painless vision loss; "cherry-red spot". Ocular emergency!
- Diabetic Retinopathy (DR):
- Retinal Degenerations:
- Age-related Macular Degeneration (AMD):
- Dry (Atrophic): Drusen, RPE atrophy. Gradual vision loss.
- Wet (Exudative): Choroidal neovascularization (CNVM), leakage. Rapid, severe vision loss.
- Age-related Macular Degeneration (AMD):
* Retinitis Pigmentosa (RP): Progressive nyctalopia, peripheral field loss, "bone spicule" pigmentation. 📌 Mnemonic: RP = Rods Perish.
- Ocular Tumors:
- Uveal Melanoma: Most common primary intraocular tumor in adults. Liver metastasis common.
- Retinoblastoma: Most common in children. Leukocoria, strabismus.
⭐ Retinoblastoma: Associated with Rb1 gene mutation. Histopathology shows Flexner-Wintersteiner rosettes.
Glaucoma & Optic Neuropathies - Pressure Problems
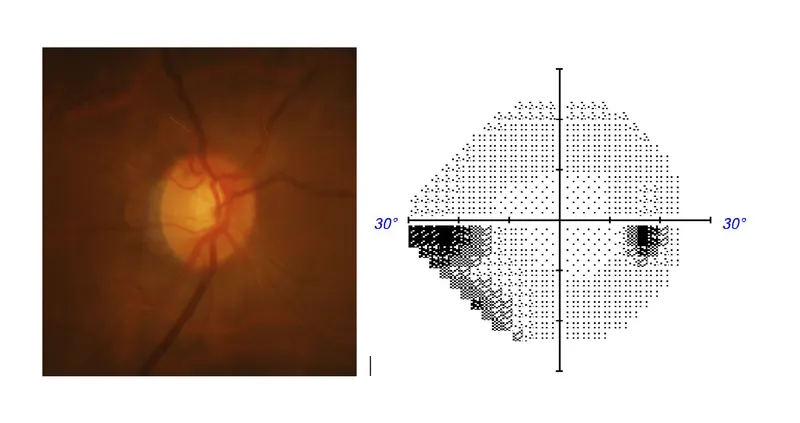
- Glaucoma: Optic neuropathy; characteristic disc cupping & visual field (VF) loss. Often associated with ↑ Intraocular Pressure (IOP).
- Primary Open-Angle Glaucoma (POAG): Most common, chronic, painless. Due to trabecular meshwork dysfunction.
- Angle-Closure Glaucoma (ACG): Iris obstructs trabecular meshwork. Acute (painful, red eye, halos, nausea) or chronic.
- Pathophysiology: ↑IOP → mechanical stress/vascular compromise at optic nerve head → Retinal Ganglion Cell (RGC) death → optic disc cupping (Cup-to-Disc Ratio > 0.5), characteristic VF defects.
- Risk Factors: Age, family history, ethnicity (African/Hispanic for POAG, Asian for ACG), myopia (POAG), hypermetropia (ACG), diabetes, prolonged steroid use.
- Diagnosis: Tonometry (IOP measurement), gonioscopy (angle assessment), optic disc exam, perimetry (VF testing).
⭐ Normal IOP is 10-21 mmHg. In acute angle closure glaucoma, IOP can rapidly rise, often exceeding 50 mmHg.
- Other Optic Neuropathies:
- Ischemic Optic Neuropathy (ION): Arteritic (AION - e.g., Giant Cell Arteritis, ESR↑, urgent steroids) & Non-Arteritic (NAION - common, vasculopathic risks like DM, HTN).
- Optic Neuritis: Inflammation, often Multiple Sclerosis-associated; pain on eye movement, ↓vision, Relative Afferent Pupillary Defect (RAPD).
- Compressive/Infiltrative: Tumors, thyroid eye disease.
High‑Yield Points - ⚡ Biggest Takeaways
- Basal cell carcinoma: most common malignant eyelid tumor; locally invasive, rarely metastasizes.
- Retinoblastoma: RB1 gene; most common childhood intraocular malignancy; leukocoria, Flexner-Wintersteiner rosettes.
- Uveal melanoma: most common adult primary intraocular malignancy; liver metastasis is frequent.
- Chalazion: chronic lipogranulomatous inflammation of a Meibomian gland (blocked duct).
- Pterygium: elastotic degeneration of collagen, fibrovascular growth from conjunctiva, linked to UV exposure.
- Diabetic retinopathy: microaneurysms (earliest sign); neovascularization (proliferative DR).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

