Ocular Immune System - Eye's Tiny Defenders
- Immune Privilege: Eye's unique defense, limiting inflammation to protect vision. Key sites: anterior chamber, vitreous cavity, subretinal space.
- Cellular Army:
- Antigen-Presenting Cells (APCs): Langerhans cells (cornea, conjunctiva), macrophages.
- Lymphocytes: T-cells & B-cells.
- Mast cells: Key in allergic reactions.
- Soluble Weapons:
- Tears: Contain Secretory IgA (sIgA) - first line of defense, lysozyme.
- Complement system, cytokines.
- Specialized Lymphoid Tissues:
- Conjunctiva-Associated Lymphoid Tissue (CALT).
- Lacrimal Gland Associated Lymphoid Tissue (LGALT).
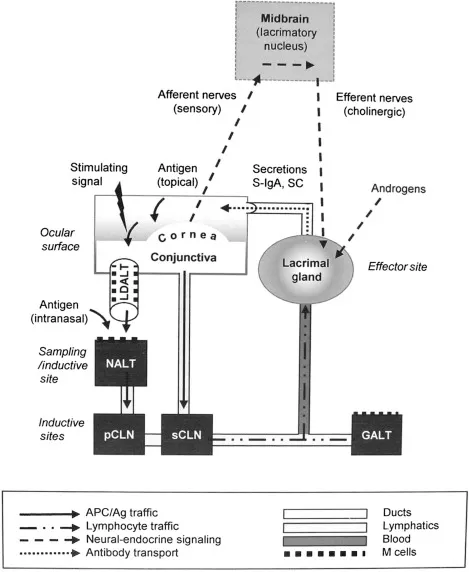
⭐ Anterior Chamber Associated Immune Deviation (ACAID) is a vital mechanism of ocular immune privilege, inducing systemic tolerance to intraocular antigens via regulatory T-cells.
Immune Privilege - Eye's VIP Pass
The eye uniquely tolerates antigens without damaging inflammation, vital for vision. This "VIP pass" is a complex protective strategy.
- Key Mechanisms:
- Barriers: Blood-ocular barriers (blood-aqueous & blood-retinal).
- Alymphatic: Cornea, lens, vitreous lack lymphatic drainage.
- Soluble Factors: Immunosuppressive TGF-β, α-MSH, FasL create an anti-inflammatory milieu.
- ACAID: Anterior Chamber Associated Immune Deviation; antigens in AC induce systemic tolerance via regulatory T cells.
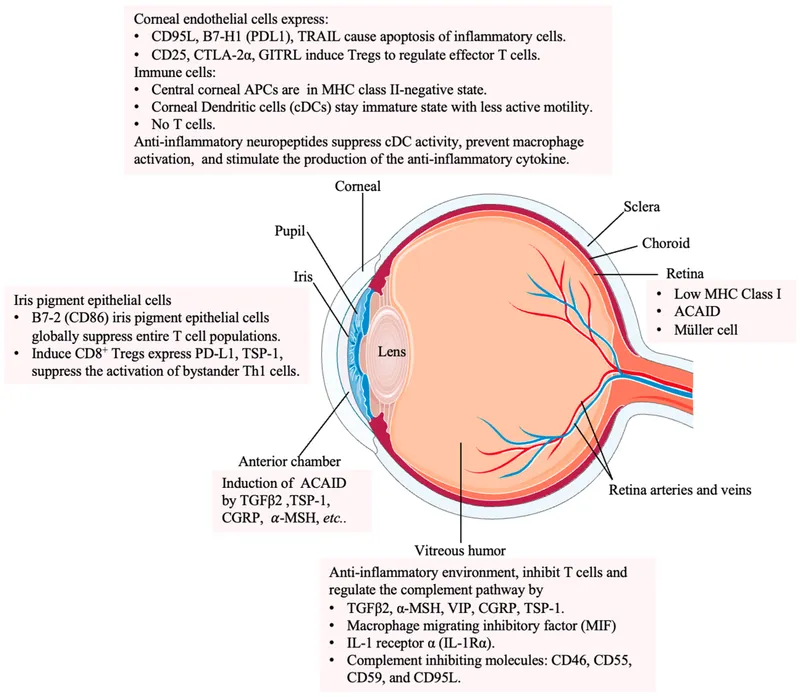
⭐ ACAID is a major reason for the high success (>90%) of initial corneal transplants, even without HLA matching.
Ocular Hypersensitivity - Allergic Eye Alarms
Ocular damage from immune overreaction. Classified by 📌 Gell & Coombs:
| Type | Name (ACID) | Mechanism | Ocular Examples |
|---|---|---|---|
| I | Allergic (A) | IgE-mediated, mast cell degranulation, histamine release | Allergic conjunctivitis, VKC, AKC |
| II | Cytotoxic (C) | Antibody (IgG/IgM) against cell surface antigens, complement activation, cell lysis | Ocular Cicatricial Pemphigoid, Mooren's ulcer |
| III | Immune Cmplx (I) | Deposition of antigen-antibody (Ag-Ab) immune complexes, complement activation, inflammation | Scleritis, some Uveitis, SJS |
| IV | Delayed (D) | Delayed T-cell mediated (Th1, CTLs), cytokine release, macrophage activation | Contact dermatitis, Phlyctenules, Graft rejection |
Key Immunopathologies & Tx - Rogue Cells & Remedies
- Uveitis: Uveal tract inflammation.
- Types: Anterior, Intermediate, Posterior, Panuveitis.
- Etiology: Infections, autoimmune (HLA-B27), trauma.
- Tx: Corticosteroids, mydriatics, immunomodulators (Methotrexate).
- Sympathetic Ophthalmia: Bilateral granulomatous panuveitis post-trauma/surgery to one eye.
- Autoimmune to uveal antigens.
- Tx: Aggressive immunosuppression; enucleation of injured eye within 2 weeks may prevent.
- Ocular Cicatricial Pemphigoid (OCP): Autoimmune conjunctivitis causing scarring.
- Type II HSR. Leads to symblepharon, blindness.
- Tx: Systemic immunosuppressants (Dapsone, Cyclophosphamide).
- Mooren's Ulcer: Idiopathic peripheral ulcerative keratitis (PUK).
- Painful, progressive. Autoimmune.
- Tx: Steroids, immunosuppressants.
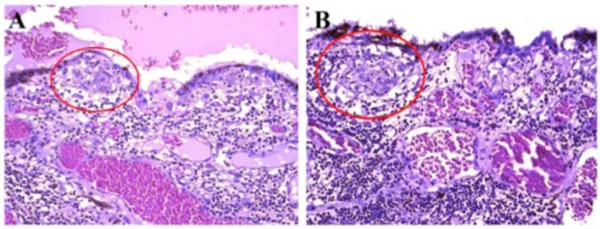
⭐ Sympathetic ophthalmia can occur weeks to decades after initial injury; early enucleation of a non-salvageable traumatized eye is key prevention if vision is lost in that eye within 14 days post-injury to prevent sensitization to self-antigens and subsequent attack on the fellow eye (sympathizing eye).
High‑Yield Points - ⚡ Biggest Takeaways
- Anterior Chamber Associated Immune Deviation (ACAID) is a key mechanism for ocular immune privilege.
- Sympathetic Ophthalmia: bilateral granulomatous uveitis post-trauma; T-cell mediated against retinal antigens.
- Type I hypersensitivity (IgE-mediated) is common in allergic conjunctivitis.
- Type IV hypersensitivity (cell-mediated) is involved in phlyctenular keratoconjunctivitis and contact dermatitis.
- Corneal graft rejection involves both cellular (T-lymphocytes) and humoral immune responses.
- Uveitis can be associated with systemic autoimmune diseases like Ankylosing Spondylitis (HLA-B27).
- Toll-like receptors (TLRs) on ocular surface cells recognize PAMPs, initiating innate immune responses.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

