Light & Optics Basics - Ray's Eye View
- Light: Electromagnetic radiation; wave-particle duality. Visible spectrum: 400-700 nm.
- Reflection: Light bounces; angle of incidence = angle of reflection.
- Refraction: Light bends passing between media. Snell's Law: $n_1 \sin(\theta_1) = n_2 \sin(\theta_2)$.
- Refractive index ($n$): $n = c/v$. Higher $n$ means slower light, more bending.
- Lenses:
- Convex (converging, +): Corrects hyperopia.
- Concave (diverging, -): Corrects myopia.
- Focal point: Where parallel rays converge/appear to diverge.
- Focal length ($f$): Lens to focal point distance.
- Diopter ($D$): Lens power; $D = 1/f$ ($f$ in meters).
- Vergence: Degree of light convergence/divergence (diopters).

⭐ The cornea is the eye's primary refractive surface, contributing ~+43D to the total ~+60D optical power.
Anterior Segment Imaging - Cornea's Close-Up
- Foundation: Slit-lamp biomicroscopy for initial detailed examination.
- Corneal Topography: Maps corneal surface power.
- Placido disk: Anterior curvature via reflected mires.
- Scheimpflug (e.g., Pentacam): Rotating camera; anterior/posterior curvature, pachymetry, anterior chamber depth (ACD).
- AS-OCT (Anterior Segment Optical Coherence Tomography): High-resolution optical cross-sections.
- Measures: Central Corneal Thickness (CCT ~540 µm), epithelial maps, anterior chamber angle.
- Uses: Glaucoma, refractive surgery planning.
- Specular Microscopy: Evaluates endothelial cell density (Normal: 2000-3000 cells/mm²) & morphology.
- Confocal Microscopy: In-vivo cellular detail (e.g., fungal/Acanthamoeba keratitis).
- UBM (Ultrasound Biomicroscopy): High frequency (35-50 MHz) ultrasound; images structures behind iris (ciliary body, sulcus).

⭐ Scheimpflug imaging uniquely provides both anterior and posterior corneal elevation and curvature data, vital for early keratoconus detection and refractive surgery screening.
Posterior Segment & Angio - Retina In Motion
- Dynamic Imaging: Visualizes blood flow & structural changes over time in the posterior segment.
- Fundus Fluorescein Angiography (FFA):
- Dye: Sodium Fluorescein (IV).
- Excitation: 465-490 nm (blue light), Emission: 520-530 nm (yellow-green light).
- Phases: Choroidal (pre-arterial), Arterial, Arteriovenous, Venous (early, mid, late), Late staining/leakage.
- Key findings: Hyperfluorescence (leakage, pooling, staining, window defect), Hypofluorescence (blockage, vascular filling defect).
- Indocyanine Green Angiography (ICGA):
- Dye: Indocyanine Green (IV).
- Near-infrared light: Deeper penetration, better visualization of choroidal circulation.
- Uses: Occult Choroidal Neovascularization (CNV), Polypoidal Choroidal Vasculopathy (PCV), choroidal tumors.
- Optical Coherence Tomography Angiography (OCT-A):
- Non-invasive, no dye required.
- Detects motion of Red Blood Cells (RBCs) to create angiograms.
- Provides depth-resolved 3D vascular maps (retinal & choroidal plexuses).
- Applications: Diabetic Retinopathy (DR), Age-related Macular Degeneration (AMD), Retinal Vein Occlusion (RVO).
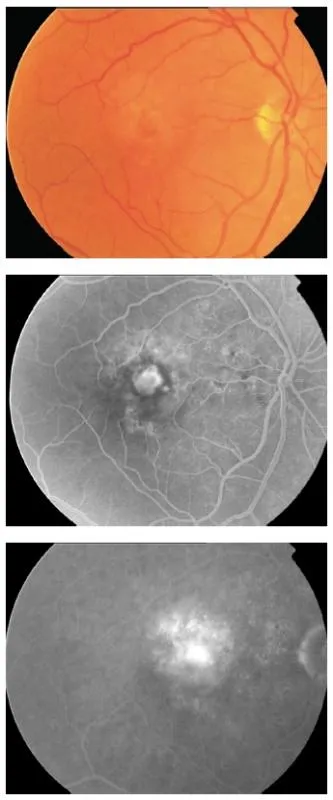
⭐ In FFA, a "hot disc" (diffuse optic disc hyperfluorescence) can indicate optic disc edema or papillitis, representing leakage from disc capillaries.
Cross-Sectional Imaging - Depth & Detail
- Ultrasound (USG): Uses sound waves.
- A-Scan: Measures axial length (IOL power). Time vs. echo amplitude.
- B-Scan: 2D cross-section. Posterior segment if opaque media.
- UBM (Ultrasound Biomicroscopy): High frequency (35-50 MHz). Anterior segment (angle, ciliary body). Limited penetration.
- Optical Coherence Tomography (OCT): Light-based, high resolution (1-15 µm), near-histological.
- Principle: Low-coherence interferometry. Measures optical backscattering.
- Types: TD-OCT, SD-OCT (faster, ↑res), SS-OCT (fastest, ↑depth).
- Applications: Macula (edema, AMD), glaucoma (RNFL), cornea.
⭐ SD-OCT & SS-OCT offer faster acquisition & higher axial resolution than TD-OCT.
- OCT Angiography (OCTA): Non-invasive, dye-less vascular imaging.
- Detects RBC motion.
- Applications: DR, RVO, AMD, neovascularization.

High‑Yield Points - ⚡ Biggest Takeaways
- A-scan USG measures axial length (IOL power); B-scan images posterior segment pathology.
- OCT uses low-coherence interferometry for high-res retinal/ONH imaging & RNFL analysis.
- FFA (fluorescein) shows retinal/choroidal circulation, leakage, and neovascularization.
- ICGA (indocyanine green) is superior for imaging choroidal vasculature and pathology.
- Corneal topography maps anterior curvature; tomography (Scheimpflug) provides 3D corneal analysis.
- Specular microscopy assesses corneal endothelial cell density and morphology.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

