Tear Film & Corneal Chemistry - Surface Shield
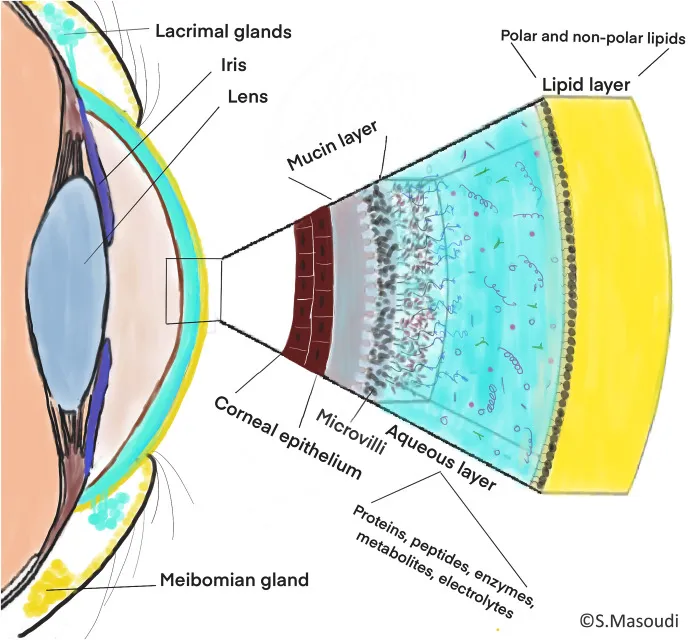
- Tear Film (3 layers): Protects & nourishes cornea. 📌 Lovely Apple Muffin (Lipid, Aqueous, Mucin).
- Lipid Layer (Outer): Meibomian glands; ↓ evaporation, smooth optics. Waxy esters, cholesterol.
- Aqueous Layer (Middle): Lacrimal glands; O₂ supply, antimicrobials (lysozyme, lactoferrin, IgA), pH ~7.4.
- Mucin Layer (Inner): Goblet cells; ↑ wettability (MUC5AC), traps debris.
- Corneal Chemistry: Maintains transparency & hydration.
- Stroma: 78% water; Type I collagen (ordered); Proteoglycans (keratan/chondroitin sulfate) for hydration.
- Epithelium/Endothelium: Na+/K+ ATPase pumps (endothelium for deturgescence). High glutathione (antioxidant).
- Glucose metabolism: Aerobic preferred.
⭐ The corneal endothelium's Na+/K+ ATPase pump is crucial for maintaining corneal deturgescence and transparency.
Aqueous & Lens Dynamics - Fluid & Focus
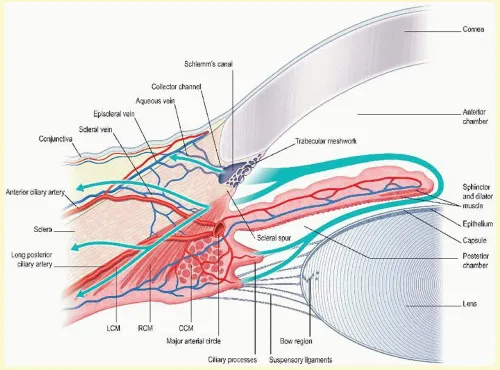
- Aqueous Humor (AH):
- Production: Ciliary body epithelium. Active secretion (Na+/K+ ATPase, carbonic anhydrase; ~80%) & ultrafiltration.
- Composition: Plasma-like; ↓ protein, ↑ ascorbate & lactate.
- Flow: Posterior chamber → pupil → anterior chamber.
- Drainage:
- Trabecular (80-95%): Trabecular meshwork → Schlemm's canal. Pressure-dependent.
- Uveoscleral (5-20%): Ciliary muscle → suprachoroidal space. Pressure-independent.
- Normal IOP: 10-21 mmHg.
- Lens:
- Avascular; high protein (crystallins).
- Metabolism: Anaerobic glycolysis. Sorbitol pathway (aldose reductase) active in hyperglycemia → osmotic damage (diabetic cataract).
- Transparency: Maintained by crystallin order, glutathione (GSH), Na+/K+ ATPase.
- Accommodation: Ciliary muscle contraction → zonules relax → ↑ lens curvature.
⭐ The lens has the body's highest protein concentration (~33%), mainly crystallins, crucial for its refractive power and transparency.
Vitreous & Retinal Pixels - Gel & Vision Quest
- Vitreous Humor:
- Composition: ~99% water, network of Collagen (Type II, IX, XI), Hyaluronic Acid (HA), proteoglycans. Provides viscoelasticity.
- Functions: Globe integrity, shock absorption, refractive medium.
- Ageing: Syneresis (liquefaction), PVD (Posterior Vitreous Detachment) → floaters.
- Retinal Phototransduction:
- Photoreceptors:
- Rods: Scotopic (low light), Rhodopsin, achromatic. ~120 million.
- Cones: Photopic (bright light), Photopsins (S, M, L types for color), chromatic. ~6 million.
- Visual Cycle: Light isomerizes 11-cis-retinal to all-trans-retinal.
- Regeneration in RPE via RPE65 enzyme.
- Dark Current: $cGMP$ opens $Na^+$ channels → depolarization.
- Light Signal Cascade:
- Photoreceptors:
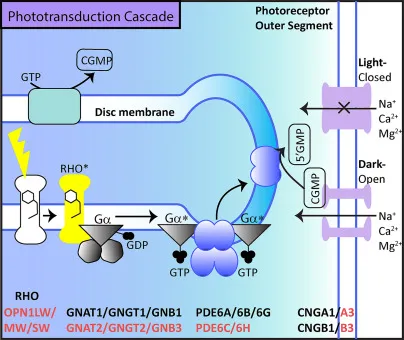
⭐ The "Dark Current" (Na+ influx) is unique; light stops this current, leading to hyperpolarization, not depolarization, of photoreceptors.
Ocular Metabolism & Defense - Energy & Guards
- Energy Source: Primarily glucose.
- Lens & Cornea: Anaerobic glycolysis; HMP shunt for NADPH (antioxidant).
- Retina: High aerobic metabolism (TCA cycle).
- Metabolic Pathways:
- Glycolysis: $Glucose \rightarrow ATP + Lactate$.
- HMP Shunt: Produces NADPH (for glutathione reduction) & ribose-5-P.
- Sorbitol Pathway: $Glucose \xrightarrow{Aldose Reductase} Sorbitol$; implicated in diabetic cataracts.
- Antioxidant Systems:
- Enzymatic: SOD, catalase, glutathione peroxidase.
- Non-enzymatic: Vitamin C (ascorbate), Vitamin E, glutathione (GSH).
⭐ Aqueous humor contains ~20x higher Vitamin C (ascorbate) than plasma, offering potent UV/oxidative protection.
High‑Yield Points - ⚡ Biggest Takeaways
- Vitamin A is vital for the visual cycle and rhodopsin regeneration.
- Lens metabolism is mainly anaerobic glycolysis; sorbitol accumulation causes diabetic cataracts.
- Corneal transparency relies on endothelial Na+/K+ ATPase and controlled hydration.
- Aqueous humor formation involves carbonic anhydrase, a key glaucoma drug target.
- The tear film has three layers: lipid, aqueous, and mucin, crucial for ocular surface integrity.
- Key ocular antioxidants include Vitamin C in aqueous humor and glutathione in the lens.
- Dominant collagens: Type I (cornea, sclera), Type II (vitreous), Type IV (lens capsule, Descemet's).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

