Eyeball Coats - Tunic Team-Up
- I. Fibrous Tunic (Outer Protective Coat):
- Sclera:
- Posterior 5/6; opaque, white.
- Dense collagen; shape, muscle attachment.
- Weakest point: Lamina cribrosa.
- Cornea:
- Anterior 1/6; transparent.
- Refractive power (+43D-+45D).
- Avascular. Layers 📌 (ABCDE).
- Sclera:
- II. Vascular Tunic (Uvea/Middle Coat): 📌 Uvea = ICU (Iris, Ciliary body, Choroid)
- Iris:
- Pupil control; eye color.
- Ciliary Body:
- Aqueous production (pars plicata).
- Accommodation (ciliary muscle).
- Choroid:
- Posterior, vascular, pigmented.
- Nourishes outer retina.
- Iris:
- III. Nervous Tunic (Inner Sensory Coat):
- Retina:
- Photosensitive; converts light to neural signals.
- Photoreceptors (rods & cones).
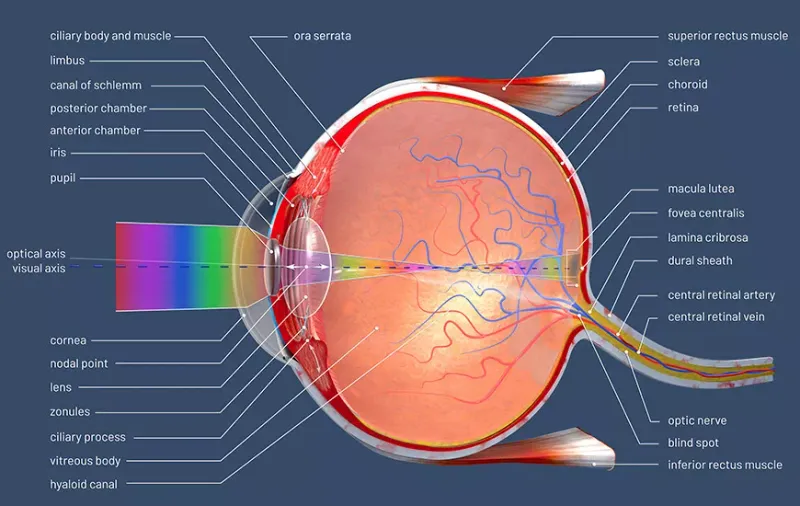 , vascular tunic (uvea: iris, ciliary body, choroid), and nervous tunic (retina))
, vascular tunic (uvea: iris, ciliary body, choroid), and nervous tunic (retina))
- Retina:
⭐ The sclera is thinnest just posterior to the insertions of the rectus muscles (approx. 0.3 mm).
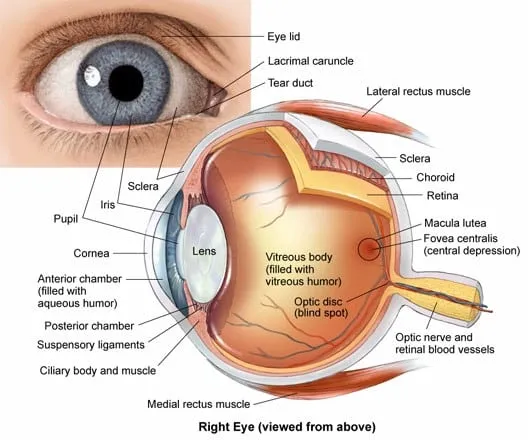
Inner Vision - Retina & Refractors
- Retina: Light-sensitive neural layer; 10 layers.
- Photoreceptors: Rods (scotopic vision, peripheral), Cones (photopic vision, central, color).
- Fovea centralis: Cones only, highest visual acuity. Macula lutea: surrounds fovea.
- Optic disc: Physiological blind spot (no photoreceptors).
- Refractive Media & Chambers:
- Aqueous Humor: Fills anterior & posterior chambers. Produced by ciliary body (pars plicata). Drains via trabecular meshwork & Schlemm's canal. Maintains Intraocular Pressure (IOP).
- Lens: Biconvex, transparent. Accommodation (ciliary muscle). Held by zonules.
- Vitreous Humor: Gel-like. Fills vitreous chamber (posterior segment).
⭐ Fovea centralis, located within the macula, contains only cone photoreceptors and is the site of highest visual acuity.
Ocular Orchestra - Muscles & Nerves
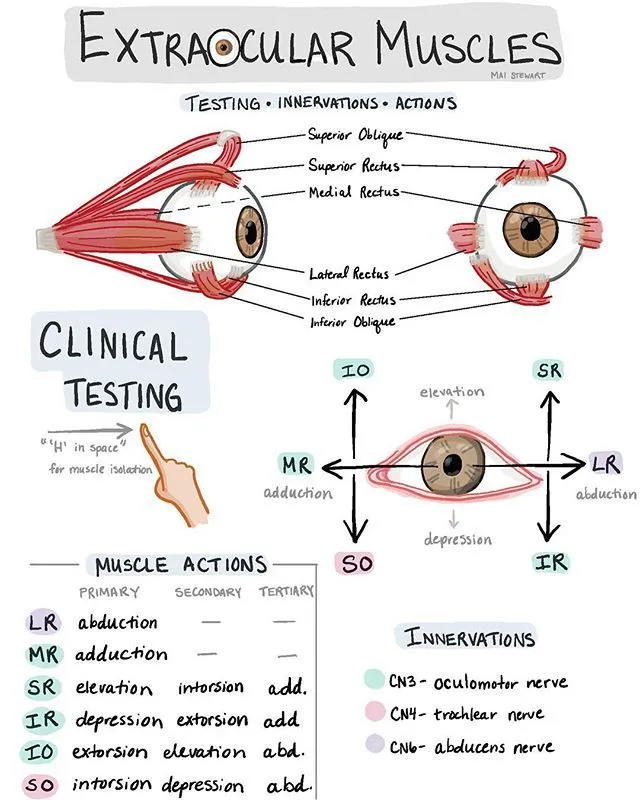
- Extraocular Muscles (EOMs): 7 (4 Recti, 2 Obliques, LPS).
- Recti (SR, IR, MR, LR): Origin Annulus of Zinn.
- MR: Adduction
- LR: Abduction
- SR: Elevation, Adduction, Intorsion
- IR: Depression, Adduction, Extorsion
- Obliques:
- SO: Origin sphenoid, via trochlea. Actions: Intorsion, Depression, Abduction.
- IO: Origin maxillary bone. Actions: Extorsion, Elevation, Abduction.
- Levator Palpebrae Superioris (LPS): Elevates upper eyelid.
- Recti (SR, IR, MR, LR): Origin Annulus of Zinn.
- Innervation: 📌 Mnemonic: $LR_6SO_4AO_3$
- CN III (Oculomotor): SR, IR, MR, IO, LPS. Parasympathetic: sphincter pupillae, ciliary muscle.
- CN IV (Trochlear): SO.
⭐ CN IV palsy: vertical diplopia, worse on downgaze & ipsilateral head tilt (Bielschowsky test +ve).
- CN VI (Abducens): LR.
- CN $V_1$ (Ophthalmic): Sensory. Nasociliary branch (cornea, iris, ciliary body).
- Sympathetic: Dilator pupillae, Müller's muscle.
 oka
oka
Vision's Voyage & Vital Vessels - Pathway & Pipelines
- Visual Pathway: Photoreceptors → Bipolar cells → Ganglion cells (axons form Optic Nerve) → Optic Nerve (CN II) → Optic Chiasm (nasal fibers decussate) → Optic Tract → Lateral Geniculate Nucleus (LGN) of Thalamus → Optic Radiations → Primary Visual Cortex (Occipital lobe, Brodmann area 17).
- Meyer's loop (temporal lobe lesion): contralateral superior quadrantanopia ("pie in the sky").
- Baum's loop (parietal lobe lesion): contralateral inferior quadrantanopia ("pie on the floor").
- Blood Supply:
- Arterial: Ophthalmic Artery (from Internal Carotid Artery).
- Central Retinal Artery (CRA): inner ⅔ retina; end-artery.
- Short Posterior Ciliary Arteries (SPCAs): choroid, outer ⅓ retina, optic nerve head.
- Long Posterior Ciliary Arteries (LPCAs) & Anterior Ciliary Arteries (ACAs): anterior segment.
- Venous: Central Retinal Vein (CRV), Vortex Veins → Superior/Inferior Ophthalmic Veins → Cavernous Sinus.
- Arterial: Ophthalmic Artery (from Internal Carotid Artery).
- Innervation:
- Sensory: CN V1 (Ophthalmic div.) → Nasociliary nerve (corneal sensation).
- Autonomic: Sympathetic (dilation); Parasympathetic (CN III → ciliary ganglion → short ciliary nerves: constriction, accommodation).
⭐ Occlusion of the Central Retinal Artery (CRAO) causes sudden, painless, profound loss of vision, often with a cherry-red spot at the macula due to intact choroidal circulation (supplied by SPCAs) visible through the ischemic inner retina.
High‑Yield Points - ⚡ Biggest Takeaways
- Cornea is the primary refractive surface, avascular and transparent.
- Lens allows accommodation for near vision, suspended by zonules.
- Retina houses rods (scotopic, peripheral) and cones (photopic, central, color).
- Optic nerve (CN II), formed by ganglion cell axons, exits at the optic disc (blind spot).
- Extraocular muscles: LR6 (abducens), SO4 (trochlear), remainder by oculomotor (CN III).
- Aqueous humor is produced by ciliary processes and drains mainly via trabecular meshwork.
- The uvea consists of the iris, ciliary body, and choroid; it is the vascular coat of the eye.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

