Cystocele & Urethrocele - Bladder Drop 101
- Cystocele: Herniation of bladder into anterior vagina (anterior colporrhaphy target).
- Urethrocele: Prolapse of urethra into vagina, often with cystocele.
- Etiology: Weakened pelvic floor (pubocervical fascia, levator ani) due to childbirth, aging, ↑intra-abdominal pressure.
- Symptoms: Vaginal bulge, urinary incontinence (stress, urge), incomplete emptying, dyspareunia.
- Diagnosis: Clinical exam; POP-Q staging.
⭐ A midline or central cystocele results from a defect in the pubocervical fascia directly beneath the bladder; a lateral cystocele (paravaginal defect) involves detachment of this fascia from the arcus tendineus fascia pelvis (ATFP).
Cystocele & Urethrocele - The Downward Triggers
- Childbirth: Vaginal delivery (esp. prolonged, instrumental, macrosomia), multiparity. Key factor.
- Menopause: ↓Estrogen → tissue atrophy, weakened support.
- Chronic ↑Intra-abdominal Pressure:
- Persistent cough (COPD)
- Constipation/straining
- Heavy lifting
- Obesity: Increased load on pelvic floor.
- Genetics: Connective tissue weakness (e.g., Marfan syndrome).
- Pelvic Surgery: Prior procedures (e.g., hysterectomy) weakening structures.
⭐ Vaginal childbirth is the single most significant risk factor for developing pelvic organ prolapse.
Cystocele & Urethrocele - Sagging Symptoms & Scales
- Symptoms:
- Vaginal bulge, pressure, heaviness, or "something coming down" sensation.
- Urinary symptoms:
- Stress Urinary Incontinence (SUI) - often prominent with urethrocele.
- Urgency, frequency, nocturia.
- Incomplete bladder emptying, hesitancy, weak/spraying stream.
- Need for splinting (manual vaginal pressure) to initiate or complete voiding.
- Recurrent UTIs.
- Sexual dysfunction: Dyspareunia, altered coital sensation.
- Scales for Assessment:
- Pelvic Organ Prolapse Quantification (POP-Q) System:
- Gold standard: Objective, reproducible, site-specific measurements.
- Hymen is the anatomical landmark (fixed reference point = 0 cm).
- Stages prolapse from Stage 0 (no prolapse) to Stage IV (complete eversion/procidentia). Essential for grading severity and surgical planning.
- Pelvic Organ Prolapse Quantification (POP-Q) System:
⭐ The most common presenting symptom of pelvic organ prolapse is the sensation of a vaginal bulge or that "something is falling out of the vagina."
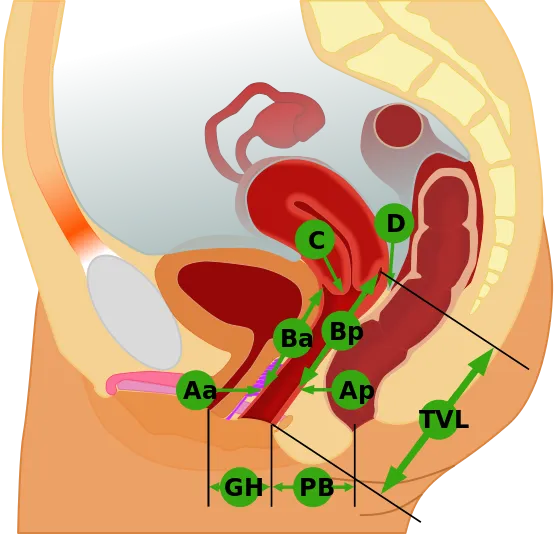
Cystocele & Urethrocele - Spotting the Slump
- Cystocele: Herniation of bladder into vagina (anterior wall).
- Urethrocele: Urethral prolapse into vagina.
- Symptoms: Vaginal bulge, pressure, urinary incontinence (stress, urge, mixed), incomplete emptying, dyspareunia.
- Diagnosis: Clinical exam (speculum, Sims, Valsalva), POP-Q staging.
⭐ High-yield: Anterior vaginal wall prolapse is the most common type of pelvic organ prolapse.
- Investigations: Urinalysis, Post-Void Residual (PVR) volume, Urodynamic studies if incontinence or voiding dysfunction is significant. Consider renal function tests if hydronephrosis suspected (severe prolapse).
Cystocele & Urethrocele - Uplift & Repair
- Cystocele: Bladder prolapse into anterior vagina. Urethrocele: Urethral prolapse, often with cystocele.
- Conservative Management (Mild/moderate symptoms):
- Pelvic Floor Muscle Training (PFMT/Kegels): Strengthens pelvic floor support. 📌 "Squeeze & Lift"
- Pessaries: Ring, Gellhorn types; non-surgical mechanical support.
- Lifestyle: Weight control, manage constipation/cough, avoid heavy lifting.
- Surgical Management (Severe symptoms / failed conservative):
- Anterior Colporrhaphy: Primary native tissue vaginal wall repair.
- Mesh Augmentation: For complex/recurrent defects; risks: erosion, chronic pain.
- Paravaginal Defect Repair: For lateral vaginal wall defects.
⭐ Anterior colporrhaphy is the most common surgery for cystocele; anatomical recurrence can be 30-40%. Mesh may reduce recurrence but has specific complications like erosion.
High‑Yield Points - ⚡ Biggest Takeaways
- Cystocele: Bladder herniation into anterior vagina. Urethrocele: Urethral prolapse.
- Major risk factors: Vaginal childbirth, multiparity, obesity, menopause (↓estrogen).
- Symptoms: Vaginal bulge, pelvic pressure, stress urinary incontinence (SUI), incomplete emptying.
- Diagnosis: Primarily clinical pelvic exam; POP-Q system for staging.
- Treatment: Kegel exercises, pessaries for mild/moderate; anterior colporrhaphy for symptomatic/severe.
- Urethrocele is a key cause of SUI due to loss of vesicourethral angle support_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

