Desire Disorders: Intro - Low Libido Lowdown
- Hypoactive Sexual Desire Disorder (HSDD): Defined as persistently or recurrently deficient (or absent) sexual/erotic thoughts or fantasies and desire for sexual activity.
- Must cause clinically significant personal distress.
- Diagnostic duration: Symptoms typically present for ≥6 months.
- Not better accounted for by:
- A nonsexual mental disorder.
- Severe relationship distress or other significant stressors.
- Effects of a substance/medication or another medical condition.
- Key DSM-5 Specifiers: Lifelong vs. Acquired; Generalized vs. Situational.
- Female Sexual Interest/Arousal Disorder (FSIAD): In DSM-5, this diagnosis is used for women, often encompassing low desire and/or arousal difficulties.
⭐ The presence of personal distress is crucial for differentiating HSDD from naturally low, but non-distressing, levels of sexual desire.
Desire Disorders: Etiology - Desire Dampeners
- Multifactorial Origin: Biological, psychological, interpersonal, sociocultural.
- Medical Conditions:
- Chronic illness: Diabetes, CVD, CKD, chronic pain.
- Endocrine: Hypothyroidism, hyperprolactinemia, hypogonadism (↓Testosterone/Estrogen).
- Pelvic issues: Endometriosis, PID, severe dyspareunia.
- Psychological Factors:
- Mood disorders: Depression, anxiety.
- Stress (chronic).
- Past trauma (e.g., sexual abuse).
- Negative body image.
- Medications (Iatrogenic): 📌 S.H.A.P.O.
- SSRIs (e.g., paroxetine), SNRIs.
- Hormonal agents (some OCPs, GnRH analogs, anti-androgens).
- Antihypertensives (β-blockers, spironolactone).
- Psychotropics (some antipsychotics like risperidone).
- Opioids.

- Relationship & Lifestyle:
- Interpersonal conflict, lack of intimacy.
- Substance abuse (alcohol, drugs), fatigue.
⭐ Among medications, SSRIs are frequently implicated in reducing libido; consider bupropion as an alternative if depression coexists.
Desire Disorders: Diagnosis - Interest Investigation
Core Evaluation:
- Detailed history: Key to diagnosis. Sexual (onset, duration, context), medical (comorbidities, medications like SSRIs), psychosocial (mood, relationship quality).
- Focused physical exam: Rule out organic causes. Signs of systemic illness, endocrine dysfunction (e.g., hypogonadism).
Screening Tools:
- Validated Questionnaires: e.g., FSFI (Female Sexual Function Index - desire domain), DSDS (Decreased Sexual Desire Screener).
Investigations (clinically guided):
- Hormonal assays: Testosterone (total/free), prolactin, TSH.
- Metabolic screen: Consider HbA1c, lipid profile.
Psychological Assessment:
- Evaluate for depression, anxiety, significant stressors, relationship distress.
⭐ Crucial: Always assess for underlying depression or medication side effects (e.g., SSRIs, anti-hypertensives) as common reversible causes of low desire.
Desire Disorders: Management - Libido Lifelines
- Core Strategy: Biopsychosocial approach; address contributing factors.
- Non-Pharmacological (Often First-Line):
- Psychosexual education & counseling: Correct misconceptions, improve communication.
- Cognitive Behavioral Therapy (CBT): Target negative thoughts/beliefs about sex.
- Sensate focus exercises: Reduce performance anxiety, enhance intimacy. (📌 Masters & Johnson)
- Mindfulness-based interventions: Improve body awareness & acceptance.
- Pharmacological (Specific Indications):
- Female (Generalized Acquired HSDD, Premenopausal):
- Flibanserin (Addyi®): Daily oral; 5-HT1A agonist/5-HT2A antagonist.
- Bremelanotide (Vyleesi®): Subcutaneous, as-needed; melanocortin receptor agonist.
- Male (HSDD with Hypogonadism):
- Testosterone Replacement Therapy (TRT): After confirming low testosterone.
- Bupropion: May help if SSRI-induced.
- Female (Generalized Acquired HSDD, Premenopausal):
- Crucial: Manage comorbidities (depression, anxiety) & relationship issues.
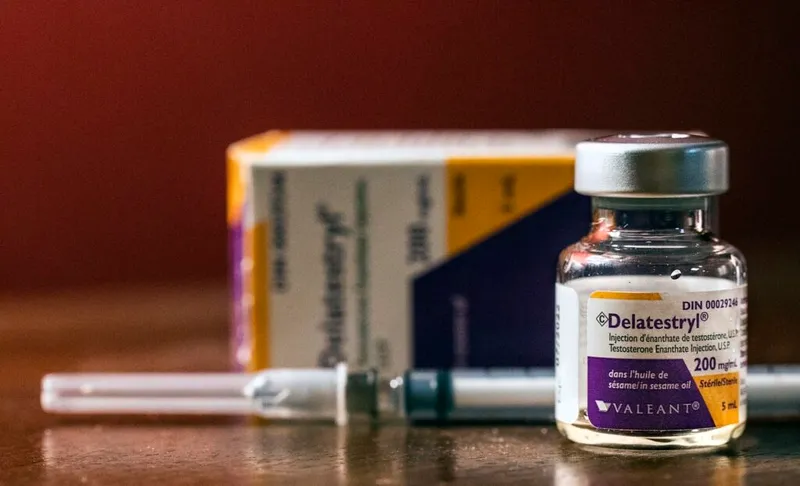
⭐ Flibanserin requires 4 weeks of daily use to assess efficacy and carries a boxed warning for hypotension and syncope, especially with alcohol.
High‑Yield Points - ⚡ Biggest Takeaways
- Hypoactive Sexual Desire Disorder (HSDD) is the most common female sexual dysfunction.
- Characterized by persistent lack of sexual thoughts, fantasies, or desire, causing marked personal distress.
- Exclude desire issues from relationship conflicts, medical illness, or substance/medication effects.
- A biopsychosocial approach is essential for comprehensive assessment and management.
- Management includes sex therapy/psychotherapy (CBT) and FDA-approved medications (e.g., Flibanserin).
- Always evaluate for underlying mood disorders (depression, anxiety) or endocrine dysfunction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

