HPO Axis & Key Players - Hormone Harmony HQ
The Hypothalamic-Pituitary-Ovarian (HPO) axis governs female reproduction through precise hormonal interplay and feedback.
- Hypothalamus: Releases GnRH (pulsatile).
- Anterior Pituitary: GnRH triggers FSH & LH release.
- FSH: Follicular growth, Estrogen ($E_2$) synthesis.
- LH: Ovulation, corpus luteum, Progesterone synthesis.
- Ovaries: Produce key hormones.
- Estrogen ($E_2$): Proliferative effects, feedback.
- Progesterone: Secretory effects, feedback.
- Inhibin: Suppresses FSH.
- Feedback:
- Negative: $E_2$/Progesterone/Inhibin on hypothalamus/pituitary.
- Positive: High $E_2$ → LH surge.
⭐ The pulsatile nature of GnRH secretion is essential; continuous GnRH administration leads to downregulation of pituitary receptors and suppressed gonadotropin release.
Ovarian Reserve Testing - Egg Timer Check
- Assesses quantity & quality of remaining oocytes.
- Key Tests:
- Anti-Müllerian Hormone (AMH):
- Produced by granulosa cells of preantral & small antral follicles.
- Stable throughout menstrual cycle.
- Normal: 1.5 - 4.0 ng/mL. ↓ AMH indicates ↓ ovarian reserve.
- Antral Follicle Count (AFC):
- Transvaginal ultrasound (TVS) count of follicles 2-10 mm in both ovaries (early follicular phase).
- Good reserve: AFC > 10-15; Poor reserve: AFC < 5-7.
- Day 3 FSH & Estradiol (E2):
- FSH: Normal < 10 mIU/mL. ↑ FSH suggests ↓ reserve.
- E2: Normal < 50-80 pg/mL. ↑ E2 (with normal FSH) can mask poor reserve.
- Anti-Müllerian Hormone (AMH):
⭐ AMH is currently considered one of the most reliable markers of ovarian reserve and correlates well with oocyte yield during IVF procedures.
- Other tests: Clomiphene Citrate Challenge Test (CCCT), Inhibin B (less common).
Ovulation & Luteal Phase Testing - Cycle Sleuth
- Ovulation Detection Methods:
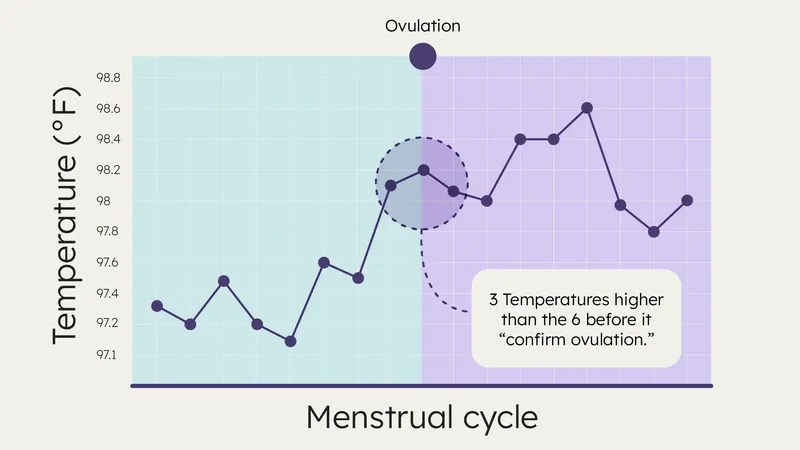
- BBT: Biphasic; ↑ 0.5-1°F post-ovulation.
- Urinary LH Kits: Detect LH surge 24-36h prior.
- Serum Progesterone (Mid-luteal, e.g., Day 21):
-
3 ng/mL = Ovulation occurred.
-
10 ng/mL = Adequate luteal function.
-
- Ultrasound (Folliculometry): Monitors follicle, confirms rupture.
- Luteal Phase Evaluation:
- Serum Progesterone (as above).
- Luteal Phase Length: <10-12 days suggests defect.
- Endometrial Biopsy (rare): Dating lag >2 days.
⭐ > Mid-luteal serum progesterone (>3 ng/mL) is key to confirm ovulation retrospectively.
 oka
oka
Androgen, Prolactin & Thyroid Tests - Hormone Hotspots
- Androgens (Testosterone, DHEAS):
- Indications: Hirsutism, virilization, irregular menses, PCOS suspicion.
- Total Testosterone: If ↑, consider SHBG.
- DHEAS: Adrenal androgen marker.
- Prolactin (PRL):
- Indications: Galactorrhea, amenorrhea, infertility.
- Rule out: Pregnancy, drug-induced, stress.
- Macroprolactin if PRL mildly ↑.
⭐ Prolactinomas are the most common pituitary adenomas; PRL >100 ng/mL is highly suggestive.
- Thyroid (TSH, free T4):
- Indications: Menstrual irregularities, infertility, goiter, hypo/hyperthyroid symptoms.
- TSH: Best initial screening test for thyroid dysfunction impacting reproduction.
- Subclinical hypothyroidism (↑TSH, normal fT4) can affect fertility. 📌 Thyroid Status Helps (TSH).
High‑Yield Points - ⚡ Biggest Takeaways
- Day 2/3 FSH, LH, Estradiol and AMH assess baseline ovarian reserve.
- AMH is a key cycle-independent marker of the ovarian follicular pool.
- Mid-luteal (Day 21) serum progesterone confirms ovulation.
- TSH and Prolactin are vital initial tests for amenorrhea and infertility.
- For hirsutism/virilization, evaluate serum testosterone and DHEAS.
- 17-hydroxyprogesterone (17-OHP) is crucial for diagnosing non-classical CAH.
- Always perform an hCG test to rule out pregnancy first.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

