Antenatal Multiple Gestation Care - Womb Wonders Welcome
- Diagnosis: Ultrasound confirms multiple gestation.
- Chorionicity & Amnionicity: Key for risk stratification. Determine ideally < 14 weeks.
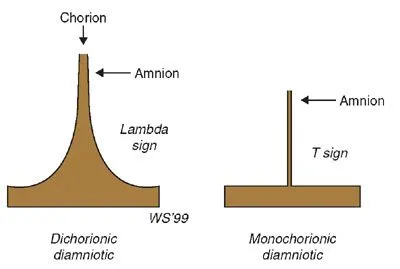
- Dichorionic-Diamniotic (DCDA): Lambda (λ) sign.
- Monochorionic-Diamniotic (MCDA): T-sign.
- Monochorionic-Monoamniotic (MCMA): No separating membrane.
- Enhanced Surveillance:
- Nutrition: ↑ Folic acid (1 mg/day), ↑ Iron supplements.
- Frequent visits: Monitor maternal (preeclampsia, GDM) & fetal complications (Preterm Labor, IUGR/sIUGR).
- Growth Scans & Monitoring:
- DCDA: Every 4 weeks from 20 weeks.
- MCDA: Every 2 weeks from 16 weeks (screen for TTTS, TAPS).
- MCMA: Individualized; inpatient monitoring often from 24-28 weeks.
- Complication Watch (Monochorionic):
- Twin-to-Twin Transfusion Syndrome (TTTS).
- Twin Anemia Polycythemia Sequence (TAPS).
- Twin Reversed Arterial Perfusion (TRAP) sequence.
⭐ Early and accurate determination of chorionicity (ideally before 14 weeks) is the cornerstone of managing multiple pregnancies as it dictates surveillance frequency and potential complications.
Intrapartum Multiple Gestation Management - Delivery Dance Duo
- Team Approach: Skilled obstetrician, anesthetist, pediatrician essential.
- Monitoring: Continuous EFM (both twins). IV access, blood ready.
- Delivery Interval: Aim < 20-30 min between twins.
- PPH Prevention: Active 3rd stage management (Oxytocin).
- MCMA Twins: Elective CS at 32+0 to 33+6 weeks (⚠️ high cord entanglement risk).
⭐ For diamniotic twin pregnancies, planned delivery is typically recommended between 37+0 to 37+6 weeks for uncomplicated cases; for monochorionic diamniotic (MCDA), 36+0 to 36+6 weeks; and for MCMA twins, 32+0 to 33+6 weeks via Caesarean section.
Multiple Gestation Complications - Syndrome Showdowns
Monochorionic twin pregnancies risk severe complications from placental vascular anastomoses. Key syndromes:
| Feature | TTTS (Twin-to-Twin Transfusion Syndrome) | TAPS (Twin Anemia Polycythemia Sequence) | sFGR (Selective Fetal Growth Restriction) |
|---|---|---|---|
| Patho. | Unbalanced AV shunt | Slow net AV shunt (<1mm anast.) | Unequal placenta share |
| Donor | Oligo (MVP <2cm), anemia, stuck | Anemia (MCA-PSV >1.5MoM) | EFW <10%ile, UA Doppler types |
| Recipient | Poly (MVP >8cm <20w; >10cm ≥20w), polycythemia | Polycythemia (MCA-PSV <1.0MoM; Hb diff >8 g/dL) | Normal/LGA (relative) |
| Key Dx | Oligo/Poly, Quintero Staging (I-V) | MCA-PSV discordance, no oligo/poly | EFW discordance >25%; UA Types (I-III) |
| Mgmt | FLP (16-26wks, Q II-IV) | IUT/PET, delivery | Type-dependent (expectant, laser, delivery) |
TTTS Management Algorithm:
⭐ Fetoscopic laser photocoagulation of anastomotic vessels is the preferred treatment for severe Twin-to-Twin Transfusion Syndrome (TTTS) diagnosed between 16 and 26 weeks of gestation (Quintero stages II-IV).
High‑Yield Points - ⚡ Biggest Takeaways
- Mode of delivery in twins: Vertex-vertex often vaginal; non-vertex first twin usually C-section.
- MCMA twins: Elective C-section at 32-34 weeks due to high cord entanglement risk.
- MCDA twins: Deliver at 36-37 weeks; screen for Twin-to-Twin Transfusion Syndrome (TTTS).
- DCDA twins: Deliver at 37-38 weeks; lowest risk twin type.
- Continuous intrapartum EFM for both twins is crucial during labor.
- Postpartum hemorrhage (PPH) risk is significantly increased in multiple gestations.
- External Cephalic Version (ECV) for a non-vertex second twin can be attempted.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

