Cervical Cerclage: Basics - Stitching Up a Weak Link
- Definition: Surgical procedure involving placing a stitch (suture) around the cervix to keep it closed.
- Goal: Prevent premature cervical dilation and preterm birth in women with cervical insufficiency (incompetence).
- Mechanism: Provides mechanical support to a weakened cervix.
- **Indications (General):
- History-indicated: Previous preterm birth < 34 weeks due to cervical factors.
- Ultrasound-indicated: Short cervical length (CL) < 25 mm before 24 weeks gestation.
- Exam-indicated (rescue): Painless cervical dilation in 2nd trimester.
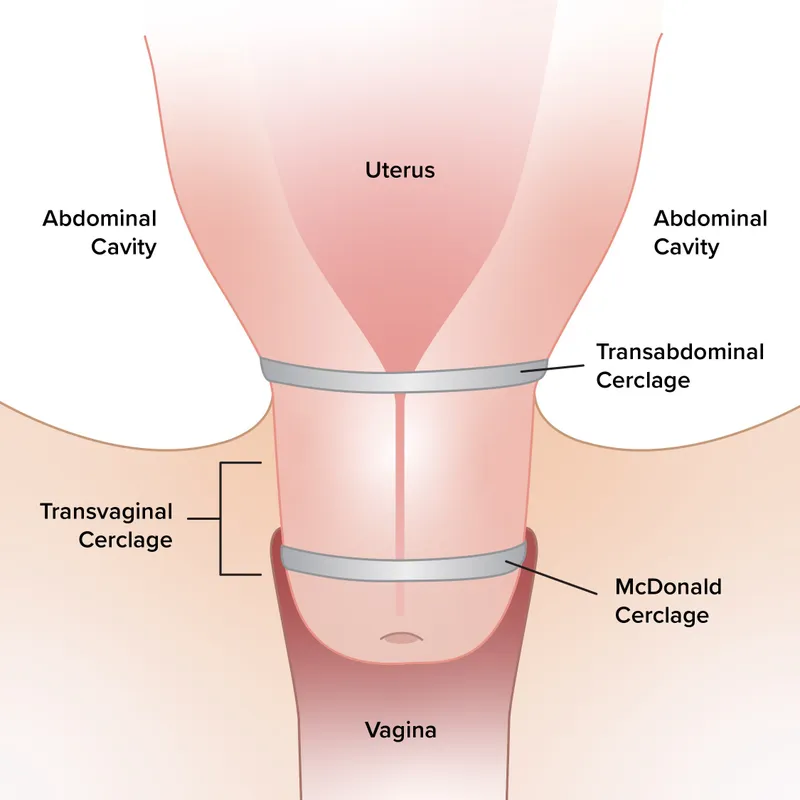
⭐ McDonald cerclage is the most commonly performed procedure and is technically simpler than Shirodkar.
- Timing: Ideally placed between 12-14 weeks gestation for history-indicated; can be up to 24 weeks for ultrasound/exam-indicated.
- Contraindications: Active labor, chorioamnionitis, fetal anomaly incompatible with life, vaginal bleeding, PPROM.
- 📌 McDonald = Most common, More superficial stitch around cervix.
Cerclage Indications & Timing - The When and Why
- Goal: Prevent PTB due to cervical insufficiency.
- Types: See flowchart (Prophylactic, Therapeutic, Rescue).
- Contraindications: Active labor, infection (chorioamnionitis), PPROM, fetal demise/major anomaly, significant bleeding.
⭐ For singleton pregnancy with prior spontaneous PTB <34 wks, offer cerclage if TVS shows CL <25 mm before 24 wks.
Cerclage Types & Techniques - Suture Strategies

- Vaginal Cerclage Types:
- McDonald Cerclage:
- Technique: Simple purse-string suture (e.g., Mersilene tape, Prolene #1) at the cervicovaginal junction.
- Timing: Insert 12-14 weeks; Remove 36-37 weeks or at onset of labor.
- Pros: Simpler, less dissection. Cons: Higher risk of suture slippage/displacement.
- Shirodkar Cerclage (Modified):
- Technique: Submucosal dissection (anterior & posterior) to place suture (e.g., Mersilene tape) as high as possible, near internal os.
- Timing: Insert 12-14 weeks; Remove 36-37 weeks or suture may be left if Cesarean delivery planned.
- Pros: Stronger, lower displacement risk. Cons: More complex, ↑ risk of cervical trauma, bladder/rectum injury.
- McDonald Cerclage:
- Abdominal Cerclage (Transabdominal Cervicoisthmic Cerclage - TAC):
- Indications: Prior failed vaginal cerclages, congenitally short cervix, amputated cervix (e.g., post-trachelectomy), severe scarring.
- Technique: Suture (e.g., Mersilene tape) placed at the cervicoisthmic junction via laparotomy or laparoscopy.
- Timing: Ideally pre-conceptional or in early pregnancy (~10-12 weeks).
- Delivery: Requires Cesarean section.
⭐ The Shirodkar technique aims to place the suture as close as possible to the level of the internal os for better anatomical support and efficacy, especially in cases with a significantly shortened or effaced cervix.
Cerclage Complications & Care - Post-Stitch Pointers
- Complications:
- Immediate: Bleeding, Anesthetic risks, Premature Rupture of Membranes (PROM), Chorioamnionitis, Cervical trauma/laceration.
- Delayed: Suture displacement/migration, Cervical stenosis/dystocia, Preterm Labor (PTL), PPROM, Infection, Uterine rupture (rare, if in situ during active labor).
- Post-Operative Care:
- Monitoring: Uterine activity, Fetal Heart Rate (FHR), vaginal bleeding, signs of infection (fever, foul discharge).
- Tocolysis: Prophylactic use not routine; consider for persistent uterine contractions.
- Antibiotics: Perioperative course common; regimen varies.
- Discharge: 24-48h post-op if stable.
- Follow-up & Advice:
- Activity: Pelvic rest (coitus avoidance), modified physical activity.
- Patient Education: Counsel on recognizing PTL, PPROM, infection symptoms.
- Suture Removal:
- Elective: 36-37 weeks gestation.
- Emergency: For active PTL, PPROM, chorioamnionitis.
- ⭐ > Cerclage in situ during labor significantly ↑ risk of cervical laceration or uterine rupture.
High‑Yield Points - ⚡ Biggest Takeaways
- Indications include history-indicated (≥1 late miscarriage/PTB), ultrasound-indicated (short cervix <25mm before 24wks with prior PTB), and exam-indicated/rescue (painless mid-trimester dilation).
- Common techniques are McDonald (simple purse-string, most common) and Shirodkar (requires bladder dissection, more complex).
- Elective placement is typically at 12-14 weeks; removal at 36-37 weeks or with onset of labor/PPROM.
- Rescue cerclage is placed for cervical dilation/effacement in mid-trimester; success rates are variable.
- Absolute contraindications include active labor, chorioamnionitis, PPROM, lethal fetal anomaly, and significant vaginal bleeding.
- Key risks involve PPROM, chorioamnionitis, cervical laceration/trauma, and suture migration/displacement.
- Transabdominal cerclage may be considered after failed transvaginal cerclage or with very short/absent cervix.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

