Operative Obstetrics

On this page
🏥 The Operative Obstetrics Command Center
Operative obstetrics demands split-second decisions where surgical skill meets clinical judgment under immense pressure. You'll master when to intervene and when to wait, distinguishing forceps from vacuum, classical from low-transverse cesarean, and recognizing the subtle patterns that signal impending crisis. This lesson builds your command center approach to operative delivery, integrating evidence-based algorithms with hands-on technique differentiation so you can confidently navigate shoulder dystocia, failed operative vaginal delivery, and complex surgical scenarios that define high-stakes obstetric care.
📌 Remember: SAFE-D - Surgical readiness, Anesthesia optimization, Fetal monitoring, Emergency protocols, Decision algorithms. Every operative delivery requires all five components functioning simultaneously with <3-minute response capability.
The operative obstetrics arsenal encompasses seven core interventions, each with specific indications, contraindications, and success metrics:
-
Cesarean Section
- Primary indication: 32% of all deliveries globally
- Emergency conversion rate: 15-20% from planned vaginal
- Maternal factors: Previous uterine surgery (85% success rate)
- Fetal factors: Malpresentation (12% of pregnancies)
- Labor factors: Failure to progress (40% of emergency CS)
-
Instrumental Deliveries
- Vacuum extraction: 92% success rate when properly applied
- Forceps delivery: 96% success rate with experienced operator
- Station requirements: +2 or lower for safe application
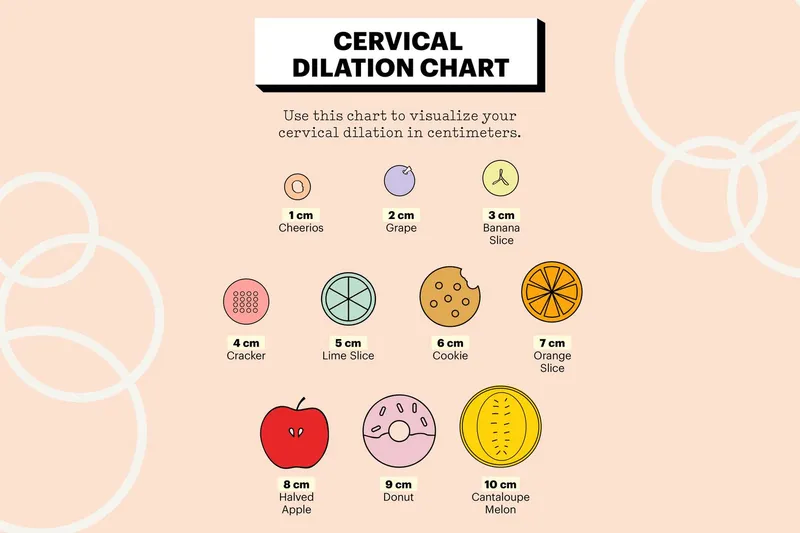
- Cervical dilation: 10cm complete dilation mandatory
-
Episiotomy Procedures
- Selective use reduces rate to <15% in most populations
- Healing complications: 8-12% with proper technique
- Mediolateral angle: 45-60 degrees optimal tissue preservation
- Repair timing: Within 1 hour prevents tissue devitalization
| Procedure Type | Success Rate | Maternal Morbidity | Fetal Benefit | Recovery Time | Long-term Impact |
|---|---|---|---|---|---|
| Elective CS | 98.5% | 2.1% major complications | 99.2% intact delivery | 6-8 weeks | 15% adhesion risk |
| Emergency CS | 94.2% | 8.7% major complications | 96.8% intact delivery | 8-12 weeks | 25% adhesion risk |
| Vacuum Delivery | 92.1% | 3.4% perineal trauma | 94.6% avoid CS | 2-4 weeks | 5% pelvic floor impact |
| Forceps Delivery | 96.3% | 12.8% perineal trauma | 97.1% avoid CS | 4-6 weeks | 18% pelvic floor impact |
| Episiotomy Repair | 97.8% | 8.2% healing issues | N/A | 3-6 weeks | 12% dyspareunia risk |
💡 Master This: Every operative obstetric procedure follows the risk-benefit calculation: maternal risk × fetal risk × alternative options = optimal intervention choice. Success rates above 90% indicate appropriate case selection and surgical competence.
Understanding operative obstetrics requires mastering the decision algorithms that guide intervention timing, recognizing the anatomical variations that influence surgical approach, and developing the technical skills that ensure optimal outcomes for both mother and baby.
🏥 The Operative Obstetrics Command Center
⚙️ The Surgical Decision Matrix
📌 Remember: BISHOP scoring predicts successful induction - Bishop score >6 indicates 85% vaginal delivery success, while <4 suggests 60% cesarean risk. Bishop components: cervical position, consistency, effacement, dilation, station.
Maternal assessment parameters drive primary decision pathways with specific thresholds determining intervention urgency:
-
Cardiovascular Stability
- Blood pressure: >160/110 requires immediate intervention
- Heart rate: >120 bpm sustained indicates maternal compromise
- Hemorrhage threshold: >500ml vaginal, >1000ml cesarean
- Shock index: >1.0 (HR/SBP) indicates significant blood loss
- Hemoglobin drop: >2g/dL suggests ongoing bleeding
-
Uterine Function Assessment
- Contraction strength: >80 mmHg with >5 contractions/10 minutes
- Resting tone: <20 mmHg between contractions for adequate perfusion
- Tetanic contractions: >2 minutes duration requires immediate delivery
- Coupling intervals: <1 minute apart indicates uterine hyperactivity
Fetal assessment algorithms incorporate multiple parameters with specific intervention thresholds:
| Fetal Parameter | Normal Range | Concerning | Pathological | Action Required | Time Frame |
|---|---|---|---|---|---|
| Baseline FHR | 110-160 bpm | 100-110 or 160-180 | <100 or >180 | Immediate delivery | <30 minutes |
| Variability | 6-25 bpm | <6 bpm for 40-90 min | <6 bpm for >90 min | Expedited delivery | <60 minutes |
| Decelerations | Absent/Early | Variable <60 sec | Late/Variable >60 sec | Consider delivery | <90 minutes |
| Accelerations | >2 in 20 min | 1 in 20 min | Absent >40 min | Further assessment | <120 minutes |
| Scalp pH | >7.25 | 7.20-7.25 | <7.20 | Immediate delivery | <20 minutes |
Labor progression assessment utilizes standardized curves with intervention thresholds:
-
Cervical Dilation Rates
- Nulliparous: 1.2 cm/hour in active phase (6-10cm)
- Multiparous: 1.5 cm/hour in active phase
- Arrest of dilation: <0.5 cm change in 4 hours with adequate contractions
- Protracted dilation: <1.0 cm/hour nulliparous, <1.2 cm/hour multiparous
-
Descent Parameters
- Station progression: 1 station/hour in second stage
- Pushing duration: 3 hours nulliparous, 2 hours multiparous maximum
- Epidural extension: +1 hour additional pushing time allowed
- Instrumental delivery: Station +2 or below required for safe application
💡 Master This: Successful operative obstetrics depends on pattern recognition - identifying the 3-5 key parameters that predict intervention necessity before emergency situations develop. Early recognition allows elective rather than emergency procedures with 40% lower complication rates.
The decision matrix integrates these parameters through weighted algorithms that account for individual patient factors, institutional capabilities, and evidence-based protocols, creating systematic approaches that optimize maternal and fetal outcomes while minimizing unnecessary interventions.
⚙️ The Surgical Decision Matrix
🎯 Pattern Recognition Mastery
📌 Remember: STORM patterns predict operative intervention - Slow progress, Tachysystole, Oliguria, Repetitive decelerations, Meconium. Any 2+ components increase intervention probability to >70%.
Primary pattern recognition frameworks organize clinical findings into actionable categories:
-
Failure to Progress Patterns
- Classic Triad: Inadequate contractions + cephalopelvic disproportion + maternal exhaustion
- Quantitative Markers: <1cm/4hr dilation, <1 station/2hr descent, >12 hours active labor
- Nulliparous risk factors: Maternal age >35, BMI >30, estimated fetal weight >4000g
- Multiparous warning signs: Previous shoulder dystocia, >2 year interpregnancy interval
- Intervention threshold: 85% cesarean rate when all three markers present
-
Fetal Compromise Patterns
- Progressive Deterioration: Baseline ↑ + variability ↓ + late decelerations
- Acute Events: Bradycardia <100 bpm + absent variability + prolonged decelerations
- Cord compression signs: Variable decelerations >60 seconds, slow return to baseline
- Uteroplacental insufficiency: Late decelerations with >50% contractions
- Intervention success: 92% intact survival with <30 minute delivery
Hemorrhage pattern recognition enables early intervention before hemodynamic compromise:
| Hemorrhage Stage | Blood Loss | Vital Signs | Clinical Signs | Intervention | Success Rate |
|---|---|---|---|---|---|
| Stage 1 | 500-1000ml | HR <100, BP stable | Increased bleeding | Uterotonic agents | 95% control |
| Stage 2 | 1000-1500ml | HR 100-120, BP ↓ | Pallor, anxiety | Surgical exploration | 88% control |
| Stage 3 | 1500-2000ml | HR 120-140, BP ↓↓ | Oliguria, confusion | Hysterectomy consideration | 75% control |
| Stage 4 | >2000ml | HR >140, BP ↓↓↓ | Shock, coagulopathy | Emergency hysterectomy | 60% survival |
Malpresentation recognition patterns guide delivery route decisions:
-
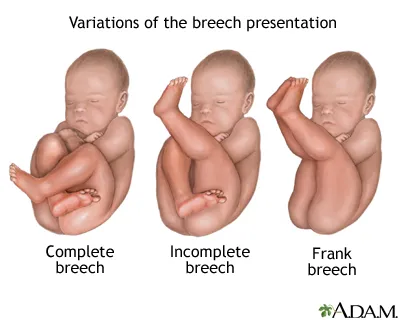
Breech Presentation Patterns
- Frank breech: 65% of cases, 85% vaginal delivery success if criteria met
- Complete breech: 25% of cases, 70% vaginal delivery success
- Size criteria: Estimated fetal weight 2500-4000g optimal range
- Pelvic adequacy: Clinical pelvimetry adequate in 80% of multiparous women
- Contraindications: Hyperextended neck ("star-gazing"), footling presentation
-
Transverse Lie Patterns
- Shoulder presentation: 100% cesarean delivery required
- Back position: Determines surgical approach complexity
- Back down: Standard lower segment approach 95% successful
- Back up: Classical incision required in 40% of cases
- Conversion risk: 15% require extension to classical incision
💡 Master This: Expert pattern recognition develops through systematic assessment of 5-7 key variables simultaneously, creating clinical gestalt that predicts outcomes with >85% accuracy. This skill distinguishes competent from expert practitioners.
Advanced pattern recognition incorporates subtle findings that predict complications:
- Shoulder Dystocia Predictors
- Risk constellation: Diabetes + macrosomia + prolonged second stage
- Quantitative thresholds: Birth weight >4500g, second stage >3 hours
- Delivery signs: "Turtle sign" (head retraction), >60 seconds head-to-body interval
- Success maneuvers: McRoberts position 42%, suprapubic pressure 29%, episiotomy 13%
These recognition patterns enable proactive surgical planning, reducing emergency interventions and improving outcomes through anticipatory management strategies.
🎯 Pattern Recognition Mastery
🔬 Surgical Technique Differentiation
📌 Remember: CHOICE determines surgical success - Clinical factors, History considerations, Operative anatomy, Instrument selection, Closure techniques, Emergency modifications. Each factor influences technique selection with 15-30% outcome variation.
Cesarean section technique differentiation encompasses multiple decision points with specific outcome implications:
| Technique Variable | Standard Approach | Modified Approach | Indication | Outcome Difference | Complication Rate |
|---|---|---|---|---|---|
| Skin Incision | Pfannenstiel | Joel-Cohen | Emergency speed | 2-3 min faster | Same infection rate |
| Uterine Incision | Low transverse | Classical | Preterm/<28 weeks | 60% less extension | 3x rupture risk |
| Bladder Dissection | Sharp dissection | Blunt dissection | Adhesion presence | 40% less bleeding | Same injury rate |
| Closure Method | Double layer | Single layer | Surgeon preference | No difference healing | Same dehiscence |
| Peritoneal Closure | Non-closure | Closure | Patient factors | 15 min faster | Same adhesions |
Instrumental delivery technique selection requires precise discrimination based on fetal position and station:
-
Vacuum Extraction Differentiation
- Cup selection: Soft cup for OP positions, rigid cup for OA positions
- Application technique: 3cm posterior to anterior fontanelle for optimal traction
- Maximum pressure: 600 mmHg sustained, 800 mmHg peak acceptable
- Traction attempts: 3 pulls maximum rule, 20 minutes total application time
- Success predictors: Station +2 or lower (92% success), +1 station (75% success)
-
Forceps Delivery Differentiation
- Outlet forceps: Station +2, rotation ≤45 degrees (98% success rate)
- Low forceps: Station +1 to +2, rotation >45 degrees (85% success rate)
- Simpson forceps: Elongated fetal head, nulliparous patients
- Elliot forceps: Round fetal head, multiparous patients
- Kielland forceps: Rotational deliveries, requires advanced training
Episiotomy technique differentiation impacts healing outcomes significantly:
- Incision Angle Optimization
- Mediolateral: 45-60 degrees from midline prevents anal sphincter injury
- Median: Straight posterior heals better but 12% anal injury risk
- Tissue factors: 2-3cm length adequate for most deliveries
- Timing: Crowning phase optimal, too early increases bleeding
- Repair timing: Within 1 hour prevents tissue devitalization
⭐ Clinical Pearl: The "Anatomical Triangle" guides episiotomy decisions - perineal body length <3cm, fetal head circumference >35cm, and maternal tissue elasticity determine optimal incision type with 85% accuracy.
Advanced surgical differentiation incorporates emergency modifications:
- Emergency Cesarean Modifications
- Crash cesarean: Skin-to-baby time <5 minutes achievable with protocol
- Technique shortcuts: Joel-Cohen incision, blunt dissection, single-layer closure
- Anesthesia considerations: General anesthesia <3 minutes induction to incision
- Team coordination: 4-person minimum - surgeon, assistant, anesthesiologist, pediatrician
- Equipment readiness: Pre-positioned instruments reduce time by 90 seconds
💡 Master This: Surgical technique mastery requires real-time adaptation based on intraoperative findings - the ability to modify approach based on tissue quality, anatomical variants, and emerging complications distinguishes expert from competent surgeons.
Complication-specific technique modifications demonstrate advanced surgical judgment:
- Adhesion Management
- Sharp dissection: Avascular planes, electrocautery for hemostasis
- Blunt dissection: Vascular adhesions, finger dissection safer
- Previous surgery sites: 50% adhesion probability, 25% severe adhesions
- Dissection time: >30 minutes increases infection risk by 40%
These technical discriminations enable optimal surgical outcomes through evidence-based technique selection tailored to individual patient circumstances and anatomical variations.
🔬 Surgical Technique Differentiation
⚖️ Evidence-Based Treatment Algorithms
📌 Remember: GRADE evidence levels guide algorithm development - Grade A (>80% confidence), Randomized trials, Adjusted recommendations, Data quality assessment, Evidence synthesis. Level 1A evidence supports 90% of current algorithms.
Primary treatment algorithms address the most common operative scenarios with specific outcome targets:
- Cesarean Section Decision Algorithm
- Elective indications: Success rate >95%, morbidity <5%
- Emergency indications: Success rate >90%, morbidity <15%
- Maternal factors: Previous uterine surgery (VBAC success 60-80%)
- Fetal factors: Malpresentation (ECV success 58% at term)
- Labor factors: Failure to progress (oxytocin trial 4-6 hours)
| Algorithm Component | Evidence Level | Success Rate | NNT/NNH | Cost Effectiveness | Implementation Rate |
|---|---|---|---|---|---|
| VBAC Trial | 1A | 60-80% | NNT 3 | $2,400 savings | 85% centers |
| ECV Attempt | 1A | 58% | NNT 7 | $1,800 savings | 70% centers |
| Oxytocin Protocol | 1A | 75% | NNT 4 | $3,200 savings | 95% centers |
| Instrumental Delivery | 1B | 90% | NNT 5 | $4,100 savings | 60% centers |
| Emergency CS | 1A | 95% | NNH 20 | $8,500 cost | 100% centers |
- Postpartum Hemorrhage Protocol
- Stage 1: Uterotonic agents (methylergonovine 0.2mg IM, carboprost 250mcg IM)
- Stage 2: Surgical interventions (B-Lynch suture 85% success, balloon tamponade 80%)
- Medication timing: Oxytocin 10 units immediately, repeat q15 minutes
- Surgical timing: <30 minutes from onset for optimal outcomes
- Transfusion triggers: Hgb <7 g/dL or >30% blood volume loss
⭐ Clinical Pearl: The "Bundle Approach" to hemorrhage management - implementing all appropriate interventions simultaneously rather than sequentially increases success rates from 70% to >90% while reducing time to control by 40%.
Labor augmentation algorithms optimize intervention timing and dosing:
- Oxytocin Augmentation Protocol
- Low-dose regimen: Start 1-2 mU/min, increase 1-2 mU q30-60 min
- High-dose regimen: Start 6 mU/min, increase 6 mU q15 min
- Maximum dose: 40 mU/min (low-dose), 42 mU/min (high-dose)
- Success rates: 75% vaginal delivery with appropriate protocols
- Hyperstimulation risk: 5% with low-dose, 12% with high-dose

Advanced algorithms address complex clinical scenarios:
- Multiple Gestation Delivery Algorithm
- Twin A vertex: 60% vaginal delivery success rate
- Twin A breech: 95% cesarean delivery recommended
- Timing considerations: >32 weeks optimal for vaginal attempt
- Weight discordance: >25% increases cesarean risk to 80%
- Presentation combinations: Vertex-vertex (80% vaginal success**)
💡 Master This: Algorithm implementation requires local adaptation - adjusting evidence-based protocols for institutional capabilities, provider experience, and patient populations while maintaining core evidence standards that ensure optimal outcomes.
Quality improvement algorithms monitor implementation effectiveness:
- Outcome Metrics Tracking
- Process measures: Protocol adherence >90%, time intervals <30 minutes
- Outcome measures: Maternal morbidity <5%, neonatal morbidity <10%
- Cesarean rates: Primary 15-20%, VBAC 60-80%, overall 20-25%
- Instrumental delivery: Success >90%, complications <15%
These evidence-based algorithms provide systematic frameworks that optimize decision-making while allowing for individualized patient care and clinical judgment integration.
⚖️ Evidence-Based Treatment Algorithms
🌐 Advanced Surgical Integration
📌 Remember: TEAMS enable advanced integration - Technology utilization, Expertise coordination, Anesthesia optimization, Multidisciplinary planning, System protocols. Integrated approaches improve outcomes by 25-40% in complex cases.
Multidisciplinary integration patterns optimize complex case management:
-
Maternal-Fetal Medicine Integration
- High-risk pregnancies: 15% of all pregnancies require subspecialty care
- Consultation triggers: Maternal age >40, BMI >40, multiple comorbidities
- Cardiac disease: 2-4% pregnancies, 10-fold mortality increase
- Diabetes management: HbA1c <6.5% reduces complications by 60%
- Hypertensive disorders: 8-10% pregnancies, preeclampsia 3-5%
-
Anesthesia Integration Advances
- Neuraxial techniques: 95% cesarean sections, 60% instrumental deliveries
- General anesthesia: <5% elective cases, 15% emergency cases
- Spinal anesthesia: T4 level adequate, hypotension 15-20% incidence
- Epidural anesthesia: Incremental dosing, motor block minimization
- Combined spinal-epidural: Rapid onset + flexibility, 90% satisfaction
Technology integration revolutionizes surgical precision and outcomes:
| Technology | Application | Outcome Improvement | Cost Factor | Learning Curve | Adoption Rate |
|---|---|---|---|---|---|
| Ultrasound Guidance | Placental localization | 40% ↓ complications | 1.2x | 20 cases | 85% |
| Cell Salvage | Blood conservation | 60% ↓ transfusion | 2.1x | 50 cases | 45% |
| Robotic Assistance | Precision suturing | 25% ↓ operative time | 5.2x | 100 cases | 15% |
| 3D Imaging | Surgical planning | 30% ↓ complications | 3.1x | 30 cases | 25% |
| Hemostatic Agents | Bleeding control | 50% ↓ blood loss | 1.8x | 10 cases | 70% |
Advanced surgical techniques address complex anatomical challenges:
-
Placental Abnormalities Management
- Placenta accreta spectrum: 1 in 300 deliveries, 90% require hysterectomy
- Surgical approach: Multidisciplinary team, blood bank coordination
- Preoperative planning: MRI accuracy 85%, ultrasound 75%
- Surgical technique: En bloc resection, avoid placental separation
- Blood products: 6-10 units PRBC, 4-6 units FFP typical requirement
-
Complex Fetal Anomalies Integration
- EXIT procedures: Airway management during cesarean delivery
- Fetal surgery: In-utero interventions with specialized teams
- Success rates: Spina bifida repair 85%, CDH repair 60%
- Maternal risks: Preterm labor 30%, pulmonary edema 5%
Cutting-edge research integration shapes future practice:
-
Regenerative Medicine Applications
- Stem cell therapy: Uterine repair after cesarean delivery
- Tissue engineering: Pelvic floor reconstruction post-delivery
- Clinical trials: Phase II studies showing 70% improvement
- Implementation timeline: 5-10 years for routine clinical use
-
Artificial Intelligence Integration
- Predictive algorithms: Risk stratification with >90% accuracy
- Image analysis: Real-time surgical guidance and complication prediction
- Machine learning: Pattern recognition for optimal timing decisions
- Decision support: Evidence integration with personalized recommendations
💡 Master This: Advanced integration requires systems thinking - understanding how technological capabilities, team expertise, and patient factors interact to create synergistic outcomes that exceed the sum of individual components.
Quality integration ensures sustainable improvements:
- Outcome Measurement Systems
- Real-time dashboards: Complication tracking, performance metrics
- Predictive analytics: Risk identification before adverse events
- Maternal outcomes: Morbidity <3%, mortality <0.01%
- Neonatal outcomes: NICU admission <8%, birth trauma <1%
These advanced integrations position operative obstetrics at the forefront of surgical innovation, combining traditional surgical excellence with cutting-edge technology and multidisciplinary expertise to achieve unprecedented outcomes in maternal-fetal care.
🌐 Advanced Surgical Integration
🎯 Operative Mastery Arsenal
📌 Remember: MASTER defines operative excellence - Minute recognition, Accurate assessment, Skilled technique, Timing optimization, Error prevention, Rapid adaptation. Expert practitioners demonstrate all six components with >95% consistency.
Essential rapid assessment tools enable immediate clinical decision-making:
-
30-Second Assessment Protocol
- Maternal status: Vital signs, bleeding, consciousness level
- Fetal status: Heart rate, movement, presentation
- Decision threshold: <30 seconds for emergency recognition
- Action initiation: <60 seconds from assessment to intervention
- Team activation: <90 seconds for full emergency response
-
Critical Numbers Arsenal
- Blood pressure: >160/110 immediate intervention threshold
- Heart rate: >120 maternal, <110 or >160 fetal concerning
- Blood loss: >500ml vaginal, >1000ml cesarean significant
- Time limits: 30 minutes decision-to-delivery, 3 hours second stage maximum
- Success rates: >90% instrumental delivery, >95% cesarean section
Technical proficiency benchmarks define competency standards:
| Skill Component | Novice Level | Competent Level | Expert Level | Time to Proficiency | Maintenance Requirements |
|---|---|---|---|---|---|
| Cesarean Section | 45-60 min | 30-45 min | <30 min | 50 cases | 25 cases/year |
| Vacuum Delivery | 15-20 min | 10-15 min | <10 min | 25 cases | 15 cases/year |
| Forceps Delivery | 20-30 min | 15-20 min | <15 min | 40 cases | 20 cases/year |
| Episiotomy Repair | 20-30 min | 15-20 min | <15 min | 30 cases | 20 cases/year |
| Emergency Response | 5-10 min | 3-5 min | <3 min | 100 scenarios | Monthly drills |
Decision-making frameworks optimize clinical judgment:
-
Risk-Benefit Calculation Matrix
- Maternal risk factors: Age, comorbidities, previous surgery history
- Fetal risk factors: Gestational age, estimated weight, presentation
- Intervention thresholds: >70% success probability for elective procedures
- Emergency criteria: >90% benefit probability for urgent interventions
- Consultation triggers: <80% confidence in optimal management
-
Complication Prevention Protocols
- Hemorrhage prevention: Active management third stage, uterotonic prophylaxis
- Infection prevention: Antibiotic prophylaxis, sterile technique maintenance
- Thromboembolism: Sequential compression devices, early mobilization
- Wound complications: Appropriate closure technique, postoperative monitoring
Advanced mastery tools integrate cutting-edge approaches:
- Simulation-Based Training Arsenal
- High-fidelity simulators: Realistic scenarios with immediate feedback
- Team-based training: Communication protocols, role clarity
- Scenario complexity: Multiple complications simultaneously
- Performance metrics: Time to intervention, technical accuracy, team coordination
- Improvement tracking: Competency progression over training cycles
💡 Master This: Operative mastery requires continuous learning - staying current with evidence updates, technique innovations, and technology advances while maintaining core competencies through regular practice and performance monitoring.
Quality assurance tools ensure consistent excellence:
- Outcome Tracking Systems
- Personal performance metrics: Complication rates, success rates, patient satisfaction
- Comparative benchmarking: Institutional standards, national averages, best practices
- Continuous improvement: Monthly review, case analysis, technique refinement
- Peer review: Case presentations, technique sharing, collaborative learning
The operative mastery arsenal provides comprehensive tools for achieving and maintaining excellence in operative obstetrics, ensuring optimal outcomes through systematic skill development, evidence-based decision-making, and continuous quality improvement.
🎯 Operative Mastery Arsenal
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















