Perinatal Mortality and Morbidity - Setting the Stage
- Perinatal Period:
- WHO: From 22 completed weeks gestation to 7 completed days after birth.
- India (National): From 28 completed weeks gestation to 7 completed days after birth.
- Birth weight criteria: >500g (WHO) or >1000g (India, if gestation unknown).
- Stillbirth (SB): Fetal death at or after 28 weeks gestation (India) or 22 weeks (WHO), before/during birth.
- Neonatal Death (NND): Death of a live-born infant within the first 28 completed days of life.
- Early NND: Death in the first 7 days.
- Late NND: Death from 7 up to 28 days.
- Perinatal Mortality Rate (PMR): $PMR = \frac{\text{(Stillbirths + Early Neonatal Deaths)}}{\text{Total Births (Live Births + Stillbirths)}} \times 1000$
- Stillbirth Rate (SBR): $SBR = \frac{\text{Stillbirths}}{\text{Total Births}} \times 1000$
- Neonatal Mortality Rate (NMR): $NMR = \frac{\text{Neonatal Deaths}}{\text{Live Births}} \times 1000$
⭐ India's approximate PMR (SRS 2020) is 20 per 1000 total births. The global target (Every Newborn Action Plan - ENAP) is <12 per 1000 births by 2030.
Perinatal Mortality and Morbidity - The Why Behind Loss
Key etiological factors, especially relevant in India:
- Prematurity & LBW: Leading overall cause.
- Birth Asphyxia: Major preventable factor.
- Infections: Maternal (e.g., TORCH, sepsis) & neonatal.
- Congenital Anomalies: Structural/functional defects.
- Maternal Conditions: Severe anemia, hypertensive disorders, diabetes.
Breakdown of Causes:
| Category | Examples |
|---|---|
| Maternal | Anemia, Hypertensive disorders (Pre-eclampsia), Infections, Malnutrition, APH, Age (<20 or >35) |
| Fetal | Prematurity, Congenital anomalies, IUGR, Birth asphyxia, Multiple gestation |
| Placental | Insufficiency, Abruption, Previa, Cord prolapse/knots |
| Intrapartum | Obstructed labor, Prolonged labor, Birth trauma, Asphyxia |
| Neonatal | Respiratory Distress Syndrome (RDS), Sepsis, Hypothermia, Severe jaundice |
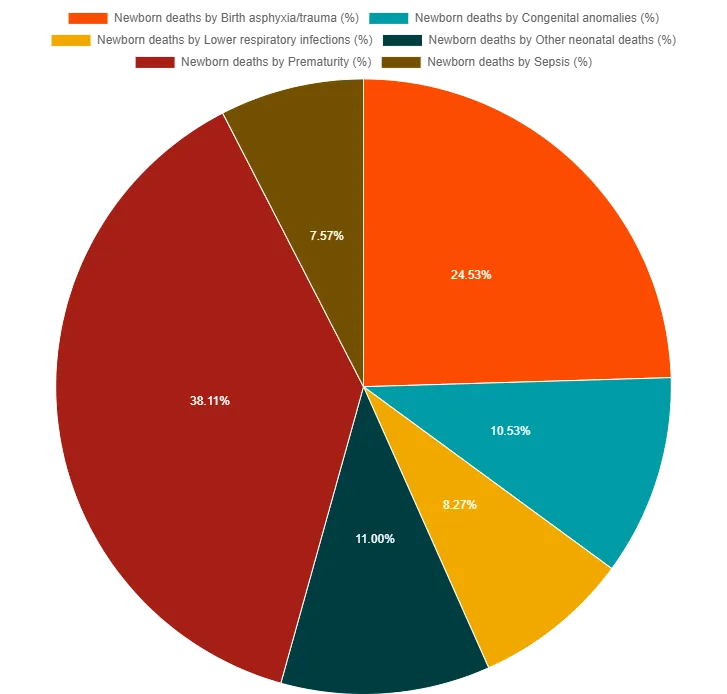
⭐ In India, approximately 20-25% of perinatal deaths are attributed to birth asphyxia and trauma, highlighting the critical need for skilled obstetric and neonatal care during delivery and immediately postpartum.
Perinatal Mortality and Morbidity - Surviving with Scars
- Hypoxic-Ischemic Encephalopathy (HIE): Brain injury from perinatal asphyxia.
- Sarnat Staging: I (mild), II (moderate), III (severe).
- Therapeutic hypothermia for moderate/severe HIE within 6 hours.
- Sequelae: Cerebral palsy, epilepsy, cognitive impairment.
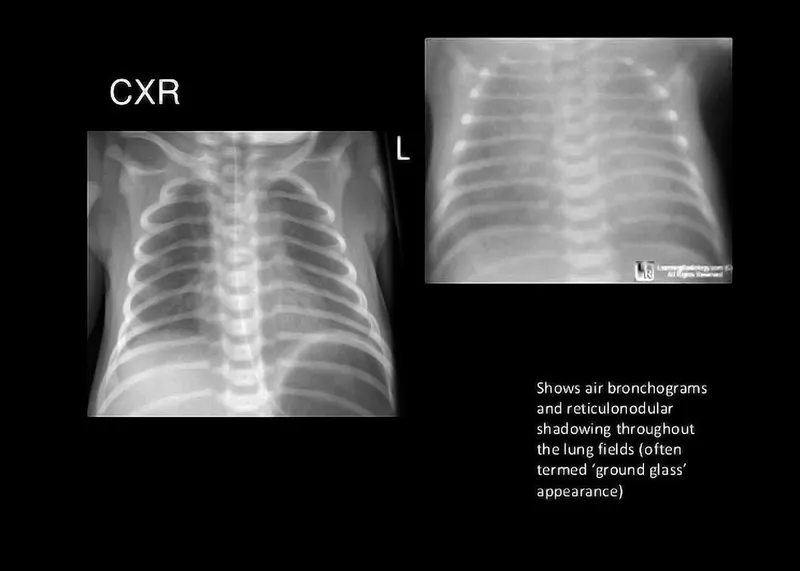
- Respiratory Distress Syndrome (RDS): Surfactant deficiency in preterms (<34 weeks).
- CXR: Ground-glass, air bronchograms.
- Rx: Antenatal steroids, surfactant, CPAP.
- Complications: Bronchopulmonary dysplasia (BPD), Retinopathy of Prematurity (ROP).
- Neonatal Sepsis:
- Early onset (<72h): Maternal Group B Streptococcus (GBS), E. coli.
- Late onset (>72h): Nosocomial/community.
- Rx: IV antibiotics.
- Birth Injuries:
- Brachial plexus: Erb's palsy (C5-C6), Klumpke's palsy (C8-T1).
- Fractures: Clavicle (most common).
- Cephalohematoma (subperiosteal, respects sutures).
⭐ Severe HIE (Stage III) is a major predictor of long-term neurodevelopmental disabilities like cerebral palsy and severe cognitive deficits.
Perinatal Mortality and Morbidity - Saving Tiny Lives
Perinatal Mortality Rate (PMR): Deaths from 22 weeks gestation to 7 days post-birth per 1000 total births. Key causes: prematurity, birth asphyxia, infections, congenital anomalies.
Wigglesworth Classification of Perinatal Deaths:
| Group | Description |
|---|---|
| I | Congenital Malformations |
| II | Unexplained Antepartum Stillbirth |
| III | Intrapartum Asphyxia (Fresh SB or NND) |
| IV | Immaturity-related Conditions |
| V | Specific Other Causes (e.g., Infection, Trauma) |
- Antenatal: ≥4 ANC visits, Iron-Folic Acid, Tetanus Toxoid, High-risk screening.
- Intrapartum: Skilled birth attendance, Clean delivery (5 Cs), Essential Newborn Care (ENC).
- Postnatal: Kangaroo Mother Care (KMC), Exclusive breastfeeding, Danger sign recognition.
Perinatal Death Audit Steps:
⭐ Kangaroo Mother Care (KMC) is a high-impact, low-cost intervention proven to reduce mortality by up to 40% in stable preterm infants.
High-Yield Points - ⚡ Biggest Takeaways
- Perinatal period: 22 weeks gestation to 7 days post-birth.
- PMR: Stillbirths (≥28 wks) + Early Neonatal Deaths (≤7 days) per 1000 total births.
- NMR: Deaths in first 28 days of life per 1000 live births.
- Leading causes of PMR: Prematurity, birth asphyxia, infections, congenital anomalies.
- IUGR significantly ↑ perinatal morbidity & mortality.
- Key maternal risk factors: Hypertension, diabetes, anemia, maternal infections.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

