Neonatal Jaundice Basics - Yellow Alert Intro
- Jaundice: Visible if Total Serum Bilirubin (TSB) > 5 mg/dL.
- Types: Physiological (common, benign) vs. Pathological (concerning).
- Physiological: Appears after 24 hrs, TSB usually < 15 mg/dL. 📌 Physiological = Post 24h.
- Pathological: Within 24 hrs, rapid TSB rise (>5 mg/dL/day), high direct bilirubin (>2 mg/dL or >20% TSB), or prolonged.
- Bilirubin: Unconjugated (neurotoxic) → Conjugated (excreted) via UGT enzyme.

⭐ Jaundice in the first 24 hours of life is ALWAYS pathological and requires urgent investigation.
Etiology Exploration - Unmasking the Causes
- Unconjugated Hyperbilirubinemia (Indirect Bilirubin ↑)
- Increased Production (Hemolysis)
- Isoimmune: Rh, ABO incompatibility
- RBC enzyme defects: G6PD deficiency
- RBC membrane defects: Spherocytosis
- Sepsis, Cephalohematoma
- Decreased Conjugation/Excretion
- Physiological jaundice (peaks day 3-5)
- Crigler-Najjar syndrome, Gilbert syndrome
- Hypothyroidism
- Breast milk jaundice (onset after day 7, prolonged)
- Breastfeeding failure jaundice (early, poor intake)
- Increased Production (Hemolysis)
- Conjugated Hyperbilirubinemia (Direct Bilirubin ↑ >2 mg/dL or >20% TSB)
- Biliary Obstruction: Biliary atresia, Choledochal cyst
- Neonatal Hepatitis: Idiopathic, Infections (TORCH, sepsis)
- Metabolic Disorders: Galactosemia, Tyrosinemia, A1AT deficiency
- Genetic Syndromes: Dubin-Johnson, Rotor syndrome
⭐ ABO incompatibility is the most common cause of hemolytic disease of the newborn (HDN), often appearing within 24 hours of life.
Clinical & Diagnostic Clues - Jaundice Detective Work
- Clinical Eye:
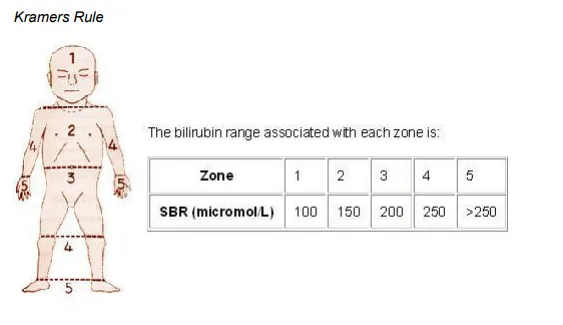
- Visual (Kramer's Zones, approx. TSB mg/dL): Face (4-6), Upper Trunk (8-10), Lower Trunk/Thighs (12-14), Arms/Legs (15-18), Palms/Soles (>15).
- ⚠️ Danger Signs: Jaundice <24 hrs; TSB ↑ >5 mg/dL/day or >0.2 mg/dL/hr; Prolonged (>2 wks term, >3 wks preterm); Acute Bilirubin Encephalopathy (ABE) signs (lethargy, poor feeding).
- Lab Investigations:
- Core: TSB (total & direct), Blood group (baby & mother, Rh), Direct Coombs Test (DCT).
- Guided: Hb/PCV, Reticulocyte count, Peripheral smear (RBC morphology), G6PD screen, Sepsis screen, Thyroid function (if prolonged).
⭐ Jaundice in the first 24 hours of life is ALWAYS pathological and warrants immediate investigation.
Management Strategies - Beating Bilirubin
- Phototherapy (PT):
- Mechanism: Converts bilirubin to excretable photoisomers (lumirubin).
- Light: Blue-green (460-490 nm), irradiance ≥30 µW/cm²/nm.
- Indications: TSB thresholds per AAP/NNF guidelines (GA, age, risk factors).
- Side effects: Retinal damage (eye shields!), loose stools, dehydration, bronze baby. 📌 BILI

- Exchange Transfusion (ET):
- Indications: Failed intensive PT, rapidly rising TSB, ABE signs, or high TSB (e.g., >20-25 mg/dL term infant).
- Procedure: Double volume exchange (160-170 mL/kg).
- Complications: Hypocalcemia, ↓glucose, ↓platelets, arrhythmias, infection, NEC.
⭐ Double volume exchange transfusion replaces approximately 85% of the neonate's red blood cells and reduces bilirubin by about 50%.
- Pharmacological (Adjunctive):
- IVIG: For isoimmune hemolysis if TSB rises despite PT (0.5-1 g/kg).
Complications & Kernicterus - The Danger Zone
- Kernicterus: Chronic, irreversible bilirubin encephalopathy.
- Unconjugated bilirubin deposits in basal ganglia, brainstem nuclei.
- Bilirubin-Induced Neurologic Dysfunction (BIND):
- Acute: Lethargy, hypotonia, high-pitched cry, opisthotonus, seizures.
- Chronic: Choreoathetoid cerebral palsy, sensorineural hearing loss, dental dysplasia, upward gaze palsy.

⭐ Kernicterus classically involves bilirubin staining of the basal ganglia (globus pallidus, subthalamic nucleus), hippocampus, and cranial nerve nuclei (III, IV, VI, VIII).
High‑Yield Points - ⚡ Biggest Takeaways
- Physiological jaundice: Onset >24 hours, peaks 3-5 days, resolves by 1-2 weeks.
- Pathological jaundice: Onset <24 hours, TSB ↑ >5 mg/dL/day, or direct bilirubin >2 mg/dL.
- Kernicterus: Risk with high unconjugated bilirubin; causes brain damage.
- Phototherapy: Primary treatment; converts bilirubin to lumirubin.
- Exchange transfusion: For severe hyperbilirubinemia or signs of encephalopathy.
- Hemolytic causes: Include ABO/Rh incompatibility, G6PD deficiency.
- Breastfeeding jaundice vs. Breast milk jaundice: Differ by onset/etiology (intake vs. milk factors).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

