Overview & Teratogens - Blueprint Blips
- Malformation: Intrinsic, primary error in morphogenesis (e.g., anencephaly, cleft lip).
- Deformation: Extrinsic mechanical forces on normally developing structures (e.g., clubfoot due to oligohydramnios).
- Disruption: Secondary breakdown of, or interference with, an originally normal developmental process (e.g., amniotic band syndrome).
Key Teratogens & Effects:
| Teratogen | Major Adverse Effect(s) |
|---|---|
| Alcohol | Fetal Alcohol Syndrome (FAS): microcephaly, smooth philtrum, intellectual disability |
| Phenytoin | Fetal Hydantoin Syndrome: hypoplastic nails, craniofacial anomalies, IUGR |
| Valproate | Neural tube defects (NTDs), cardiac defects, distinct facies |
| Warfarin | Nasal hypoplasia, stippled epiphyses (chondrodysplasia punctata) |
| ACE Inhibitors | Renal tubular dysgenesis, oligohydramnios, skull hypoplasia |
| Isotretinoin | CNS, craniofacial (microtia), cardiac, thymic defects (highly teratogenic) |
| Lithium | Ebstein's anomaly (cardiac) |
| TORCH Infections | 📌 (Toxoplasmosis, Other (Syphilis, VZV, Parvo B19), Rubella, CMV, Herpes) - varied systemic effects, e.g., microcephaly, chorioretinitis, hepatosplenomegaly |
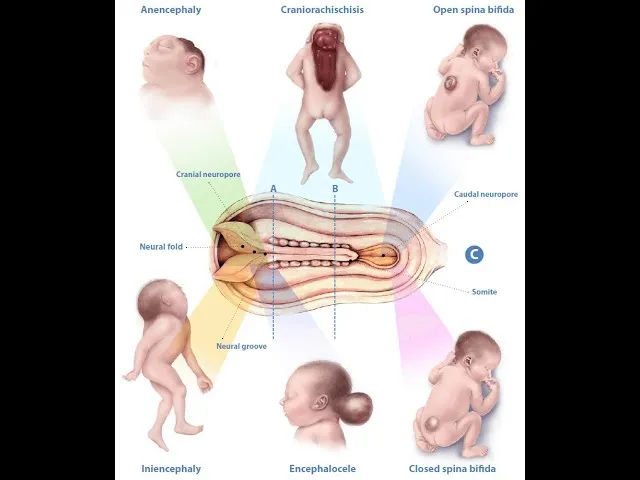
Neural Tube Defects - Spinal Surprises
Neural tube closure failure (3-4 wk gest). Key risk: folate deficiency. Prevention: Folic acid (0.4 mg/day general; 4 mg/day high-risk).
Types of Spina Bifida:
| Type | Defect | Sac Contents | Neurological Deficit |
|---|---|---|---|
| Spina Bifida Occulta | Vertebral defect, skin intact | None (tuft of hair) | Usually none |
| Meningocele | Meninges protrude | Meninges, CSF | Variable, mild |
| Myelomeningocele | Meninges & neural tissue protrude | Meninges, CSF, Cord | Always present |
| Myeloschisis | Exposed neural plate | Neural tissue | Severe |
- Anencephaly: No forebrain/skull.
- Encephalocele: Brain/meninges herniate via skull defect.
- Diagnosis: Prenatal US (lemon/banana signs), ↑MSAFP, ↑Amniotic AFP & AChE.
⭐ ↑MSAFP is a key screening marker for open NTDs.
Cardiac Defects - Tiny Ticker Troubles
Differentiating CHD:
Common Congenital Heart Defects:
| Defect | Type | Murmur | CXR Finding | Notes |
|---|---|---|---|---|
| VSD | Acyanotic | Holosystolic | ↑PVM | Most common CHD. |
| ASD | Acyanotic | Fixed split S2 | ↑PVM, Cardiomegaly | Ostium secundum type. |
| PDA | Acyanotic | Continuous "machine-like" | ↑PVM | Maternal rubella. |
| TOF | Cyanotic | Ejection Systolic | 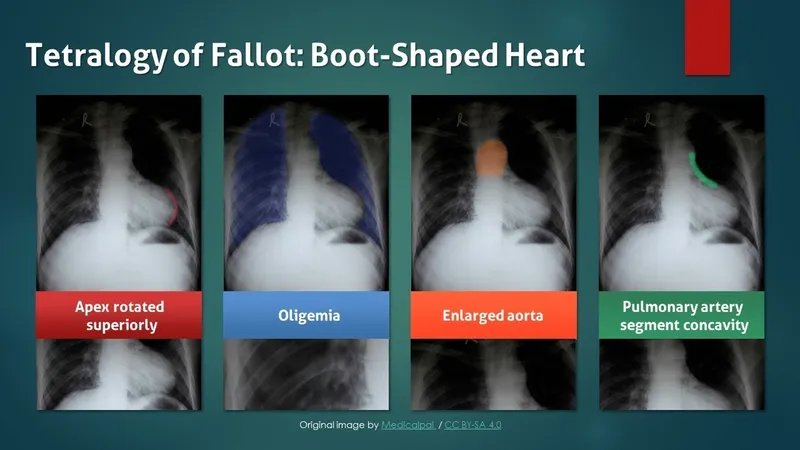 "Boot-shaped" "Boot-shaped" | 📌 PROVe; Tet spells. |
| TGA | Cyanotic | Single S2 |  "Egg-on-string" "Egg-on-string" | Needs shunt for survival. |
GI & Abdominal Wall Defects - Tummy Turmoil
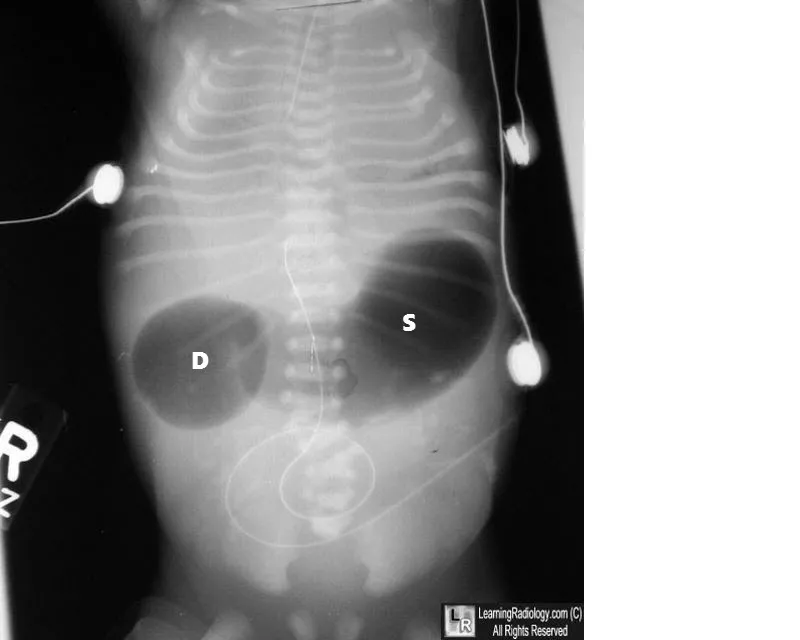
- Duodenal Atresia: ⭐
Significance of bilious vomiting in a neonate often indicates bowel obstruction distal to the ampulla of Vater, classically seen in duodenal atresia.
- Classic sign: "Double bubble" on X-ray.
- Associated with Down Syndrome (Trisomy 21).
- Abdominal Wall Defects:
| Feature | Omphalocele | Gastroschisis |
|---|---|---|
| Sac | Present (amnion/peritoneum) | Absent |
| Location | Midline, umbilical cord inserts at apex | Right of umbilicus, normal cord insertion |
| Contents | Bowel, liver, spleen | Bowel, rarely other organs |
| Bowel Appearance | Normal | Edematous, matted, inflamed |
| Associated Anomalies | Common (50-70%), cardiac, chromosomal (e.g., Trisomy 13, 18) | Less common (10-15%), primarily intestinal atresia |
| Maternal AFP | Often ↑ | Markedly ↑ |
* Most common type: Esophageal atresia with distal TEF (Type C, **~85%**).
* Presents with choking, coughing, cyanosis with feeds; inability to pass NG tube beyond **10-12 cm**.
- Neural Tube Defects (NTDs): Prevent with folic acid. Anencephaly (lethal), spina bifida (variable).
- VSD is most common CHD. Maternal rubella linked to PDA & other defects.
- Down Syndrome (Trisomy 21): Most common chromosomal disorder, intellectual disability.
- Cleft lip with or without cleft palate is the most common craniofacial anomaly.
- Congenital Diaphragmatic Hernia often causes pulmonary hypoplasia and severe respiratory distress.
- Esophageal atresia with tracheoesophageal fistula (TEF): Suspect with maternal polyhydramnios.
- TORCH infections are significant causes of multiple congenital anomalies_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

