Birth Injuries: Scalp Swellings & Risk Factors - Head Start Hurdles
- General Risk Factors: Macrosomia, malpresentation, operative delivery (forceps/vacuum), shoulder dystocia, precipitous labor.
📌 Mnemonic: Caput Crosses sutures. Hematoma Hesitates (at sutures). Subgaleal Spreads widely.
| Feature | Caput Succedaneum | Cephalohematoma | Subgaleal Hemorrhage |
|---|---|---|---|
| Location | Edema above periosteum | Subperiosteal bleed | B/w aponeurosis & periosteum |
| Sutures | Crosses | Does NOT cross | Crosses |
| Feel | Soft, pitting | Firm | Boggy, fluctuant, shifts |
| Resolution | 2-3 days | Weeks-months | Progressive; monitor! |
| Key Risks | Benign | Jaundice, calcification | Shock, massive blood loss, DIC |
⭐ Subgaleal hemorrhage is the most dangerous neonatal scalp injury due to its potential for massive blood loss and hypovolemic shock.
Birth Injuries: Nerve Palsies - Delivery Nerve Drama
-
Brachial Plexus Palsy (BPP): Brachial plexus nerve injury during delivery.
⭐ Erb's palsy (C5-C6) is the most common BPP in newborns.
- Types:
Feature Erb-Duchenne Palsy Klumpke's Palsy Nerve Roots C5-C6 📌 'पकड़ने में ERror, Bazu (arm) बेकार' C8-T1 Presentation 'Waiter's tip': adducted, int. rotated arm, extended elbow, flexed wrist 'Claw hand' Reflexes Absent Moro/biceps (affected side) Absent grasp reflex Associated - Horner's (ptosis, miosis, anhydrosis)
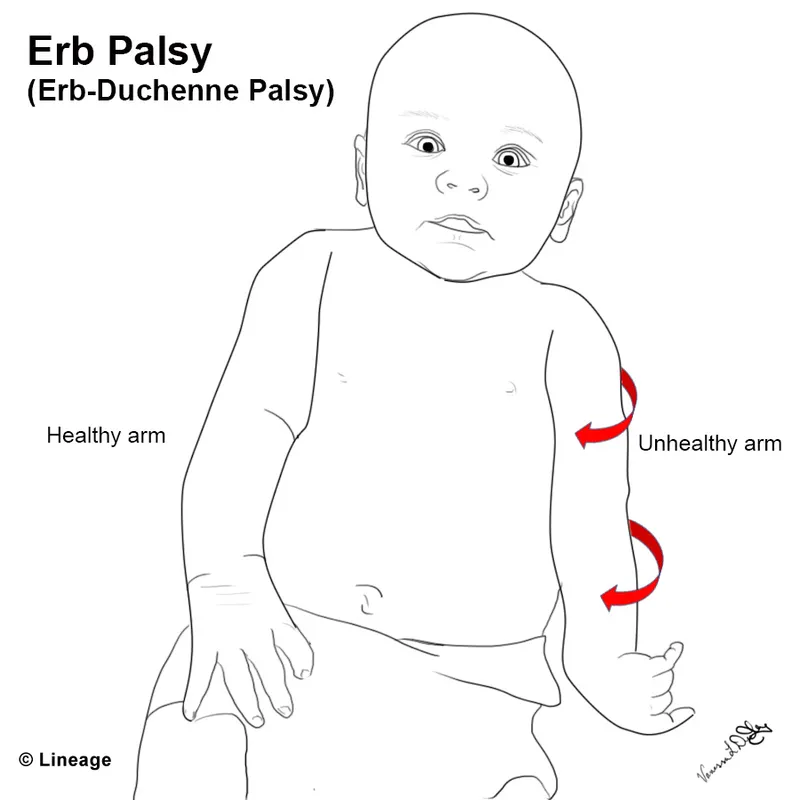
- Types:
-
Facial Nerve Palsy (CN VII):
- Cause: CN VII compression.
- Signs: Asymmetric crying facies (mouth to normal side, poor eye closure affected side).
- Prognosis: Often spontaneous resolution.
-
Phrenic Nerve Palsy (C3, C4, C5):
- Cause: Phrenic nerve injury.
- Signs: Diaphragmatic paralysis, respiratory distress, ↓ breath sounds (affected side).
- Mgmt: Ventilatory support if severe.
Birth Injuries: Bone Breaks & Muscle Strains - Skeletal Snaps
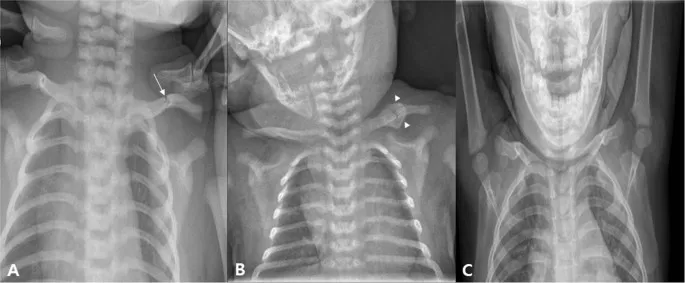
- Clavicular Fracture: Most common birth fracture, often mid-clavicle.
- Signs: Crepitus, palpable bony irregularity, asymmetric Moro reflex, infant irritable on handling.
- Management: Gentle handling, immobilize arm (pin sleeve to chest). Heals rapidly with callus.
⭐ The clavicle is the most frequently fractured bone during labor and delivery, often presenting with an absent Moro reflex on the affected side.
- Humeral Fracture: Usually shaft; from traction.
- Signs: Pain, crepitus, deformity, ↓ arm movement.
- ⚠️ Risk of radial nerve injury.
- Femoral Fracture: Rare; requires significant force.
- Signs: Deformity, swelling, pain on leg movement.
- Sternocleidomastoid Injury (Congenital Muscular Torticollis): SCM muscle hematoma/fibrosis.
- Head tilted to affected side, chin to opposite. Palpable 'tumor' in SCM.
- Head tilted to affected side, chin to opposite. Palpable 'tumor' in SCM.
Birth Injuries: Internal Organ Injuries - Visceral Vulnerabilities
- Liver Injury/Subcapsular Hematoma:
- 2nd most common abdominal injury.
- Risks: Macrosomia, breech, hepatomegaly.
- Signs: Anemia, shock, distension; rupture → hemoperitoneum.
- Splenic Rupture:
- Less common. Risks/presentation similar to liver (shock, anemia).
- Adrenal Hemorrhage:
- Common. Risks: Hypoxia, stress, trauma.
- Signs: Often asymptomatic; or mass, jaundice, anemia. Rarely adrenal insufficiency. Ultrasound aids diagnosis.

- Intracranial Hemorrhage (Traumatic):
- Subdural (SDH): Dural sinus/venous tears.
- Subarachnoid (SAH): Often asymptomatic/mild irritability. (Distinct from HIE-IVH).
⭐ Adrenal hemorrhage in a newborn can present with an abdominal mass, persistent jaundice, and anemia; it is often detected on ultrasound.
High‑Yield Points - ⚡ Biggest Takeaways
- Caput succedaneum crosses suture lines; cephalohematoma doesn't, is subperiosteal.
- Erb's palsy (C5-C6) causes waiter's tip deformity; Klumpke's palsy (C8-T1) causes claw hand ± Horner's syndrome.
- Clavicular fracture is the most common neonatal bony injury; presents with crepitus, asymmetric Moro reflex.
- Facial nerve palsy leads to asymmetric crying facies, often associated with forceps delivery.
- Subarachnoid hemorrhage is the most common type of neonatal intracranial bleed; subdural bleeds are often from tentorial tears.
- Phrenic nerve palsy (C3-C5) results in respiratory distress and unilateral diaphragmatic elevation on X-ray.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

