Implantation Issues - Sticky Situations
- Placenta Previa: Implantation in lower uterine segment over/near internal os.
- Types: Marginal, Partial, Complete. Low-lying: placenta edge within 2 cm of internal os.
- Risk factors: Prior C-section, multiparity, advanced maternal age (AMA), smoking.
⭐ Painless, causeless, recurrent vaginal bleeding in 3rd trimester.
- Diagnosis: Transvaginal sonography (TVS) is gold standard. ⚠️ Avoid per-vaginal examination.
- Placenta Accreta Spectrum (PAS): Abnormal adherence/invasion of chorionic villi into myometrium.
- Accreta: Villi attach to myometrium.
- Increta: Villi invade into myometrium.
- Percreta: Villi penetrate through myometrium, may invade adjacent organs (e.g., bladder).
- Risk factors: Prior C-section (especially with anterior previa), placenta previa, AMA.
- Diagnosis: Ultrasound (loss of retroplacental clear space, placental lacunae), MRI for posterior placenta/suspected percreta.
- Vasa Previa: Fetal vessels run near internal os, unprotected by placenta/umbilical cord. Rupture leads to fetal exsanguination.
- Associated with velamentous cord insertion, bilobed/succenturiate lobe placenta.
- Diagnosis: Antenatal USG with color Doppler. Apt test/Ogita test on vaginal blood.
Shape & Cord Capers - Odd Ones Out
- Abnormal Lobes/Shape:
- Succenturiate Lobe: Accessory placental lobe; risk of retained tissue, Post-Partum Hemorrhage (PPH).
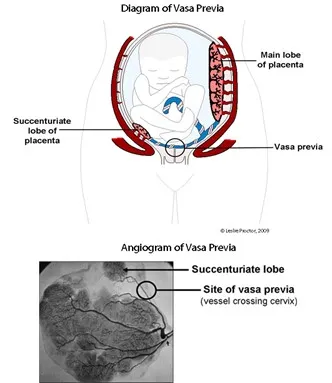
- Placenta Spuria: Detached accessory lobe, no connecting vessels.
- Circumvallate Placenta: Fetal membranes fold back on fetal surface; ↑risk of abruption, IUGR, Preterm Delivery (PTD).
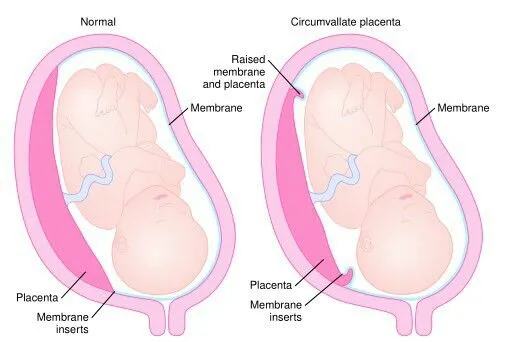
- Circummarginate Placenta: Similar, but flat transition; less clinically significant.
- Succenturiate Lobe: Accessory placental lobe; risk of retained tissue, Post-Partum Hemorrhage (PPH).
- Cord Insertion Anomalies:
- Battledore Placenta: Marginal cord insertion. Usually benign.

- Velamentous Insertion: Cord inserts into membranes; fetal vessels unprotected.

⭐ Velamentous cord insertion is associated with vasa previa and carries a high risk of fetal exsanguination if vessels rupture.
- Vasa Previa: Fetal vessels run over or near internal cervical os. High risk of rupture & fetal exsanguination.
- Battledore Placenta: Marginal cord insertion. Usually benign.
- Knots:
- False Knots: Benign; blood vessels appear as knots.
- True Knots: Rare; risk of fetal compromise/demise if tightened.
Abruption Alert - Sudden Separation

- Premature separation of normally implanted placenta after 20 weeks gestation.
- Classic triad: Sudden-onset painful vaginal bleeding, uterine tenderness/hypertonicity (tetany), fetal distress.
- Bleeding can be revealed, concealed, or mixed.
- Risk Factors: Maternal HTN (most common), trauma, smoking, cocaine, prior abruption, PPROM, polyhydramnios with rapid decompression.
- Complications: Maternal (DIC, shock, renal failure, Couvelaire uterus), Fetal (hypoxia, IUGR, prematurity, demise).
⭐ Concealed hemorrhage in placental abruption can lead to underestimation of blood loss and severe maternal/fetal compromise, including Couvelaire uterus (uteroplacental apoplexy).
Postpartum Placenta Problems - Lingering Issues
- Retained Placenta:
- Definition: Not expelled: 30 mins (active management), 60 mins (physiological).
- Causes: Uterine atony, trapped placenta (closed cervix), placenta accreta spectrum.
- Management: Controlled cord traction (CCT), IV oxytocin. Failure: manual removal (anesthesia).
- Complications: Primary PPH, endometritis, Asherman's syndrome (rare).
- Retained Placental Fragments (RPOC):
- Small placental pieces in uterus post-delivery.
- Symptoms: Secondary PPH (most common; bleeding >24h to 6-12 wks), uterine subinvolution, persistent foul lochia, low-grade fever.
- Diagnosis: Ultrasound (USG) showing endometrial mass/thickening >10-15mm, often with ↑vascularity.
- Management: Uterotonics, antibiotics (if infection suspected), D&C or hysteroscopic removal.
⭐ The most common cause of secondary PPH is retained placental fragments.
 OR medical illustration of manual placenta removal)
OR medical illustration of manual placenta removal) - Placental Polyp:
- Late complication: organized retained placental tissue forming a vascular endometrial mass/polyp.
- Symptoms: Intermittent or persistent abnormal vaginal bleeding, often weeks/months postpartum.
- Diagnosis: USG (color Doppler helpful), sonohysterography, direct visualization via hysteroscopy.
- Management: Hysteroscopic resection or D&C cautious of uterine perforation.
High‑Yield Points - ⚡ Biggest Takeaways
- Placenta previa: Painless bright red bleeding in late pregnancy; ultrasound for diagnosis; avoid PV exam.
- Abruptio placentae: Painful vaginal bleeding, tender, rigid uterus; associated with hypertension, trauma.
- Placenta accreta spectrum: Abnormal adherence to myometrium; previous C-section is a major risk; high risk of massive PPH.
- Vasa previa: Fetal vessels over internal os; painless bleeding at ROM with fetal bradycardia.
- Succenturiate lobe: Risk of retained placental tissue leading to PPH.
- Velamentous cord insertion: Unprotected vessels; risk of rupture and fetal hemorrhage.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

