Multiple Gestation - Double Trouble ID
- Types:
- Dizygotic (DZ): Fertilization of 2 ova; always dichorionic-diamniotic (DCDA).
- Monozygotic (MZ): Fertilization of 1 ovum, then splits. Chorionicity depends on timing of split:
- 0-3 days: DCDA (30%)
- 4-8 days: Monochorionic-diamniotic (MCDA) (70%)
- 9-12 days: Monochorionic-monoamniotic (MCMA) (1%)
-
13 days: Conjoined twins (<1%)
- Epidemiology: ↑ with Assisted Reproductive Technology (ART), ↑ maternal age, family history.
- Identification (Ultrasound):
- Number of gestational sacs.
- Chorionicity:
- T-sign: MCDA (thin membrane)
- Lambda (λ) sign / Twin peak sign: DCDA (thick membrane)
- Number of fetuses, fetal heart activity.
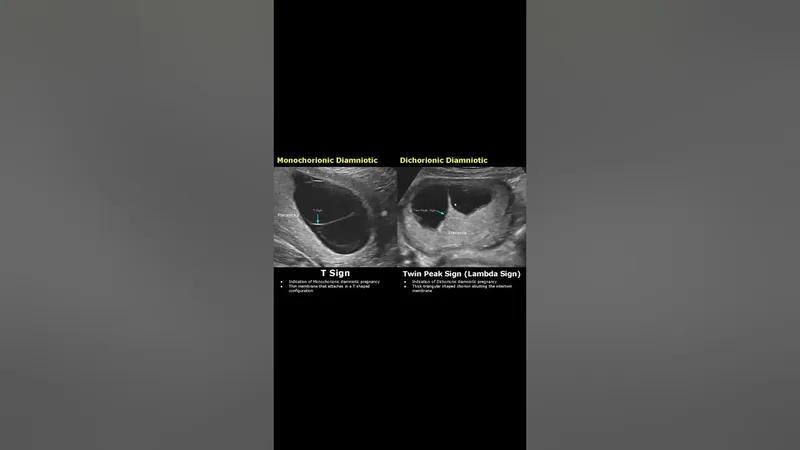
⭐ Chorionicity (determined by ultrasound via T-sign/Lambda sign) is the single most important prognostic factor in twin pregnancies.
📌 Mnemonic (Zygosity & Chorionicity): Dizygotic = Different eggs = Dichorionic. Monozygotic = Maybe one or two chorions (depends on split time).
Multiple Gestation - Mom's Twin Trials
- Physiological Changes (Exaggerated):
- ↑ Cardiac output (by 20% more than singleton)
- ↑ Plasma volume (by 500-1000 mL more)
- ↑ Tidal volume, minute ventilation
- ↑ GFR
- Supine hypotension syndrome more common
- Maternal Complications:
- Anemia (iron & folate deficiency)
- Hyperemesis gravidarum
- Gestational diabetes mellitus (GDM)
- Hypertensive disorders (preeclampsia, eclampsia)
- Thromboembolism
- Antepartum hemorrhage (placenta previa, abruption)
- Preterm labor & delivery (PPROM)
- Cesarean delivery
- Postpartum hemorrhage (uterine atony)
- Peripartum cardiomyopathy
⭐ The risk of preeclampsia is approximately 3-4 times higher in twin pregnancies, and it often presents earlier and more severely.
- Management: Increased surveillance, nutritional support, early recognition & management of complications. 📌 MOM'S PAL (Maternal Obstetric Monitoring; Preeclampsia, Anemia, Labor (preterm))
Multiple Gestation - Baby Bundle Bumps
- Types: Dizygotic (2 ova), Monozygotic (1 ovum). Chorionicity (placentation) is key risk determinant.
- DCDA: Separate placentas, lowest risk.
- MCDA: Shared placenta, intermediate risk.
- MCMA: Shared placenta & sac, highest risk.
- Maternal Risks: ↑ Preeclampsia, GDM, Anemia, PPH, operative delivery.
- Fetal Risks: ↑ Preterm birth (<37 wks), IUGR, congenital anomalies, IUFD, cerebral palsy.
- Monochorionic (MC) Twin Complications:
- TTTS: Unbalanced blood flow via placental anastomoses.
- TAPS: Significant inter-twin hemoglobin difference.
- TRAP sequence: Acardiac twin perfused by pump twin.
- sIUGR: Due to unequal placental sharing.

⭐ Twin-to-Twin Transfusion Syndrome (TTTS) affects ~10-15% of monochorionic-diamniotic (MCDA) twin pregnancies and requires specialized intervention, often laser ablation of placental anastomoses.
Multiple Gestation - Delivery Duet
- Antenatal Surveillance:
- Growth scans: DCDA q4wks (from 20wks); MCDA/MCMA q2wks (from 16wks).
- MCMA: Inpatient monitoring often 28-32 wks.
- Timing & Mode:
> ⭐ Optimal timing for delivery: uncomplicated DCDA twins **37+0 to 37+6** weeks, MCDA twins **34+0 to 36+6** weeks, and MCMA twins **32+0 to 34+0** weeks (often by elective C-section to prevent cord accidents).
- Delivery Mode:
- Vaginal: Twin 1 cephalic, no contraindications.
- CS: Twin 1 non-cephalic, fetal distress, MCMA (often), other complications (e.g., IUGR).
High‑Yield Points - ⚡ Biggest Takeaways
- Chorionicity is the single most critical factor determining outcomes in multiple gestations.
- Monochorionic (MC) twins face high risks: TTTS, TAPS, sIUGR.
- Dichorionic (DC) twins generally have more favorable outcomes.
- Ultrasound: Lambda (λ) sign indicates dichorionicity; T-sign indicates monochorionicity.
- All multiple pregnancies carry ↑ risk of preterm labor, preeclampsia, GDM, and PPH.
- Vanishing twin syndrome is a frequent finding in early pregnancy.
- Optimal delivery mode depends on GA, presentation of Twin 1, and chorionicity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

