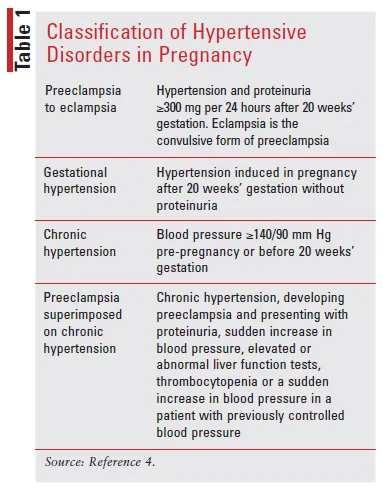
Classification & Definitions - BP Disorder Decode
- HTN: BP ≥140/90 mmHg.
- Gestational HTN (GH): HTN >20 wks. No proteinuria. Postpartum resolution.
- Preeclampsia (PE): HTN >20 wks + Proteinuria (≥0.3g/24h or PCR ≥0.3) OR end-organ damage (EOD).
- Severe features: BP ≥160/110, platelets <100k, ↑LFTs, ↑Cr, pulm edema, neuro sx.
- Eclampsia: PE + Seizures.
- Chronic HTN (CHTN): HTN <20 wks / pre-pregnancy / persists postpartum.
- Superimposed PE: CHTN + new proteinuria/EOD >20 wks.
⭐ PE: HTN + EOD suffices, proteinuria not mandatory.
Preeclampsia Pathophysiology - Placental Puzzle Pieces
- Impaired Trophoblast Invasion & Spiral Artery Remodeling:
- Leads to ↓ uteroplacental perfusion & placental hypoxia.
- Placental Stress Response:
- Release of anti-angiogenic factors (e.g., sFlt-1, soluble endoglin) & pro-inflammatory mediators.
- Systemic Endothelial Cell Dysfunction:
- Causes hypertension, proteinuria, and end-organ damage.
⭐ sFlt-1 (soluble fms-like tyrosine kinase-1) binds VEGF & PlGF, impairing angiogenesis and contributing to endothelial dysfunction and hypertension in preeclampsia.
Preeclampsia: Diagnosis & Features - Red Flag Rundown
- New HTN >20 wks: BP ≥140/90 mmHg (x2, 4h apart) OR ≥160/110 mmHg (x1).
- Plus one of:
- Proteinuria: ≥300mg/24h; Protein/Creatinine Ratio (PCR) ≥0.3; Dipstick ≥2+.
- OR End-organ dysfunction (even without proteinuria):
- Platelets <100,000/µL.
- Serum Creatinine >1.1mg/dL or doubled baseline.
- Liver transaminases (AST/ALT) ↑ (2x ULN), severe RUQ/epigastric pain.
- Pulmonary edema.
- New-onset headache unresponsive to meds / visual disturbances.
- Red Flags (Severe Features): Any listed end-organ dysfunction OR BP ≥160/110 mmHg.
⭐ Severe epigastric or Right Upper Quadrant (RUQ) pain in preeclampsia can be an ominous sign, potentially indicating HELLP syndrome or significant hepatic involvement like infarction or rupture.
Management - Treatment Triumphs Today
- Antihypertensives: (Target BP < 150/100 mmHg, urgent control if BP ≥ 160/110 mmHg)
- Oral: Labetalol, Nifedipine XL, Methyldopa (📌 LMN).
- IV (acute severe HTN): Labetalol, Hydralazine.
- Avoid: ACEi, ARBs, Diuretics (except pulmonary edema).
- MgSO4 (Magnesium Sulfate):
- Seizure prophylaxis (Severe PE) & treatment (Eclampsia).
- Dose: 4-6g IV loading, then 1-2g/hr IV.
- Monitor: DTRs, RR (>12/min), UO (>30ml/hr). Antidote: Calcium Gluconate (1g IV).
- Delivery: Definitive treatment.
- Severe PE: Deliver if ≥34 wks or unstable. If <34 wks & stable: corticosteroids, expectant management.
- Eclampsia/HELLP: Stabilize mother, then prompt delivery.
⭐ MgSO4 is continued for 24 hours postpartum for seizure prophylaxis in severe preeclampsia/eclampsia.
HELLP & Complications - Danger Zone Details
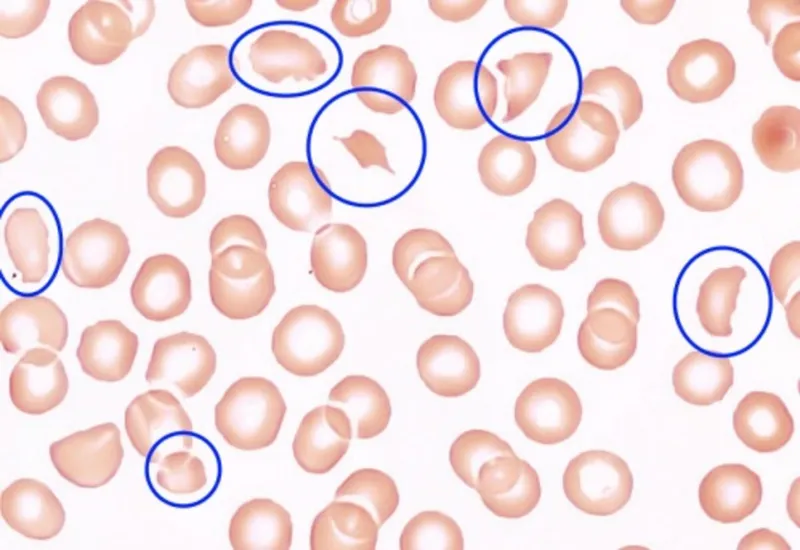
- HELLP Syndrome 📌: Hemolysis (LDH >600 U/L, schistocytes), Elevated Liver enzymes (AST/ALT >2x ULN), Low Platelets (<100,000/µL).
- Symptoms: RUQ/epigastric pain, N/V, malaise.
- Management: Prompt delivery (esp. ≥34 wks), MgSO₄, BP control.
- Maternal Complications:
- DIC, placental abruption, ARDS, ARF, hepatic rupture/infarction, eclampsia, stroke.
- Fetal Complications:
- IUGR, preterm delivery, IUFD, perinatal asphyxia.
- IUGR, preterm delivery, IUFD, perinatal asphyxia.
⭐ HELLP syndrome can occur postpartum, most commonly within 48 hours.
High‑Yield Points - ⚡ Biggest Takeaways
- Preeclampsia: New hypertension (≥140/90 mmHg) after 20 weeks gestation with proteinuria or end-organ dysfunction.
- Eclampsia: Preeclampsia plus new-onset grand mal seizures.
- HELLP syndrome: Hemolysis, Elevated Liver enzymes, Low Platelets; a severe preeclampsia variant.
- Magnesium sulfate (MgSO4): Drug of choice for seizure prophylaxis and treatment in severe preeclampsia/eclampsia.
- Definitive treatment for preeclampsia/eclampsia is delivery.
- Key antihypertensives: Labetalol, Nifedipine, Methyldopa.
- Chronic hypertension: Pre-dates pregnancy or diagnosed before 20 weeks gestation; distinguish from gestational hypertension (no proteinuria).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

