PPH Definition & Scope - Defining the Bleed
- PPH: Excessive bleeding after childbirth.
- Blood loss criteria:
- Vaginal delivery: >500ml
- Cesarean section: >1000ml
- Any amount causing hemodynamic instability or a ≥10% drop in hematocrit.
- Types by onset:
- Primary (Early): Within 24 hours postpartum (most common).
- Secondary (Late): From >24 hours up to 12 weeks postpartum.
⭐ PPH is a leading cause of maternal mortality, particularly in low-resource settings.
- Clinical signs (e.g., tachycardia, hypotension) may appear before measured loss hits thresholds, especially with concealed hemorrhage.
PPH Etiology - The Four Culprits
📌 4Ts: Tone, Trauma, Tissue, Thrombin
| Culprit | Description | Common Examples |
|---|---|---|
| Tone | Uterine Atony (most common, 70-80%) | Overdistended uterus, prolonged labor, infection |
| Trauma | Genital Tract Lacerations | Cervical/vaginal tears, uterine rupture, episiotomy |
| Tissue | Retained Products of Conception (RPOC) | Placental fragments, membranes, blood clots |
| Thrombin | Coagulopathy (rare, pre-existing/acquired) | DIC, ITP, von Willebrand disease, anticoagulants |
⭐ Uterine atony is the single most common cause of PPH, responsible for approximately 70-80% of cases.
PPH Management - Flood Control Protocol
⭐ Active Management of Third Stage of Labor (AMTSL) significantly reduces PPH incidence by over 60%.
📌 Initial Response: "HELP"
- Help: Call multidisciplinary team (Obstetrician, Anesthetist, Blood Bank).
- Ensure IV access (2 large-bore), send bloods (X-match, FBC, Coags).
- Lay flat, O2, catheterize bladder.
- Palpate uterus: Fundal massage. Identify cause (4 T's: Tone, Trauma, Tissue, Thrombin).
Stepwise Management Algorithm:
Key Interventions:
- Uterotonics (Sequence may vary):
- Oxytocin: 10-40 IU in $500\text{ml}$ NS IV infusion; or 10 IU IM.
- Methylergometrine: $0.2\text{mg}$ IM/IV (slowly, ⚠️ CI: HTN, Cardiac disease).
- Carboprost (PG F2α): $0.25\text{mg}$ IM (q15-90min, max 8 doses; ⚠️ CI: Asthma).
- Misoprostol: $800-1000\text{mcg}$ PR/PO/SL.
- Mechanical Tamponade:
- Intrauterine balloon (e.g., Bakri).
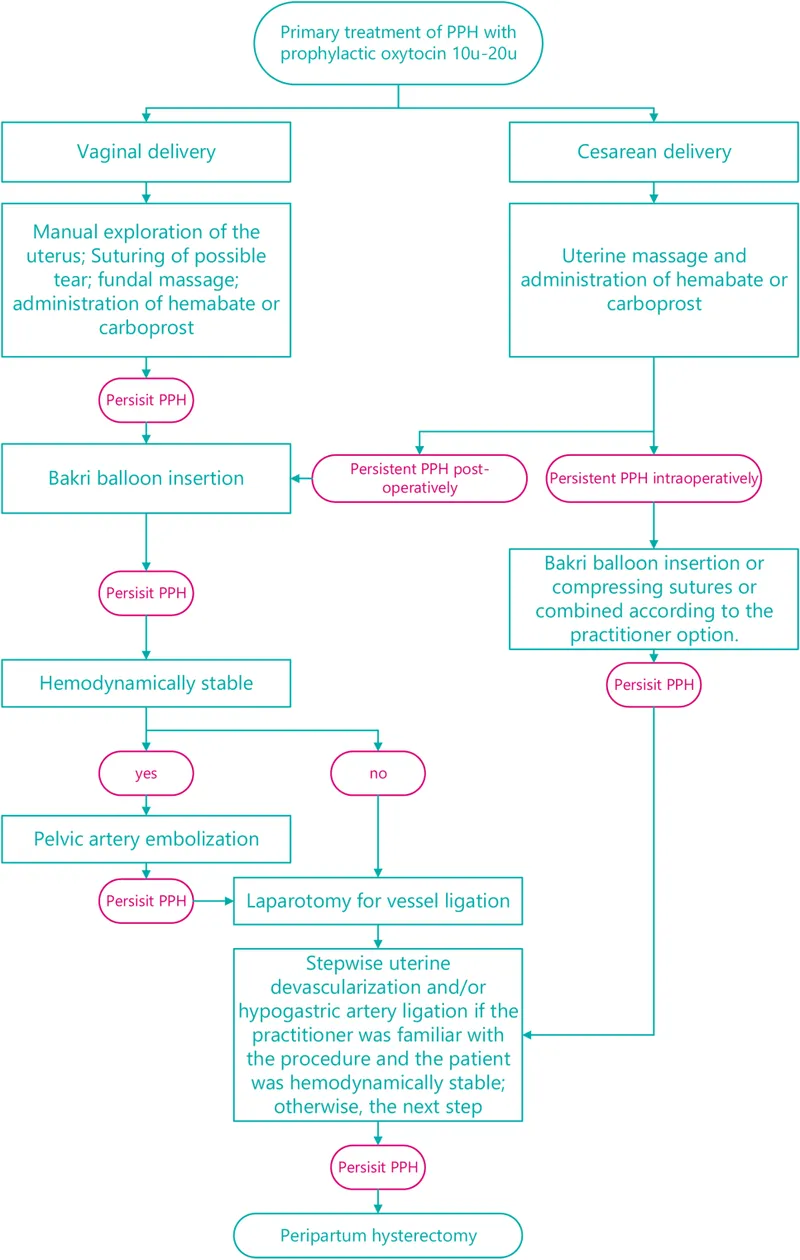
- Intrauterine balloon (e.g., Bakri).
- Surgical:
-
Repair trauma.
-
Compression sutures (e.g., B-Lynch).
-
Arterial ligation (uterine, ovarian, internal iliac).
-
Hysterectomy (last resort).
-
PPH Complications - Aftermath & Alerts
- Early Complications:
- Shock sequelae (organ damage: ARDS, AKI)
- Anemia (transfuse if Hb < 7 g/dL or symptomatic)
- Infection (endometritis, sepsis): fever, uterine tenderness
- DIC: monitor coagulation, manage cause
- Delayed Complications:
- Secondary PPH (>24h - 12wks): causes: retained products, infection
- Asherman's syndrome (post-curettage)
- Psychological sequelae (PTSD, depression)
- Long-term:
⭐ Sheehan's syndrome (postpartum pituitary necrosis) is a classic, albeit rare, long-term sequela of severe PPH leading to hypovolemic shock.
- ⚠️ Alerts:
- Persistent/worsening bleeding despite uterotonics
- Shock signs disproportionate to visible loss
- Oliguria (urine output < 0.5 ml/kg/hr)
- Altered mental status
High‑Yield Points - ⚡ Biggest Takeaways
- Uterine atony is the leading cause of PPH, accounting for 70-80% of cases.
- Active Management of Third Stage of Labor (AMTSL) significantly reduces PPH incidence.
- Initial management involves bimanual uterine massage and IV oxytocin infusion.
- Second-line uterotonics: Methylergonovine (contraindicated in hypertension), Carboprost (PGF2α, contraindicated in asthma), Misoprostol.
- Administer Tranexamic acid (TXA) within 3 hours of birth to reduce bleeding death.
- Consider the Four T's (Tone, Trauma, Tissue, Thrombin) for systematic etiology identification.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

