Labor and Delivery

On this page
🚀 Labor Launch: The Orchestrated Journey
Labor transforms a pregnancy into a newborn through an intricate interplay of uterine forces, pelvic architecture, and fetal positioning-a process you'll learn to anticipate, monitor, and guide. You'll master how contractions generate expulsive power, how pelvic dimensions shape the passage, and how fetal cardinal movements navigate descent. By integrating these dynamics with systematic progress assessment and delivery techniques, you'll build the clinical judgment to recognize normal labor, identify deviations early, and intervene decisively when maternal or fetal safety demands it.
📌 Remember: SHOW - Spontaneous rupture of membranes, Hormonal changes, Onset of contractions, Widening cervix - The four cardinal signs of labor onset
The labor process involves three primary components working in harmony:
- Uterine contractions - Generate 25-75 mmHg baseline pressure with peaks reaching 100+ mmHg
- Frequency: 2-5 contractions per 10 minutes
- Duration: 45-90 seconds each
- Intensity: Measured via intrauterine pressure catheter or external tocodynamometry
- Cervical changes - Progressive effacement (0-100%) and dilation (0-10 cm)
- Nulliparous: Effacement precedes dilation
- Multiparous: Simultaneous effacement and dilation
- Fetal descent - Measured in stations from -5 to +5 cm relative to ischial spines
⭐ Clinical Pearl: Normal labor progression requires 1.2 cm/hour cervical dilation in nulliparous women and 1.5 cm/hour in multiparous women during active phase
| Parameter | Nulliparous | Multiparous | Clinical Significance |
|---|---|---|---|
| Latent Phase Duration | ≤20 hours | ≤14 hours | Prolonged latent phase indication |
| Active Phase Rate | ≥1.2 cm/hour | ≥1.5 cm/hour | Arrest of dilation threshold |
| Second Stage Duration | ≤3 hours (epidural) | ≤2 hours (epidural) | Operative delivery consideration |
| Descent Rate | ≥1 cm/hour | ≥2 cm/hour | Arrest of descent evaluation |
| Total Labor Duration | 12-20 hours | 6-12 hours | Expected timeframe ranges |
Understanding these foundational principles sets the stage for recognizing when labor deviates from normal patterns, requiring clinical intervention to ensure maternal and fetal safety.
🚀 Labor Launch: The Orchestrated Journey
⚡ Power Systems: The Uterine Engine
📌 Remember: FUND - Fundal dominance, Uniform propagation, Normal intensity, Duration adequate - Essential contraction characteristics
Contraction assessment utilizes multiple measurement parameters:
- Frequency - Measured from onset of one contraction to onset of next
- Normal: 2-5 contractions per 10 minutes
- Tachysystole: >5 contractions per 10 minutes
- Intensity - Peak pressure minus baseline pressure
- Mild: 25-40 mmHg
- Moderate: 40-60 mmHg
- Strong: 60-80 mmHg
- Duration - Time from contraction onset to return to baseline
- Normal: 45-90 seconds
- Prolonged: >90 seconds
⭐ Clinical Pearl: Montevideo units (MVUs) = (Peak pressure - Baseline pressure) × Number of contractions in 10 minutes. >200 MVUs indicates adequate uterine activity for labor progression
| Contraction Type | Intensity (mmHg) | Duration (sec) | Frequency (/10 min) | Clinical Context |
|---|---|---|---|---|
| Braxton Hicks | 10-20 | 30-45 | Irregular | False labor |
| Early Labor | 25-40 | 45-60 | 2-3 | Latent phase |
| Active Labor | 50-75 | 60-80 | 3-4 | Progressive dilation |
| Transition | 75-100 | 80-90 | 4-5 | Complete dilation |
| Pushing | 80-120 | 60-90 | 3-5 | Second stage |
Recognizing optimal uterine function enables clinicians to distinguish between normal labor progression and power-related dystocia requiring intervention.
⚡ Power Systems: The Uterine Engine
🚪 Passage Dynamics: The Pelvic Gateway
- Pelvic Inlet (Plane of Greatest Dimension)
- Anteroposterior diameter: ≥11 cm (obstetric conjugate)
- Transverse diameter: ≥13 cm
- Posterior sagittal: ≥4.5 cm
- Midpelvis (Plane of Least Dimension)
- Anteroposterior: ≥11.5 cm
- Transverse (interspinous): ≥10.5 cm - Most restrictive measurement
- Posterior sagittal: ≥4.5 cm
- Pelvic Outlet
- Anteroposterior: ≥11.5 cm
- Transverse (intertuberous): ≥8 cm
- Posterior sagittal: ≥7.5 cm
📌 Remember: STOP - Sacral promontory to symphysis (11 cm), Transverse inlet (13 cm), Outlet intertuberous (8 cm), Posterior sagittal (4.5 cm) - Critical pelvic measurements
| Pelvic Type | Frequency | Inlet Shape | Midpelvis | Delivery Prognosis |
|---|---|---|---|---|
| Gynecoid | 50% | Round | Adequate | Excellent - Normal delivery |
| Android | 20% | Heart-shaped | Narrow | Poor - C-section risk ↑ |
| Anthropoid | 25% | Oval AP | Variable | Good - OP position risk |
| Platypelloid | 5% | Flat transverse | Shallow | Poor - Transverse arrest |
| Mixed Types | Variable | Combined features | Variable | Depends on limiting plane |
Clinical assessment of pelvic adequacy involves systematic evaluation during labor:
- Digital examination - Assess diagonal conjugate (≥11.5 cm)
- Ischial spine prominence - Grade 0-4 scale
- Sacral curvature - Straight vs. curved configuration
- Subpubic arch - ≥90 degrees for adequate outlet
- Coccyx mobility - Fixed vs. mobile assessment
💡 Master This: Cephalopelvic disproportion occurs when fetal head diameter (9.5-10 cm) exceeds available pelvic space, diagnosed by lack of descent despite adequate contractions (>200 MVUs) for ≥2 hours in nulliparous or ≥1 hour in multiparous women
Understanding pelvic architecture enables prediction of delivery challenges and guides decisions regarding route of delivery.
🚪 Passage Dynamics: The Pelvic Gateway
👶 Passenger Navigation: Fetal Positioning Mastery
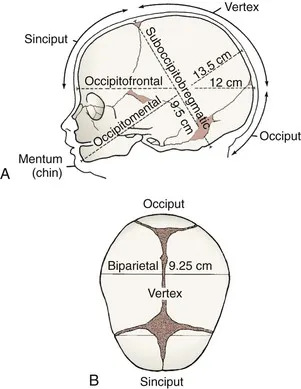
Fetal positioning determines delivery success through precise anatomical relationships between fetal dimensions and maternal pelvic capacity. The fetal head presents multiple diameter options, with optimal positioning minimizing the presenting diameter.
- Fetal Head Diameters
- Suboccipitobregmatic: 9.5 cm (vertex presentation - optimal)
- Occipitofrontal: 11.5 cm (deflexed head)
- Mentovertical: 13.5 cm (face presentation)
- Biparietal: 9.5 cm (transverse diameter)
- Fetal Positions - Relationship of occiput to maternal pelvis
- LOA (Left Occiput Anterior): 40% of deliveries
- ROA (Right Occiput Anterior): 25% of deliveries
- OP (Occiput Posterior): 15% - Prolonged labor risk
- Transverse: 5% - Operative delivery likely
📌 Remember: FLEX - Flexion reduces diameter, Left occiput anterior most common, Extension at outlet, Xternal rotation follows - Optimal fetal mechanics
| Fetal Position | Frequency | Labor Duration | Delivery Mode | Complications |
|---|---|---|---|---|
| LOA/ROA | 65% | Normal | Spontaneous 90% | Minimal |
| LOP/ROP | 15% | +2-4 hours | Operative 60% | Back pain, arrest |
| Transverse | 5% | Prolonged | C-section 80% | Shoulder dystocia |
| Face/Brow | <1% | Variable | C-section 70% | Facial edema |
| Breech | 3-4% | Normal | C-section 85% | Cord prolapse |
Assessment of fetal position utilizes multiple clinical techniques:
- Leopold's maneuvers - External palpation identifying fetal parts
- First maneuver: Fundal contents (breech vs. head)
- Second maneuver: Fetal back location
- Third maneuver: Presenting part mobility
- Fourth maneuver: Cephalic prominence and engagement
- Vaginal examination - Palpation of sutures and fontanelles
- Sagittal suture orientation indicates position
- Posterior fontanelle triangular, anterior diamond-shaped
- Ultrasound confirmation - 95% accuracy for position determination
💡 Master This: Station assessment measures fetal head descent relative to ischial spines (station 0), with -5 to +5 cm scale. Engagement occurs at 0 station, and crowning at +4 to +5 station
Understanding fetal positioning enables prediction of labor progression and guides management decisions for optimal delivery outcomes.
👶 Passenger Navigation: Fetal Positioning Mastery
📊 Progress Monitoring: The Labor Dashboard
- Cervical Dilation Monitoring
- Alert line: Expected progress rate (1 cm/hour minimum)
- Action line: 4 hours to right of alert line
- Crossing action line: Indicates need for intervention
- Fetal Descent Assessment
- Station measurements: -5 to +5 cm relative to ischial spines
- Expected descent: 1 cm/hour in nulliparous, 2 cm/hour multiparous
- Arrest criteria: No descent for ≥2 hours (nulliparous) or ≥1 hour (multiparous)
📌 Remember: PACE - Partograph plotting, Assess every hour, Cervix and station, Evaluate for action line crossing - Systematic monitoring approach
| Monitoring Parameter | Normal Range | Assessment Frequency | Abnormal Findings | Action Required |
|---|---|---|---|---|
| Cervical Dilation | ≥1 cm/hour | Every 2-4 hours | <0.5 cm/hour | Evaluate dystocia |
| Fetal Descent | ≥1 cm/hour | Every 2-4 hours | No change 2+ hours | Consider operative delivery |
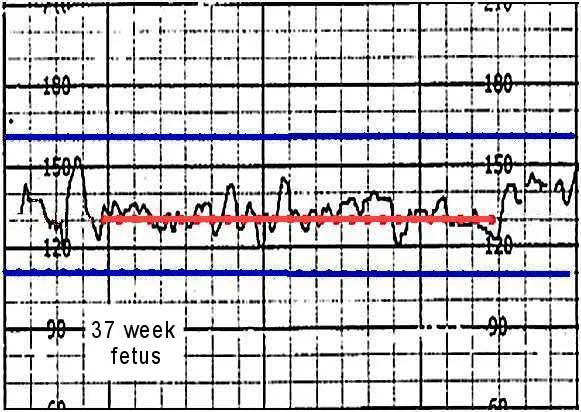
| FHR Baseline | 110-160 bpm | Continuous | <110 or >160 | Immediate evaluation |
| Contractions | 200+ MVU | Continuous | <200 MVU | Augmentation needed |
| Maternal Vitals | Stable | Every 1-2 hours | Fever >38°C | Infection workup |
Advanced monitoring techniques enhance assessment accuracy:
- Intrauterine pressure catheter - Direct measurement of contraction strength
- Montevideo units calculation: >200 MVU indicates adequacy
- Baseline pressure: 8-12 mmHg normal resting tone
- Fetal scalp electrode - Continuous FHR monitoring
- Beat-to-beat variability: 6-25 bpm indicates fetal well-being
- Accelerations: ≥15 bpm for ≥15 seconds reassuring
- Ultrasound assessment - Fetal position and estimated weight
- Position changes: May explain arrest patterns
- Macrosomia: >4000g increases dystocia risk
💡 Master This: Active management of labor protocols reduce C-section rates by 25-30% through early amniotomy, oxytocin augmentation for inadequate progress, and continuous support, maintaining delivery within 12 hours for nulliparous women
Systematic monitoring enables early recognition of labor abnormalities and guides evidence-based interventions to optimize maternal and fetal outcomes.
📊 Progress Monitoring: The Labor Dashboard
🎯 Delivery Orchestration: The Final Symphony
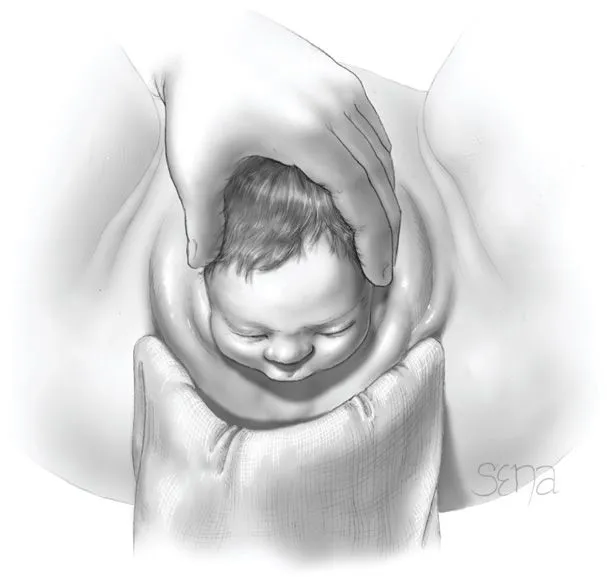
The second stage begins with complete cervical dilation (10 cm) and ends with fetal delivery, requiring coordinated maternal effort and clinical guidance to achieve safe passage through the final 5 cm of descent.
- Second Stage Duration Limits
- Nulliparous without epidural: ≤3 hours
- Nulliparous with epidural: ≤4 hours
- Multiparous without epidural: ≤2 hours
- Multiparous with epidural: ≤3 hours
- Pushing Technique Optimization
- Open-glottis pushing: Reduces fetal acidosis risk
- Delayed pushing: Allow 1-2 hours passive descent with epidural
- Position variations: Upright positions reduce duration by 15-30 minutes
📌 Remember: PUSH - Position upright, Use open glottis, Support perineum, Handle shoulders carefully - Optimal delivery technique
| Delivery Technique | Indication | Success Rate | Complications | Recovery Time |
|---|---|---|---|---|
| Spontaneous | Normal progress | 85-90% | Minimal | 1-2 weeks |
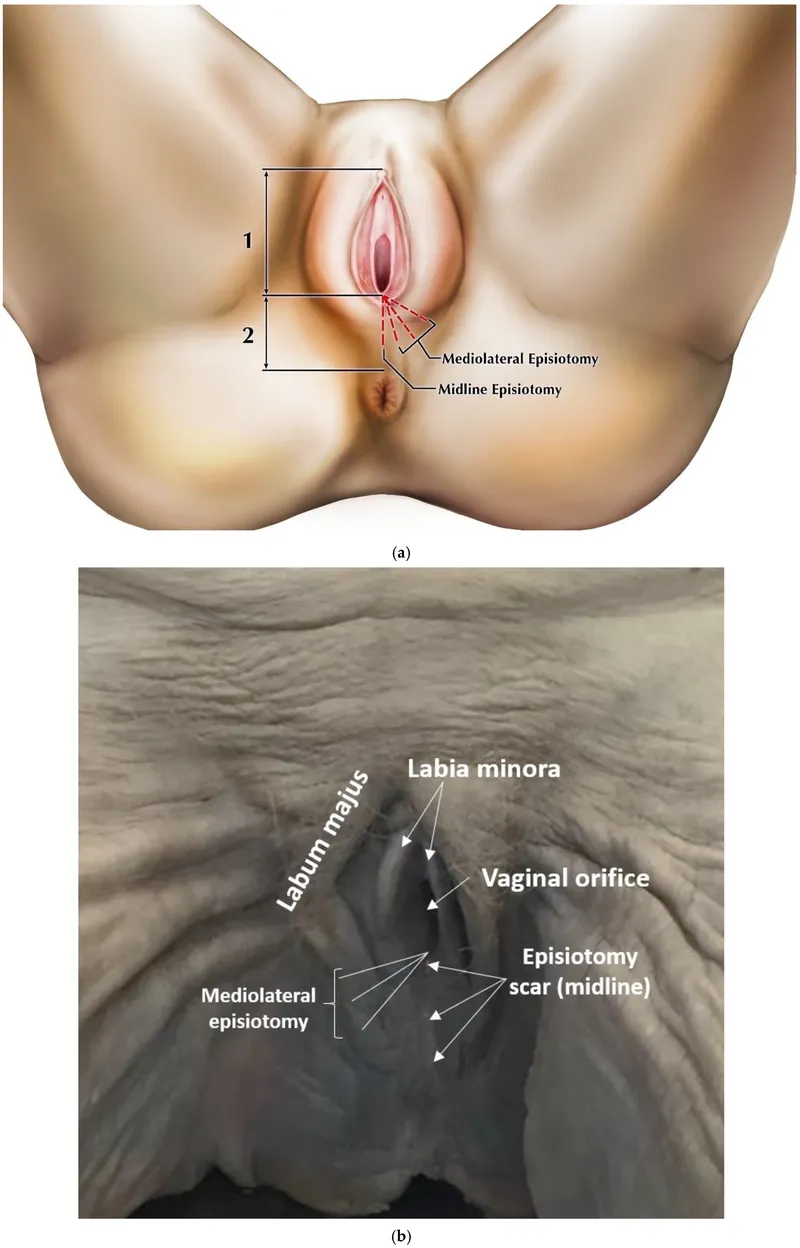
| Episiotomy | Fetal distress | 95% | Pain, infection 10% | 3-4 weeks |
| Vacuum | Prolonged 2nd stage | 80-85% | Scalp injury 5% | 2-3 weeks |
| Forceps | Arrest of descent | 90-95% | Facial marks 15% | 2-3 weeks |
| C-section | Failed operative | 99% | Surgical risks | 6-8 weeks |
Shoulder delivery requires specific maneuvers to prevent shoulder dystocia, occurring in 0.6-1.4% of deliveries:
- McRoberts maneuver - Maternal hip flexion, 90% success rate
- Suprapubic pressure - Reduces anterior shoulder diameter
- Episiotomy - Increases space for maneuvers, not primary treatment
- Internal maneuvers - Woods screw, delivery of posterior arm
💡 Master This: Shoulder dystocia management follows HELPERR mnemonic - Help (call for assistance), Evaluate for episiotomy, Legs (McRoberts), Pressure (suprapubic), Enter maneuvers (internal rotation), Remove posterior arm, Roll patient (all-fours position)
Third stage management focuses on placental delivery within 30 minutes:
- Active management reduces hemorrhage risk by 60%
- Oxytocin 10 units IM immediately after delivery
- Controlled cord traction with uterine counter-pressure
- Uterine massage after placental delivery
- Signs of separation: Uterine globular shape, cord lengthening, gush of blood
- Manual removal indicated if >30 minutes or excessive bleeding
Understanding delivery orchestration enables clinicians to guide the final phase of labor safely while minimizing maternal and fetal complications.
🎯 Delivery Orchestration: The Final Symphony
🏆 Labor Mastery: The Clinical Command Center
The clinical mastery framework synthesizes all labor components into actionable decision trees and rapid assessment tools for immediate clinical application.
📌 Remember: MASTER - Monitor continuously, Assess the 3 Ps, Support physiologic process, Time interventions appropriately, Evaluate progress hourly, Recognize complications early
Essential Clinical Arsenal:
- Normal Labor Parameters
- Cervical dilation: ≥1.2 cm/hour (nulliparous), ≥1.5 cm/hour (multiparous)
- Descent rate: ≥1 cm/hour (nulliparous), ≥2 cm/hour (multiparous)
- Contraction adequacy: ≥200 Montevideo units
- FHR baseline: 110-160 bpm with moderate variability
- Intervention Thresholds
- Augmentation: <200 MVU for ≥4 hours active labor
- Operative delivery: No descent for ≥2 hours (nulliparous) or ≥1 hour (multiparous)
- C-section: Failed operative delivery or non-reassuring FHR with failed conservative measures
| Clinical Scenario | Assessment Priority | Immediate Action | Success Metric |
|---|---|---|---|
| Arrest of Dilation | Contraction adequacy | Oxytocin augmentation | Progress in 2-4 hours |
| Arrest of Descent | Fetal position/size | Operative delivery trial | Delivery within 1 hour |
| Non-reassuring FHR | Fetal oxygenation | Intrauterine resuscitation | FHR improvement |
| Shoulder Dystocia | Delivery urgency | McRoberts + pressure | Delivery <5 minutes |
| Postpartum Hemorrhage | Bleeding source | Uterotonic agents | Bleeding control |
💡 Master This: Safe labor management balances physiologic patience with timely intervention, recognizing that 85% of labors progress normally without intervention, while 15% require active management to prevent maternal-fetal compromise
This comprehensive framework transforms theoretical knowledge into practical clinical expertise, enabling confident management of labor and delivery across the full spectrum of normal and complicated presentations.
🏆 Labor Mastery: The Clinical Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















