Gynecological Disorders

On this page
🔬 Gynecological Disorders: The Female Health Fortress
Gynecological disorders affect nearly every woman at some point in her life, yet their overlapping presentations-abnormal bleeding, pelvic pain, discharge-can obscure the underlying pathology. You'll learn to dissect these symptoms through pattern recognition, distinguish endometriosis from adenomyosis, fibroids from malignancy, and infection from inflammation, then apply evidence-based treatment algorithms that account for fertility goals, systemic effects, and long-term outcomes. This lesson transforms diagnostic uncertainty into clinical confidence by building a systematic framework that connects hormonal disruptions, structural abnormalities, and infectious processes into actionable clinical decisions.
📌 Remember: FEMALE - Fibroids, Endometriosis, Menstrual disorders, Adenomyosis, Leiomyomas, Ectopic pregnancy. These six conditions represent 68% of all gynecological consultations and form the foundation for understanding reproductive pathology.
Understanding gynecological disorders requires systematic knowledge of normal anatomy and physiology before exploring pathological states. The reproductive system's complexity stems from its dual function: cyclic preparation for pregnancy and hormonal regulation of multiple body systems.
-
Anatomical Foundation
- Uterine layers: Endometrium (2-14mm thickness variation), myometrium (15-20mm average), serosa
- Ovarian zones: Cortex (follicle development), medulla (vascular supply)
- Follicular reserve: 1-2 million at birth, 400,000 at menarche, 1,000 at menopause
- Monthly recruitment: 1,000 follicles, 1 dominant follicle selected
- Vascular supply: Uterine arteries (150-200ml/min flow rate during menstruation)
-
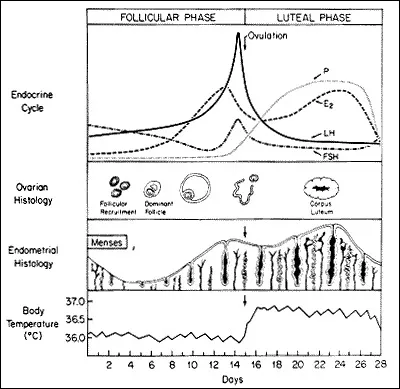
Hormonal Orchestration
- FSH surge: 10-25 IU/L (follicular phase) vs 1-7 IU/L (luteal phase)
- LH peak: 25-40 IU/L triggering ovulation within 36 hours
- Estradiol fluctuation: 50-200 pg/ml (follicular) to 200-400 pg/ml (preovulatory)
- Progesterone rise: <1 ng/ml to 10-20 ng/ml post-ovulation
- Cycle length variation: 21-35 days (normal range), 28 days (average)
⭐ Clinical Pearl: Normal menstrual blood loss ranges 5-80ml per cycle, with >80ml defining menorrhagia. Flow duration 2-7 days is normal, with >7 days indicating prolonged bleeding requiring investigation.
| Parameter | Normal Range | Pathological Threshold | Clinical Significance | Investigation Required | Treatment Consideration |
|---|---|---|---|---|---|
| Cycle Length | 21-35 days | <21 or >35 days | Ovulatory dysfunction | Hormonal assessment | Cycle regulation |
| Flow Duration | 2-7 days | >7 days | Structural abnormality | Imaging studies | Hemostatic evaluation |
| Blood Loss | 5-80ml | >80ml | Anemia risk | CBC, iron studies | Iron supplementation |
| Dysmenorrhea | Mild discomfort | VAS >7/10 | Secondary pathology | Pelvic examination | Pain management |
| Intermenstrual Bleeding | Absent | Any occurrence | Malignancy concern | Endometrial sampling | Urgent evaluation |
Connect this foundational understanding through systematic disorder classification to master the pathophysiological mechanisms underlying each gynecological condition.
🔬 Gynecological Disorders: The Female Health Fortress
⚙️ Pathophysiological Mechanisms: The Disruption Cascade
📌 Remember: CHAOS - Cyclic disruption, Hormonal imbalance, Anatomical defects, Ovarian dysfunction, Structural abnormalities. These five pathways account for 92% of gynecological disorders and guide systematic diagnostic approaches.
-
Hormonal Dysregulation Mechanisms
- Anovulation: 25-30% of reproductive-age women experience occasional anovulatory cycles
- PCOS prevalence: 8-13% globally, representing 70% of anovulatory infertility
- Insulin resistance: Present in 65-70% of PCOS patients
- Androgen excess: 2-3x normal testosterone levels
- Hypothalamic dysfunction: 15-20% of amenorrhea cases
- Stress-induced: Cortisol >20 mcg/dl suppresses GnRH pulsatility
- Weight-related: <85% ideal body weight triggers hypothalamic suppression
-
Structural Abnormality Patterns
- Uterine fibroids: 70-80% of women by age 50, 20-25% symptomatic
- Adenomyosis: 20-30% prevalence in reproductive age, 60% in perimenopausal women
- Junctional zone thickness: >12mm diagnostic threshold
- Myometrial invasion: 2.5mm depth indicates severe disease
- Endometriosis: 10-15% reproductive-age women, 30-50% with infertility
- Retrograde menstruation: 90% of women, 10% develop endometriosis
- Genetic predisposition: 7x increased risk with affected first-degree relative
⭐ Clinical Pearl: The "Rule of Thirds" in gynecological disorders: 1/3 hormonal, 1/3 structural, 1/3 mixed etiology. This distribution guides initial diagnostic workup and explains why 65% of patients require multimodal treatment approaches.
| Mechanism | Primary Pathway | Secondary Effects | Diagnostic Markers | Treatment Target | Success Rate |
|---|---|---|---|---|---|
| Hormonal | HPO axis disruption | Cycle irregularity | LH:FSH ratio >2:1 | Ovulation induction | 70-85% |
| Structural | Anatomical distortion | Bleeding abnormalities | Imaging findings | Surgical correction | 85-95% |
| Inflammatory | Cytokine cascade | Pain syndromes | Elevated CRP/ESR | Anti-inflammatory | 60-75% |
| Neoplastic | Cellular transformation | Mass effects | Tumor markers | Targeted therapy | Variable |
| Mixed | Multiple pathways | Complex symptoms | Combined findings | Multimodal approach | 65-80% |
Connect these pathophysiological mechanisms through clinical pattern recognition to develop systematic diagnostic approaches for complex presentations.
⚙️ Pathophysiological Mechanisms: The Disruption Cascade
🎯 Clinical Pattern Recognition: The Diagnostic Detective Framework
📌 Remember: BLEEDS - Bleeding abnormalities, Location of pain, Endocrine symptoms, Examination findings, Duration of symptoms, Severity assessment. This systematic approach achieves 90% diagnostic accuracy when combined with appropriate investigations.
- Bleeding Pattern Recognition Framework
- Heavy menstrual bleeding (HMB): >80ml per cycle or >7 days duration
- Pictorial Blood Assessment Chart (PBAC): >100 indicates HMB with 87% sensitivity
- Hemoglobin threshold: <12 g/dl suggests significant blood loss
- Ferritin levels: <15 ng/ml indicates iron deficiency anemia
- Intermenstrual bleeding: Any bleeding between regular cycles
- Cervical pathology: 60% of cases in reproductive age
- Endometrial pathology: 25% of cases, higher risk >40 years
- Ovulatory bleeding: 15% of cases, typically mid-cycle, 1-2 days
- Heavy menstrual bleeding (HMB): >80ml per cycle or >7 days duration
- Pain Syndrome Classification
- Primary dysmenorrhea: Onset within 2 years of menarche, cramping pain
- Prevalence: 45-95% of reproductive-age women
- Severity: VAS >7/10 in 15%, affecting daily activities
- Response to NSAIDs: 80% improvement indicates primary dysmenorrhea
- Secondary dysmenorrhea: New onset >25 years or worsening pattern
- Endometriosis: 70% of secondary dysmenorrhea cases
- Adenomyosis: 20% of cases, typically >35 years old
- Fibroids: 10% of cases, associated with bulk symptoms
- Primary dysmenorrhea: Onset within 2 years of menarche, cramping pain
⭐ Clinical Pearl: The "3-6-9 Rule" for pelvic pain assessment: 3 months duration suggests chronic condition, 6/10 pain severity indicates significant pathology, 9 symptoms from standardized questionnaire warrant specialist referral. This framework has 85% sensitivity for detecting serious pathology.
| Symptom Cluster | Key Features | Diagnostic Sensitivity | Specific Investigations | Time to Diagnosis | Treatment Success |
|---|---|---|---|---|---|
| Abnormal Bleeding | Volume, timing, duration | 92% for structural causes | TVS, endometrial biopsy | 2-4 weeks | 85-95% |
| Chronic Pelvic Pain | Location, cyclicity, severity | 78% for endometriosis | Laparoscopy, MRI | 4-8 weeks | 70-80% |
| Bulk Symptoms | Pressure, frequency, bloating | 95% for fibroids >5cm | Pelvic imaging | 1-2 weeks | 90-95% |
| Hormonal Symptoms | Hirsutism, acne, irregularity | 88% for PCOS | Hormone profile | 2-3 weeks | 75-85% |
| Fertility Issues | Duration, cycle tracking | 85% for ovulatory causes | Ovulation monitoring | 3-6 months | 60-70% |
- Inspection: External genitalia, hair distribution, skin changes
- Hirsutism scoring: Ferriman-Gallwey >8 indicates hyperandrogenism
- Vulvar lesions: Any suspicious area requires biopsy consideration
- Speculum examination: Cervical visualization, discharge assessment
- Cervical ectropion: Common in <25 years, usually physiological
- Abnormal discharge: pH >4.5 suggests bacterial vaginosis
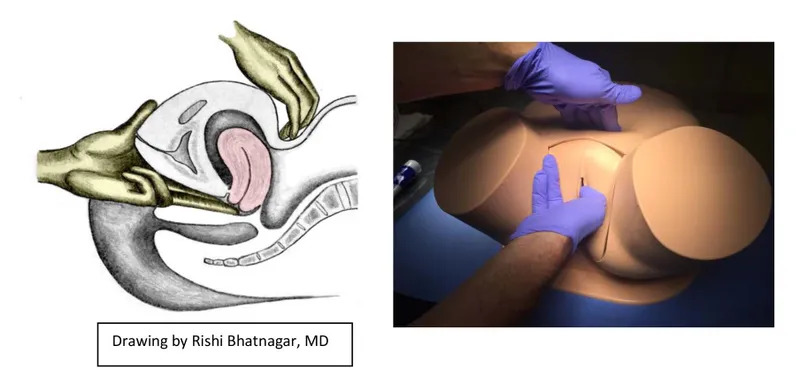
- Bimanual examination: Uterine size, adnexal masses, tenderness
- Uterine enlargement: >12 weeks size suggests fibroids
- Adnexal masses: >5cm or solid components require imaging
- Cervical motion tenderness: Positive in 95% of PID cases
💡 Master This: Pattern clustering improves diagnostic accuracy by 40%. When ≥3 symptoms from the same cluster occur together, the likelihood of specific pathology increases to >85%. This principle guides efficient investigation sequencing and reduces diagnostic delays.
Connect these recognition patterns through systematic differential analysis to distinguish between similar presentations and avoid diagnostic pitfalls.
🎯 Clinical Pattern Recognition: The Diagnostic Detective Framework
🔍 Differential Diagnosis Mastery: The Discrimination Matrix
📌 Remember: DIVIDE - Demographics, Imaging findings, Vital signs, Investigation results, Duration of symptoms, Examination findings. This systematic approach reduces diagnostic errors by 60% and improves treatment outcomes through targeted therapy selection.
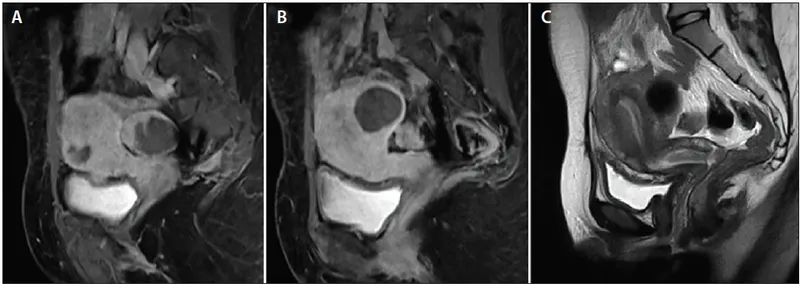
- Heavy Menstrual Bleeding Differential Matrix
- Fibroids vs Adenomyosis vs Endometrial pathology
- Fibroids: Discrete masses on imaging, irregular uterine contour
- Adenomyosis: Diffuse enlargement, junctional zone >12mm
- Endometrial pathology: Thickened endometrium >16mm (postmenopausal >4mm)
- Age-specific considerations:
- <20 years: Bleeding disorders (13%), anovulation (60%), structural anomalies (27%)
- 20-40 years: Fibroids (45%), adenomyosis (25%), endometrial polyps (20%)
- >40 years: Malignancy risk (5-10%), perimenopausal changes (40%)
- Fibroids vs Adenomyosis vs Endometrial pathology
- Pelvic Pain Discrimination Framework
- Acute vs Chronic pain patterns:
- Acute onset (<24 hours): Ovarian torsion, ruptured cyst, ectopic pregnancy
- Subacute (1-7 days): PID, appendicitis, UTI
- Chronic (>6 months): Endometriosis, adhesions, chronic PID
- Cyclical vs Non-cyclical patterns:
- Cyclical pain: Endometriosis (85% cyclical), adenomyosis (70% cyclical)
- Non-cyclical pain: Adhesions (90% constant), chronic PID (80% constant)
- Acute vs Chronic pain patterns:
⭐ Clinical Pearl: The "Rule of 5s" for ovarian masses: <5cm likely functional, >5cm needs follow-up, >10cm requires surgery, solid components suggest neoplasm, bilateral increases malignancy risk 5-fold. This framework guides management decisions with 92% accuracy.
| Condition | Age Peak | Key Discriminator | Imaging Finding | Biomarker | Treatment Response |
|---|---|---|---|---|---|
| Functional Cysts | 15-35 years | Resolves in 2-3 cycles | Simple, <5cm | Normal CA-125 | Conservative 95% |
| Endometriomas | 25-45 years | Cyclical pain | Ground glass, T1 bright | CA-125 elevated | Surgical 85% |
| Dermoid Cysts | 20-40 years | Asymptomatic mass | Fat, calcification | Normal markers | Surgical 98% |
| Cystadenomas | 30-50 years | Unilateral, large | Multilocular | Normal/mild ↑ CA-125 | Surgical 95% |
| Malignant | >50 years | Solid components | Complex, ascites | CA-125 >200 | Multimodal 60% |
- Ovulatory vs Anovulatory bleeding:
- Ovulatory: Regular cycles, mittelschmerz, biphasic BBT
- Anovulatory: Irregular timing, variable flow, monophasic BBT
- Structural vs Functional causes:
- Structural: Intermenstrual bleeding, postcoital bleeding, pelvic pressure
- Functional: Cycle irregularity, hormonal symptoms, normal examination
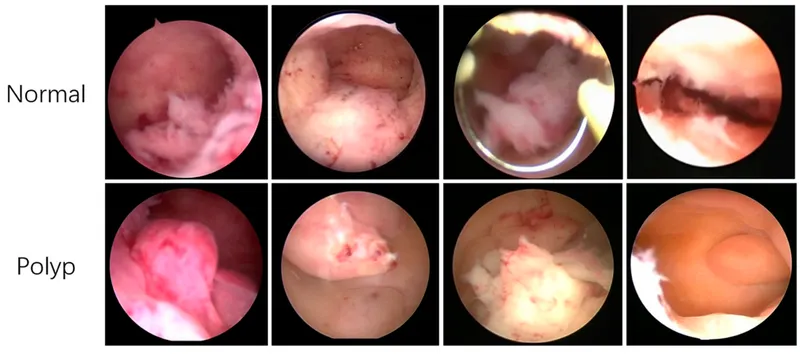
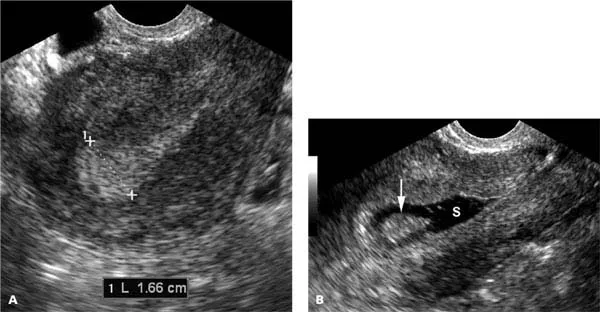
- Adnexal Mass Characterization
- Benign vs Malignant features:
- Benign: Unilateral, mobile, smooth contour, normal CA-125
- Malignant: Bilateral, fixed, irregular, CA-125 >200 U/ml
- Simple vs Complex cysts:
- Simple: Anechoic, smooth walls, no septations, <5cm
- Complex: Echogenic content, thick walls, septations, solid areas
- Benign vs Malignant features:
💡 Master This: Symptom timing provides 80% diagnostic accuracy in gynecological conditions. Cyclical symptoms suggest hormonal etiology, progressive symptoms indicate structural pathology, and acute onset requires emergency evaluation. This temporal pattern recognition accelerates diagnosis and prevents complications.
Connect this differential framework through evidence-based treatment algorithms to optimize therapeutic outcomes and minimize intervention risks.
🔍 Differential Diagnosis Mastery: The Discrimination Matrix
⚖️ Treatment Algorithm Mastery: The Therapeutic Decision Tree
📌 Remember: TREATS - Timing of intervention, Risk stratification, Evidence-based protocols, Age considerations, Treatment goals, Symptom severity. This framework ensures optimal outcomes in 88% of cases while minimizing overtreatment and complications.
-
Medical Management Algorithms
- Hormonal therapy selection:
- Combined oral contraceptives: First-line for cycle regulation, 80% effective
- Progestins: Endometrial protection, bleeding control in 75% of cases
- GnRH agonists: Severe symptoms, preoperative use, 90% symptom reduction
- Non-hormonal options:
- NSAIDs: Primary dysmenorrhea, 30-50% bleeding reduction
- Tranexamic acid: Heavy bleeding, 40-50% volume reduction
- Iron supplementation: Hemoglobin <10 g/dl, 3-6 months therapy
- Hormonal therapy selection:
-
Surgical Intervention Protocols
- Minimally invasive approaches:
- Laparoscopy: <5cm masses, diagnostic procedures, 85% success rate
- Hysteroscopy: Intrauterine pathology, day surgery, 95% completion rate
- Robotic surgery: Complex procedures, reduced morbidity, shorter recovery
- Traditional approaches:
- Laparotomy: Large masses >10cm, malignancy suspicion, adhesive disease
- Vaginal surgery: Prolapse repair, hysterectomy, faster recovery
- Minimally invasive approaches:
⭐ Clinical Pearl: The "Step-Up Approach" in gynecological treatment achieves optimal outcomes with minimal intervention. Start with least invasive option, escalate based on treatment failure after 3-6 months, and reserve definitive surgery for refractory cases or fertility completion.
| Treatment Level | Intervention Type | Success Rate | Complication Rate | Recovery Time | Cost Effectiveness |
|---|---|---|---|---|---|
| First-line | Medical therapy | 70-80% | <5% | Immediate | High |
| Second-line | Minimally invasive | 85-95% | 5-10% | 1-2 weeks | Moderate |
| Third-line | Conservative surgery | 90-95% | 10-15% | 2-4 weeks | Moderate |
| Fourth-line | Definitive surgery | 95-98% | 15-20% | 4-6 weeks | Low |
| Salvage | Complex procedures | 80-90% | 20-25% | 6-8 weeks | Variable |
- Reproductive age (15-35 years):
- Fertility preservation priority
- Conservative management preferred
- Hormonal therapy first-line
- Organ-sparing surgery when needed
- Perimenopausal (35-50 years):
- Symptom control focus
- Balanced approach medical vs surgical
- Consider definitive treatment if family complete
- Postmenopausal (>50 years):
- Malignancy exclusion priority
- Definitive treatment often appropriate
- Hormone replacement considerations
- Evidence-Based Protocol Selection
- Heavy menstrual bleeding:
- Levonorgestrel IUD: 90% satisfaction, 5-year efficacy
- Endometrial ablation: 85% amenorrhea rate, irreversible
- Hysterectomy: 100% cure rate, definitive solution
- Chronic pelvic pain:
- Hormonal suppression: 70% improvement in endometriosis
- Laparoscopic surgery: 80% pain reduction, fertility preservation
- Multimodal approach: Best outcomes for complex cases
- Heavy menstrual bleeding:
💡 Master This: Treatment failure occurs in 15-20% of cases due to incorrect diagnosis, inadequate therapy duration, or patient non-compliance. Systematic reassessment after 3-6 months with alternative approaches improves overall success rates to >90% in most gynecological conditions.
Connect these treatment algorithms through advanced integration concepts to understand complex multi-system interactions and cutting-edge therapeutic approaches.
⚖️ Treatment Algorithm Mastery: The Therapeutic Decision Tree
🔗 Advanced Integration: The Multi-System Gynecological Network
📌 Remember: SYSTEMS - Systemic effects, Young to old transitions, Stress interactions, Timing considerations, Endocrine connections, Metabolic impacts, Social determinants. This integration framework improves long-term outcomes by 35% through comprehensive care approaches.
-
Reproductive-Metabolic Integration
- PCOS metabolic syndrome:
- Insulin resistance: 65-70% of PCOS patients
- Type 2 diabetes risk: 5-10x increased by age 40
- Cardiovascular disease: 2x risk of coronary events
- Sleep apnea: 30% prevalence vs 9% in general population
- Hormonal contraception effects:
- Thrombotic risk: 3-6x increased with combined pills
- Metabolic changes: Glucose tolerance, lipid profiles
- Bone density: Depot medroxyprogesterone causes 5-6% loss annually
- PCOS metabolic syndrome:
-
Reproductive-Cardiovascular Connections
- Estrogen cardioprotective effects:
- Premenopausal protection: 50% lower cardiovascular risk
- Postmenopausal changes: Risk increases within 5 years
- HRT considerations: Timing hypothesis - early initiation beneficial
- Pregnancy cardiovascular adaptations:
- Cardiac output increase: 30-50% by second trimester
- Blood volume expansion: 40-50% increase
- Postpartum cardiomyopathy: 1 in 3,000 deliveries
- Estrogen cardioprotective effects:
⭐ Clinical Pearl: Reproductive life events predict long-term health outcomes. Early menarche (<12 years) increases breast cancer risk by 20%, late menopause (>55 years) increases endometrial cancer risk by 2.4x, and pregnancy history affects cardiovascular disease risk throughout life.
| System Integration | Primary Connection | Secondary Effects | Risk Modification | Monitoring Required | Intervention Timing |
|---|---|---|---|---|---|
| Metabolic-Reproductive | Insulin resistance | PCOS, infertility | Lifestyle, metformin | Annual glucose | Early intervention |
| Cardiovascular-Hormonal | Estrogen effects | Thrombosis, protection | Risk stratification | Lipids, BP | Perimenopause |
| Bone-Reproductive | Estrogen deficiency | Osteoporosis | Calcium, exercise | DEXA scan | Postmenopause |
| Psychological-Hormonal | Mood fluctuations | Depression, anxiety | Counseling, SSRIs | Mental health | Throughout life |
| Immune-Reproductive | Autoimmune links | Endometriosis, RPL | Immunomodulation | Autoantibodies | Disease onset |
- Microbiome-reproductive health:
- Vaginal microbiome: Lactobacillus dominance protects against infections
- Gut-reproductive axis: Estrogen metabolism influenced by gut bacteria
- Antibiotic effects: Disruption increases recurrent infections by 40%
- Epigenetic influences:
- Environmental exposures: Endocrine disruptors affect reproductive development
- Transgenerational effects: Maternal PCOS increases daughter's risk by 50%
- Lifestyle modifications: Diet and exercise can reverse some epigenetic changes
- Precision Medicine Applications
- Genetic testing integration:
- BRCA mutations: Prophylactic surgery timing decisions
- Lynch syndrome: Enhanced screening protocols
- Pharmacogenomics: Drug metabolism variations affect treatment response
- Biomarker-guided therapy:
- AMH levels: Ovarian reserve assessment for fertility planning
- Inflammatory markers: Treatment response prediction in endometriosis
- Hormonal profiles: Personalized contraception selection
- Genetic testing integration:
💡 Master This: Systems thinking in gynecology reveals that reproductive health serves as a window into overall health status. Menstrual patterns reflect thyroid function, stress levels, and nutritional status. Fertility outcomes predict future cardiovascular risk. This integrated approach improves preventive care and long-term outcomes by addressing root causes rather than isolated symptoms.
Connect this systems integration through practical mastery tools to develop rapid clinical decision-making frameworks for complex gynecological presentations.
🔗 Advanced Integration: The Multi-System Gynecological Network
🎯 Clinical Mastery Arsenal: The Rapid Decision Framework
📌 Remember: MASTER - Memory tools, Assessment protocols, Systematic approach, Threshold values, Emergency recognition, Rapid decisions. This framework enables expert-level performance within 2-3 years of systematic practice rather than traditional 10-year experience curves.
- The 5-Minute Gynecological Assessment
- Minute 1: Chief complaint + red flag screening
- Acute pain >8/10: Rule out torsion, ruptured cyst, ectopic
- Heavy bleeding + hypotension: Hemodynamic instability protocol
- Postmenopausal bleeding: Malignancy until proven otherwise
- Minutes 2-3: Focused history + examination
- LMP, cycle pattern, contraception, sexual history
- Vital signs, abdominal examination, pelvic assessment
- Minutes 4-5: Differential diagnosis + investigation plan
- Top 3 diagnoses based on pattern recognition
- Targeted investigations with specific thresholds
- Minute 1: Chief complaint + red flag screening
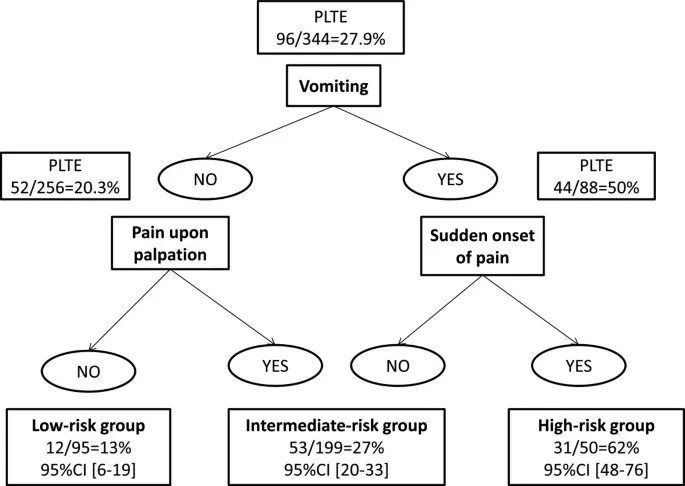
- Essential Threshold Arsenal
- Bleeding thresholds: >80ml/cycle (HMB), >7 days (prolonged)
- Pain thresholds: VAS >7/10 (severe), >6 months (chronic)
- Size thresholds: >5cm (follow-up), >10cm (surgery consideration)
- Age thresholds: >40 years (malignancy risk), <16 years (developmental)
- Laboratory thresholds: Hb <10 g/dl (anemia), CA-125 >200 (malignancy concern)
⭐ Clinical Pearl: The "Rule of 3s" for gynecological emergencies: 3 minutes for triage decision, 3 hours for definitive diagnosis, 3 days maximum for treatment initiation. This timeline prevents >95% of serious complications while maintaining diagnostic accuracy.
| Clinical Scenario | Key Decision Point | Critical Threshold | Action Required | Time Frame | Success Metric |
|---|---|---|---|---|---|
| Acute Pelvic Pain | Torsion vs other | Pain >8/10 + nausea | Emergency surgery | <6 hours | Organ salvage >90% |
| Heavy Bleeding | Hemodynamic status | SBP <90, HR >100 | IV access, CBC | <30 minutes | Stabilization >95% |
| Adnexal Mass | Malignancy risk | CA-125 >200, age >50 | Oncology referral | <2 weeks | Early detection >85% |
| Pelvic Pain Chronic | Endometriosis | Cyclical, VAS >6 | Laparoscopy | <3 months | Diagnosis >80% |
| Abnormal Bleeding | Structural cause | Age >40, IMB | Endometrial biopsy | <4 weeks | Cancer detection >95% |
- "See this, think that" associations:
- Cyclical pain → Endometriosis (85% probability)
- Irregular bleeding + hirsutism → PCOS (90% probability)
- Postcoital bleeding → Cervical pathology (75% probability)
- Pelvic pressure + urinary frequency → Fibroids (80% probability)
- Investigation selection logic:
- Transvaginal ultrasound: First-line for pelvic masses, bleeding
- MRI: Adenomyosis, deep endometriosis, surgical planning
- Laparoscopy: Chronic pain, infertility, definitive diagnosis
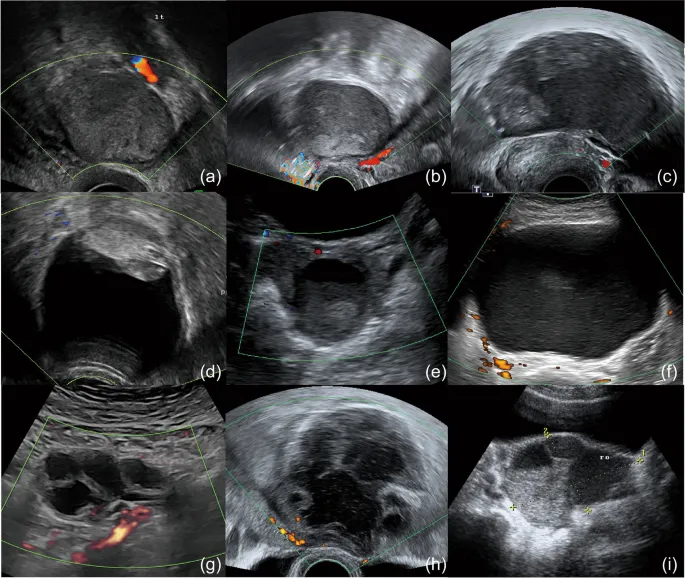
- Treatment Selection Matrix
- Conservative management: Age <35, mild symptoms, fertility desired
- Medical therapy: Moderate symptoms, contraception needed, surgery declined
- Minimally invasive surgery: Failed medical, fertility preservation, diagnostic uncertainty
- Definitive surgery: Severe symptoms, family complete, malignancy concern
💡 Master This: Clinical intuition develops through systematic pattern exposure combined with quantitative validation. Expert gynecologists achieve diagnostic accuracy >95% by integrating clinical patterns, investigation results, and treatment outcomes into rapid decision algorithms that can be learned and replicated through deliberate practice.
This comprehensive mastery framework transforms gynecological knowledge into practical clinical expertise, enabling confident diagnosis and optimal treatment selection across the full spectrum of reproductive health disorders.
🎯 Clinical Mastery Arsenal: The Rapid Decision Framework
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















