RT Fundamentals - Ray Basics & Bio
- Radiation Types:
- Photons (X-rays, γ-rays): Low LET, common.
- Particles (electrons, protons): Variable LET.
- Key Terms:
- Linear Energy Transfer (LET): Energy/unit path; ↑LET = ↑damage.
- Relative Biological Effectiveness (RBE): Biological damage vs reference radiation.
- Radiobiology's 4 R's:
- Repair (sublethal DNA damage)
- Redistribution (cells to sensitive cycle phases)
- Repopulation (normal & tumor cells)
- Reoxygenation (hypoxic tumor cells, ↑sensitivity)
⭐ Hypoxic cells: 2.5-3x more radioresistant than oxic cells.
Brachytherapy - Close Combat Radiation
- Delivers radiation directly to/near tumor, sparing normal tissues.
- Types:
- Low Dose Rate (LDR): Continuous, ~0.4-2 Gy/hr.
- High Dose Rate (HDR): Short bursts, >12 Gy/hr; common now.
- Pulsed Dose Rate (PDR): Pulses simulate LDR.
- Isotopes: $^{137}$Cs (LDR), $^{192}$Ir (HDR), $^{60}$Co, $^{125}$I.
- Indications: Cervical (boost after EBRT), endometrial, vaginal cancers.

⭐ HDR brachytherapy for cervical cancer often targets Point A (2 cm superior to external os, 2 cm lateral to cervical canal) to ~80-85 Gy total EQD2 (External Beam + Brachytherapy).
EBRT Techniques - Beaming from Afar
- External Beam Radiotherapy (EBRT) uses external radiation sources to target malignancies, complementing brachytherapy.
- Key Techniques:
- 3D-CRT (3D Conformal RT): Shapes radiation beams to match the planning target volume (PTV).
- IMRT (Intensity-Modulated RT): Advanced; modulates beam intensity for superior conformity and sparing of organs at risk (OARs).
- VMAT (Volumetric Modulated Arc Therapy): IMRT delivered in continuous rotational arcs, often improving treatment speed.
- Planning: Involves CT simulation for precise target volume delineation (GTV, CTV, PTV).
- Typical Pelvic EBRT Dose: 45-50 Gy in 1.8-2 Gy per fraction over 5-6 weeks.
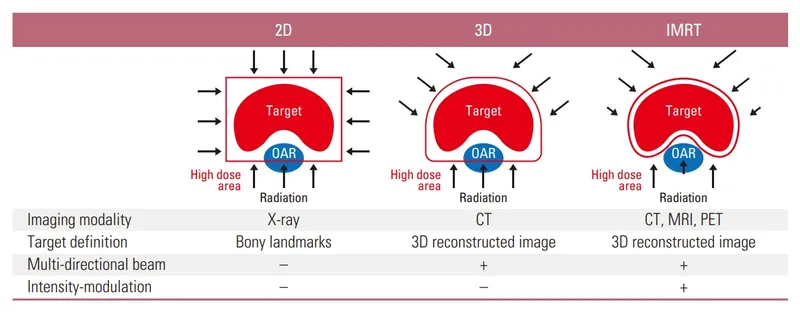
⭐ IMRT significantly reduces acute and late gastrointestinal and genitourinary toxicities compared to 3D-CRT in gynecologic cancers by better sparing the bladder and rectum. 📌 Intensity Modulation Reduces Toxicity (IMRT).
RT for Gynae Cancers - Site-Specific Strategies
-
Cervical Cancer:
- Early (FIGO IA-IIA1): Surgery primary. Adjuvant RT for high-risk (LVSI, +margins, nodes).
- Locally Advanced (FIGO IB2-IVA): Definitive Concurrent ChemoRT (CCRT).
- EBRT: 45-50 Gy + Brachytherapy (BT).
- Chemo: Weekly Cisplatin 40 mg/m².
- Flowchart:
-
Endometrial Cancer:
- Adjuvant RT post-surgery for high-risk:
- Vaginal Brachytherapy (VBT) for vaginal cuff recurrence prevention.
- EBRT for nodal/extensive disease (e.g., Grade 3, deep invasion, LVSI, Stage II/III).
- Adjuvant RT post-surgery for high-risk:
-
Vulvar/Vaginal Cancer:
- Vulvar: Adjuvant RT for +margins, +nodes. Primary RT for unresectable.
- Vaginal: Primary RT (EBRT + BT) often curative.
⭐ Point A in cervical cancer brachytherapy is defined as 2 cm superior to the cervical os and 2 cm lateral to the uterine canal; it's a critical dose prescription point.
RT Complications & Care - Damage Control
- Acute (During/Post-RT < 90 days):
- Skin: Erythema, dry/moist desquamation
- Mucosal: Cystitis, proctitis, vaginitis (pain, discharge, bleeding)
- GI: Nausea, vomiting, diarrhea
- Hematologic: Myelosuppression (esp. with chemo-RT)
- Late (Months-Years > 90 days):
- Fibrosis & Stenosis: Vaginal, rectal, ureteral
- Chronic: Proctitis, cystitis, enteropathy (malabsorption, obstruction)
- Fistulae (VVF, RVF), lymphedema, telangiectasias
- Ovarian failure, bone necrosis/fractures, secondary malignancies
- Management:
- Acute: Symptomatic (hydration, anti-emetics, anti-diarrheals, topical agents)
- Late: Vaginal dilators, pelvic floor PT, hyperbaric oxygen, surgical correction for fistulae/obstruction.
⭐ Vaginal stenosis is a common late effect of pelvic RT; counsel patients on regular use of vaginal dilators post-treatment to maintain patency and sexual function.
High‑Yield Points - ⚡ Biggest Takeaways
- Cervical cancer: Brachytherapy (LDR/HDR) is crucial with EBRT. Point A (2cm lateral, 2cm superior to os) is key.
- Endometrial cancer: Adjuvant vaginal brachytherapy for high-intermediate risk; EBRT for advanced disease.
- Ovarian cancer: Generally radioresistant; radiation is mainly palliative.
- Vulvar/Vaginal cancers: EBRT +/- brachytherapy, often with chemosensitization, for advanced stages.
- IMRT/VMAT spares organs, reducing acute toxicities like cystitis and proctitis.
- Chronic effects: Vaginal stenosis, fibrosis, fistulae formation possible after treatment for gynecologic malignancies with radiation therapy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

