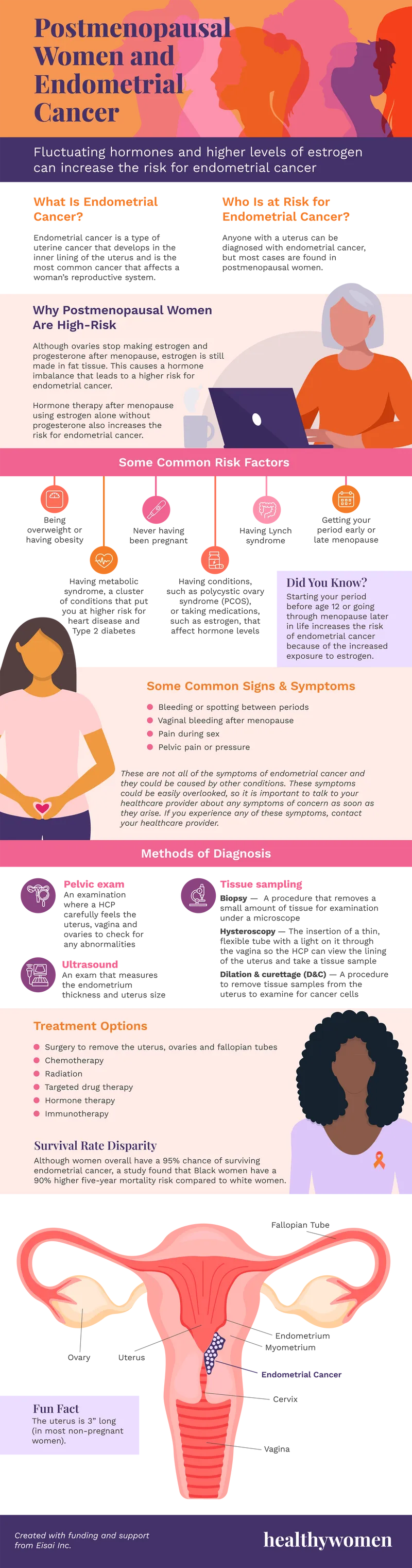
Endometrial Cancer: Epi & Risks - Cancer's Guest List
- Most common GYN malignancy (developed nations); 4th common cancer in women.
- Peak: 55-65 yrs (postmenopausal).
- Key Risk: Unopposed Estrogen
- Exogenous: Estrogen Replacement Therapy (ERT) without progestin.
- Endogenous:
- Obesity (↑ peripheral estrone).
- Nulliparity.
- Early menarche (<12 yrs).
- Late menopause (>52 yrs).
- PCOS (chronic anovulation).
- Estrogen-secreting tumors.
- Other Major Risks:
- Tamoxifen (endometrial agonist).
- Diabetes Mellitus, Hypertension.
- Lynch Syndrome (HNPCC).
- Family Hx (endometrial, ovarian, breast, colon).
- Prior pelvic radiation.
⭐ Lynch Syndrome (HNPCC) significantly ↑ endometrial cancer risk (40-60% lifetime), often preceding or co-occurring with colon cancer.
- Protective: Combined Oral Contraceptives (COCs), progestins, multiparity, smoking (paradoxical).
Endometrial Cancer: Patho & Types - Tumor's ID Card
- Precursor: Endometrial Hyperplasia (EH) → Atypical EH / Endometrial Intraepithelial Neoplasia (EIN) → Carcinoma.
- EH without atypia: Low malignant potential.
- Atypical EH / EIN: High risk (~30-50%) progression to carcinoma if untreated.

- Two Main Types: 📌 (Remember: Type I = Indolent/Estrogen; Type II = IIl/p53)
| Feature | Type I (Estrogen-Dependent) | Type II (Estrogen-Independent) |
|---|---|---|
| Frequency | ~80% | ~10-20% |
| Histology | Endometrioid | Serous, Clear cell, Carcinosarcoma |
| Pathogenesis | Unopposed E2, EIN precursor | p53 mut, atrophy |
| Patient Profile | Perimenopausal, obese | Postmenopausal, thin |
| Key Mutations | PTEN, KRAS, MSI, ARID1A | TP53, PPP2R1A |
| Prognosis | Better | Poorer |
- POLE ultramutated (Best prog, younger, immune "hot")
- MSI hypermutated (Good prog, Lynch, immune "hot")
- CN-low (Endometrioid, Intermediate prog)
- CN-high (Serous-like, TP53mut, Worst prog, immune "cold")
⭐ Lynch syndrome (HNPCC) significantly ↑ risk of endometrial cancer (MSI pathway), often the sentinel cancer.
Endometrial Cancer: Symptoms & Dx - Detective Work
- Symptoms:
- Most Common: Abnormal Uterine Bleeding (AUB).
- Postmenopausal Bleeding (PMB): Cancer until proven otherwise.
- Premenopausal: Irregular, heavy, or intermenstrual bleeding.
- Less Common:
- Serosanguinous/watery vaginal discharge.
- Pelvic pain or pressure (advanced).
- Pyometra (uterine pus).
- Most Common: Abnormal Uterine Bleeding (AUB).
- Diagnosis:
- Initial: Transvaginal Sonography (TVS).
- Measures Endometrial Thickness (ET).
- PMB: ET > 4-5 mm suspicious, requires sampling.
- Asymptomatic PM: ET > 11 mm may need investigation.
- Gold Standard: Endometrial Sampling.
- Office endometrial biopsy (Pipelle).
- Hysteroscopy + D&C if biopsy inconclusive or focal lesion.
- Staging: MRI pelvis, CT chest/abdomen.
- Initial: Transvaginal Sonography (TVS).

⭐ Any postmenopausal bleeding mandates investigation to rule out endometrial cancer.
Endometrial Cancer: Staging & Tx - Treatment Roadmap
FIGO 2023 Staging (Simplified)
| Stage | Description |
|---|---|
| I | Confined to corpus uteri |
| IA | No or <50% myometrial invasion |
| IB | ≥50% myometrial invasion |
| II | Cervical stromal invasion |
| > ⭐ Stage II: Cervical stromal invasion is key. | |
| III | Local/regional spread (serosa, adnexa, vagina, LN) |
| IIIC | Pelvic (IIIC1) or Para-aortic (IIIC2) LN mets |
| IV | Bladder/bowel mucosa (IVA) or distant mets (IVB) |
- Histologic Type (Endometrioid vs Non-endometrioid), Grade
- Depth of myometrial invasion, LVSI
- Lymph Node (LN) status, Molecular profile (POLE, MMRd, p53abn, NSMP)
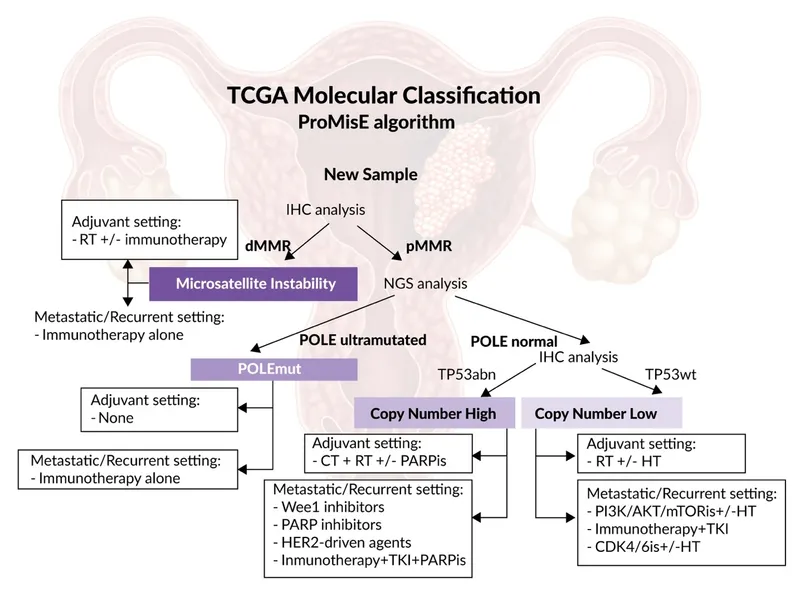
Simplified Treatment:
TAH+BSO: Total Hysterectomy + Bilateral Salpingo-oophorectomy; LND: Lymph Node Dissection; RT: Radiotherapy; VBT: Vaginal Brachytherapy; Rx: Therapy; EC: Endometrial Cancer.
High‑Yield Points - ⚡ Biggest Takeaways
- Endometrial cancer is the most common gynecologic malignancy, mainly in postmenopausal women.
- Unopposed estrogen (obesity, PCOS, tamoxifen) is the primary risk factor.
- Postmenopausal bleeding is the hallmark symptom; requires TVUS and endometrial biopsy.
- Type 1 (endometrioid): common (80%), estrogen-dependent, good prognosis.
- Type 2 (serous/clear cell): aggressive, p53 mutation, poorer prognosis.
- Strong association with Lynch syndrome (HNPCC).
- FIGO staging is surgical; cornerstone of management.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

