Gynecologic Oncology

On this page
🎯 Gynecologic Oncology: The Cancer Command Center
Gynecologic cancers demand precision at every turn-from recognizing subtle presentations to mapping disease extent, selecting optimal therapies, and coordinating complex care across specialties. You'll master the staging systems that guide treatment decisions, the diagnostic tools that reveal hidden disease, and the therapeutic strategies that balance cure with quality of life. This lesson builds your command of ovarian, endometrial, cervical, vulvar, and vaginal malignancies through integrated frameworks that connect pathophysiology to prognosis. By synthesizing detection, staging, treatment, and multidisciplinary collaboration, you'll develop the clinical judgment to navigate these challenging cases with confidence and deliver care that changes outcomes.
The epidemiological landscape reveals striking patterns: cervical cancer dominates in developing nations with 85% of cases occurring in resource-limited settings, while endometrial cancer prevails in developed countries with 75% of cases linked to obesity and metabolic syndrome. Ovarian cancer, the "silent killer," presents late in 70% of cases, contributing to its 5-year survival rate of 47% compared to cervical cancer's 66% when detected early.
📌 Remember: COVE-V - Cervix (HPV-driven), Ovary (silent presentation), Vulva (elderly), Endometrium (estrogen-excess), Vagina (rare, radiation-associated). Each site has distinct risk profiles and presentation patterns.
Understanding molecular pathogenesis reveals critical therapeutic targets. TP53 mutations occur in 96% of high-grade serous ovarian cancers, while PIK3CA mutations appear in 52% of endometrial cancers. HPV integration drives 99.7% of cervical cancers, with types 16 and 18 responsible for 70% of cases.
| Cancer Type | Peak Age | 5-Year Survival | Primary Risk Factor | Screening Method | Treatment Modality |
|---|---|---|---|---|---|
| Cervical | 35-44 years | 66% | HPV infection | Pap smear/HPV testing | Surgery + RT |
| Endometrial | 55-64 years | 81% | Estrogen excess | No routine screening | Surgery primary |
| Ovarian | 55-64 years | 47% | BRCA mutations | No effective screening | Surgery + chemo |
| Vulvar | 65-74 years | 71% | HPV/lichen sclerosus | Visual inspection | Wide local excision |
| Vaginal | 60-69 years | 52% | Prior radiation | Pap smear | Radiation therapy |
Staging systems follow FIGO classifications updated every 3-4 years to incorporate molecular markers and imaging advances. TNM staging parallels FIGO but emphasizes anatomical extent, while histologic grading (Grade 1-3) predicts biological behavior independent of stage.
💡 Master This: Gynecologic oncology success depends on the "Staging-Surgery-Systemic" triad. Accurate staging guides surgical planning, complete surgical resection determines local control, and systemic therapy addresses micrometastatic disease. Master this sequence, and you understand 90% of treatment decision-making.
The therapeutic arsenal includes surgery (primary modality for 80% of cases), radiation therapy (external beam + brachytherapy), chemotherapy (platinum-based combinations), targeted therapy (PARP inhibitors, bevacizumab), and immunotherapy (pembrolizumab for MSI-high tumors). Treatment selection follows evidence-based algorithms incorporating stage, histology, molecular markers, and performance status.
Connect these foundational concepts through systematic staging approaches to understand how anatomical extent determines treatment intensity and survival predictions.
🎯 Gynecologic Oncology: The Cancer Command Center
🗺️ Staging Systems: The Cancer Cartography
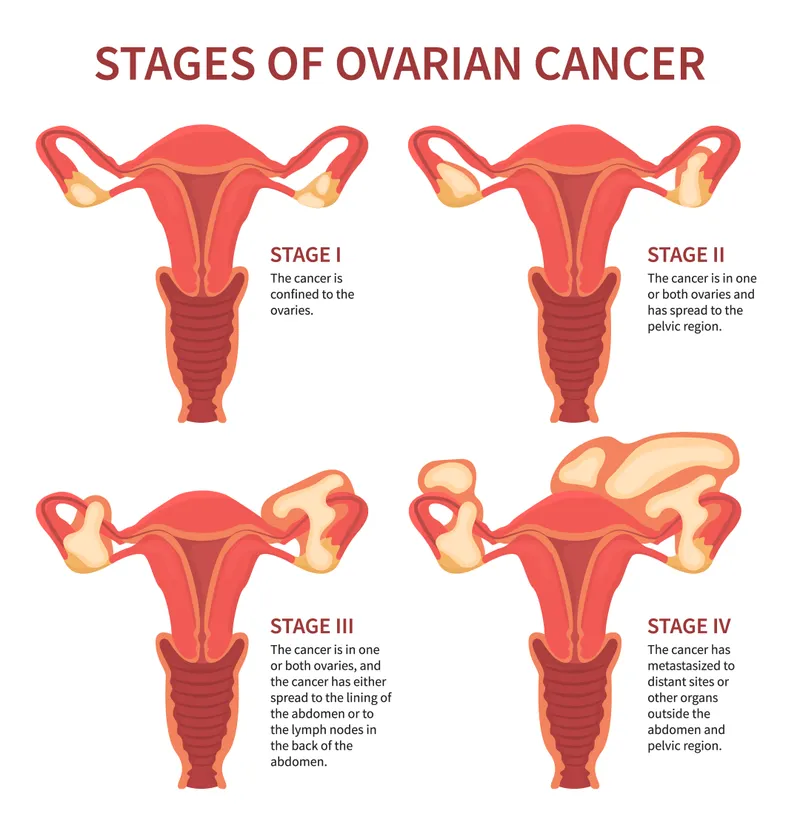
The staging philosophy follows anatomical progression patterns: Stage I (confined to organ of origin), Stage II (local extension), Stage III (regional spread), and Stage IV (distant metastases). However, each cancer type has unique staging criteria reflecting distinct spread patterns and prognostic factors.
📌 Remember: "FIGO Flows Forward" - First organ confined, Involvement local, Goes regional, Outside distant. Stage progression follows predictable anatomical pathways specific to each cancer type.
Cervical cancer staging emphasizes parametrial involvement and nodal status. Stage IB1 (≤2 cm) versus IB2 (2-4 cm) determines surgical versus chemoradiation approach. Stage IIA (upper vaginal involvement) maintains 85% 5-year survival, while Stage IIIC (pelvic node involvement) drops to 45%.
Endometrial cancer staging focuses on myometrial invasion depth and extrauterine spread. Stage IA (<50% myometrial invasion) has 95% 5-year survival versus Stage IB (≥50% invasion) with 85% survival. Lymphovascular space invasion (LVSI) upgrades risk category regardless of stage.
| Staging Factor | Cervical Impact | Endometrial Impact | Ovarian Impact | Survival Change |
|---|---|---|---|---|
| Tumor size >4cm | IB1→IB2 | No stage change | No stage change | 15% decrease |
| Myometrial >50% | N/A | IA→IB | N/A | 10% decrease |
| Positive nodes | Any→IIIC | Any→IIIC | Any→IIIC | 25-40% decrease |
| Distant mets | Any→IV | Any→IV | Any→IV | 60-70% decrease |
| Peritoneal cytology | No impact | No impact (2018) | IIIA if positive | 5-10% decrease |
⭐ Clinical Pearl: The "Centimeter Rule" governs ovarian cancer outcomes - <1 cm residual disease after surgery doubles median survival compared to >1 cm residual. This drives the aggressive cytoreductive approach, including bowel resection and diaphragm stripping when necessary.
Imaging integration revolutionized staging accuracy. PET-CT detects 85% of nodal metastases versus 65% for CT alone in cervical cancer. MRI demonstrates 92% accuracy for myometrial invasion depth in endometrial cancer. CA-125 levels correlate with disease burden in ovarian cancer, with >500 U/mL predicting suboptimal cytoreduction in 75% of cases.
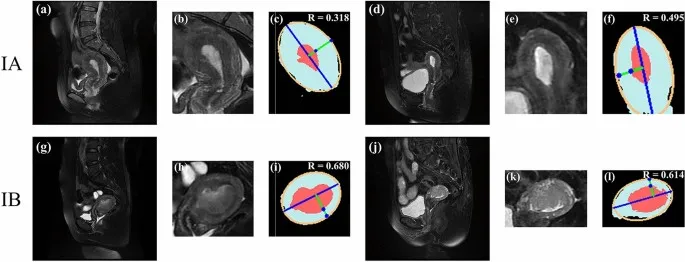
Molecular staging emerges as the future paradigm. MSI-high endometrial cancers (15% of cases) respond to immunotherapy regardless of stage. BRCA-mutated ovarian cancers show superior response to PARP inhibitors independent of traditional staging. p16 expression in cervical cancer correlates with HPV integration and radiation sensitivity.
💡 Master This: Modern staging integrates anatomical extent + molecular markers + imaging findings to create personalized risk profiles. Traditional FIGO stages provide the framework, but molecular characteristics increasingly determine treatment selection and prognosis prediction.
Surgical staging remains the gold standard for endometrial and ovarian cancers, requiring systematic lymphadenectomy and peritoneal sampling. Clinical staging suffices for cervical cancer due to excellent MRI correlation and the chemoradiation standard for locally advanced disease.
Connect staging precision through treatment selection algorithms to understand how anatomical mapping translates into therapeutic intensity and survival optimization.
🗺️ Staging Systems: The Cancer Cartography
⚔️ Treatment Arsenal: The Therapeutic Command Center
Surgical principles emphasize complete resection with negative margins while preserving functional anatomy when possible. Radical hysterectomy for cervical cancer requires parametrial resection and pelvic lymphadenectomy. Cytoreductive surgery for ovarian cancer aims for <1 cm residual disease, often requiring bowel resection and diaphragm stripping.
📌 Remember: "SCOPE" surgical principles - Staging complete, Cytoreduction optimal, Organ preservation when safe, Parameters molecular, Expertise specialized. These principles guide surgical decision-making across all gynecologic cancers.
Radiation therapy utilizes external beam (EBRT) and brachytherapy combinations. Intensity-modulated radiation therapy (IMRT) delivers 45-50.4 Gy to pelvic fields while limiting bowel dose to <45 Gy and bladder dose to <50 Gy. High-dose-rate brachytherapy provides targeted boost to 85-90 Gy equivalent dose.
Chemotherapy regimens follow platinum-based combinations as the backbone. Carboplatin + paclitaxel every 21 days for 6 cycles represents the standard for ovarian and endometrial cancers. Cisplatin + radiation (chemoradiation) provides the standard for locally advanced cervical cancer.
| Cancer Type | First-Line Regimen | Response Rate | Median PFS | Median OS | Key Toxicities |
|---|---|---|---|---|---|
| Ovarian | Carboplatin + Paclitaxel | 75-80% | 18-22 months | 44-57 months | Neuropathy, myelosuppression |
| Endometrial | Carboplatin + Paclitaxel | 60-70% | 13-16 months | 32-38 months | Neuropathy, fatigue |
| Cervical | Cisplatin + Radiation | 85-90% | 24-30 months | 43-49 months | Nephrotoxicity, neuropathy |
| Recurrent | Bevacizumab combinations | 40-50% | 10-14 months | 17-24 months | Hypertension, bleeding |
⭐ Clinical Pearl: The "BRCA Advantage" - Patients with BRCA1/2 mutations show superior response to platinum chemotherapy (85% vs 60%) and PARP inhibitors (median PFS 22 months vs 10 months). Genetic testing should be performed in all ovarian cancer patients and high-risk endometrial cancers.
Immunotherapy emerges for microsatellite instability-high (MSI-H) tumors. Pembrolizumab achieves 57% response rate in MSI-H endometrial cancer versus 9% in microsatellite stable tumors. Dostarlimab shows 100% complete response in MSI-H rectal cancer, suggesting similar potential in gynecologic cancers.
Treatment sequencing optimizes outcomes through neoadjuvant, adjuvant, and maintenance strategies. Neoadjuvant chemotherapy for advanced ovarian cancer achieves similar survival to primary cytoreduction with reduced morbidity. Adjuvant radiation for high-risk endometrial cancer reduces local recurrence by 50%.
Toxicity management requires proactive monitoring and dose modifications. Carboplatin AUC 5-6 provides optimal efficacy-toxicity balance. Paclitaxel neuropathy affects 60% of patients, requiring dose reduction at Grade 2 symptoms. Bevacizumab requires blood pressure monitoring and proteinuria assessment.
💡 Master This: Modern gynecologic oncology follows "Precision Medicine Principles" - molecular profiling guides targeted therapy selection, genetic testing identifies hereditary syndromes, and biomarker assessment predicts treatment response. Master these connections, and you optimize outcomes for every patient.
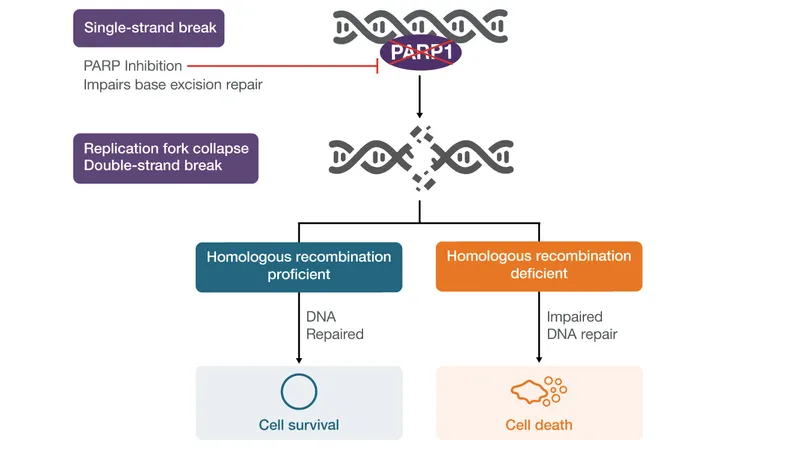
Combination strategies enhance efficacy through synergistic mechanisms. Chemoradiation exploits radiation sensitization by cisplatin. PARP inhibitor maintenance capitalizes on platinum-induced DNA damage. Immunotherapy combinations overcome immune suppression in the tumor microenvironment.
Connect treatment precision through outcome monitoring to understand how therapeutic algorithms translate into survival optimization and quality of life preservation.
⚔️ Treatment Arsenal: The Therapeutic Command Center
🔍 Diagnostic Mastery: The Detection Command Center
Clinical presentation patterns follow predictable anatomical distributions. Cervical cancer presents with postcoital bleeding in 75% of early cases and pelvic pain in 60% of advanced cases. Endometrial cancer causes postmenopausal bleeding in 90% of cases, with <5% having normal bleeding patterns. Ovarian cancer remains asymptomatic until Stage III in 70% of cases.
📌 Remember: "BLEEDING Signals" - Bladder symptoms (cervical), Late presentation (ovarian), Early bleeding (endometrial), Elderly vulvar lesions, Discharge abnormal, Increasing abdominal girth, Nodular masses, Gastrointestinal symptoms. Each cancer has distinct presentation patterns.
Imaging modalities provide complementary information for detection and staging. Transvaginal ultrasound detects endometrial thickness >4 mm in postmenopausal women with 96% sensitivity for cancer. MRI demonstrates 92% accuracy for myometrial invasion depth and 85% accuracy for cervical parametrial involvement.
| Imaging Modality | Primary Use | Sensitivity | Specificity | Key Findings | Limitations |
|---|---|---|---|---|---|
| Transvaginal US | Endometrial screening | 96% | 68% | Thickness >4mm | Operator dependent |
| Pelvic MRI | Local staging | 85-92% | 88-95% | T2 signal changes | Motion artifacts |
| CT chest/abdomen | Metastases detection | 75-85% | 90-95% | Lymphadenopathy | Radiation exposure |
| PET-CT | Recurrence detection | 90-95% | 85-90% | FDG uptake | False positives |
| CA-125 | Ovarian monitoring | 80% | 75% | >35 U/mL abnormal | Benign elevations |
Histopathological diagnosis requires adequate tissue sampling and expert interpretation. Endometrial biopsy achieves 95% accuracy for cancer detection with <1% complication rate. Cervical biopsy following abnormal cytology provides definitive diagnosis in 98% of cases. Ovarian tissue requires frozen section analysis during surgery for immediate treatment planning.
⭐ Clinical Pearl: The "Tissue is the Issue" principle - Cytology screens, imaging localizes, but histopathology diagnoses. Never treat gynecologic cancer without tissue confirmation except in life-threatening emergencies requiring immediate intervention.
Molecular diagnostics increasingly guide treatment decisions. HPV testing identifies high-risk types in 99.7% of cervical cancers. MSI testing detects microsatellite instability in 15% of endometrial cancers, predicting immunotherapy response. BRCA testing identifies hereditary mutations in 15-20% of ovarian cancers.
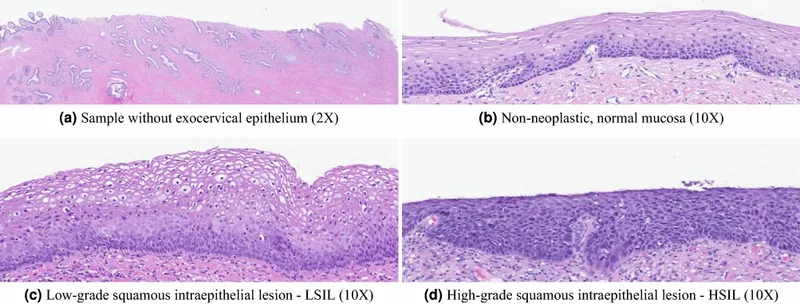
Screening effectiveness varies dramatically by cancer type. Cervical cancer screening with Pap smears reduces incidence by 65% and mortality by 70%. HPV testing extends screening intervals to 5 years with superior sensitivity. Ovarian cancer screening with CA-125 + ultrasound shows no mortality benefit in randomized trials.
Diagnostic accuracy depends on pre-test probability and test characteristics. Positive predictive value of abnormal Pap smear ranges from 15% (low-grade) to 85% (high-grade) depending on cytological severity. Endometrial biopsy in postmenopausal bleeding has positive predictive value of 25% for cancer.
💡 Master This: Diagnostic mastery requires understanding "Bayesian Principles" - pre-test probability (patient risk factors) combined with test characteristics (sensitivity/specificity) determines post-test probability (likelihood of disease). Master this calculation, and you optimize diagnostic accuracy while minimizing unnecessary procedures.
Quality assurance ensures diagnostic reliability through standardized protocols and expert review. Cytopathology requires annual proficiency testing and 5% random review. Histopathology benefits from subspecialty consultation for complex cases and immunohistochemical confirmation.
Connect diagnostic precision through prognostic stratification to understand how accurate detection enables personalized treatment planning and outcome optimization.
🔍 Diagnostic Mastery: The Detection Command Center
⚖️ Prognostic Stratification: The Outcome Prediction Engine
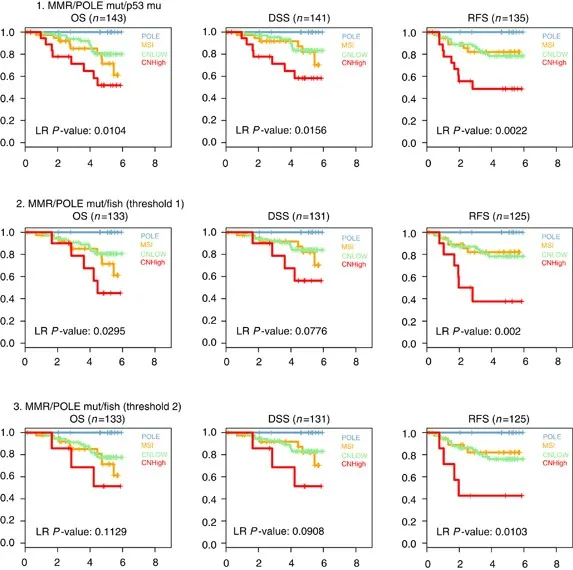
Traditional prognostic factors provide the foundation for risk assessment. Stage remains the strongest predictor, with 5-year survival ranging from 95% (Stage I) to 15% (Stage IV) across cancer types. Histologic grade independently predicts recurrence risk, with Grade 3 tumors showing 3-fold higher recurrence rates than Grade 1.
📌 Remember: "STAGE-GRADE-AGE" trinity - STAGE determines anatomical extent, GRADE predicts biological behavior, AGE influences treatment tolerance. These three factors account for 70% of prognostic variance in gynecologic cancers.
Molecular prognostic markers revolutionize risk stratification. p53 mutations in ovarian cancer correlate with chemoresistance and shorter survival. POLE mutations in endometrial cancer predict excellent prognosis despite high-grade histology. HPV integration in cervical cancer determines radiation sensitivity and local control rates.
| Prognostic Factor | Cancer Type | Favorable Feature | Unfavorable Feature | Survival Impact | Clinical Action |
|---|---|---|---|---|---|
| BRCA status | Ovarian | Mutated | Wild-type | +12 months OS | PARP inhibitor |
| MSI status | Endometrial | MSI-high | MSS | +24 months OS | Immunotherapy |
| HPV type | Cervical | Types 16/18 | Other types | +15% 5-year | Standard RT |
| Residual disease | Ovarian | <1 cm | >1 cm | +15 months OS | Aggressive surgery |
| LVSI | Endometrial | Absent | Present | +20% 5-year | Adjuvant therapy |
Age-related prognostic factors significantly impact outcomes. Elderly patients (>70 years) show 20-30% worse survival due to comorbidities and treatment intolerance. Young patients (<40 years) with endometrial cancer have higher rates of Lynch syndrome and aggressive histologies but better treatment tolerance.
Performance status predicts treatment completion and survival. ECOG 0-1 patients complete planned chemotherapy in 85% of cases versus 45% for ECOG 2-3 patients. Charlson Comorbidity Index >3 correlates with increased surgical morbidity and decreased overall survival.
⭐ Clinical Pearl: The "Fitness-Biology-Burden" model optimizes treatment decisions - Patient fitness (performance status, comorbidities) determines treatment tolerance, tumor biology (grade, molecular markers) predicts treatment response, and disease burden (stage, volume) defines treatment intensity requirements.
Nomograms provide individualized risk prediction by combining multiple prognostic factors. Memorial Sloan Kettering nomograms predict 5-year survival with concordance indices of 0.75-0.85 across gynecologic cancers. Online calculators enable real-time risk assessment during patient counseling.
Dynamic prognostication updates risk assessment based on treatment response. CA-125 kinetics during chemotherapy predict survival in ovarian cancer. Complete pathological response to neoadjuvant chemotherapy improves 5-year survival by 25%. Circulating tumor DNA provides real-time monitoring of treatment efficacy.
Quality of life factors increasingly influence prognostic discussions. Functional status preservation may outweigh marginal survival gains in elderly patients. Fertility preservation considerations affect treatment selection in young patients with early-stage disease.
💡 Master This: Modern prognostication follows "Precision Medicine Principles" - integrate clinical factors + molecular markers + patient preferences to create individualized treatment plans. Static staging evolves into dynamic risk assessment that adapts to treatment response and patient priorities.
Prognostic communication requires balanced honesty with realistic hope. Median survival provides population estimates but individual variation spans wide ranges. Best-case/worst-case scenarios help patients understand uncertainty while maintaining treatment motivation.
Connect prognostic precision through survivorship planning to understand how outcome prediction enables personalized follow-up strategies and long-term care optimization.
⚖️ Prognostic Stratification: The Outcome Prediction Engine
🔗 Multidisciplinary Integration: The Care Coordination Matrix
Surgical oncology provides primary treatment for 80% of gynecologic cancers, requiring subspecialty expertise in complex procedures. Gynecologic oncologists complete 4-year fellowships focusing on radical surgery, cytoreductive techniques, and perioperative management. Optimal cytoreduction rates improve from 45% (general gynecologists) to 85% (subspecialists).
Medical oncology delivers systemic therapy with evidence-based protocols and toxicity management. Chemotherapy completion rates reach 90% with subspecialty care versus 70% with general oncology. Clinical trial enrollment increases 5-fold at specialized centers, providing access to innovative therapies.
📌 Remember: "TEAM-CARE" principles - Tumor board coordination, Evidence-based protocols, Advanced subspecialty training, Multidisciplinary communication, Clinical trial access, Adjuvant therapy optimization, Recurrence monitoring, End-of-life planning. These elements define comprehensive gynecologic oncology care.
Radiation oncology requires specialized techniques for gynecologic anatomy. Intensity-modulated radiation therapy (IMRT) reduces bowel toxicity by 40% compared to conventional techniques. Image-guided brachytherapy achieves local control rates >95% in cervical cancer while minimizing late complications.
| Specialty | Primary Role | Key Expertise | Outcome Impact | Collaboration Points |
|---|---|---|---|---|
| Gynecologic Surgery | Primary treatment | Radical procedures | 25% survival improvement | Staging, cytoreduction |
| Medical Oncology | Systemic therapy | Chemotherapy protocols | 20% completion rates | Neoadjuvant, adjuvant |
| Radiation Oncology | Local control | IMRT, brachytherapy | 40% toxicity reduction | Chemoradiation |
| Pathology | Diagnosis | Molecular markers | 95% accuracy | Staging, biomarkers |
| Radiology | Imaging | Advanced techniques | 85% staging accuracy | Response assessment |
Genetic counseling identifies hereditary cancer syndromes in 15-25% of patients. BRCA testing should be performed in all ovarian cancer patients and high-risk endometrial cancers. Lynch syndrome screening uses immunohistochemistry for mismatch repair proteins in all endometrial cancers.
Supportive care integration addresses symptom management, nutritional support, and psychosocial needs. Palliative care consultation improves quality of life scores by 30% and reduces hospitalizations by 25% in advanced cancer patients. Social work involvement ensures insurance navigation and resource coordination.
⭐ Clinical Pearl: The "Hub-and-Spoke Model" optimizes care delivery - Gynecologic oncologists serve as the central hub coordinating subspecialty spokes (medical oncology, radiation, pathology, genetics). This model ensures continuity while leveraging specialized expertise for optimal outcomes.
Clinical trial integration provides access to innovative therapies and cutting-edge research. Academic centers enroll 40% of patients in clinical trials versus 5% at community centers. Biomarker-driven trials increasingly require molecular profiling and specialized infrastructure.
Quality metrics monitor multidisciplinary performance and outcome optimization. Time to treatment initiation should be <30 days from diagnosis. Tumor board presentation should occur within 7 days of tissue diagnosis. Treatment plan documentation requires consensus recommendations with evidence citations.
Communication protocols ensure seamless information transfer between specialties. Electronic health records enable real-time updates and shared decision-making. Patient portals provide treatment summaries and follow-up instructions. Nurse navigation coordinates appointments and addresses concerns.
💡 Master This: Multidisciplinary excellence requires "Orchestrated Expertise" - each specialist contributes unique knowledge while maintaining shared accountability for patient outcomes. Master the coordination principles, and you optimize every aspect of gynecologic cancer care from diagnosis through survivorship.
Technology integration enhances multidisciplinary coordination through telemedicine, molecular tumor boards, and artificial intelligence. Virtual consultations expand subspecialty access to underserved areas. AI-assisted imaging improves diagnostic accuracy and treatment planning.
Connect multidisciplinary coordination through survivorship care to understand how team-based approaches optimize long-term outcomes and quality of life preservation.
🔗 Multidisciplinary Integration: The Care Coordination Matrix
🎯 Clinical Mastery Arsenal: The Expertise Toolkit
Essential Clinical Algorithms provide decision-making frameworks for complex scenarios. Treatment selection follows evidence-based pathways incorporating stage, histology, molecular markers, and performance status. Recurrence management requires systematic evaluation of treatment history, disease-free interval, and anatomical distribution.
📌 Remember: "MASTER-GYN" clinical framework - Molecular profiling guides therapy, Algorithms standardize decisions, Staging determines prognosis, Team coordination optimizes care, Evidence drives protocols, Recurrence patterns predict outcomes, Genetics identify syndromes, Yield optimization through subspecialty care, Navigation ensures continuity.
Critical Numbers Arsenal enables rapid clinical assessment and treatment planning:
- Cervical Cancer: Stage IB1 (≤2 cm) → surgery; Stage IB2 (>2 cm) → chemoradiation
- Endometrial Cancer: Grade 1 + <50% invasion → surgery alone; high-risk features → adjuvant therapy
- Ovarian Cancer: CA-125 >500 predicts suboptimal cytoreduction in 75%; BRCA mutation → PARP inhibitor maintenance
- Recurrence: Platinum-free interval >6 months → platinum rechallenge; <6 months → alternative agents
| Clinical Scenario | Key Decision Point | Critical Threshold | Treatment Implication | Survival Impact |
|---|---|---|---|---|
| Cervical tumor size | Surgery vs radiation | 4 cm diameter | Radical hysterectomy vs chemoRT | 15% survival difference |
| Ovarian cytoreduction | Optimal vs suboptimal | 1 cm residual | Primary vs interval surgery | 15 months median OS |
| Endometrial invasion | Adjuvant therapy | 50% myometrial depth | Observation vs treatment | 10% recurrence reduction |
| Platinum sensitivity | Rechallenge eligibility | 6 months disease-free | Same vs different regimen | 8 months PFS difference |
- "See postmenopausal bleeding → Think endometrial cancer" (90% association)
- "See postcoital bleeding → Think cervical lesion" (75% association)
- "See abdominal distension + CA-125 >200 → Think ovarian cancer" (85% association)
- "See young patient + endometrial cancer → Think Lynch syndrome" (25% association)
⭐ Clinical Pearl: The "Rule of Sixes" in gynecologic oncology - 6 cycles standard chemotherapy, 6 months platinum sensitivity threshold, 6 weeks post-surgery recovery, 6 months follow-up intervals early stage, 6 years peak recurrence risk, 60 years average diagnosis age. These sixes guide timing decisions across treatment phases.
Molecular Medicine Integration transforms treatment selection:
Toxicity Management Protocols ensure treatment completion and quality of life:
- Carboplatin: Monitor AUC dosing, renal function, platelet counts
- Paclitaxel: Premedication prevents hypersensitivity; dose reduction for Grade 2 neuropathy
- Bevacizumab: Blood pressure control, proteinuria monitoring, wound healing considerations
- PARP inhibitors: Fatigue management, nausea control, myelosuppression monitoring
💡 Master This: Clinical excellence requires "Algorithmic Thinking" - systematic evaluation of clinical variables through evidence-based pathways that optimize outcomes while minimizing toxicity. Master these decision trees, and you provide expert-level care for every gynecologic cancer patient.
Follow-up Optimization balances recurrence detection with cost-effectiveness:
- Physical examination every 3-4 months for 2 years, then every 6 months
- Imaging only for symptomatic patients or clinical suspicion
- CA-125 monitoring in ovarian cancer with rising levels prompting evaluation
- Survivorship care addressing late effects, sexual health, psychological support
Emergency Recognition enables rapid intervention for life-threatening complications:
- Bowel obstruction: 80% of recurrent ovarian cancer patients
- Neutropenic fever: Immediate antibiotics within 1 hour
- Tumor lysis syndrome: Aggressive hydration and allopurinol
- Hypercalcemia: Bisphosphonates and aggressive hydration
🎯 Clinical Mastery Arsenal: The Expertise Toolkit
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















