Congenital Uterine Anomalies - Womb Wonders & Woes
- ASRM classification (Class I-VII) guides diagnosis. Prevalence: ~5.5% general, up to 24% in RPL.
- Common Types: Septate (most frequent, poorest prognosis), Bicornuate (partial/complete fusion failure), Arcuate (mildest).
- Impact: ↑ Implantation failure, RPL, preterm labor, malpresentation.
- Diagnosis:
- Screening: HSG (cavity), 3D USG (cavity + fundus).
- Confirmation: MRI (non-invasive), Hysteroscopy + Laparoscopy (gold standard).
- Management: Hysteroscopic metroplasty for symptomatic septate uterus significantly improves live birth rates.

⭐ Septate uterus has the worst obstetric outcome among Mullerian anomalies and benefits most from surgical correction (hysteroscopic metroplasty).
Uterine Fibroids & Polyps - Pesky Pelvic Growths
Uterine Fibroids (Leiomyomas): Benign myometrial tumors.
- FIGO Classification (Impacting Cavity):
- Type 0: Pedunculated intracavitary.
- Type 1: Submucosal <50% intramural.
- Type 2: Submucosal ≥50% intramural.
- Type 3: Intramural, contacts endometrium.
- Impact on Fertility: Submucosal (FIGO 0, 1, 2) & large intramural (if distorting cavity) can ↓ implantation & ↑ miscarriage via cavity distortion, inflammation, altered contractility.
- Diagnosis: USG, Saline Infusion Sonography (SIS), Hysteroscopy, MRI.
- Management (Fertility): Myomectomy (hysteroscopic for submucosal; laparoscopic/abdominal for others). UAE generally avoided.

Endometrial Polyps: Benign endometrial overgrowths.
- Impact on Fertility: May cause inflammation or mechanical interference with implantation.
- Diagnosis: USG, SIS, Hysteroscopy.
- Management (Fertility): Hysteroscopic polypectomy usually recommended.
⭐ Submucosal fibroids (FIGO type 0, 1, 2) have the most significant negative impact on fertility and ART outcomes, and their removal is generally recommended.
Management Algorithm for Fibroids in Infertility:
Intrauterine Adhesions & Endometritis - Sticky Situations & Infections
- Intrauterine Adhesions (IUA) / Asherman's Syndrome: Fibrous bands within uterine cavity.
- Etiology: Post-curettage (esp. post-partum/abortal), endometritis (e.g., genital TB).
- Clinical: Amenorrhea/hypomenorrhea, infertility, Recurrent Pregnancy Loss (RPL).
- Diagnosis: HSG/SIS (filling defects); Hysteroscopy (gold standard for diagnosis & adhesiolysis). AFS/ESGE classification.
- Management: Hysteroscopic adhesiolysis; strategies to prevent recurrence (IUD, estrogen therapy, anti-adhesion barriers).
⭐ Hysteroscopy is the gold standard for both diagnosis and treatment (adhesiolysis) of Asherman's syndrome.
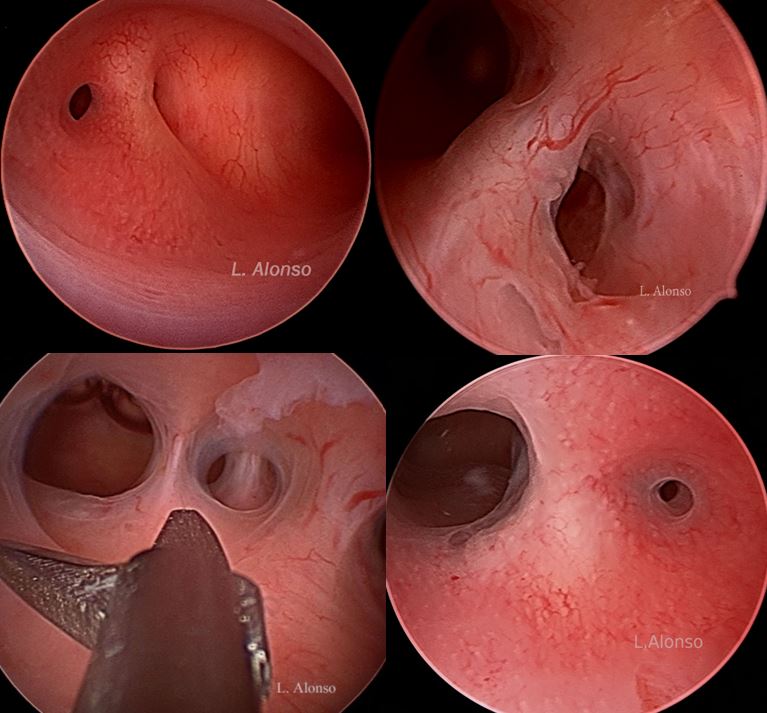
- Chronic Endometritis (CE): Persistent endometrial inflammation.
- Etiology: Bacterial (often polymicrobial).
- Diagnosis: Hysteroscopy with endometrial biopsy (key: plasma cells CD138+).
- Treatment: Antibiotics (e.g., Doxycycline 100mg BD x 14 days).
Adenomyosis & Endometrial Receptivity - Implantation Impediments
- Adenomyosis: Ectopic endometrial glands/stroma within myometrium.
- Fertility Impact: Impaired implantation, altered uterine contractility, inflammation, hostile environment.
- Diagnosis:
- TVUS: Heterogeneous myometrium, cystic anechoic spaces, '?' mark sign.

- MRI: Thickened Junctional Zone (JZ) >12mm.
- TVUS: Heterogeneous myometrium, cystic anechoic spaces, '?' mark sign.
- Management: GnRH agonists pre-IVF; surgery has limited fertility utility.
- Endometrial Receptivity:
- Key Factors:
- Endometrial thickness >7-8mm.
- Trilaminar pattern (USG).
- Molecular markers (e.g., ERA test - investigational).
- Thin Endometrium (<7mm):
- Causes: e.g., Asherman's syndrome, clomiphene use.
- Treatments (variable evidence): Estrogen, aspirin, sildenafil, G-CSF, PRP.
- Key Factors:
⭐ A junctional zone (JZ) thickness of ≥12 mm on MRI is a key diagnostic criterion for adenomyosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Asherman's syndrome (intrauterine adhesions), often post-D&C, severely impacts fertility.
- Congenital uterine anomalies, especially septate uterus (most common, surgically correctable), cause recurrent pregnancy loss.
- Submucosal and cavity-distorting intramural leiomyomas (fibroids) are key culprits for infertility.
- Endometrial polyps can interfere with embryo implantation.
- Hysterosalpingography (HSG) and hysteroscopy are primary diagnostic tools for uterine cavity evaluation.
- Chronic endometritis can impair endometrial receptivity and implantation success.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

