Tubal Anatomy & Function - Tube Tales
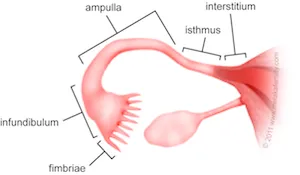
- Parts (Medial to Lateral):
- Interstitial (Intramural): narrowest, within uterine wall.
- Isthmus: narrow, thick-walled.
- Ampulla: widest, longest; commonest fertilization site.
- Infundibulum: funnel-shaped end with fimbriae.
- Fimbriae: finger-like projections; capture ovum.
- Histology:
- Mucosa: Ciliated cells (transport), Peg cells (nutrition).
- Muscularis: Peristalsis.
- Key Functions:
- Ovum pick-up by fimbriae.
- Sperm & ovum transport (cilia, peristalsis).
- Site of fertilization (ampulla).
⭐ Fertilization most commonly occurs in the ampullary region of the fallopian tube.
Tubal Pathologies - Blockage Blues
- Pelvic Inflammatory Disease (PID): Leading cause of tubal damage.
- Common organisms: Chlamydia trachomatis, Neisseria gonorrhoeae.
- Pathogenesis of tubal damage post-PID:
- Other Key Factors & Consequences:
-
Hydrosalpinx: Distally blocked tube filled with serous fluid; often visible on HSG or ultrasound.
-
Pyosalpinx: Accumulation of pus in the fallopian tube.
-
Tubal Adhesions: Fibrous bands distorting tubal anatomy; post-PID, endometriosis, or surgery.
-
Salpingitis Isthmica Nodosa (SIN): Nodular thickening and diverticula of the isthmic portion of the fallopian tube.
-
Previous Ectopic Pregnancy: Can result in significant tubal damage.
-
Tubal Surgery: Prior sterilization, reversal attempts, or other adnexal surgery.
-
Congenital Tubal Anomalies: Rare, e.g., segmental atresia.
-
⭐ Chlamydia trachomatis is a leading cause of tubal factor infertility due to silent PID, often asymptomatic until infertility investigation.
Peritoneal Problems - Adhesion Afflictions
- Endometriosis:
- Impacts fertility: distorted anatomy, adhesions, altered peritoneal fluid.
- Severity graded by staging systems (e.g., r-ASRM).
- Pelvic Adhesions:
- Etiology: Post-surgical (common), post-infectious (e.g., PID), Inflammatory Bowel Disease.
- Forms: Peritubal, omental adhesions.
- Mechanism: Impair fimbrial mobility & ovum pick-up.

⭐ Endometriosis can cause infertility through distorted anatomy, adhesions, and altered peritoneal fluid.
Diagnostic Detective Work - Imaging Insights
- Hysterosalpingography (HSG):
- Procedure: Fluoroscopic imaging after uterine injection of contrast (oil or water-based).
- Findings: Tubal patency (spill), uterine cavity (filling defects like polyps, synechiae), hydrosalpinx.

- Sonohysterosalpingography (HyCoSy/SHG):
- Ultrasound-based; uses agitated saline or contrast.
- Advantages: No radiation, office procedure, good for uterine cavity assessment, often better tolerated.
- Laparoscopy & Dye Test (Chromopertubation):
- Gold standard for tubal and peritoneal factor assessment.
- Direct visualization of pelvic anatomy, dye spill (patency), adhesions, endometriosis.
- Indications: High suspicion of tubal/peritoneal disease, failed previous investigations/treatments.
- Chlamydia Antibody Testing (CAT):
- Screens for past Chlamydia trachomatis infection (IgG antibodies), a key risk factor for tubal damage.
⭐ Laparoscopy with chromopertubation is considered the gold standard for assessing tubal patency and peritoneal factors.
Treatment Tactics - Fertility Fixes
- Surgery Success: Salpingostomy/Fimbrioplasty ~20-30%; Reanastomosis ~50-70% pregnancy rates.
- IVF: Primary for severe disease. Pre-IVF: treat hydrosalpinx (salpingectomy/occlusion).
- Adhesiolysis for adhesions; manage endometriosis.
⭐ IVF often bypasses tubal issues, being most effective for significant tubal factor infertility.
High‑Yield Points - ⚡ Biggest Takeaways
- Pelvic Inflammatory Disease (PID), often from Chlamydia, is the leading cause of tubal factor infertility.
- HSG is key for initial tubal patency assessment; laparoscopy with chromopertubation is gold standard diagnosis.
- Endometriosis and pelvic adhesions (post-surgical/infection) are critical peritoneal factors affecting fertility.
- Hydrosalpinx markedly ↓ IVF success rates; pre-IVF salpingectomy is often beneficial.
- IVF frequently bypasses these issues, offering superior outcomes to surgical repair.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

