Intro & Armamentarium - Tiny Titans' Tools
- Microsurgery: Surgery under magnification (loupes/microscope) for fine structures.
- Key uses: Free tissue transfer, replantation, nerve repair, lymphatic reconstruction.
- Magnification:
- Loupes: 2x-8x.
- Operating Microscope: 4x-40x; provides illumination, depth.
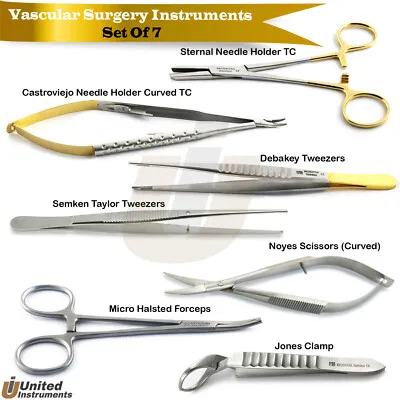
- Core Instruments:
- Needle holders (e.g., Castroviejo).
- Forceps (e.g., Jeweler's, DeBakey micro).
- Scissors (e.g., Vannas).
- Vessel dilators.
- Microvascular clamps (e.g., Acland).
- Contrast background (e.g., blue/green).
- Fine-tip bipolar cautery.
- Microsutures:
- Sizes: 8-0 to 12-0 (typically 9-0, 10-0).
- Material: Nylon (common), Polypropylene.
- Needles: Fine, tapered, 3/8 or 1/2 circle.
- Essentials:
- Irrigation: Heparinized saline/Ringer's lactate.
- Good ergonomics & tremor control.
⭐ For microvascular anastomosis, suture sizes 9-0 and 10-0 are most commonly used.
Vascular Choreography - Stitching Lifelines
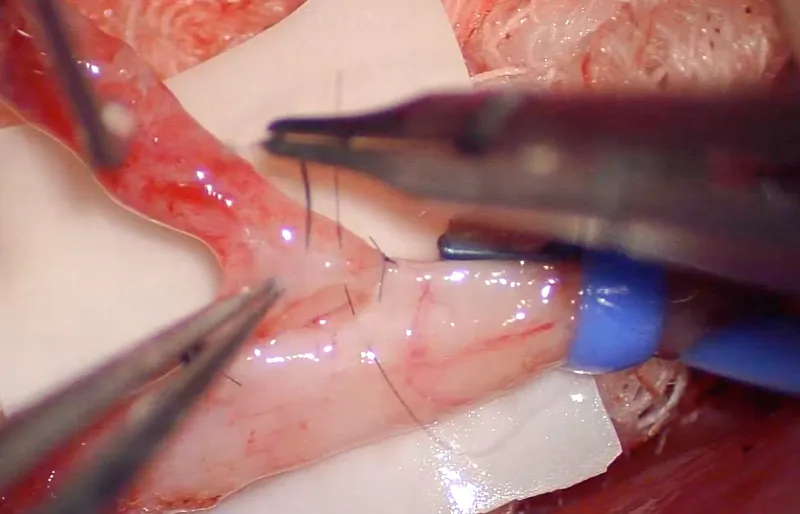
- Vessel Prep: Gentle handling, adventitial stripping (~2mm), heparinized saline irrigation, Acland clamps.
- Anastomosis Types:
- E-E (End-to-End): Standard, similar diameters.
- E-S (End-to-Side): Size mismatch, bypass, flow-through.
- Suturing (Interrupted):
- Suture: 8-0 to 12-0 Nylon. Needle: Tapered, 50-150µm.
- Stay Sutures: 2-3 (bi-/triangulation).
- Bites: Full thickness, equidistant, evert intima.
- Knots: 6-10 per 1mm vessel; 2-1-1 or 3-1-1 throws.
- Patency Check: Acland "milking" test, Doppler ("whoosh").
- Avoid: Tension, torsion, kinking, backwalling, intimal trauma.
⭐ The "Acland" or "empty-and-refill" test (milking test) is a simple, reliable intraoperative method to confirm microvascular anastomosis patency by observing blood flow dynamics.
Neural Networks & Tissue Travels - Wiring & Wrapping
- Nerve Repair (Neurorrhaphy): Aim for tension-free coaptation.
- Types: Epineurial (common), Perineurial (fascicular), Group fascicular.
- Suture: 8-0 to 11-0 monofilament.
- Nerve Grafts: For gaps > 2-3 cm. Donors: Sural, medial antebrachial cutaneous nerve.
- Axonal Regeneration: ~1 mm/day. 📌 "A Millimeter A Day"
- Nerve Conduits: Short gaps (< 3 cm); e.g., vein, collagen.
- Free Tissue Transfer (Free Flaps):
- Vascularized tissue (skin, muscle, bone) transferred & re-anastomosed.
- Indications: Large/complex defects, avascular beds.
- Monitoring: Clinical (color, temp, CRT), Doppler.
⭐ The radial forearm free flap is a workhorse for intraoral reconstruction due to its thin, pliable skin paddle and reliable vascular pedicle.
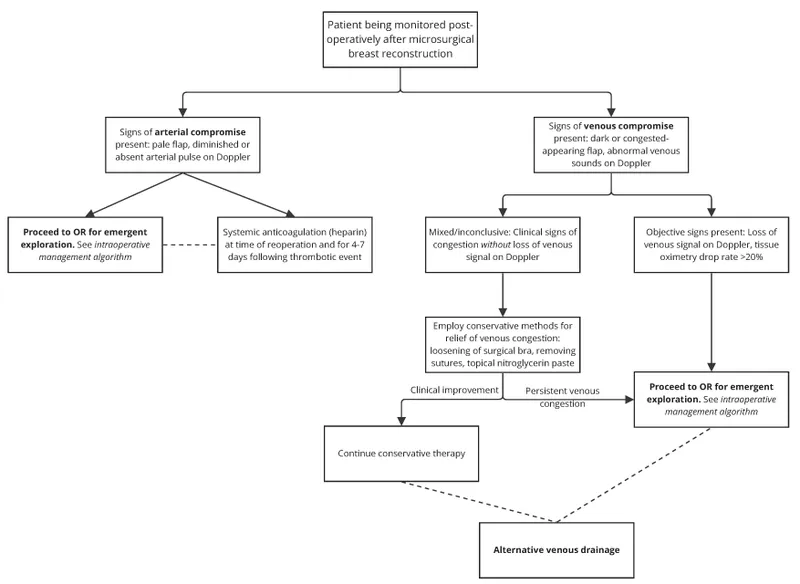
Flap Vigilance - Watching & Woes
- Clinical Monitoring (📌 5 C's):
- Color: Pink (normal); Pale (arterial↓); Dusky/Blue (venous↑)
- Capillary Refill: 1-2s; ↓/absent (arterial); brisk then absent (venous)
- Cold/Warmth: Cool (arterial↓); Warm then cool (venous↑)
- Consistency: Normal turgor; Doughy (venous↑)
- Cut (Pinprick): Bright red; No blood (arterial↓); Dark (venous↑)
- Adjuncts: Doppler (handheld/implantable), Tissue pO₂ (>30 mmHg), temperature probes.
- ⚠️ Compromise:
- Arterial: Pale, cool, no bleed.
- Venous: Swollen, dusky, dark bleed.
- Urgent re-exploration: <4-6 hours.
⭐ Venous thrombosis: most common cause of early free flap failure.
- Woes: Hematoma, seroma, thrombosis (A/V), kinking, infection, partial/total loss.
High‑Yield Points - ⚡ Biggest Takeaways
- Microsurgery utilizes magnification (loupes/microscope) for structures typically < 2-3 mm.
- Vessel anastomosis (end-to-end, end-to-side) is fundamental for free tissue transfer.
- The "no-touch" technique minimizes intimal trauma, preventing thrombosis.
- Suture materials are typically 8-0 to 11-0 monofilament nylon.
- Warm ischemia time is critical; prolonged duration risks flap necrosis.
- Key applications: free flaps, replantation (digits, limbs), nerve repair, lymphatic surgery.
- Common complications: vasospasm, thrombosis (arterial/venous), flap failure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

