Whipple Procedure: Basics - The Big Chop
- Also known as: Pancreaticoduodenectomy.
- A major surgical resection involving removal of:
- Pancreatic head
- Duodenum
- Gallbladder
- Distal common bile duct (CBD)
- Proximal jejunum (segment)
- +/- Gastric antrum (Classic vs. Pylorus-Preserving Whipple)
- Regional lymph nodes.
- Primary Indications: Resectable periampullary (ampullary, distal CBD, duodenal) and pancreatic head malignancies.
⭐ Most common indication is adenocarcinoma of the head of the pancreas.
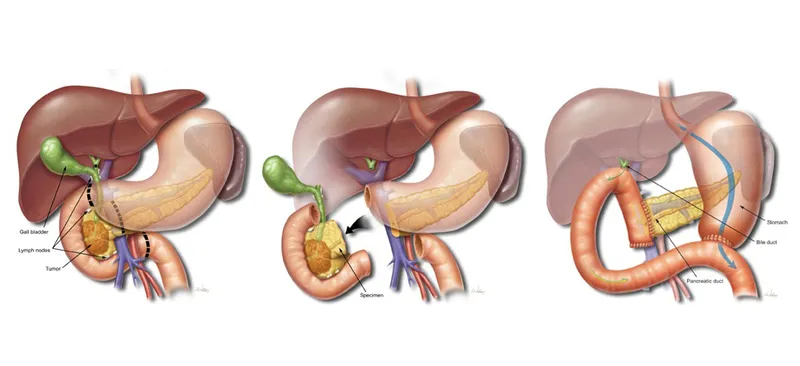
Whipple: Anatomy Resected - What's Out?
Classic Whipple (pancreaticoduodenectomy) resects:
- Pancreatic Head
- Duodenum (entire C-loop)
- Gallbladder
- Common Bile Duct (distal segment)
- Antrum of Stomach (distal stomach)
- Pylorus-Preserving Whipple (PPW) spares pylorus & antrum.
- Jejunum (proximal segment, ~15 cm)
- Regional Lymph Nodes
📌 Mnemonic: "Please Deliver Grapes, Chocolates, And Juice" (Pancreatic head, Duodenum, Gallbladder, CBD, Antrum, Jejunum)

⭐ Pylorus-preserving pancreaticoduodenectomy (PPPD) is often preferred to reduce post-operative dumping syndrome and improve nutritional outcomes by preserving gastric reservoir function.
Whipple: Reconstruction - Plumbing Job
Re-establishing GI continuity post-resection. Three key anastomoses, sequenced to minimize complications.
- Pancreaticojejunostomy (PJ): Pancreatic remnant to jejunum. Most critical; highest leak rate (POPF). Done first to divert pancreatic enzymes.
- Techniques: Duct-to-mucosa (Blumgart), invagination (Cattell-Warren).
- Hepaticojejunostomy (HJ): Common hepatic duct to jejunum. Ensures bile flow into GI tract.
- Gastrojejunostomy (GJ) / Duodenojejunostomy (DJ): Stomach/duodenal stump to jejunum. Restores food passage. Pylorus-preserving (PPPD) uses DJ.
⭐ Pancreatic fistula (POPF) is the most dreaded complication post-Whipple, classified by ISGPS.
Whipple: Complications - Trouble Spots
- Pancreatic Fistula (POPF): Most common & serious.
- Grades A, B, C (ISGPF classification).
- Risk factors: soft pancreas, small duct.
- Delayed Gastric Emptying (DGE): Common, often self-limiting.
- Grades A, B, C (ISGPS classification).
- Hemorrhage:
- Early (<24h): Technical error.
- Late (>24h): Sentinel bleed, pseudoaneurysm (often post-POPF).
- Wound Infection & Dehiscence.
- Intra-abdominal Abscess.
- Bile Leak/Cholangitis.
- Chyle Leak: Rare, due to lymphatic disruption.
- Marginal Ulceration: At gastro/duodenojejunostomy.
⭐ Pancreatic fistula is the most common and feared complication following a Whipple procedure, significantly impacting morbidity and mortality.
Whipple: Peri-op Care - Smooth Sailing
- Pre-op: Optimize nutrition (albumin >3 g/dL). Biliary drainage if bilirubin >15 mg/dL (controversial). Smoking cessation. VTE & antibiotic prophylaxis.
- Intra-op: Goal-directed fluid therapy. Normothermia. Glycemic control.
- Post-op: ICU care. Early mobilization & enteral feeds. Pain control (epidural/PCA). Monitor drain amylase.
- Watch for: DGE, POPF, bleeding.
⭐ Post-Operative Pancreatic Fistula (POPF) is the most feared complication, significantly impacting morbidity and mortality.
High‑Yield Points - ⚡ Biggest Takeaways
- Whipple procedure (pancreaticoduodenectomy): For resectable periampullary cancers.
- Resections: Pancreatic head, duodenum, gallbladder, distal CBD, proximal jejunum.
- PPPD (Pylorus-Preserving): Spares stomach & pylorus; may improve nutrition.
- Most common complication: Delayed Gastric Emptying (DGE).
- Most serious complication: Pancreatic fistula (POPF).
- Reconstruction: Pancreaticojejunostomy, hepaticojejunostomy, gastro/duodenojejunostomy.
- Key contraindication: Vascular encasement (SMA/SMV) or metastases.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

