OSA & Surgery - The Groundwork
- Obstructive Sleep Apnea (OSA): Recurrent upper airway collapse during sleep, causing hypoxemia & fragmented sleep.
- Surgical Candidacy Criteria:
- CPAP failure or intolerance (most common).
- Identifiable anatomical obstruction (e.g., tonsillar hypertrophy, retrognathia).
- Patient preference after full counseling.
- Moderate-Severe OSA (AHI ≥ 15) or Mild OSA (AHI 5-14) with significant symptoms/comorbidities (e.g., hypertension).
- Essential Pre-operative Evaluation:
- Polysomnography (PSG): Confirms OSA diagnosis & severity (Apnea-Hypopnea Index - AHI).
- Drug-Induced Sleep Endoscopy (DISE): Dynamically visualizes site(s) & pattern of airway collapse.
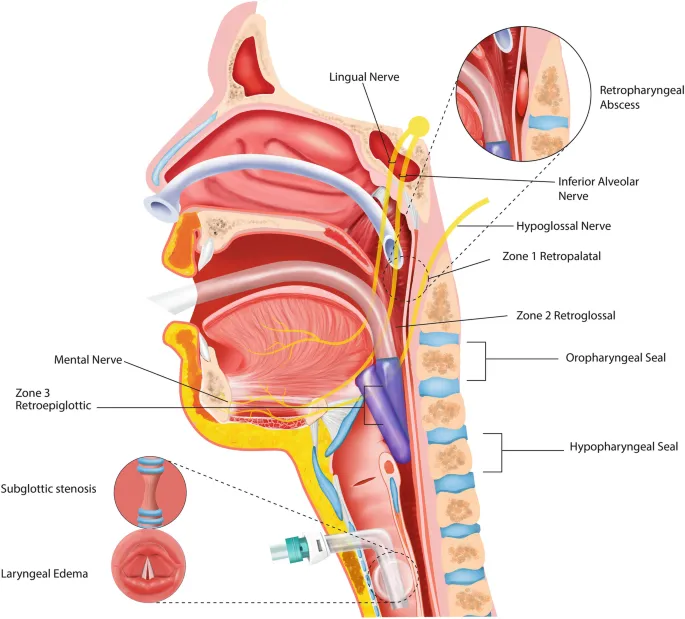
⭐ DISE is crucial for selecting appropriate surgical procedures by identifying specific levels of obstruction: velum, oropharyngeal lateral walls, tongue base, or epiglottis (VOTE classification).
Airway Opening Acts - Nose & Soft Palate
- Nasal Surgery: Aims to ↓ nasal airflow resistance & improve CPAP tolerance/efficacy.
- Septoplasty: Corrects deviated nasal septum.
- Turbinate Reduction: For hypertrophied turbinates (e.g., radiofrequency, microdebrider, partial resection).
- Nasal Valve Repair: Addresses internal/external valve collapse.
- Polypectomy: For nasal polyps.
- Often adjunctive, rarely curative alone for OSA.
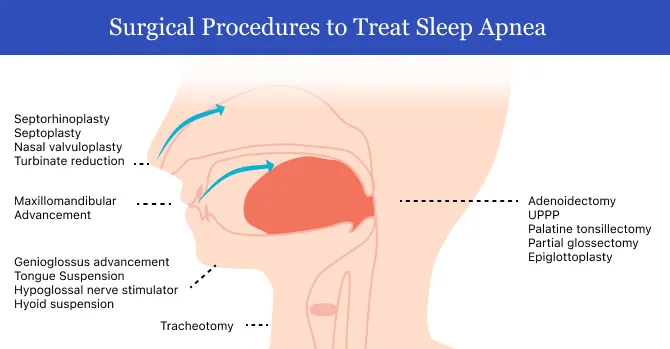
- Soft Palate Surgery: Addresses retropalatal collapse/obstruction.
- Traditional Uvulopalatopharyngoplasty (UPPP):
- Resects uvula, posterior soft palate margin, tonsils (if present).
- Success: AHI ↓ >50% in ~40-60% selected patients.
- Risks: Velopharyngeal insufficiency (VPI), dysphagia, globus sensation, nasopharyngeal stenosis.
- Laser-Assisted Uvulopalatoplasty (LAUP): Staged, office procedure; generally less effective.
- Radiofrequency Ablation (RFA) of Palate: Tissue volume reduction & stiffening.
- Palatal Implants (Pillar®): Polyester rods stiffen soft palate.
- Modern Pharyngoplasties: (e.g., Expansion Sphincter Pharyngoplasty, Z-Palatoplasty, Barbed Reposition Pharyngoplasty) aim for more physiologic airway expansion.
- Traditional Uvulopalatopharyngoplasty (UPPP):
⭐ UPPP success hinges on careful patient selection, particularly identifying retropalatal obstruction without significant tongue base collapse if UPPP is the sole procedure.
Tongue Tied No More - Base & Bones
Targets hypopharyngeal obstruction via tongue base reduction or skeletal framework expansion.
- Tongue Base Procedures:
- Midline Glossectomy/Lingualplasty: Reduces posterior tongue volume.
- Lingual Tonsillectomy: For lingual tonsil hypertrophy.
- Radiofrequency Ablation (RFABT): Shrinks tongue base tissue.
- Genioglossus Advancement (GGA): Advances tongue base by moving genial tubercle.
- Hyoid Suspension (HS): Elevates and stabilizes hyoid bone, indirectly pulling tongue base anteriorly.

- Skeletal Procedures:
- Maxillomandibular Advancement (MMA): Highly effective; enlarges entire upper airway. Success >90%.
⭐ MMA is the most effective surgical option for OSA, expanding the velo-oro-hypopharyngeal airway by advancing both jaws.
- Genioplasty: Anterior chin movement; may improve airway.
- Maxillomandibular Advancement (MMA): Highly effective; enlarges entire upper airway. Success >90%.
Beyond the Knife - Nerves & New Tech
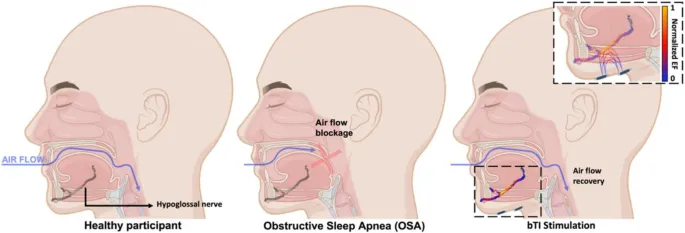
- Hypoglossal Nerve Stimulation (HGNS):
- Mechanism: XII N. stimulation → genioglossus contracts → ↑airway patency.
- Indications: Mod-Sev OSA, CPAP failure/intolerance, BMI < 32-35 kg/m².
- Contraindication: Complete concentric collapse (CCC) at velopharynx on DISE.
- Tracheostomy:
- Definitive; bypasses entire upper airway obstruction.
- Indications: Severe OSA, failed therapies, craniofacial anomalies.
- Risks: Stenosis, infection, bleeding, fistula.
- General Post-Op Care & Risks:
- Airway monitoring, pain relief.
- Complications: Bleeding, infection, nerve injury.
- Follow-up PSG; CPAP may still be required.
⭐ HGNS is contraindicated by complete concentric collapse (CCC) of the velopharynx on drug-induced sleep endoscopy (DISE).
High‑Yield Points - ⚡ Biggest Takeaways
- Uvulopalatopharyngoplasty (UPPP) is a common surgery for palatal obstruction in OSA; success rates vary.
- Genioglossus advancement (GA) specifically targets tongue base collapse by pulling the tongue forward.
- Maxillomandibular advancement (MMA) is highly effective for severe OSA, significantly enlarging the entire velo-oro-hypopharyngeal airway.
- Tracheostomy remains the definitive treatment for life-threatening or refractory severe OSA, bypassing all upper airway obstruction.
- Drug-Induced Sleep Endoscopy (DISE) is crucial for identifying the precise level(s) and pattern of airway obstruction to guide surgical selection.
- Hypoglossal nerve stimulation (HNS) is a newer, implant-based therapy for moderate to severe OSA, improving upper airway muscle tone during sleep.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

