COPD Overview - Breathless Beginnings
- Chronic, progressive disease with persistent airflow obstruction; largely irreversible. Diagnosis: post-bronchodilator FEV1/FVC < 0.7.
- Key Phenotypes:
- Chronic Bronchitis (Clinical): Productive cough ≥ 3 months/yr for ≥ 2 consecutive yrs. "Blue bloaters".
- Emphysema (Pathological): Alveolar wall destruction; permanent distal airspace enlargement. "Pink puffers".
- Risk Factors: Smoking (dominant), air pollution, occupational exposure, α1-antitrypsin deficiency (AATD).
⭐ Reid Index (mucous gland to bronchial wall thickness ratio) > 0.4 characterizes chronic bronchitis.
CXR Findings - COPD's Shadow Play
CXR reveals key signs, especially in emphysema-dominant COPD:
- Hyperinflation Signs:
- Flattened hemidiaphragms (most reliable).
- Increased retrosternal space (> 2.5 cm, lateral CXR).
- Widened intercostal spaces.
- Long, narrow, vertical heart.
- Parenchymal Changes (Emphysema):
- Hyperlucency of lung fields.
- Paucity of peripheral vascular markings (oligemia).
- Bullae/blebs (lucent areas > 1 cm, thin walls).
- Chronic Bronchitis ("Dirty Lungs"):
- CXR often normal or non-specific.
- Increased bronchovascular markings (tram-tracks).
- Thickened bronchial walls.
- Cardiomegaly (cor pulmonale in advanced disease).
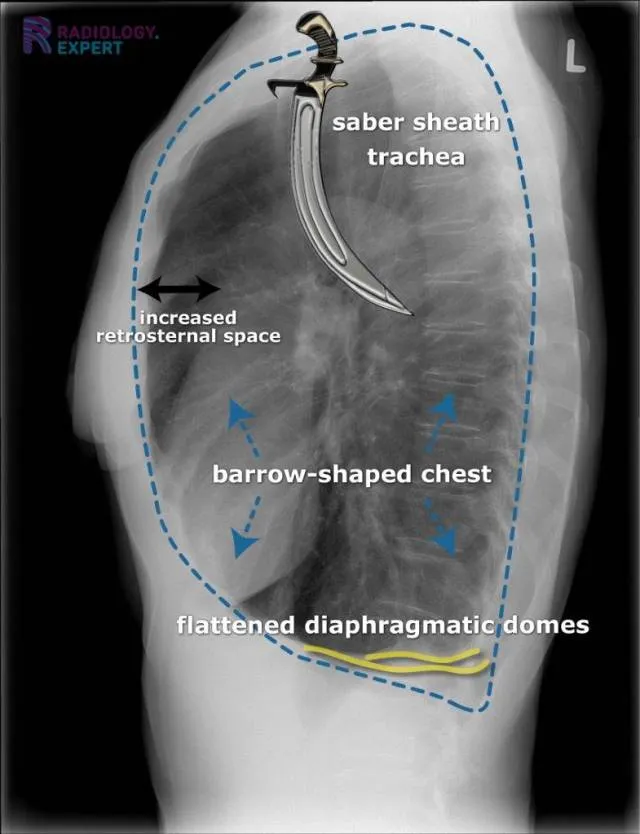
⭐ Saber-sheath trachea (coronal narrowing, sagittal widening of intrathoracic trachea) is a specific, though insensitive, sign of COPD.
HRCT Imaging - COPD's Sharp Focus
HRCT: Key for detailed COPD lung assessment, identifying emphysema and airway changes.
Emphysema Subtypes:
| Subtype | Key HRCT Features | Location | Association |
|---|---|---|---|
| Centrilobular | Centrilobular lucencies (± central dot), uneven | Upper Lobes | Smoking |
| Panlobular | Diffuse lucencies, ↓vascularity, uniform destruction | Lower Lobes | AATD |
| Paraseptal | Subpleural lucencies, bullae/blebs, along septa | Periphery | Spont. Pneumothorax |
Airways Disease:
- Bronchial Wall Thickening (BWT):
- Normal: < 1.5 mm or BWT/diameter ratio < 0.25.
- COPD: ↑ BWT (> 2 mm), bronchial dilatation.
- Air Trapping (Expiratory HRCT):
- ↓Attenuation areas (lucent) not increasing density on expiration.
- Mosaic pattern.
- Other: Mucous plugging.
Associated Findings:
- Saber-sheath trachea.
- Pulmonary HTN signs (MPA diameter > 29 mm or MPA/Aorta ratio > 1).
⭐ Centrilobular emphysema: most common in smokers, shows upper lobe predominant lucencies on HRCT.
COPD Complications - When Lungs Cry Foul
- Pulmonary Hypertension (PHT):
- Signs: Main pulmonary artery (MPA) diameter > 29mm (CT), RV hypertrophy, peripheral pruning.
- Acute Exacerbations (AECOPD):
- Imaging: ↑ Bronchial wall thickening, new/worsening consolidation, ↑ air trapping.
- Spontaneous Pneumothorax:
- Cause: Ruptured bullae/blebs.
- Sign: Visceral pleural line, absent lung markings peripherally.
- Cor Pulmonale:
- Sequela: RV enlargement & dysfunction due to PHT.
- Lung Cancer:
- ↑ Risk, especially in emphysematous areas.

- ↑ Risk, especially in emphysematous areas.
⭐ Pulmonary artery to aorta (PA:A) ratio > 1 on CT is a common indicator of pulmonary hypertension in COPD patients, often seen alongside MPA diameter > 29mm.
High‑Yield Points - ⚡ Biggest Takeaways
- COPD is defined by persistent, irreversible airflow limitation, predominantly caused by cigarette smoking.
- Chest X-ray findings include hyperinflation, flattened hemidiaphragms, and an increased retrosternal space.
- HRCT is superior for detecting emphysema (centrilobular, panlobular, paraseptal) and bronchial wall thickening.
- Common complications are pulmonary hypertension and cor pulmonale.
- Alpha-1 antitrypsin deficiency is linked to early-onset panlobular emphysema, typically in lower lung zones.
- Presence of bullae, blebs, and saber-sheath trachea are notable signs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

