Cardiomyopathies: Intro & Types - Heart's Structural Woes
Myocardial diseases with structural/functional abnormalities, not explained by CAD, HTN, valvular, or congenital heart disease (WHO/ESC criteria).
- Primary: Predominantly confined to heart muscle.
- Secondary: Myocardial involvement as part of systemic disease.
Main Morpho-functional Types:
- Dilated Cardiomyopathy (DCM): LV/RV dilation & systolic dysfunction.
- Hypertrophic Cardiomyopathy (HCM): Unexplained LV hypertrophy.
- Restrictive Cardiomyopathy (RCM): Impaired ventricular filling, diastolic dysfunction.
- Arrhythmogenic Right Ventricular Dysplasia/Cardiomyopathy (ARVD/C): Fibrofatty replacement of RV myocardium.
- Unclassified: e.g., Takotsubo cardiomyopathy, Left Ventricular Non-compaction (LVNC).

⭐ Cardiomyopathies are diseases of the myocardium associated with cardiac dysfunction, leading to impaired heart performance and often heart failure or arrhythmias.
Dilated Cardiomyopathy: Big Baggy Chambers
- Pathophysiology: Systolic dysfunction with impaired contractility, ↓ ejection fraction (EF).
- Etiology: Primarily idiopathic; also alcohol, viral (Coxsackie B), genetic, peripartum.
- 📌 Mnemonic (ABCCCD): Alcohol, Beri-beri, Coxsackie B, Cocaine, Chagas, Doxorubicin.
- Key Findings:
-
CXR: Cardiomegaly (classic 'water bottle' sign), pulmonary venous hypertension, pleural effusion.
-
Echocardiography: Hallmark: LV dilation, global hypokinesia, ↓EF < 45%; often functional MR/TR.
-
Cardiac MRI: Assesses LV dilation & dysfunction; LGE (mid-myocardial linear or absent) helps differentiate etiology.
-
⭐ Dilated cardiomyopathy is the most common type of cardiomyopathy and a leading indication for heart transplantation.
Hypertrophic Cardiomyopathy: Thickened Heart Walls
- Etiology: Autosomal dominant genetic disorder (sarcomeric protein mutations, e.g., MYH7, MYBPC3).
- Pathophysiology:
- Diastolic dysfunction (impaired LV relaxation/filling).
- Dynamic LV Outflow Tract Obstruction (LVOTO) due to:
- Asymmetric Septal Hypertrophy (ASH): Septum > free wall.
- Systolic Anterior Motion (SAM) of mitral valve.
- Imaging:
- CXR: Often normal; may show LA enlargement, LVH signs.
- Echocardiography: LVH ≥15mm (in absence of other cause); ≥13mm in relatives. Shows ASH, SAM, LVOTO gradient, diastolic dysfunction.
- Cardiac MRI: Gold standard for morphology, hypertrophy distribution, fibrosis (Late Gadolinium Enhancement - LGE at RV insertion points), crypts.
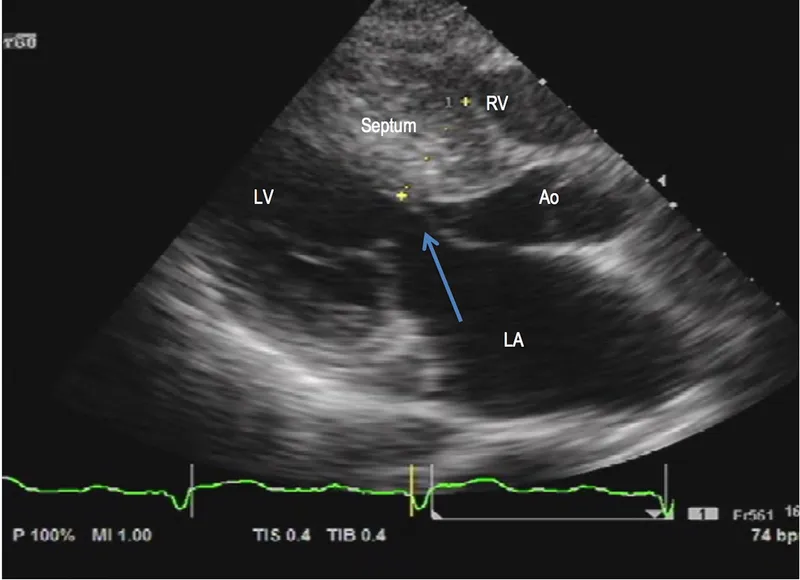
⭐ Hypertrophic cardiomyopathy is the most common genetic cardiovascular disease and a leading cause of sudden cardiac death in young athletes.
Restrictive & ARVC: Stiff Walls & Fatty Scars
- Restrictive Cardiomyopathy (RCM): Stiff Ventricles
- Causes: 📌 ASHES To ASHES (Amyloid, Sarcoid, Hemochromatosis, Endomyocardial fibrosis, Scleroderma), idiopathic.
- Patho: Stiff ventricles, impaired diastolic filling, preserved EF (early).
- Echo: Biatrial enlargement, normal/small LV, thick walls (infiltrative), diastolic dysfunction; 'sparkling' (amyloid).

- MRI: LGE (amyloid: diffuse subendocardial/transmural; sarcoid: patchy).
- Arrhythmogenic RV Cardiomyopathy/Dysplasia (ARVC/D): Fatty Scars
- Cause: Genetic (desmosomal proteins).
- Patho: RV fibrofatty replacement.
- MRI (key): RV dilation, akinesia/dyskinesia, wall thinning, fatty infiltration, RV LGE.

⭐ ARVC/D classically involves the 'triangle of dysplasia' in the right ventricle (RV inflow, RV outflow, and RV apex).
High‑Yield Points - ⚡ Biggest Takeaways
- HCM: Asymmetric septal hypertrophy (ASH), LVOTO, SAM. Apical HCM: "ace-of-spades".
- DCM: Global LV dilatation, systolic dysfunction, ↓EF.
- RCM: Impaired diastolic filling, biatrial enlargement. Amyloidosis: diffuse LGE.
- ARVD/C: Fibrofatty replacement of RV, RV dilatation/aneurysms.
- LVNC: Prominent trabeculations, NC/C ratio >2.3:1.
- Takotsubo: Apical ballooning, transient dysfunction, normal coronaries.
- Cardiac MRI LGE: Differentiates types (e.g., mid-myocardial in HCM, diffuse in amyloid).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

