Male Breast A&P - Not Just Gals!
- Rudimentary Structure: Skin, nipple-areola, subcutaneous fat, basic ductal system within stroma.
- Ductal System:
- Few, small, branching ducts converging at nipple.
- Lined by inner epithelial & outer myoepithelial cells.
- Lobules: Generally absent/rudimentary; no acini due to low estrogen/progesterone.
- Stroma: Mainly fibrous connective tissue, some adipose.
- Hormonal Balance: Testosterone inhibits; estrogen (even low levels) can stimulate ducts.

⭐ Male breast lacks significant lobular development, primarily consisting of ducts and stroma. This is key for pathology.
Benign Male Lumps - Mostly Harmless
⭐ Gynecomastia is the most common benign condition of the male breast.
- Gynecomastia: Proliferation of glandular & stromal elements.
- Causes: Hormonal imbalance (↑estrogen/androgen ratio), drugs (📌 Spironolactone, Cimetidine, Alcohol, Digoxin - SCAD), systemic diseases (liver, renal, hyperthyroidism), idiopathic.
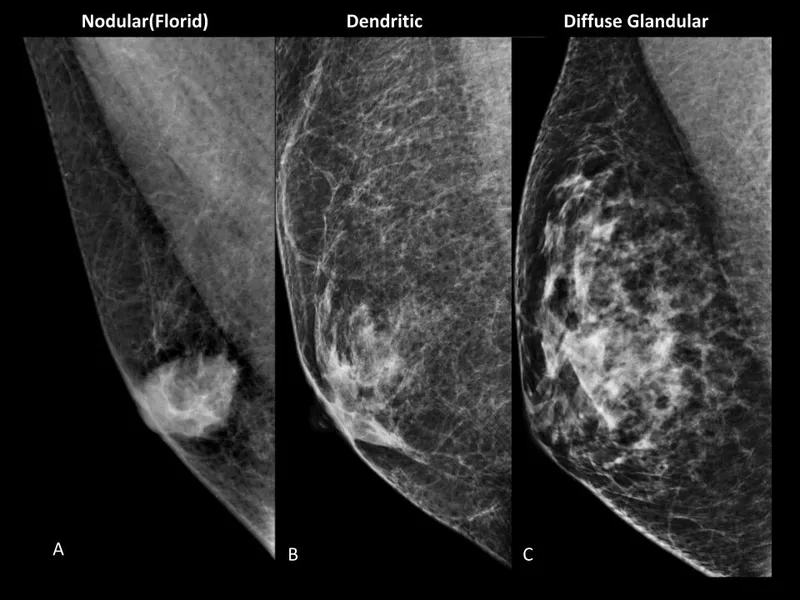
- Patterns:
Pattern MG Features US Features Chronicity Nodular Flame-shaped/nodular retroareolar Hypoechoic retroareolar nodule <1 yr Dendritic Finger-like projections Heterogeneous, prominent ducts Variable Diffuse Glandular Female-like, heterogeneous density Diffuse glandular proliferation >1 yr
- Pseudogynecomastia: Fat deposition, no glandular tissue. MG: Radiolucent. US: ↑Subcutaneous fat.
- Other Benign: Lipoma (radiolucent, encapsulated fat), sebaceous cyst (well-defined, superficial, dermal), hematoma (post-trauma), abscess (inflammatory signs).
Male Breast Cancer - Rare But Real
- Accounts for < 1% of all breast cancers; incidence is ↑.
- Presents later than in females (mean age: 60-70 years).
Risk Factors:
| Category | Risk Factors |
|---|---|
| Genetic | BRCA2 (strongest), BRCA1, CHEK2, PALB2 |
| Hormonal | ↑ Estrogen, ↓ Androgen, Klinefelter (XXY) |
| Family History | Positive family Hx of breast/ovarian cancer |
| Other | Age, obesity, testicular conditions, radiation |
Clinical Presentation:
- Painless, firm, subareolar lump (often eccentric).
- Nipple changes: retraction, discharge (bloody), ulceration.
- Axillary lymphadenopathy.
Imaging:
- Mammography: Eccentric, retroareolar, spiculated mass. Calcifications less common than in females.
- Ultrasound: Hypoechoic, irregular, spiculated mass; posterior acoustic shadowing. Doppler shows vascularity.

Histology:
⭐ Invasive Ductal Carcinoma (IDC), No Special Type, is the most common histological type (> 85%), similar to females. Ductal Carcinoma In Situ (DCIS) is also seen.
- Lobular carcinoma is rare (due to rudimentary lobules in males).
Imaging Male Breasts - Spotting Trouble

-
Key Modalities: Mammography (MMG) & Ultrasound (USG).
- MMG: Standard CC & MLO views. Adjust for male anatomy (smaller paddle, ensure pectoralis visualization).
- USG: Differentiates cystic/solid; characterizes masses; guides biopsy.
-
Benign vs. Malignant Features:
Feature Benign (e.g., Gynecomastia) Malignant (e.g., Invasive Ductal Carcinoma) MMG Mass Diffuse, flame-shaped, nodular Irregular, spiculated mass Margins Circumscribed, indistinct Spiculated, ill-defined Calcifications Coarse, benign-appearing Pleomorphic, fine linear microcalcifications USG Mass Oval, wider-than-tall, circumscribed Irregular, taller-than-wide, spiculated Echotexture Variable, often hypoechoic (glandular) Marked hypoechogenicity, heterogeneous Location Typically subareolar Often subareolar, may be eccentric
⭐ Most male breast cancers occur in the subareolar region due to the concentration of ductal tissue there.
- BI-RADS Assessment & Management Flowchart:
High‑Yield Points - ⚡ Biggest Takeaways
- Gynecomastia, most common, is typically bilateral, retroareolar; US differentiates it from cancer.
- Male breast cancer: rare (<1%), usually Invasive Ductal Carcinoma (IDC), often presents late.
- Risk factors: BRCA2 mutations, Klinefelter's, family history, obesity, advanced age, liver disease.
- Mammography (CC & MLO views) & Ultrasound are key for diagnosis and characterization.
- Cancer signs: eccentric, spiculated mass, suspicious microcalcifications, skin/nipple retraction, axillary nodes.
- Biopsy for BI-RADS 4/5 lesions; typical gynecomastia is BI-RADS 2 (benign).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

