Psychiatric Interview - The Mind Meld Kickoff
- Purpose & Goals:
- Diagnosis: Identifying the disorder.
- Formulation: Understanding contributing factors.
- Treatment Plan: Guiding interventions.
- Rapport: Building a therapeutic alliance.
- Ethical Pillars:
- Informed Consent: Patient autonomy.
- Confidentiality: Protecting patient information.
⭐ Tarasoff duty: Clinician's duty to warn potential victims if a patient poses a serious threat.
- Building Rapport:
- Empathy: Understanding patient's perspective.
- Active Listening: Attentive engagement.
- Non-judgmental Stance: Unconditional positive regard.
- Optimal Setting:
- Privacy: Ensuring confidentiality.
- Safety: For both patient and clinician.
- Comfort: Facilitating open communication.
Psychiatric History - The Past Unpacked
- Identifying Data & Chief Complaint: Key demographics; patient's primary concern verbatim.
- History of Present Illness (HPI): Detail onset (acute/insidious), duration, course (episodic/continuous), severity, precipitants, and impact on functioning. Note associated mood, thought, perception, or behavioral changes.
- Past Psychiatric History: Previous episodes (nature, duration, outcome), treatments received (type, dose, duration, response, side effects, compliance), hospitalizations (voluntary/involuntary), history of suicide attempts or self-harm.
- Family History: Inquire about psychiatric illnesses, substance use, and suicides among first-degree relatives.
- Consider Genogram structure.
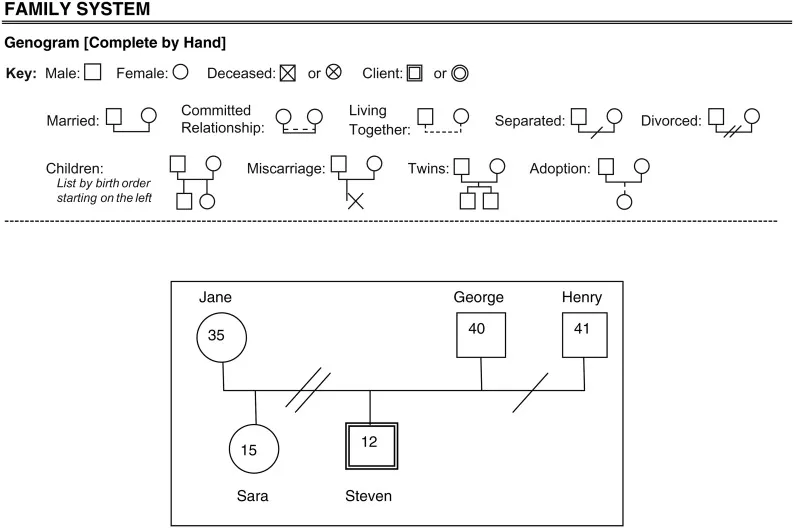
- Consider Genogram structure.
- Personal History:
- Developmental milestones, childhood, education, occupation, relationship history, psychosexual history.
- For adolescents: HEADSSS 📌 (Home, Education/Employment, Activities, Drugs, Sexuality, Suicide/Safety).
- Substance Use History: Type, amount, frequency, duration, pattern of use, last use, features of dependence/withdrawal for alcohol, nicotine, cannabis, opioids, stimulants, etc.
- CAGE questionnaire 📌 for alcohol: Cut down, Annoyed, Guilty, Eye-opener. Score > 2 is significant.
- Past Medical & Surgical History: Significant illnesses, surgeries, head injuries. Current medications & allergies.
⭐ Collateral history from reliable informants (family, friends) is invaluable, especially in cases of psychosis, severe depression, mania, or cognitive impairment, to obtain an objective and comprehensive account.
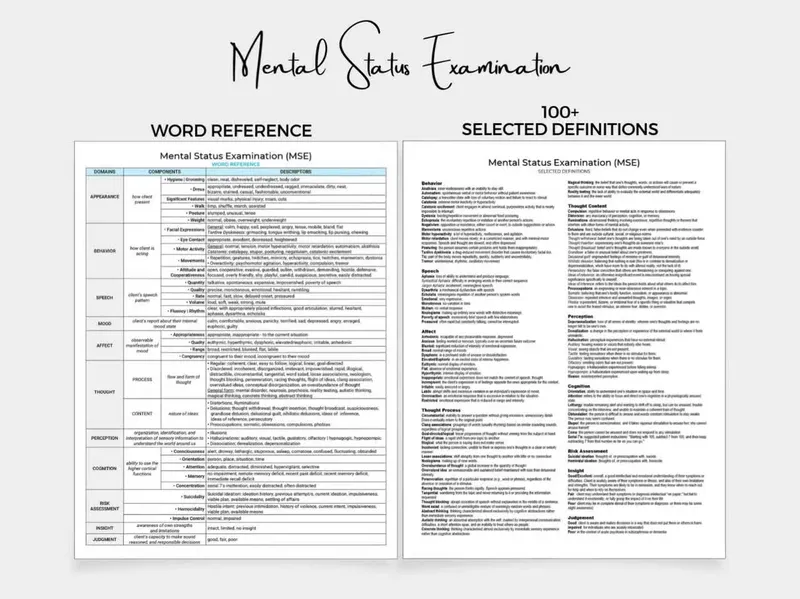
Mental Status Exam - The MSE Snapshot
Systematic evaluation of a patient's current mental state. 📌 Mnemonic: ASEPTIC (+J)
- Appearance & Behavior: Hygiene, grooming, eye contact, posture, psychomotor activity (agitation/retardation), rapport.
- Speech: Rate (e.g., pressured, slow), rhythm, volume, tone, articulation, quantity.
- Emotion:
Feature Mood Affect Nature Subjective (patient's words) Objective (observed expression) Descriptors e.g., "sad", "elated", "anxious" Range (flat, blunted), appropriateness, intensity, lability - Perception: Hallucinations (auditory, visual, tactile, olfactory, gustatory), illusions, depersonalization, derealization.
- Thought:
- Process (Form): Coherence, flight of ideas, tangentiality, circumstantiality, thought block.
- Content: Delusions, obsessions, phobias, suicidal/homicidal ideations.
- Insight: Awareness of illness (Grades 1-6).
- Cognition: Orientation (TPP), attention (serial 7s), memory (immediate, recent, remote), abstract thought. MMSE score < 24 suggests impairment.
- Judgment: Social and test judgment.
⭐ Auditory hallucinations are most common in schizophrenia; visual hallucinations are more common in organic mental disorders.
Risk & Formulation - The Danger Zone Check
- Risk Assessment:
- Suicide: Assess ideation, plan, intent, means. Use SAD PERSONS scale 📌 (Scores: 0-4 low/med, 5-6 high, ≥7 very high risk).
- Homicide/Violence: Assess ideation, intent, plan, past violence, impulsivity.
- Physical Exam & Investigations: When indicated (e.g., baseline bloods, TFTs, toxicology, neuroimaging).
- Case Formulation (Biopsychosocial): Integrate 4Ps: Predisposing (vulnerability), Precipitating (triggers), Perpetuating (maintains), Protective (strengths).
- Diagnosis: Provisional & Differential (DSM/ICD criteria).
⭐ Past suicide attempt is the strongest predictor of future suicide.
High‑Yield Points - ⚡ Biggest Takeaways
- Psychiatric history includes HPI, past illnesses, family, personal history (developmental, substance use), and premorbid personality.
- MSE evaluates appearance, behavior, speech, mood, affect, thought, perception, cognition, insight, and judgment.
- Rapport building through empathy and a non-judgmental attitude is vital.
- Key thought assessments: formal thought disorders (e.g., flight of ideas) and delusions/obsessions (content).
- Evaluate patient's insight into illness and their judgment (social/test).
- Risk assessment for suicide and violence is a priority.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

