Oxygen Therapy Basics - Breath of Life
- Definition: Administering oxygen at FiO2 > 21% (room air).
- Primary Goal: Treat or prevent hypoxemia and subsequent tissue hypoxia.
- Core Indications:
- Acute hypoxemia (e.g., pneumonia, ARDS, PE).
- Chronic hypoxemia (e.g., severe COPD, ILD).
- Increased metabolic demand (e.g., sepsis, major trauma).
- Carbon monoxide poisoning.
- Monitoring: Pulse oximetry (SpO2), Arterial Blood Gas (PaO2, SaO2).
⭐ Goal of O2 therapy is to maintain PaO2 > 60 mmHg or SaO2 > 90% in most acute settings.
Delivery Devices - Mask & Cannula Crew
- Low-Flow Devices: Variable FiO2 (patient-dependent).
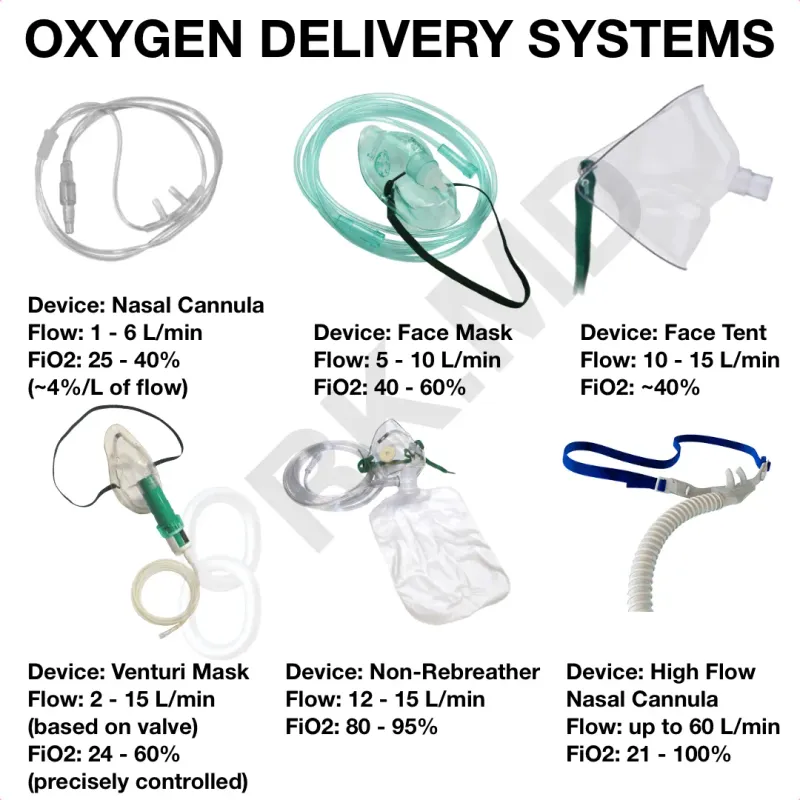
- Nasal Cannula: 1-6 L/min → FiO2 24-44%. Mild hypoxia. 📌 CANnula = CAN eat/talk.
- Simple Face Mask: 5-10 L/min → FiO2 40-60%. Min 5 L/min (↓CO2 rebreath).
- Partial Rebreather Mask: 6-10 L/min → FiO2 60-80%. Reservoir bag, no 1-way valve.
- Non-Rebreather Mask (NRM): 10-15 L/min → FiO2 80-95%. Reservoir bag + 1-way valves. Severe hypoxia.
- High-Flow Devices: Fixed FiO2.
- Venturi Mask: FiO2 24-60% via color-coded adapters (Venturi principle).
⭐ Venturi masks are high-flow devices that deliver a precise and constant FiO2, ideal for COPD patients.
- High-Flow Nasal Cannula (HFNC): Up to 60 L/min; heated, humidified O2; FiO2 21-100%; PEEP.
- Venturi Mask: FiO2 24-60% via color-coded adapters (Venturi principle).
Monitoring & Titration - Watching the Sats
- Goal: Maintain target SpO2; use lowest FiO2.
- Tools:
- Pulse Oximetry (SpO2): Continuous, non-invasive.
⭐ Pulse oximetry is unreliable in CO poisoning, methemoglobinemia, severe anemia; ABG is essential.
- Arterial Blood Gas (ABG): PaO2, PaCO2, pH. Gold standard if SpO2 unreliable or for ventilation assessment.
- Pulse Oximetry (SpO2): Continuous, non-invasive.
- Targets (SpO2):
- General: 94-98%.
- COPD/Hypercapnia risk: 88-92%.
- Process: Titrate FiO2 per SpO2. Wean gradually when stable.
Oxygen's Dark Side - Too Much of a Good Thing
- COPD & CO2 Narcosis:
⭐ In COPD patients with chronic CO2 retention, excessive oxygen can depress the hypoxic ventilatory drive, leading to CO2 narcosis and respiratory acidosis.
- Retinopathy of Prematurity (ROP):
- Premature infants: high, prolonged O2 → retinal vasoconstriction, abnormal vessel growth (neovascularization), potential detachment.
- Pulmonary Oxygen Toxicity:
- Prolonged FiO2 > 0.6 (e.g., > 24-48 hrs).
- Symptoms: substernal pain, cough, dyspnea; can lead to ARDS-like damage.
- Mechanism: ↑ reactive oxygen species.
- Absorption Atelectasis:
- High FiO2 washes out alveolar nitrogen (splinting effect lost) → alveolar collapse, V/Q mismatch_._
Special Uses & Targets - O2 for VIPs
- CO Poisoning: 100% O2 (non-rebreather), consider HBO.
- Cluster Headache: High-flow O2 (10-15 L/min).
- Pneumothorax: High FiO2 to ↑ N2 washout.
- Decompression Sickness: HBO.
- Anaerobic Infections (e.g., gas gangrene): HBO.
- Cyanide Poisoning: Adjunct.
- Acute Mountain Sickness: Primary treatment.
⭐ For carbon monoxide poisoning, administer 100% oxygen via a non-rebreather mask; consider hyperbaric oxygen (HBO) for severe cases.
High‑Yield Points - ⚡ Biggest Takeaways
- Key indication: Hypoxemia (PaO2 < 60 mmHg or SaO2 < 90%).
- Venturi masks offer precise FiO2, vital for COPD (target SaO2 88-92%).
- Non-rebreathing masks deliver highest FiO2 (near 100%) for severe cases.
- Oxygen toxicity can cause retinopathy of prematurity and pulmonary damage.
- In COPD, avoid suppressing hypoxic drive to prevent CO2 narcosis.
- Hyperbaric oxygen (HBOT) treats CO poisoning, decompression sickness, and gas gangrene.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

