Definition & Urgency - Seizure Showdown SOS
- Status Epilepticus (SE): Critical neurological emergency.
- Defined as:
- Continuous seizure >5 minutes.
- OR ≥2 seizures, no full recovery of consciousness between.
- Types: Convulsive (CSE), Non-Convulsive (NCSE).
- Defined as:
- Why Urgent?
- Risk of neuronal injury, systemic complications.
- ↑ Mortality. Act fast! 📌 TIME IS BRAIN!
⭐ The >5 min threshold is for initiating treatment; >30 min defines "established SE" with higher risk of long-term consequences.
Initial & First-Line Rx - Benzo Blitz Begins
(Timeframe: 0-20 min)
- 📌 Benzos: L-M-D (Lorazepam, Midazolam, Diazepam).
- Thiamine first if alcoholism/malnutrition suspected before glucose.
⭐ Exam Favourite: IM Midazolam: key for pre-hospital/no-IV, efficacy like IV Lorazepam for rapid seizure control.
Second-Line Pharmacotherapy - AED Avengers Assemble
If seizures persist 20-40 min after 2 benzodiazepine doses, initiate second-line IV AEDs. 📌 Mnemonic: "Load Very Potent Pharmaceuticals" (Levetiracetam, Valproate, Phenytoin/Fosphenytoin, Phenobarbital). Choice depends on patient factors.
| Drug | Loading Dose | Infusion | AEs/Monitoring |
|---|---|---|---|
| Fosphenytoin | 20 mg PE/kg | Max 150 mg PE/min | Hypotension, arrhythmias (ECG, BP). ↓ Local reactions. |
| Phenytoin | 20 mg/kg | Max 50 mg/min | Hypotension, arrhythmias (ECG, BP), ⚠️ purple glove. |
| Valproic Acid | 20-40 mg/kg | Over 5-10 min | ⚠️ Hepatotoxicity (LFTs), pancreatitis, ↑NH3. |
| Levetiracetam | 60 mg/kg (max 4500mg) | Over 15 min | Somnolence, behavioral. Few interactions. |
| Phenobarbital | 15-20 mg/kg (alt.) | 50-100 mg/min | ⚠️ Sedation, resp. depression, hypotension. |
Refractory SE Rx - Anesthesia Endgame
- Definition: Status Epilepticus (SE) persisting >40-60 minutes despite adequate first and second-line agents.
- Immediate Steps:
- Transfer to Intensive Care Unit (ICU).
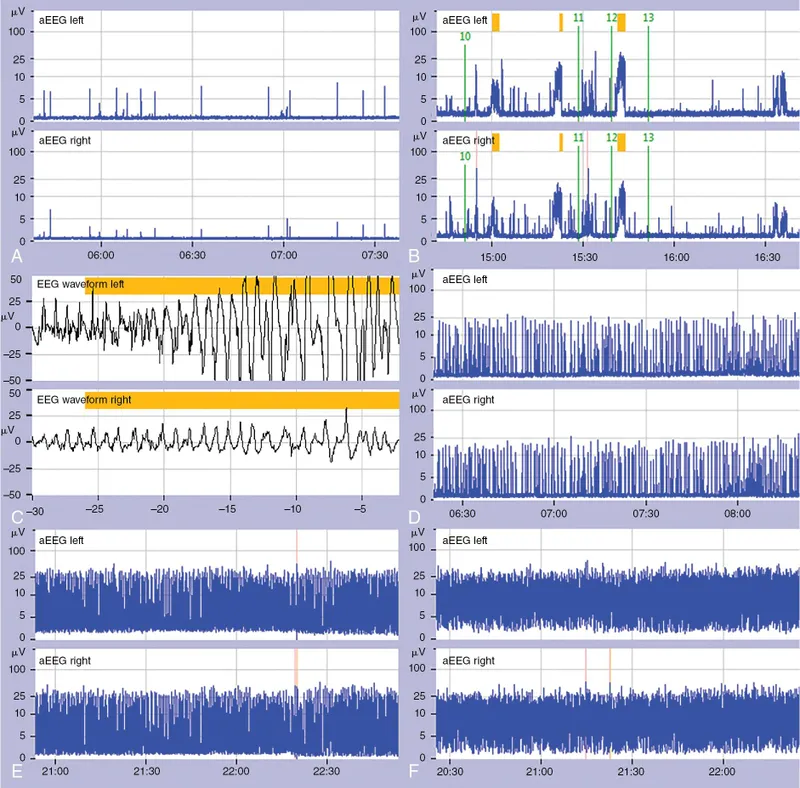
- Continuous EEG (cEEG) monitoring is mandatory for titration and seizure detection.
- Therapeutic Goal: Achieve seizure cessation on cEEG. Burst suppression pattern may be targeted.
- Anesthetic Agent Options (Administer as continuous IV infusions):
- Adjunct: Ketamine can be considered.
⭐ Propofol Infusion Syndrome (PRIS) risk ↑ with doses >4 mg/kg/hr or duration >48 hrs; presents with metabolic acidosis, rhabdomyolysis, arrhythmias, renal failure.
Etiology & Investigations - Cause Clues & Checks
- Crucial: Identify & treat underlying cause!
- Common Causes (📌 think "triggers"): AED withdrawal/non-compliance, stroke, CNS infection, metabolic (e.g., $\downarrow\text{glucose}$, $\downarrow\text{Na}^+$), hypoxia, toxins, alcohol withdrawal, trauma, tumor, autoimmune.
- Key Investigations:
- Labs: Glucose, CMP, CBC, AED levels, Tox screen.
- LP (if infection suspected).
- Neuroimaging: CT (urgent), MRI.
- EEG.
⭐ Always check blood glucose early; hypoglycemia is a readily reversible cause!
High‑Yield Points - ⚡ Biggest Takeaways
- Initial: Secure ABCs, check glucose, gain IV access.
- First-line: IV Lorazepam is drug of choice; IM Midazolam if no IV access.
- Second-line: IV Fosphenytoin (preferred) or Phenytoin if seizures persist.
- Third-line: IV Valproate, Levetiracetam, or Phenobarbital.
- Refractory SE: Consider Midazolam infusion, Propofol, or Pentobarbital coma.
- Time is brain: Escalate therapy every 5-10 minutes if seizures continue.
- Monitor for respiratory depression with benzodiazepines and barbiturates_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

