Intro & Vulnerability - Kiddie Toxin Trackers
- Children are uniquely vulnerable to environmental toxins due to distinct physiological and behavioral differences compared to adults.
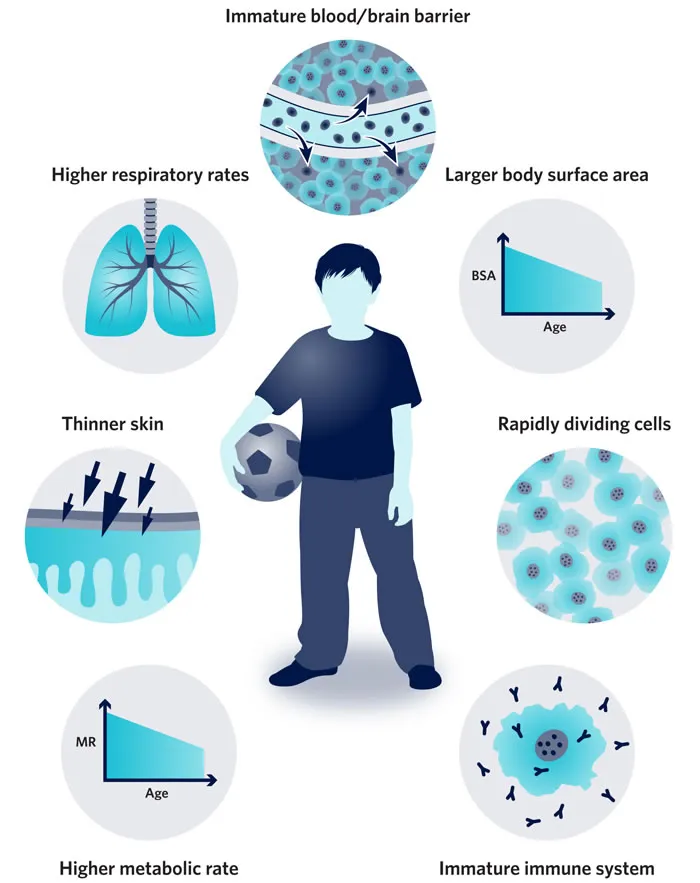
- Key Vulnerability Factors:
- ↑ Metabolic rate & surface area to body mass ratio → ↑ absorption & dose per unit body weight.
- Immature detoxification pathways (e.g., liver, kidneys).
- Developing organ systems (brain, lungs, immune system) are highly susceptible to damage.
- Longer future life expectancy allows more time for chronic disease development.
- Unique behaviors: hand-to-mouth activity, playing close to the ground, pica.
- 📌 Mnemonic: HEAL (Higher intake/unit body weight, Exploratory behaviors, Absorb more, Longer life span for effects).
- Environmental history is crucial for diagnosis, prevention, and anticipatory guidance.
⭐ Children absorb a significantly higher fraction of ingested lead (up to 50%) compared to adults (10-15%).
History Components - Snoop for Pollutants
- Systematic environmental history is key for exposure identification.
- Use mnemonics for questioning. 📌 S.N.O.O.P. helps:
- Sources: Pollutant origins (home, school, play, parents' work).
- Nature: Toxin type (chemical, physical, biological).
- Onset & Timing: Link symptoms to exposure periods.
- Others Affected: Symptoms in family, pets, contacts?
- Protective Measures: Current safeguards (ventilation, hygiene, PPE).
⭐ A detailed environmental history can uncover the etiology in up to 80% of pediatric toxin-related conditions.
Key Indian Exposures - Desi Toxin Hotspots
- Lead (Pb)
- Sources: Surma, kajal, old paint, batteries (improper recycling), some folk remedies, contaminated toys.
- Effects: Neurotoxicity (↓IQ, behavioral issues), anemia, abdominal colic. Blood Lead Level (BLL) > 5 µg/dL concerning.
- Arsenic (As)
- Sources: Contaminated groundwater (e.g., West Bengal, Bihar), pesticides, some traditional medicines.
- Effects: Skin lesions (keratosis, pigmentation), cancers (skin, bladder, lung), neuropathy. Mee's lines.
- Fluoride (F)
- Sources: Groundwater in Fluorosis Belt (e.g., Rajasthan, Gujarat), excessive toothpaste ingestion.
- Effects: Dental fluorosis (mottling), skeletal fluorosis. Optimal drinking water: 0.7-1.2 ppm.
- Pesticides (Organophosphates, Organochlorines)
- Sources: Agricultural runoff, improper home storage/use, contaminated food/water.
- Effects: OPs: Cholinergic crisis (📌 SLUDGE: Salivation, Lacrimation, Urination, Defecation, GI distress, Emesis). OCs: Neurotoxic, endocrine disruptors.
- Mercury (Hg)
- Sources: Broken thermometers, CFL bulbs, some skin-lightening creams, contaminated fish.
- Effects: Neurotoxic (tremors, ataxia - Minamata-like), nephrotoxic.
- Indoor Air Pollution
- Sources: Biomass fuel (wood, dung) for cooking in poorly ventilated homes, tobacco smoke, mosquito coils.
- Effects: ↑Risk of Acute Lower Respiratory Infections (ALRI), asthma, otitis media, ↓lung function.

⭐ Chronic arsenic exposure from contaminated groundwater in states like West Bengal and Bihar is a significant public health problem, leading to characteristic skin changes (melanosis, keratosis) and increased cancer risk.
Clinical Clues & Action - Red Flag Roundup
- Developmental Delay/Regression:
- Clues: Lead, mercury, pesticides.
- Action: Exposure Hx; Blood Lead Levels (BLL); neurodevelopmental assessment.
- Recurrent Respiratory Issues (wheeze, asthma):
- Clues: Indoor (mold, VOCs) / outdoor air pollution.
- Action: Environmental Hx (home/school); spirometry.
- Unexplained Skin Rashes:
- Clues: Allergens, irritants, pesticides.
- Action: Exposure Hx; consider patch testing if chronic.
- Chronic GI Symptoms (pain, V/D):
- Clues: Contaminated water/food (heavy metals, nitrates).
- Action: Dietary Hx; water/stool tests.
- New Neurological Symptoms (headache, seizure, ataxia):
- Clues: CO, pesticides, solvents, lead.
- Action: Exposure Hx; specific toxin testing.
- Pica:
- Clues: Lead; iron deficiency.
- Action: BLL; iron studies.
- Multiple Affected Household Members (incl. pets):
- Clue: Common source exposure.
- Action: Investigate shared environment.
⭐ > Blood lead levels (BLL) ≥ 5 µg/dL in children are a critical action threshold, mandating environmental investigation and follow-up.
High‑Yield Points - ⚡ Biggest Takeaways
- Systematic inquiry into home, school, and play environments is crucial for identifying hazards.
- Key exposures include lead, pesticides, molds, tobacco smoke, indoor/outdoor air pollutants, and contaminated water.
- Indian context: Probe biomass fuel use, water source/purity, and local agricultural/industrial activities.
- Children's unique vulnerabilities: ↑intake per kg, developing organs, hand-to-mouth activity, lesser detoxification.
- Parental occupational history is vital for identifying "take-home" toxins.
- Always correlate symptoms and developmental progress with potential environmental exposure timelines.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

