Indications for RRT in Children - RRT SOS Signals
📌 AEIOU Mnemonic:
- Acidosis: Severe metabolic (pH < 7.1-7.2), refractory to therapy.
- Electrolytes (refractory):
- Hyperkalemia (K⁺ > 6.5-7 mEq/L or ECG changes).
- Symptomatic Na⁺ imbalance.
- Severe hyperphosphatemia.
- Intoxications: Dialyzable drugs/toxins (e.g., salicylates, methanol, lithium).
- Overload: Fluid overload refractory to diuretics, causing respiratory compromise.
- Uremia: Symptomatic (encephalopathy, pericarditis, uremic bleeding).
⭐ Early RRT is crucial in pediatric AKI with severe fluid overload (>15-20% body weight).
RRT Modalities Overview - The Pediatric Toolkit
| Modality | Access | Key Features & Pediatric Suitability | Main Drawbacks |
|---|---|---|---|
| PD | PD Catheter | Preferred neonates/infants; home-based; continuous (e.g., CAPD/APD) | Peritonitis risk; protein loss; catheter issues |
| IHD | CVC, AVF/G | Older children; efficient; intermittent (e.g., 3-5 hr sessions, 3x/wk) | Hemodynamic instability; disequilibrium; access |
| CRRT | CVC | PICU unstable patients; continuous (24 hr); slow, precise control | Requires ICU; complex; anticoagulation; costly |
Peritoneal Dialysis (PD) Deep Dive - Belly Bath Method
- Mechanism: Peritoneal membrane as filter for solute & water exchange.
-
Catheter: Tenckhoff common; surgically placed.
- Solutions: Dextrose (1.5%, 2.5%, 4.25%); Icodextrin for long dwells.
- Cycles: Fill (infuse), Dwell (exchange), Drain (remove).
- Types:
- CAPD: Manual, 3-5 exchanges/day.
- APD/CCPD: Automated cycler, overnight.
- Parameters:
- Fill volume: 800-1100 mL/m² or 30-40 mL/kg.
- Dwell: CAPD 4-6 hrs; APD 1-2 hrs.
- Complications: Peritonitis (cloudy fluid, pain), exit-site/tunnel infections, leaks, hernias.
⭐ Peritonitis is the most common serious PD complication; often S. epidermidis or S. aureus.
Hemodialysis (HD) & CRRT - Blood Purifying Power
- Hemodialysis (HD): Efficiently clears toxins & excess fluid via diffusion/convection.
- Access: AV fistula/graft, CVC.
- Anticoagulation: Heparin. BFR: 5-7 ml/kg/min. DFR: ~2x BFR.
- Adequacy: $Kt/V > extbf{1.2}$. $URR = ((Pre_{BUN} - Post_{BUN}) / Pre_{BUN}) \times 100%$.
- Key risks: Hypotension, disequilibrium syndrome.
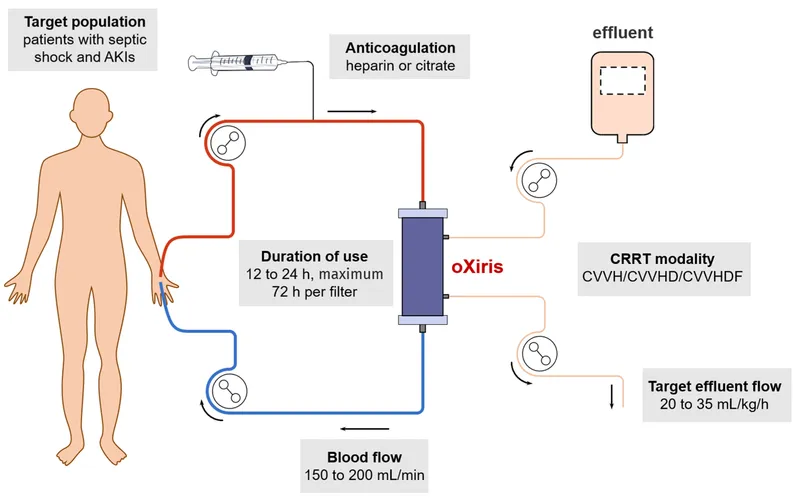
- CRRT (Continuous Renal Replacement Therapy): For unstable AKI; maintains physiologic balance.
- Modes: CVVH (convection), CVVHD (diffusion), CVVHDF.
- Anticoagulation: Regional citrate preferred.
- Effluent dose: 20-25 ml/kg/hr for optimal clearance.
⭐ CRRT is preferred in hemodynamically unstable children with AKI due to better fluid balance control and cardiovascular stability.
Complications & Special Issues - Navigating RRT Challenges
- Infections: Peritonitis (PD), CRBSI (HD/CRRT).
- Cardiovascular: Hypertension, LVH, arrhythmias.
- Nutrition & Growth: Malnutrition, growth failure (critical).
- Anemia: ↓EPO, blood loss; manage with ESA, iron.
- Mineral Bone Disorder (MBD): Monitor Ca, P, PTH, Vit D.
- Access Issues: Thrombosis, stenosis, infection.
- Psychosocial: Schooling, adherence, family stress.
- Fluid/Electrolyte Imbalance: HyperK, hypoCa, acidosis.
⭐ Growth failure is a major long-term complication in children on RRT, impacting final adult height and quality of life.
High‑Yield Points - ⚡ Biggest Takeaways
- Peritoneal dialysis (PD) is preferred in neonates/infants; easier access.
- Hemodialysis (HD) needs good vascular access; AV fistula ideal but challenging.
- CRRT for hemodynamically unstable children, mainly in PICU.
- Indications: AKI with fluid overload, severe electrolyte imbalance, uremia, intoxications.
- Complications: Peritonitis (PD), hypotension (HD), access issues, electrolyte disturbances.
- Dialysis dose calculation is critical, based on pediatric body size.
- Growth failure is a major concern with chronic RRT.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

