Common URTIs - Sniffles & Soreness
- Common Cold (Viral Rhinitis):
- Etiology: Rhinovirus (MC), Adenovirus, RSV.
- Sx: Rhinorrhea, nasal congestion, sore throat, cough.
- Tx: Symptomatic relief (fluids, rest).
- Acute Otitis Media (AOM):
- Etiology: Streptococcus pneumoniae (MC), Haemophilus influenzae (non-typable), Moraxella catarrhalis. 📌 SHiM.
- Sx: Otalgia, fever, irritability, red bulging Tympanic Membrane (TM).
- Tx: Analgesia. Amoxicillin (80-90 mg/kg/d) if severe/bilateral <2y/otorrhea.
⭐ Most common bacterial cause of Acute Otitis Media is Streptococcus pneumoniae.
- Pharyngitis/Tonsillitis:
- Etiology: Viral (MC). Bacterial: Group A Streptococcus (GAS) - S. pyogenes.
- Sx: Sore throat, fever. Tonsillar exudates, palatal petechiae (GAS). Modified Centor criteria.
- Tx: Symptomatic (viral); Penicillin/Amoxicillin (GAS) to prevent Rheumatic Fever.
- Acute Bacterial Rhinosinusitis (ABRS):
- Sx: Persistent nasal discharge/cough >10 days without improvement, OR severe (fever ≥39°C, purulent discharge) for ≥3 days, OR worsening symptoms.
- Etiology: S. pneumoniae, H. influenzae.
- Tx: Amoxicillin.
Acute Airway Obstruction - Alarming Breaths
Stridor, distress, voice change. Rapid assessment vital.
-
Epiglottitis (Supraglottitis):
- Rapid onset, toxic, high fever. 📌 4 D's: Drooling, Dysphagia, Distress, Dysphonia (muffled). Tripod position.
- X-ray: Thumbprint sign (lateral neck).
- Mgmt: Secure airway (OR!), IV Ceftriaxone. Avoid agitation.
⭐ Epiglottitis classically presents with 'tripod position', drooling, dysphagia, and distress (the 4 D's).
-
Croup (Laryngotracheobronchitis):
- Viral (Parainfluenza). Barking cough, hoarseness, inspiratory stridor.
- X-ray: Steeple sign (AP neck).
- Mgmt: Dexamethasone; nebulized Epinephrine (moderate-severe).
-
Foreign Body Aspiration (FBA):
- Sudden choking/gagging Hx. Unilateral wheeze/↓air entry.
- X-ray: May show object, unilateral hyperinflation/atelectasis.
- Mgmt: Rigid bronchoscopy.
-
Bacterial Tracheitis:
- S. aureus (often post-viral). Toxic, high fever, purulent secretions.
- Mgmt: Airway support, IV antibiotics. Poor response to croup Rx.
Lower Respiratory Infections - Deeper Lung Troubles
Bronchiolitis
- Acute viral inflammation of bronchioles; primarily affects infants < 2 years (peak 2-6 months).
- Etiology: Respiratory Syncytial Virus (RSV) most common; also Parainfluenza, Adenovirus.
⭐ RSV is the leading cause of bronchiolitis, typically affecting infants <2 years old, with peak incidence at 2-6 months.
- Clinical: Coryza, cough, expiratory wheeze, tachypnea, retractions. Apnea in young infants.
- Diagnosis: Clinical. CXR (not routine): hyperinflation, peribronchial thickening.
- Management: Supportive (O2 for SpO2 < 90-92%), hydration. Palivizumab prophylaxis for high-risk.
Pneumonia
- Infection of lung parenchyma.
- Etiology (Community-Acquired):
- Neonates: Group B Strep, E. coli.
- Infants/Young Children: Viruses (RSV), S. pneumoniae.
- Older Children: Mycoplasma pneumoniae, S. pneumoniae.
- Clinical: Fever, cough, tachypnea (WHO: <2m: >60/min; 2-12m: >50/min; 1-5y: >40/min 📌 Mnemonic: 60-50-40), crackles, ↓air entry.
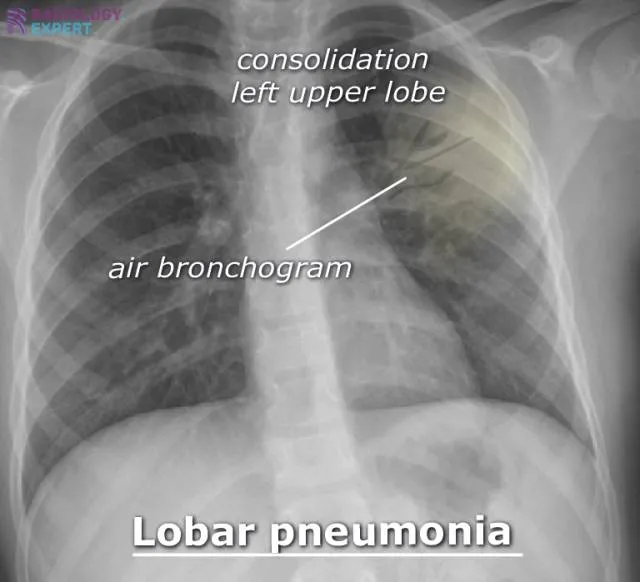
- Diagnosis: Clinical; CXR shows infiltrates/consolidation.
- Management: Amoxicillin (first-line for typical bacterial CAP). Supportive care.
Specific Chronic/Recurrent Infections - Lingering Lung Woes
-
Pertussis (Whooping Cough)
- Agent: Bordetella pertussis.
- Stages: Catarrhal (highly contagious, URI sx), Paroxysmal (inspiratory "whoop", post-tussive emesis, lymphocytosis), Convalescent.
- Dx: PCR (NP swab), culture.
- Rx: Macrolides (e.g., Azithromycin).
- Prevention: DTaP/Tdap vaccine.
- Complications: Apnea (infants), pneumonia, seizures.
⭐ Characteristic 'whooping' cough and marked lymphocytosis are key features of the paroxysmal stage of Pertussis.
-
Pediatric Tuberculosis (TB)
- Agent: Mycobacterium tuberculosis.
- Sx: Persistent cough >2 wks, fever >2 wks, weight loss/failure to thrive.
- Dx:
- TST (Mantoux): Induration ≥5 mm (HIV/close contact), ≥10 mm (<4yrs/high risk/chronic illness), ≥15 mm (>4yrs/low risk).
- IGRA, CXR (hilar adenopathy), AFB smear/culture (gastric aspirate/sputum), NAAT.
- Rx: Standard Anti-Tubercular Therapy (ATT).
- Prevention: BCG vaccine (prevents severe forms).
High‑Yield Points - ⚡ Biggest Takeaways
- Bronchiolitis (<2 yrs) is mainly by RSV; treatment is supportive.
- Croup presents with barking cough & stridor; Parainfluenza virus is the usual cause.
- Epiglottitis (often Hib) shows drooling, dysphagia, distress; it's an emergency.
- Pertussis (B. pertussis) has a paroxysmal cough and inspiratory "whoop".
- S. pneumoniae is the top cause of typical bacterial pneumonia in children.
- Mycoplasma pneumoniae causes atypical pneumonia, especially in older children.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

