Normal Puberty - The Hormone Symphony
Puberty: A neuroendocrine cascade driven by pulsatile Gonadotropin-Releasing Hormone (GnRH) from the hypothalamus. Influenced by genetics, nutrition (Leptin: permissive), and Kisspeptin.
- Core Pathway (Gonadarche):
- Hypothalamus: Pulsatile GnRH release.
- Anterior Pituitary: Secretes LH & FSH.
- Gonads (Ovaries/Testes): Produce sex steroids (Estrogen-♀ / Testosterone-♂) under LH/FSH stimulation.
- Effects: Development of secondary sexual characteristics, growth spurt, achievement of fertility.
- Adrenarche:
- Separate adrenal androgen (DHEA, DHEAS) surge around 6-8 years.
- Contributes to pubic/axillary hair (pubarche), body odor, acne.

⭐ The first sign of puberty in girls is thelarche (breast budding); in boys, it's testicular enlargement (≥ 4ml or > 2.5cm length).
Precocious Puberty - Early Bloomers
- Definition: Onset of secondary sexual characteristics before age 8 in girls, 9 in boys.
- Types:
- Central (GnRH-dependent): Premature activation of Hypothalamic-Pituitary-Gonadal (HPG) axis.
- Idiopathic (most common, esp. girls).
- CNS lesions: Hamartoma (most common tumor), astrocytoma, hydrocephalus.
- Peripheral (GnRH-independent): Excess sex steroids from gonads, adrenals, or exogenous sources.
- Girls: Ovarian cysts/tumors.
- Boys: Leydig cell tumors, Congenital Adrenal Hyperplasia (CAH), HCG-secreting tumors.
- McCune-Albright Syndrome (MAS).
- Central (GnRH-dependent): Premature activation of Hypothalamic-Pituitary-Gonadal (HPG) axis.
- Incomplete variants: Premature thelarche, premature adrenarche/pubarche.
- Diagnosis:
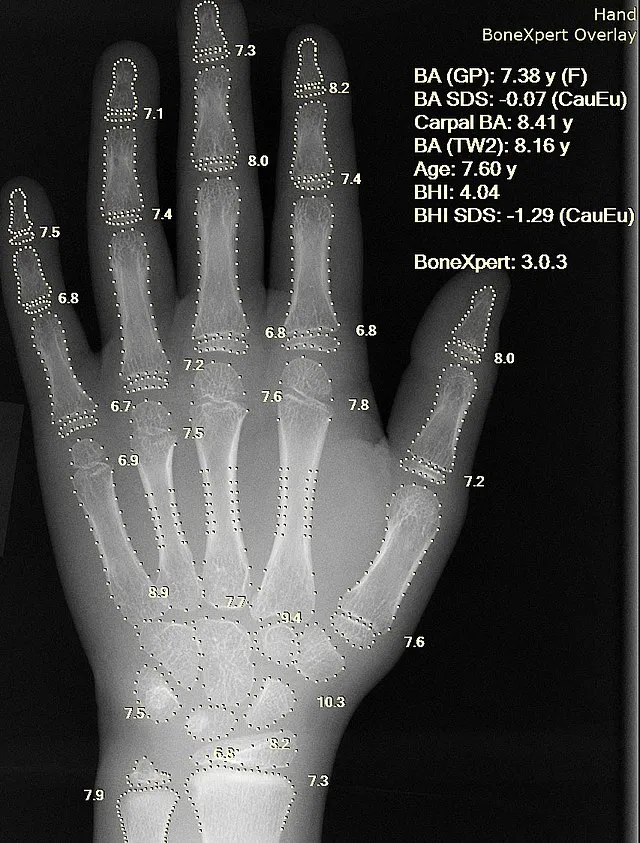
- Advanced bone age (X-ray hand/wrist).
- GnRH stimulation test: Differentiates Central (LH surge) from Peripheral (suppressed LH). Peak LH >5-8 IU/L; LH/FSH ratio >0.6.
- Pelvic/Testicular USG. Brain MRI for Central PP (esp. boys & girls <6 yrs).
- Treatment:
- Central: GnRH analogs (e.g., Leuprolide).
- Peripheral: Address underlying cause.
⭐ McCune-Albright Syndrome triad:
- Peripheral precocious puberty.
- Café-au-lait macules (irregular "coast of Maine" border).
- Polyostotic fibrous dysplasia.
Delayed Puberty - Late to the Party
- Definition:
- Girls: No breast development (thelarche) by 13 years; no menarche by 16 years or >5 years after thelarche.
- Boys: No testicular enlargement (testicular volume <4 mL or longest diameter <2.5 cm) by 14 years.
- Most common: Constitutional Delay of Growth & Puberty (CDGP) - "late bloomers"; delayed bone age, positive family history.
- Classification & Key Causes:
- Hypogonadotropic Hypogonadism (Central; ↓FSH/LH):
- Functional: Chronic illness, malnutrition, hypothyroidism, intense exercise.
- Congenital: Kallmann syndrome (anosmia), Prader-Willi.
- Acquired: CNS tumors (e.g., craniopharyngioma).
- Hypergonadotropic Hypogonadism (Primary Gonadal Failure; ↑FSH/LH):
- Girls: Turner syndrome (45,XO).
- Boys: Klinefelter syndrome (47,XXY).
- Other: Gonadal dysgenesis, post-chemo/radiation.
- Hypogonadotropic Hypogonadism (Central; ↓FSH/LH):
- Initial Evaluation: History, exam (Tanner staging), bone age. Then FSH, LH, Estradiol/Testosterone.
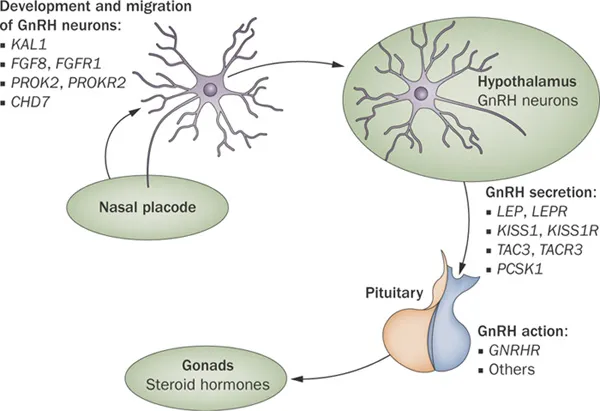
⭐ Kallmann syndrome: Defective GnRH neuron migration leading to hypogonadotropic hypogonadism and anosmia/hyposmia. Often KAL1 gene mutation.
High‑Yield Points - ⚡ Biggest Takeaways
- Tanner staging is crucial for pubertal assessment.
- Precocious puberty: onset <8 years (girls), <9 years (boys).
- Delayed puberty: no signs by 13 years (girls), 14 years (boys).
- McCune-Albright syndrome: triad of precocious puberty, café-au-lait spots, polyostotic fibrous dysplasia.
- Kallmann syndrome: hypogonadotropic hypogonadism plus anosmia.
- Constitutional delay (CDGP): most common cause of delayed puberty in boys.
- Central precocious puberty is GnRH-dependent; peripheral is GnRH-independent.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

