Pleural Effusions - Fluid Follies
Fluid in pleural space. Differentiated by Light's Criteria.
- Light's Criteria (Exudate if ≥1):
- Pleural/Serum Protein > 0.5
- Pleural/Serum LDH > 0.6
- Pleural LDH > $\frac{2}{3}$ ULN serum LDH (>200 IU/L)
- Transudate (Systemic: ↑Hydrostatic/↓Oncotic pressure):
- CHF (commonest), Cirrhosis, Nephrotic Syndrome, PE.
- Exudate (Local: ↑Pleural permeability/↓Lymphatic drainage):
- Infection (Pneumonia, TB - commonest exudative in India), Malignancy, PE, Autoimmune.

- Features: Dyspnea, cough, pleuritic pain. Stony dullness, ↓breath sounds.
- Dx: CXR (PA >200ml, Lat Decubitus >50ml), Thoracentesis.
- Rx: Treat cause. Therapeutic tap for large effusions.
⭐ Meigs' syndrome: Benign ovarian tumor + ascites + pleural effusion (transudate). Resolves post-tumor removal.
Pneumothorax - Air Escapades
- Definition: Air in pleural space → lung collapse.
- Types:
- Spontaneous:
- Primary (PSP): No lung disease; apical bleb rupture (tall, thin young males).
- Secondary (SSP): Underlying lung disease (COPD, TB, asthma).
- Traumatic: Penetrating/blunt chest trauma.
- Iatrogenic: Post-medical procedure (central line, biopsy).
- Spontaneous:
- Tension Pneumothorax: ⚠️ Emergency!
- One-way valve → ↑ intrapleural pressure.
- Mediastinal shift (away), ↓ venous return, cardiovascular collapse. Tracheal deviation.
- Clinical: Acute dyspnea, pleuritic pain, ↓ breath sounds, hyperresonant percussion.
- Diagnosis:
- CXR: Visceral pleural line, absent lung markings. Deep sulcus sign (supine).
- USG: No lung sliding ("barcode sign"); lung point sign (specific).
- CT: Most sensitive; detects small pneumothorax, bullae.

- Management:
- Pleurodesis: For recurrent/persistent cases (talc, doxycycline).
⭐ Deep Sulcus Sign: On supine CXR, a deep, lucent costophrenic angle suggests pneumothorax.
Pleuritis & Empyema - Inflammatory Invasions
- Pleuritis: Pleural inflammation. Causes: Infection (pneumonia, TB), malignancy, autoimmune (SLE). Sx: Sharp pleuritic chest pain, fever.
- Empyema: Pus in pleural space. Common organisms: S. aureus, S. pneumoniae, anaerobes.
- Stages:
- Exudative: Sterile exudate, ↑capillary permeability.
- Fibrinopurulent: Bacterial invasion, frank pus, fibrin deposition.
- Organizing: Fibroblast proliferation, thick pleural peel, potential trapped lung.
- Diagnosis: Thoracentesis. Pleural fluid: pH < 7.20, glucose < 60 mg/dL, LDH > 1000 IU/L, ↑WBCs, positive Gram stain/culture.
⭐ Frank pus on aspiration, positive Gram stain/culture from pleural fluid, OR pleural fluid pH < 7.20 confirms empyema.
- Stages:
- Treatment: Systemic antibiotics, complete pleural fluid drainage (e.g., chest tube, VATS/decortication). Complication: Fibrothorax.

Pleural Tumors - Neoplastic Nightmares
- Primary tumor: Malignant Mesothelioma (MM); Secondary: Metastases (more common).
- Malignant Mesothelioma (MM)
- Strongly linked to asbestos exposure (long latency: 20-40 years). 📌 "A"sbestos for "M"esothelioma.
- Gross: Thick, white, gelatinous sheets encasing lung ("pleural rind").
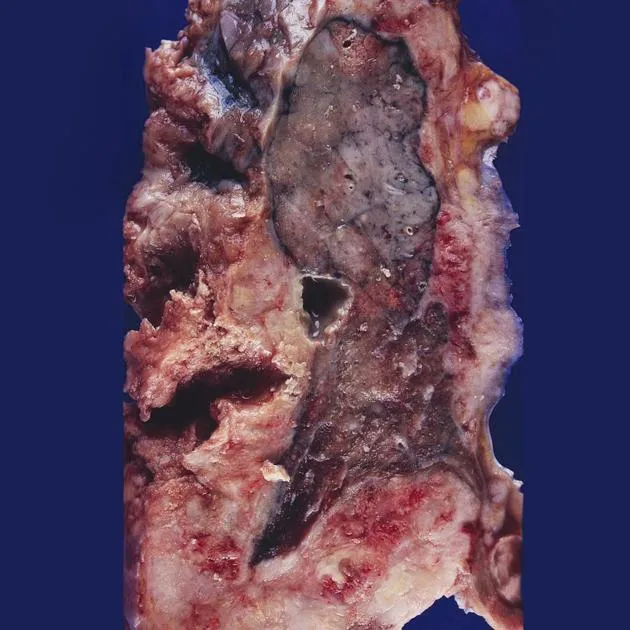
- Histology:
- Epithelioid (most common, ~60%; better prognosis).
- Sarcomatoid (~20%; worst prognosis).
- Biphasic (~20%; intermediate prognosis).
- IHC Markers: Calretinin+, WT-1+, CK5/6+, D2-40+ (positive); CEA- (negative) (vs. Adenocarcinoma).
- Symptoms: Insidious onset chest pain, dyspnea, weight loss, recurrent effusions.
⭐ Psammoma bodies can be seen in epithelioid mesothelioma.
- Metastatic Pleural Tumors
- Most common pleural malignancy.
- Primaries: Lung > Breast > Ovary, Lymphoma.
- Often presents as malignant pleural effusion, leading to dyspnea.
High‑Yield Points - ⚡ Biggest Takeaways
- Light's criteria differentiate transudative (e.g., CHF, cirrhosis) from exudative (e.g., infection, malignancy) effusions.
- Tuberculous pleurisy typically presents as a lymphocytic exudate with elevated ADA (>40 U/L).
- Malignant effusions are often hemorrhagic; cytology is key for diagnosis.
- Empyema, pus in the pleural space, necessitates thoracentesis and often chest tube drainage.
- Tension pneumothorax is a medical emergency requiring immediate needle decompression.
- Mesothelioma is strongly linked to asbestos exposure and has a poor prognosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

