Acute Pancreatitis: Definition & Etiology - Pancreas Ablaze!
- Definition: Acute inflammatory process of the pancreas, typically reversible, with variable involvement of regional tissues or remote organ systems.
- Etiology:
- Gallstones (most common, ~40-50%)
- Alcohol (~30-40%)
- 📌 I GET SMASHED mnemonic:
- Idiopathic
- Gallstones
- Ethanol
- Trauma
- Steroids
- Mumps/Malignancy
- Autoimmune (e.g., IgG4-related)
- Scorpion sting
- Hypercalcemia/Hypertriglyceridemia (Triglycerides > 1000 mg/dL)
- ERCP
- Drugs (e.g., azathioprine, valproate, thiazides)
⭐ Gallstones and alcohol together account for approximately 70-80% of acute pancreatitis cases in most populations.
 oka
oka
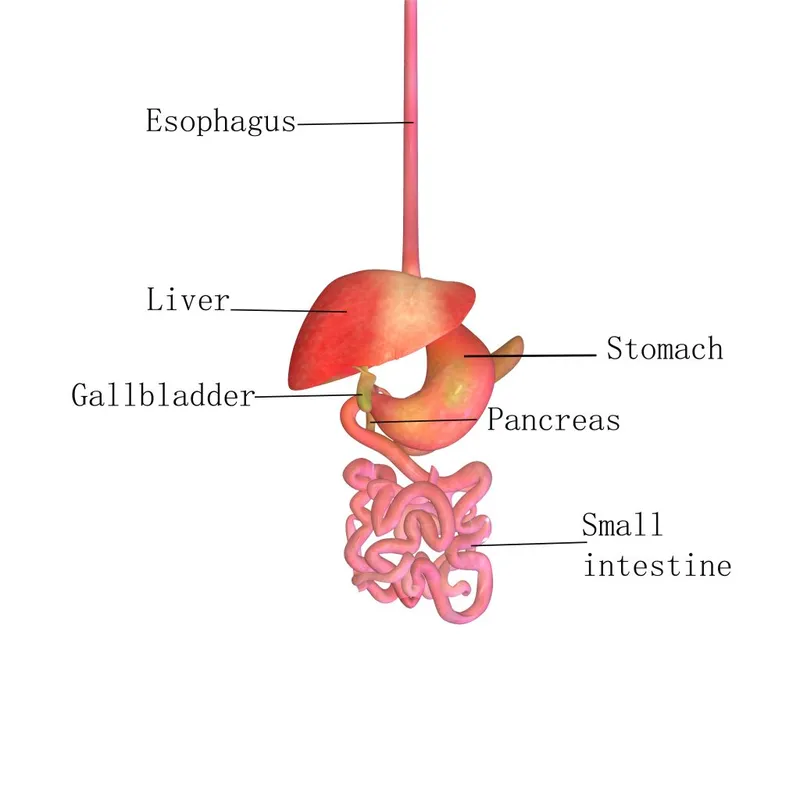
Acute Pancreatitis: Pathophysiology - Enzyme Mayhem
- Core: Pancreatic autodigestion by prematurely activated enzymes in acinar cells.
- Initiation & Enzyme Cascade:
- Critical event: Intra-acinar activation of trypsinogen to trypsin.
- Trypsin activates other zymogens:
- Proelastase $\rightarrow$ Elastase (vessel/tissue damage).
- Prophospholipase A2 $\rightarrow$ Phospholipase A2 (membrane damage).
- Pathological Consequences:
- Acinar cell injury and necrosis.
- Local inflammation and cytokine release (TNF-α, IL-1, IL-6), leading to systemic effects (SIRS).
- Fat necrosis via saponification: $Ca^{2+} + \text{fatty acids} \rightarrow \text{calcium soaps}$; may cause hypocalcemia.
⭐ The critical initiating event in acute pancreatitis is the intra-acinar activation of trypsinogen to trypsin.
Acute Pancreatitis: Clinical & Diagnosis - Spotting the Flames
- Symptoms: Acute, severe, persistent epigastric pain radiating to back; relieved by leaning forward. Nausea, vomiting.
- Signs:
- Epigastric tenderness, guarding.
- Severe: Tachycardia, hypotension, jaundice.
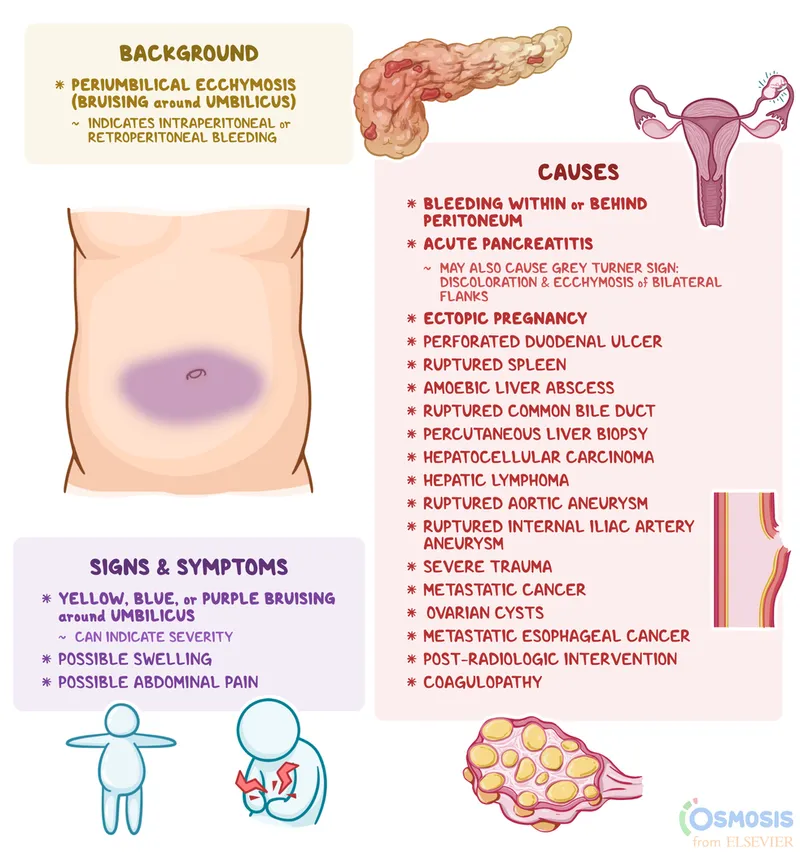
- ⚠️ Cullen's sign (periumbilical ecchymosis), Grey Turner's sign (flank ecchymosis) → retroperitoneal hemorrhage, severe disease, poor prognosis.
- Diagnosis (Revised Atlanta Criteria - Need 2 of 3):
- Characteristic abdominal pain.
- Serum amylase and/or lipase ≥ 3x ULN.
- Characteristic imaging findings (CECT, MRI, USG).
- Labs:
- Lipase: More sensitive & specific than amylase, remains ↑ longer.
- CRP: ↑ indicates severity.
⭐ Serum lipase is preferred over amylase for diagnosing acute pancreatitis due to its higher specificity and longer duration of elevation.
- Imaging:
- USG Abdomen: Initial (to detect gallstones).
- CECT: Best for diagnosis confirmation (if unclear), assessing severity (e.g., necrosis), and detecting complications (usually 48-72 hours after onset if indicated).
Acute Pancreatitis: Severity & Complications - Gauging the Inferno
- Revised Atlanta Classification:
- Mild: No organ failure, no local/systemic complications.
- Moderately Severe: Transient organ failure (<48h) OR local/systemic complications (no persistent organ failure).
- Severe: Persistent organ failure (>48h).
- Severity Scoring:
- BISAP (Bedside Index of Severity in Acute Pancreatitis): 1 point each for:
- BUN >25 mg/dL
- Impaired mental status (GCS <15)
- SIRS (≥2 criteria)
- Age >60 years
- Pleural Effusion
- Score ≥3 indicates ↑ mortality.
- Others: Ranson's criteria, APACHE II.
- BISAP (Bedside Index of Severity in Acute Pancreatitis): 1 point each for:
- Local Complications:
- Acute Peripancreatic Fluid Collection (APFC)
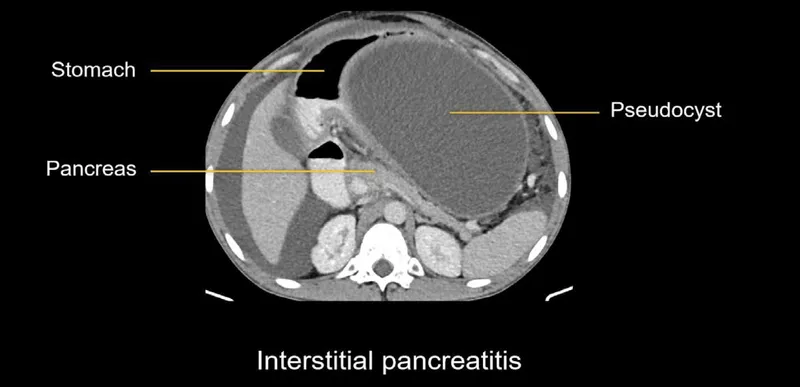
- Pancreatic Pseudocyst (>4 wks, encapsulated fluid, defined wall)
- Acute Necrotic Collection (ANC)
- Walled-Off Necrosis (WON) (>4 wks, encapsulated necrosis ± debris)
- Infected necrosis (critical)
- Pancreatic abscess
- Systemic Complications:
- SIRS, ARDS, AKI
- Cardiovascular collapse/shock, DIC
- Metabolic: Hypocalcemia (saponification), Hyperglycemia
⭐ Hypocalcemia (serum Ca < 8 mg/dL or ionized Ca < 1.0 mmol/L) indicates severe disease and poor prognosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Gallstones and alcohol abuse are the leading causes of acute pancreatitis.
- Characterized by severe epigastric pain, often radiating to the back, with nausea and vomiting.
- Elevated serum lipase (more specific) and amylase are crucial for diagnosis.
- Ranson's criteria and APACHE II score are used to assess severity and prognosis.
- Major complications include pancreatic pseudocyst, necrosis, ARDS, and hypocalcemia (saponification).
- Sentinel loop on X-ray and Grey Turner's/Cullen's signs indicate severe disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

