Urinary Specimens & Normal Cells - What's In Your Wee?
- Specimen Types:
- Voided (midstream clean-catch): Most common.
- Catheterized: Avoids vulvovaginal contamination.
- Bladder Washings/Lavage: ↑ cellularity, for suspected lesions.
- Ileal Conduit: Post-cystectomy.
- Ureteric/Renal Pelvic Brushings: Upper tract evaluation.
- Processing & Preservation:
- Fresh: Examine within 1-2 hrs.
- Refrigerate (4°C): Up to 24 hrs.
- Fixatives: 50% Ethanol, Saccomanno (Carbowax).
- Normal Cellular Elements:
- Urothelial (Transitional): Superficial (umbrella), intermediate, deep (basal).
- Squamous: Common (esp. females); usually contaminants.
- RBCs: <5/HPF.
- WBCs: <5/HPF (neutrophils).
- Casts: Occasional hyaline.
- Crystals, mucus, spermatozoa.
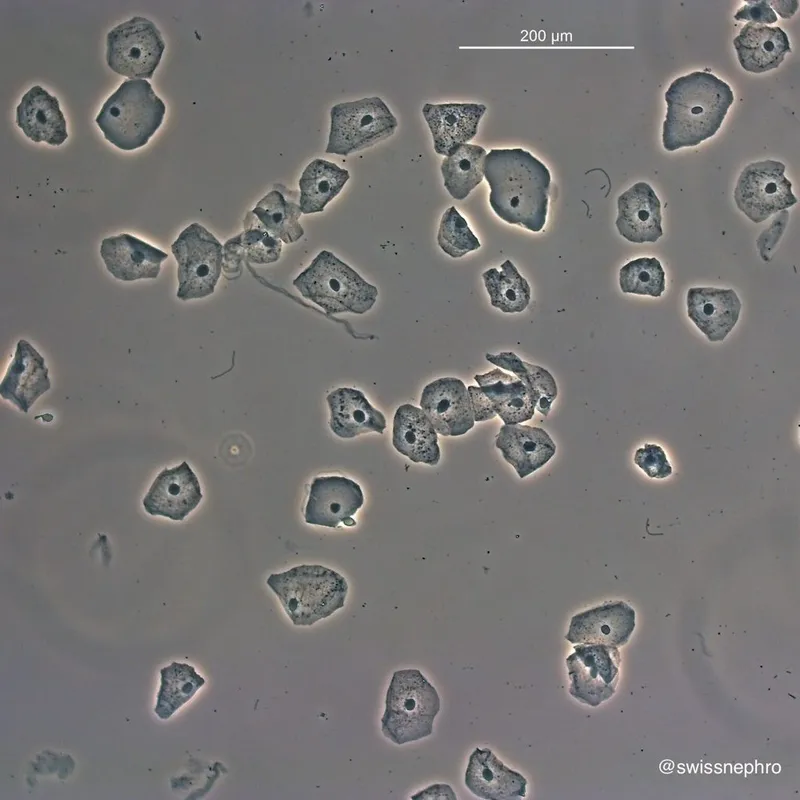
⭐ Deep urothelial cells naturally show a higher N/C ratio than superficial cells; misinterpreting this as atypia is a common pitfall.
Benign & Reactive Atypia - Not Always Bad News
- Non-neoplastic cellular changes that can mimic malignancy; crucial for differential diagnosis.
- Common Causes:
- Inflammation (UTI): Neutrophils, bacteria, reactive urothelial cells.
- Urolithiasis (stones): Mechanical irritation, cell clusters, mild atypia.
- Instrumentation (catheter, cystoscopy): Sheets or clusters of reactive cells.
- Therapy-induced changes:
- Radiation: Cytomegaly, nucleomegaly, bizarre cell shapes, smudged chromatin, but often maintained N/C ratio.
- Chemotherapy (e.g., Cyclophosphamide, Thiotepa): Similar to radiation; multinucleation common.
- Key Cytologic Features:
- Mild nuclear enlargement, smooth nuclear membranes.
- Finely granular, evenly distributed chromatin (or smudged/degenerated).
- Prominent, centrally located nucleoli (if reactive).
- Inflammatory background, cytoplasmic vacuolization.

⭐ Polyomavirus (BK virus) infection characteristically produces "Decoy cells": urothelial cells with large, homogenous, basophilic or amphophilic ground-glass intranuclear inclusions, which can be mistaken for High-Grade Urothelial Carcinoma (HGUC), especially in immunocompromised patients like renal transplant recipients.
Urothelial Neoplasia & Paris System - Grading the Grim
The Paris System (TPS) for Reporting Urinary Cytology standardizes diagnosis, enhancing High-Grade Urothelial Carcinoma (HGUC) detection and reducing Atypical Urothelial Cells (AUC) rates.
-
Core Principle: Identify HGUC; other findings are secondary.
-
Key TPS Diagnostic Categories:
- Non-Diagnostic (ND)
- Negative for HGUC (NHGUC)
- Atypical Urothelial Cells (AUC)
- Suspicious for HGUC (SHGUC)
- High-Grade Urothelial Carcinoma (HGUC)
- Low-Grade Urothelial Neoplasm (LGUN)
-
HGUC Cytomorphologic Criteria (Mandatory):
- Nuclear to Cytoplasmic (N/C) ratio ≥ 0.7
- Severe hyperchromasia
- Marked nuclear pleomorphism (size/shape variation)
- Irregular nuclear contours/notched nuclei
- Coarsely granular, clumped chromatin
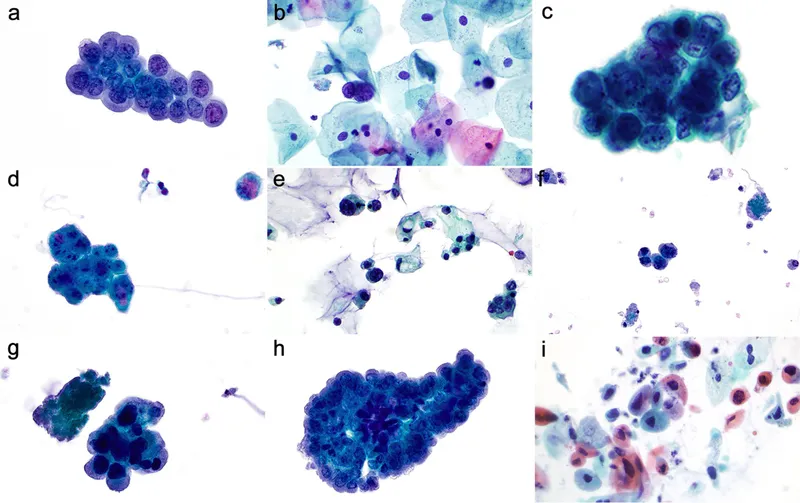
⭐ The Paris System (TPS) aims for high sensitivity for HGUC (>85%) while maintaining specificity, significantly improving interobserver reproducibility for HGUC diagnosis.
Other Malignancies & Ancillary Tests - Beyond Urothelial Scope
- Non-Urothelial Primaries:
- Squamous Cell Ca (SCC): Chronic irritation (Schistosoma). Keratin, bizarre cells. Markers: p63, CK5/6.
- Adenocarcinoma: Glandular, mucin. Primary (e.g., urachal) vs. metastatic (colorectal, prostate). Markers: CK7, CK20, CDX2, PSA.
- Small Cell Ca: Neuroendocrine. Nuclear molding, scant cytoplasm. Markers: Synaptophysin, Chromogranin.
- Metastatic Tumors: Most frequent non-urothelial. Common sources: prostate, colorectal, renal (RCC), lung, melanoma, lymphoma.
- Ancillary Tests (General):
- Immunocytochemistry (ICC): Key for lineage. Examples above.
- Molecular: FISH (UroVysion for urothelial Ca, detects aneuploidy of chr 3, 7, 17; 9p21 loss).
⭐ In urine cytology, adenocarcinoma cells from prostate typically show PSA & PSAP positivity.
High‑Yield Points - ⚡ Biggest Takeaways
- Voided urine is most common; catheterized for upper tract. Papanicolaou stain is standard.
- Decoy cells (polyomavirus) are key mimics of High-Grade Urothelial Carcinoma (HGUC).
- HGUC criteria: high N/C ratio, marked pleomorphism, coarse chromatin, irregular nuclear membranes.
- Low-Grade Urothelial Neoplasms (LGUN) show minimal atypia, making cytology diagnosis challenging.
- The Paris System (TPS) standardizes reporting, emphasizing HGUC detection.
- Schistosoma haematobium infection is a risk factor for squamous cell carcinoma.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

