MISS Fundamentals - Tiny Incisions, Big Relief
- Concept: Spine surgery via minimal incisions (e.g., 1-2 cm) using specialized tools like tubular retractors & endoscopes.
- Aim: Achieve surgical goals with ↓ iatrogenic injury to soft tissues, especially paraspinal muscles.
- Advantages:
- ↓ Blood loss & post-operative pain
- Shorter hospital stay & faster recovery
- Improved cosmesis
- Preservation of muscle function
- Enablers: Advanced imaging (fluoroscopy, navigation), specialized instruments, muscle-sparing corridors.
⭐ MISS significantly reduces iatrogenic muscle injury and paraspinal muscle atrophy compared to traditional open approaches, leading to better long-term functional outcomes and reduced chronic back pain related to surgery itself (failed back surgery syndrome component).
MISS Toolkit - Precision Instruments Galore
- Core: Specialized instruments enabling surgery via small incisions, minimizing iatrogenic soft tissue injury.
- Key Components:
- Sequential Dilators: Gradually create a working channel.
- Tubular/Expandable Retractors: Maintain surgical corridor (e.g., METRx™, Quadrant™ systems).
- Endoscopes & Microscopes: Provide magnified, illuminated views.
- Specialized Long Instruments: Bayoneted drills, curettes, Kerrison rongeurs for confined spaces.
- Guidance Tech:
- Intraoperative fluoroscopy (C-arm).
- Neuronavigation (e.g., O-arm based).
- Robotic assistance for enhanced precision.
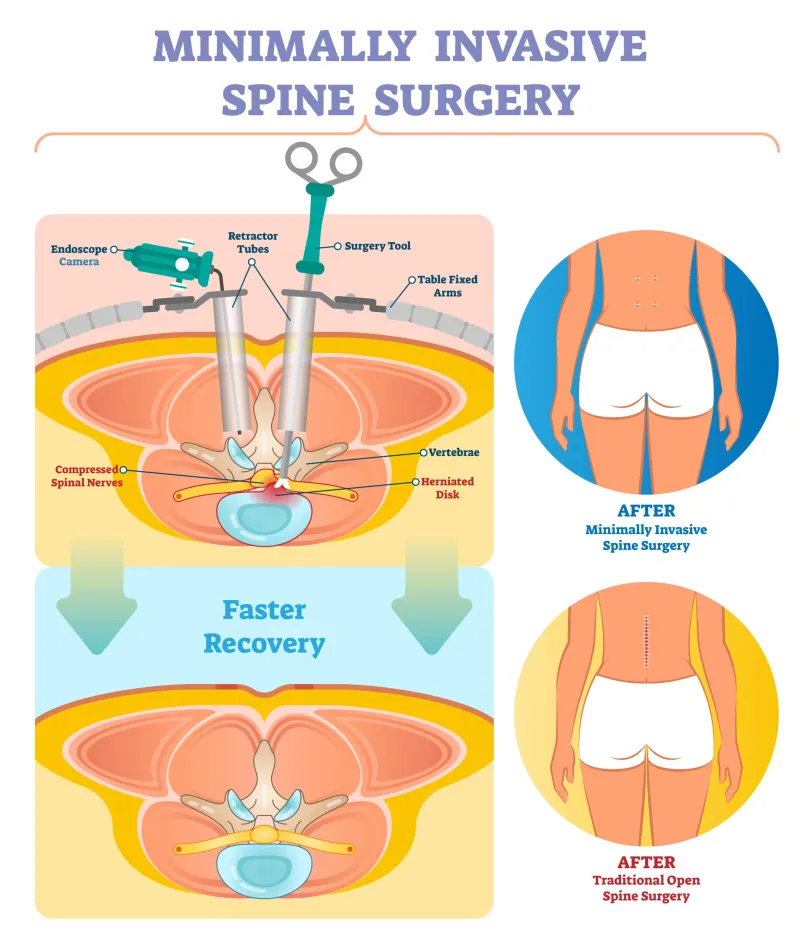
⭐ Tubular retractor systems are pivotal in MISS, facilitating a muscle-splitting approach rather than extensive muscle stripping, leading to reduced postoperative pain and faster recovery.
Common MISS Ops - Spine Fixes Simplified
- Principle: Match open surgery outcomes, minimize iatrogenic injury, preserve spinal stability.
- Enablers: Tubular retractors, endoscopes, percutaneous screws, advanced imaging/navigation.
Frequent Procedures & Targets:
- Microdiscectomy/Endoscopic Discectomy: For symptomatic herniated disc. Direct nerve root decompression.
- MISS TLIF/PLIF (Fusion): For instability, spondylolisthesis. Achieves fusion with percutaneous screws & interbody cage via muscle-sparing corridor.
- Vertebroplasty/Kyphoplasty: For painful osteoporotic vertebral compression fractures (VCF). PMMA cement for stabilization; Kyphoplasty adds balloon tamp for height restoration.
- MISS Decompression (Laminotomy/Foraminotomy): For lumbar spinal stenosis. Targeted bone/ligament removal for neural element relief.
⭐ MISS significantly reduces post-op infection risk (often <1%) and pain, leading to faster functional recovery.
Who Gets MISS? - Patient Selection Pointers
- Primary Indications:
- Focal, single or two-level pathology (e.g., contained disc herniation, unilateral stenosis).
- Predominant radicular pain > axial pain.
- Failure of adequate conservative management (typically >6-12 weeks).
- Absence of gross instability or severe deformity.
- Consider With Caution (Relative Contraindications):
- Severe osteoporosis (risk of fixation failure).
- Morbid obesity (BMI > 40).
- Multiple previous surgeries at the same level (scarring).
- Significant central stenosis with myelopathy (case-dependent).
⭐ Key indication: Unilateral, single-level lumbar disc herniation with radiculopathy refractory to 6 weeks of non-operative care.
MISS Pitfalls - Navigating Potential Problems
- Learning Curve: Steep; initial ↑ operative time; requires specialized training.
- Radiation Exposure: Significant C-arm use for surgeon & OR team. ⚠️
- Instrumentation: Limited tactile feedback; restricted working angles.
- Complications:
- Neural injury: Nerve root irritation/damage, dural tears (difficult repair).
- Implant malposition: Pedicle screw misplacement; navigation crucial.
- Incomplete decompression: Residual stenosis or disc.
- Access-related issues: Vascular or visceral injury (e.g., lateral approaches).
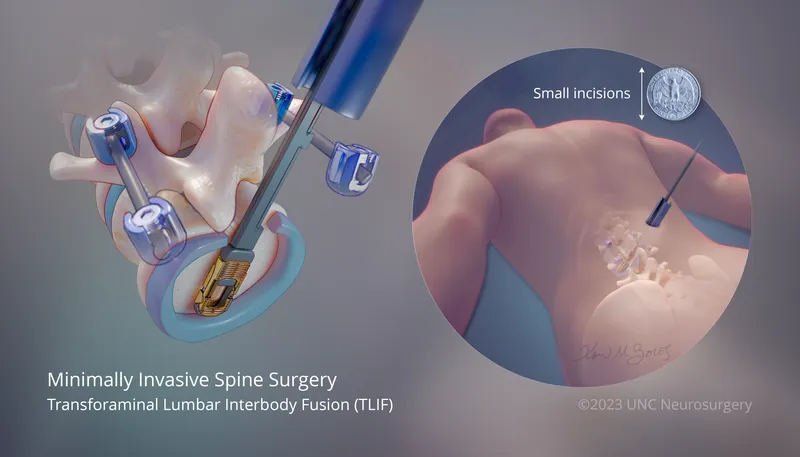
⭐ Persistent radicular pain post-MISS often indicates incomplete foraminal decompression or nerve root irritation during surgery.
High‑Yield Points - ⚡ Biggest Takeaways
- MISS goals: Reduced iatrogenic injury (muscle, blood loss), shorter hospital stay, quicker recovery.
- Key procedures: Microdiscectomy for disc herniation, percutaneous fixation for instability, MIS-TLIF/XLIF/OLIF for fusion.
- Enabling tech: Fluoroscopy, navigation systems, robotics, endoscopy, specialized tubular retractors.
- Primary indications: Degenerative disc disease, lumbar spinal stenosis, herniated nucleus pulposus, select deformity/trauma.
- Complications (lower than open): Nerve root injury, dural tear, infection, implant issues, persistent pain.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

