Intro & Pre-Prosthetic Care - Goals & Groundwork
- Primary Goals: Restore function, mobility, independence, cosmesis, and improve Quality of Life (QoL).
- Patient Assessment (Holistic):
- Medical: Comorbidities, stump condition (vascularity, skin).
- Psychological: Motivation, realistic expectations, body image.
- Social: Support system, vocational needs, home environment.
- Pre-Prosthetic Management (Stump Focused):
- Stump Care:
- Hygiene, skin inspection, wound healing.
- Edema control: Elastic bandaging (figure-of-8), shrinker socks.
- Stump shaping & maturation: Aim for conical/cylindrical shape.
- Desensitization: Tapping, massage, friction.
- Exercises:
- Prevent contractures (esp. hip/knee flexion).
- Strengthen residual limb, core, trunk, upper limbs.
- Maintain/improve Range of Motion (ROM) of proximal joints.
- Manage phantom limb sensation/pain.
- Stump Care:
⭐ Optimal stump length for Below-Knee Amputation (BKA) is 12.5-17.5 cm (Transtibial) from medial tibial plateau for best prosthetic fit and function.
Prosthetic Prescription - Fit For Function
- Prescription: Individualized, considering:
- Amputation: Level, residual limb (length, shape, skin, power).
- Patient: K-level (functional potential), goals, comorbidities, motivation.
- Component Selection:
- Socket: Critical for fit (e.g., PTB, TSB, Ischial Containment).
- Suspension: For secure attachment (e.g., Suction, Pin/Lock, VASS).
- Knee/Ankle Units: Based on K-level (e.g., single-axis, multi-axis, microprocessor).
- Terminal Device: Foot (SACH, dynamic response) or hand/hook.
- Checkout & Verification: Ensures optimal fit and function.
> ⭐ Proper socket fit (total contact, specific pressure distribution) is paramount for prosthetic success and user comfort.
Lower Limb Training - Steps to Strides
- Objective: Achieve safe, symmetrical, energy-efficient gait for functional independence.
- Core Principles: Early mobilization, progressive weight-bearing, balance (static & dynamic), proprioceptive training.
- Gait Training Sequence:
- Essential Skills:
- Prosthesis donning/doffing, stump hygiene.
- Transfers: Sit-to-stand, bed, chair, floor.
- Fall prevention & "up from floor" techniques.

⭐ Energy expenditure with a transtibial prosthesis is typically 10-30% higher than normal; transfemoral can be 40-70% higher, impacting endurance.
Upper Limb Training - Grasping Independence
- Goal: Achieve functional independence in Activities of Daily Living (ADLs) with the prosthesis.
- Training Phases:
- Controls Training: Mastering operation of terminal device (TD), wrist, elbow (if applicable). Body-powered (cable tension) or myoelectric (EMG signals).
- Use Training: Repetitive drills for grasp, release, positioning. Focus on smooth, coordinated movements.
- Functional Training: Integrating prosthesis into ADLs (e.g., eating, dressing, writing).
- Grasp Patterns: Practice tripod, lateral (key), cylindrical, spherical, hook grasps with varied objects.
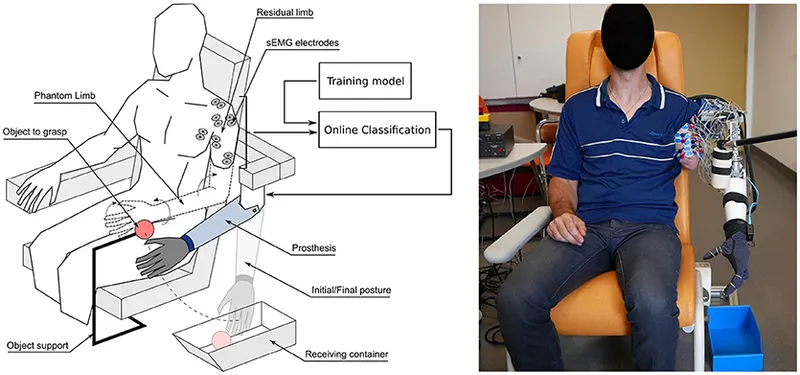
⭐ Phantom limb sensation/pain can significantly impact training; early management is crucial for prosthetic acceptance and functional use.
Complications & Outcomes - Bumps & Beyond
- Stump Issues:
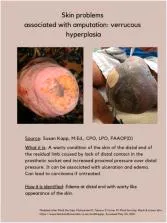
- Skin: Dermatitis, ulcers, infection, verrucous hyperplasia, epidermoid cysts.
- Pain: Residual Limb Pain (RLP) - neuroma, spurs; Phantom Limb Pain (PLP).
- Prosthetic Problems: Socket misfit (pistoning, bell-clapping), alignment issues, component wear/failure.
- Systemic: ↑Energy expenditure, contralateral joint OA, psychological impact.
- Management: Hygiene, socket adjustments, pain meds (gabapentin for PLP), therapy.
- Outcomes: Measured by Amputee Mobility Predictor (AMP), Timed Up and Go (TUG), 6-Minute Walk Test (6MWT); patient satisfaction (TAPES).
⭐ Verrucous hyperplasia at stump end often due to distal negative pressure/poor fit.
High‑Yield Points - ⚡ Biggest Takeaways
- Early mobilization and comprehensive pre-prosthetic training are vital for successful outcomes.
- Phantom limb pain requires multimodal management: pharmacotherapy, mirror therapy, TENS.
- Meticulous stump care (hygiene, desensitization, shaping) prevents infection and skin issues.
- Progressive gait training focuses on balance, symmetrical weight-bearing, and efficient ambulation.
- Correct socket fit is paramount; poor fit causes pain and prosthetic rejection.
- Energy expenditure is notably ↑, particularly for transfemoral amputations.
- Psychosocial support is crucial for addressing body image concerns and depression.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

