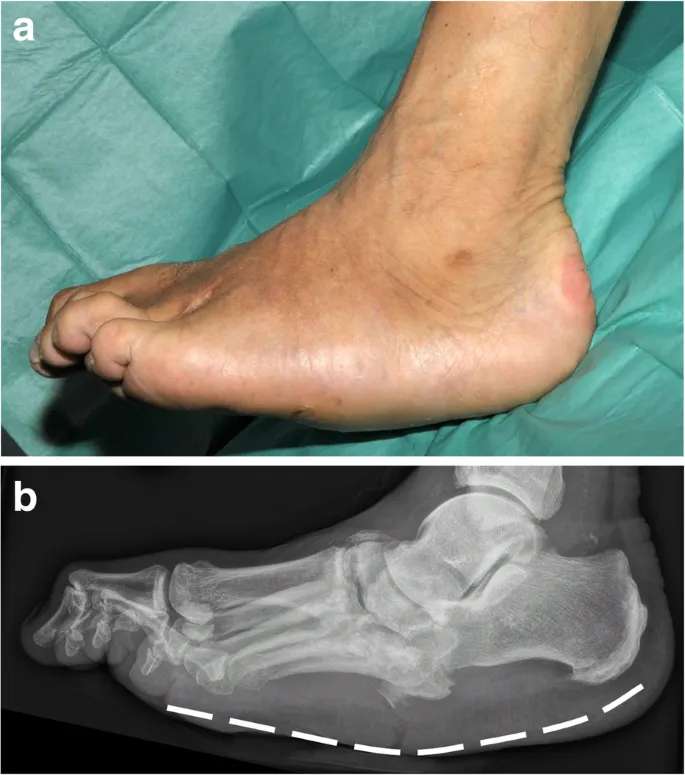
Hallux Valgus - Bunion Busters
Lateral deviation of great toe (valgus) & medial deviation of 1st metatarsal (varus).
- Key Angles:
- HVA (Hallux Valgus Angle): Normal < 15°
- IMA (Intermetatarsal Angle): Normal < 9°
- DMAA (Distal Metatarsal Articular Angle): Normal < 10°
- Severity (approx.):
- Mild: HVA 15-20°, IMA 9-11°
- Moderate: HVA 21-39°, IMA 12-17°
- Severe: HVA ≥ 40°, IMA ≥ 18°
- Surgical Principles: Correct deformity, relieve pain, restore function. Involves soft tissue release (e.g., adductor hallucis), medial eminence resection, osteotomies, or arthrodesis.
- Common Procedures:
- Chevron/Austin (distal osteotomy): Mild to moderate deformity.
- Scarf (diaphyseal osteotomy): Moderate to severe deformity.
- Lapidus (1st TMT arthrodesis): Severe deformity, hypermobility, arthritis.
- Akin (phalangeal osteotomy): Adjunct for residual hallux valgus interphalangeus.
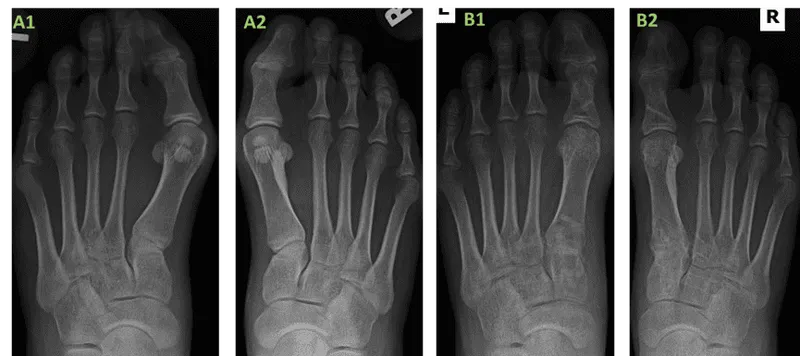
⭐ The position of the tibial sesamoid relative to the first metatarsal head is a key radiographic indicator of hallux valgus severity (Hardy and Clapham classification).
AAFD - Flat Foot Fixes
AAFD: Progressive flatfoot from Posterior Tibial Tendon Dysfunction (PTTD).

Ankle Arthritis - Joint Relief Roadmap
-
Etiologies: Post-traumatic (most common), inflammatory (e.g., RA), primary OA.
-
Clinical/Radiographic: Pain, ↓ROM, swelling. X-ray: ↓joint space, osteophytes, subchondral cysts/sclerosis.
-
Ankle Arthrodesis (Fusion):
- Indications: Younger, active patients; severe deformity; failed TAA; infection; heavy labor.
- Outcome: Durable pain relief, stability; sacrifices ankle motion.
-
Total Ankle Arthroplasty (TAA):
- Indications: Older (>60 yrs), lower-demand patients; desire to preserve motion; bilateral disease.
- Contraindications: Active infection, severe talar AVN, significant deformity, young/high-demand.
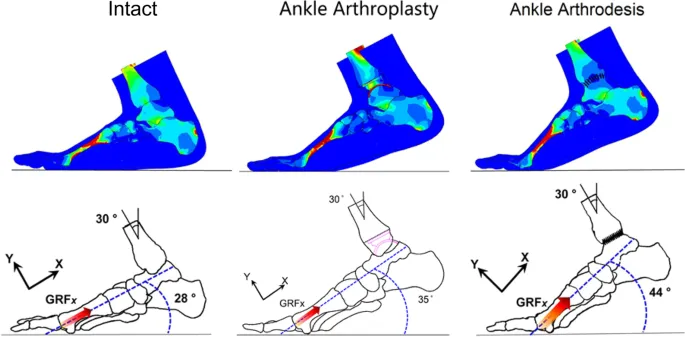
Arthrodesis vs. TAA Comparison:
| Feature | Ankle Arthrodesis | Total Ankle Arthroplasty (TAA) |
|---|---|---|
| Durability | High, often lifelong | Lower, potential for revision |
| Ankle Motion | Eliminates | Preserves some |
| Activity Level | Tolerates higher loads, impact limited | Low impact activities preferred |
| Complications | Nonunion, malunion, adjacent arthritis | Aseptic loosening, wear, infection, subsidence |
Charcot Foot - Stability Strategies
- Patho: Neurotraumatic (insensate microtrauma) & Neurovascular (↑ flow → osteolysis).
- Risk: DM + peripheral neuropathy.
- Eichenholtz Stages (X-ray):
- 0 (Prodromal): Inflammation, normal X-ray.
- I (Development): Fragmentation, dislocation, debris.
- II (Coalescence): Debris absorption, early fusion.
- III (Reconstruction): Remodeling, deformity (rocker-bottom).
- Clinical: Acute (hot, red, swollen, bounding pulses) vs. Chronic (deformity, instability).
- Goal: Stable, plantigrade, shoeable foot.
- Management:
- Offloading: TCC crucial (gold standard).
- Medical: Bisphosphonates (controversial).
- Surgical (instability, deformity, ulcers): Exostectomy, osteotomy, arthrodesis, fixation.
⭐ Total Contact Casting (TCC) is the gold standard for offloading in acute Charcot foot, achieving healing in up to 90% of cases when combined with appropriate wound care.
High‑Yield Points - ⚡ Biggest Takeaways
- Triple arthrodesis: Fuses TC, TN, CC joints for rigid hindfoot deformity.
- Lapidus procedure: 1st TMT fusion for hallux valgus with 1st ray hypermobility.
- Keller arthroplasty: Resection for hallux rigidus in elderly, low-demand patients.
- Ankle arthrodesis: Gold standard for end-stage ankle arthritis, ensuring stability.
- Tendon transfers: Key for dynamic correction in conditions like PTTD (e.g., FDL transfer).
- Lisfranc injuries: Often require ORIF or primary arthrodesis for stable reduction.
- Charcot foot: Reconstruction aims for plantigrade, stable foot, often with arthrodesis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more