Overview & Primaries - Cancer's Bony Outposts
- Definition: Secondary tumor deposits in bone from a distant primary malignancy. Most common bone tumors in adults.
- Common Adult Primaries (Mnemonic 📌 PB KTL):
- Prostate cancer
- Breast cancer
- Kidney (Renal Cell Ca)
- Thyroid cancer
- Lung cancer
- Myeloma (primary marrow cancer, presents with bone lesions).
⭐ Most common primary cancer metastasizing to bone in adult males is Prostate cancer; in adult females is Breast cancer.
- Commonest Primary in Children: Neuroblastoma.
- Skeletal Predilection: Axial skeleton (vertebrae, pelvis, ribs, skull) & proximal long bones; due to abundant red marrow (hematogenous spread).
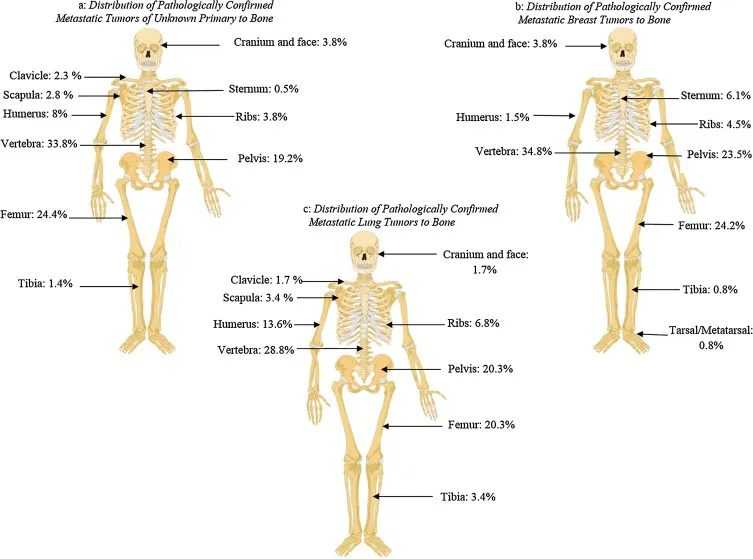
Pathophysiology & Patterns - How Tumors Invade
- Mechanisms of Tumor Spread:
- Hematogenous: Most common; Batson's plexus of veins (valveless) facilitates vertebral metastases.
- Lymphatic spread.
- Direct extension from adjacent tumor.
- Patterns of Bone Involvement:
- Osteolytic (bone destruction): Lung, Kidney, Thyroid, Multiple Myeloma. Mediated by ↑osteoclast activity (e.g., RANKL, PTHrP).
- Osteoblastic (bone formation): Prostate, Carcinoid. Mediated by ↑osteoblast activity (e.g., Endothelin-1).
- Mixed patterns: Breast, GI tumors.
- Key Molecular Players: RANKL, OPG (Osteoprotegerin), PTHrP (Parathyroid Hormone-related Protein), DKK-1 (Dickkopf-1), Endothelin-1.
- Commonest Skeletal Sites: Vertebrae (>50%), Pelvis, Ribs, Femur (proximal), Humerus (proximal). (📌 "Very Painful Ribs Feel Horrible")
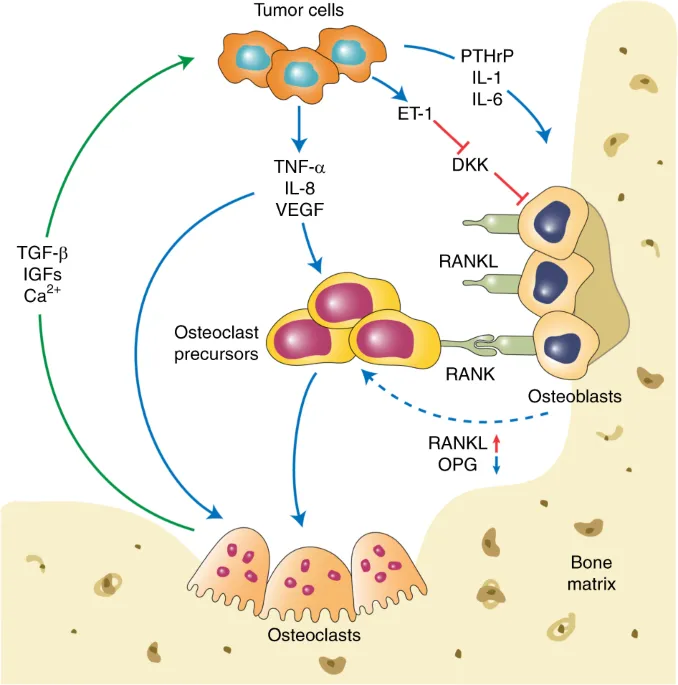
⭐ Osteolytic lesions are predominantly mediated by osteoclast activation via the RANK-RANKL pathway, often stimulated by PTHrP.
Diagnosis & Staging - Spotting the Spread
- Presentation: Bone pain (often nocturnal, mechanical, worse with activity), pathological fractures, hypercalcemia (nausea, confusion), spinal cord compression (neurological deficits, bladder/bowel dysfunction).
- Labs: Sr. Calcium, Alkaline Phosphatase (Alk Phos), PSA (for prostate cancer), other relevant tumor markers.
- Imaging:
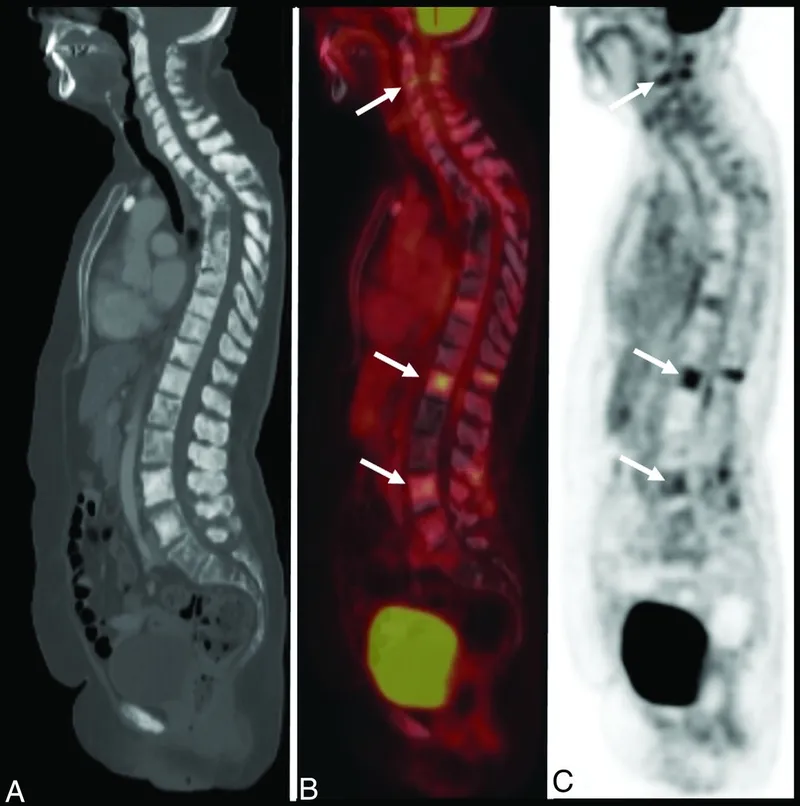
- X-ray: Initial; may show lytic (lucent), blastic (sclerotic), or mixed lesions; periosteal reaction.
- Bone Scan (Tc-99m MDP): Detects ↑osteoblastic activity / bone turnover (hot spots).
⭐ Bone scan (Tc-99m MDP) is highly sensitive for osteoblastic metastases but can be falsely negative in purely lytic lesions (e.g., multiple myeloma, renal cell carcinoma); skeletal survey or PET-CT preferred then.
- MRI: Best for marrow infiltration, soft tissue extension, spinal cord assessment (especially for compression).
- PET-CT: Whole-body staging, assessing metabolic activity, and treatment response.
- Biopsy Indications: Unknown primary tumor, solitary bone lesion (to rule out primary bone tumor), or if diagnosis is unclear after imaging.
- Mirels' Scoring: For impending pathological fracture risk in long bones (Site, Pain, Lesion type [lytic/blastic/mixed], Size). Score >8 often indicates need for prophylactic fixation.
- Diagnostic Flow:
Treatment & Complications - Fighting Back & Fallout
Goals: Pain relief, function, stability, local control, prevent fractures. Multidisciplinary.
Systemic Therapy:
- Chemo, Hormonal, Targeted, Immunotherapy.
- Bone-modifying: Zoledronic acid (4mg IV q3-4wks), Denosumab (120mg SC q4wks).
Local Therapy:
- Radiotherapy (RT): EBRT for pain (8Gy x1, 20Gy x5, 30Gy x10), MSCC.
- Surgery: Prophylactic fixation (Mirels' score), fracture stabilization, vertebroplasty.
Key Complications & Management:
- Pathological fractures: Surgical fixation.
- Spinal Cord Compression (MSCC): 🚨EMERGENCY!
- Hypercalcemia: IV fluids, bisphosphonates.
⭐ For suspected MSCC, immediate high-dose corticosteroids (e.g., Dexamethasone) are crucial pending urgent MRI and definitive treatment.
High‑Yield Points - ⚡ Biggest Takeaways
- Metastatic disease is the most common malignant bone tumor overall.
- Common primaries: Prostate (blastic), Breast (mixed/lytic), Lung (lytic), Kidney (lytic), Thyroid (lytic) (PBLKT).
- Axial skeleton (vertebrae, pelvis, ribs) is most frequently affected.
- Clinical features: Severe bone pain (worse at night), pathological fractures, hypercalcemia.
- Diagnosis: X-ray (lytic/blastic lesions), bone scan (sensitive for screening), biopsy (definitive).
- Management is primarily palliative, focusing on pain relief and fracture prevention (radiotherapy, bisphosphonates).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

