Indications & Contraindications - Joint's Last Stand?
- Indications (Why replace?):
- Severe, disabling pain; failed conservative Rx (meds, physio).
- Marked functional limitation impacting ADLs.
- Advanced joint destruction (radiographic):
- Osteoarthritis
- Rheumatoid Arthritis, other inflammatory arthritis
- Avascular necrosis (AVN)
- Post-traumatic arthritis
- Selected acute fractures (e.g., femoral neck).
- Contraindications (Why not?):
- Absolute:
- Active joint/systemic infection ⚠️.
- Medically unstable (e.g., severe cardiac/respiratory disease).
- Poor bone stock / inadequate soft tissue envelope.
- Non-functional extensor mechanism (relevant for knee arthroplasty).
- Relative:
- Younger age (< 50-55 yrs; consider implant longevity).
- Morbid obesity (BMI > 40 kg/m²; ↑risk of complications).
- Neuropathic (Charcot) joint.
- Poor patient motivation/unrealistic expectations.
- Significant peripheral vascular disease.
- Absolute:

⭐ Active infection is an absolute contraindication to arthroplasty; eradication is paramount, as performing surgery in its presence leads to high failure rates and complex revisions.
Pre-op Planning & Templating - Blueprint for Bone
Essential for surgical accuracy, aiming to restore native joint anatomy and biomechanics.
- Core Objectives:
- Determine correct implant size, type, and position.
- Precisely plan bone resections.
- Restore limb length equality (LLD), femoral/joint offset, and joint line.
- Anticipate potential intra-operative difficulties (e.g., bone defects, need for augments).
- Methodology:
- Detailed clinical history and physical examination.
- Standardized, calibrated radiographic views (AP/Lateral with magnification marker).
- Templating: Using digital software or acetate overlays.
- Hip: Acetabular inclination (40-45°), anteversion (15-20°). Femoral stem sizing and offset.
- Knee: Femoral and tibial component sizing, alignment to mechanical axis.
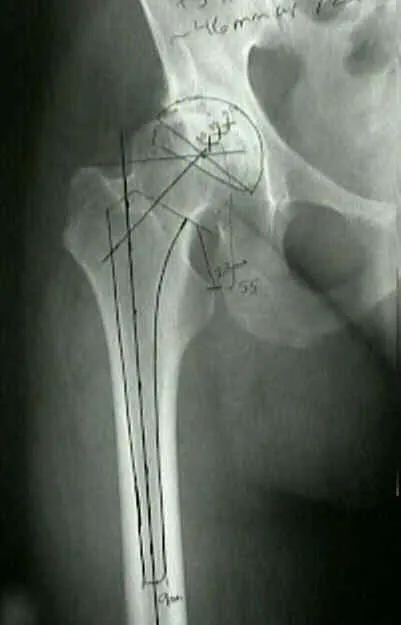
⭐ Accurate templating is proven to reduce operative time, blood loss, and improve the accuracy of implant placement, potentially decreasing early revision rates.
Implant Materials & Design - Bionic Bits & Bobs
- Metals:
- Stainless Steel (316L): Historical, corrosion.
- Cobalt-Chromium (Co-Cr): Strong, wear-resistant (heads, trays).
- Titanium & alloys (Ti-6Al-4V): Biocompatible, ↓modulus (↓stress shielding), for cementless stems (osseointegration).
- Polymers:
- UHMWPE (Ultra-High Molecular Weight Polyethylene): Standard bearing.
- HXLPE (Highly Cross-Linked Polyethylene): ↑Wear resistance.
- Ceramics:
- Alumina ($Al_2O_3$): Hard, low friction, brittle.
- Zirconia ($ZrO_2$): Tougher. For heads, liners.
- Bone Cement:
- PMMA (Polymethylmethacrylate): Acrylic grout, mechanical interlock.
- Key Design Aspects:
- Bearing Surfaces: 📌 Pairs: Metal-on-Poly (MoP), Ceramic-on-Poly (CoP), Ceramic-on-Ceramic (CoC).
- Fixation: Cemented (PMMA) vs. Cementless (porous coat for ingrowth).
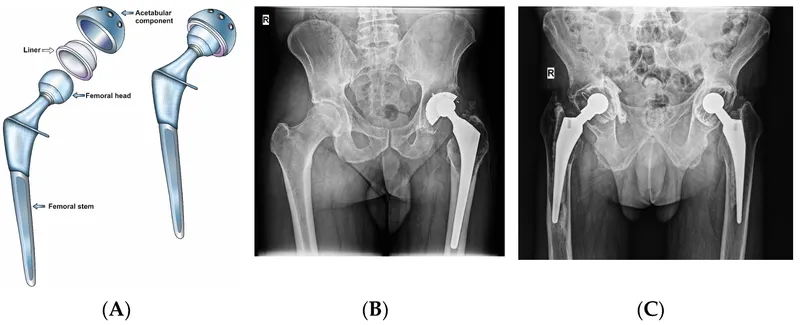
⭐ Ti alloys (Young's Modulus
110 GPa) closer to bone (10-30 GPa) than Co-Cr (~210 GPa), ↓stress shielding.
Surgical Principles & Fixation - The Replacement Ritual
-
Surgical Steps (📌 Mnemonic: Planning Always Beats Sloppy Technique Inside):
- Planning: Templating for component size, position, and alignment.
- Approach: Balance adequate exposure with soft tissue preservation.
- Bone Preparation: Precise cuts and reaming for optimal implant fit.
- Soft Tissue Balancing: Critical for joint stability, kinematics, and range of motion (ROM).
- Trialing: Assess component fit, stability, ROM, and leg length before final implantation.
- Implantation & Asepsis: Strict sterile technique to prevent Periprosthetic Joint Infection (PJI).
-
Fixation Methods:
- Cemented (PMMA - Polymethylmethacrylate):
- Mechanism: Mechanical interlock (grout).
- Indications: Typically older patients (e.g., >65-70 yrs), poor bone stock, osteoporosis, irradiated bone.
- Advantage: Immediate stability, allows early weight-bearing.
- Uncemented (Press-fit):
- Mechanism: Initial press-fit stability followed by biological fixation (osseointegration) via bone ingrowth into porous surfaces.
- Indications: Younger, more active patients (e.g., <65 yrs) with good bone stock.
- Advantage: Potential for durable, long-term biological fixation.
- Hybrid: Combination (e.g., cemented femoral stem, uncemented acetabular cup in Total Hip Replacement).
- Cemented (PMMA - Polymethylmethacrylate):

⭐ The "cement mantle" thickness is critical in cemented arthroplasty; ideal is 2-4 mm. An incomplete or uneven mantle can lead to stress concentration and early aseptic loosening.
High‑Yield Points - ⚡ Biggest Takeaways
- Primary goals: Pain relief, functional restoration, and improved quality of life.
- Key indications: End-stage arthritis (OA, RA), avascular necrosis (AVN), certain fractures.
- Absolute contraindication: Active infection (local or systemic).
- Fixation: Cemented (PMMA, older patients) vs. Uncemented (bone ingrowth, younger patients).
- Common bearings: Metal-on-Polyethylene (MoP), Ceramic-on-Polyethylene (CoP).
- Most common long-term failure: Aseptic loosening (wear debris, osteolysis).
- Most feared complication: Periprosthetic Joint Infection (PJI).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

